How many codes in ICD 10?
- ICD-10 codes were developed by the World Health Organization (WHO) External file_external .
- ICD-10-CM codes were developed and are maintained by CDC’s National Center for Health Statistics under authorization by the WHO.
- ICD-10-PCS codes External file_external were developed and are maintained by Centers for Medicare and Medicaid Services. ...
Where can one find ICD 10 diagnosis codes?
Search the full ICD-10 catalog by:
- Code
- Code Descriptions
- Clinical Terms or Synonyms
What are the new ICD 10 codes?
The new codes are for describing the infusion of tixagevimab and cilgavimab monoclonal antibody (code XW023X7), and the infusion of other new technology monoclonal antibody (code XW023Y7).
What is the ICD 10 code for unresponsive?
Unspecified coma
- Tabular List of Diseases and Injuries. The Tabular List of Diseases and Injuries is a list of ICD-10 codes, organized "head to toe" into chapters and sections with coding notes ...
- Index to Diseases and Injuries. ...
- Approximate Synonyms
- Clinical Information. ...
- Convert R40.20 to ICD-9 Code. ...
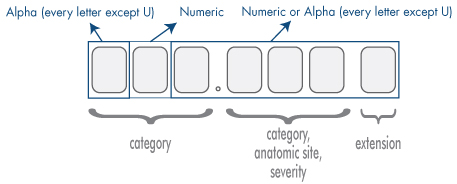
What is the ICD-10 code for confusion?
Altered mental status, unspecified. R41. 82 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM R41.
What is the ICD-10 code for altered mental status?
R41. 82 Altered mental status, unspecified - ICD-10-CM Diagnosis Codes.
What is disorientation unspecified?
A mental state in which a person is confused, disoriented, and not able to think or remember clearly. The person may also be agitated and have hallucinations, and extreme excitement. A mental state in which one is not thinking clearly.
What is the ICD-10 code for Delirium of unclear cause?
Delirium due to known physiological condition The 2022 edition of ICD-10-CM F05 became effective on October 1, 2021.
What is the difference between altered mental status and encephalopathy?
Encephalopathy is a term used for any diffuse disease of the brain that alters brain function or structure. The hallmark of encephalopathy is “altered mental status,” a clinical symptom not a diagnosis.
How do you code altered level of consciousness?
Altered mental status, unspecified (R41. 82) is a billable ICD-10 diagnostic code under HIPAA regulations from October 1, 2020, to September 30, 2021. This code is acceptable to insurers when used to describe a marked change in mental health status not attributable to other factors.
What's the difference between disoriented and disorientated?
The main difference between the two is the origin. Disorientated is a British English word, while disoriented is an American English word. Disoriented and disorientated can be used in place of each other, but it will make more sense depending on where you are located.
What does sudden confusion mean?
About sudden confusion (delirium) Being in a state of confusion means: not being able to think clearly or quickly. feeling disorientated. struggling to pay attention, make decisions, or remember things.
What is another word for disorientation?
disarray, confusion, confusedness, delusion, hallucination, mental confusion, muddiness.
What is altered mental status?
“Altered mental status” is a vague, often misleading description that encompasses a host of presentations that include changes in cognition, mood, behavior and/or level of arousal such as: Coma. Stupor. Delirium and/or encephalopathy. Dementia or other neurocognitive disorders.
What is the ICD 10 code for brain fog?
R41. 840 Attention/concentration deficit (inability to focus)
What is the diagnosis for ICD 10 code r50 9?
9: Fever, unspecified.
What is the convention of ICd 10?
The conventions for the ICD-10-CM are the general rules for use of the classification independent of the guidelines. These conventions are incorporated within the Alphabetic Index and Tabular List of the ICD-10-CM as instructional notes.
What is the ICD-10-CM?
The ICD-10-CM has two types of excludes notes. Each type of note has a different definition for use but they are all similar in that they indicate that codes excluded from each other are independent of each other.
What does "with" mean in a code?
The word “with” should be interpreted to mean “associated with” or “due to” when it appears in a code title, the Alphabetic Index, or an instructional note in the Tabular List.
How many external cause codes are needed?
More than one external cause code is required to fully describe the external cause of an illness or injury. The assignment of external cause codes should be sequenced in the following priority:
Why are diagnostics present on admission exempt?
Note: “Diagnosis present on admission” for these code categories are exempt because they represent circumstances regarding the healthcare encounter or factors influencing health status that do not represent a current disease or injury or are always present on admission
What is code assignment?
Code assignment is based on the provider’s documentation of the relationship between the condition and the care or procedure. The guideline extends to any complications of care, regardless of the chapter the code is located in. It is important to note that not all conditions that occur during or following medical care or surgery are classified as complications. There must be a cause-and-effect relationship between the care provided and the condition, and an indication in the documentation that it is a complication. Query the provider for clarification, if the complication is not clearly documented.
When to use counseling Z code?
Counseling Z codes are used when a patient or family member receives assistance in the aftermath of an illness or injury , or when support is required in coping with family or social problems. They are not used in conjunction with a diagnosis code when the counseling component of care is considered integral to standard treatment.
Popular Posts:
- 1. icd 10 code for elongated palate
- 2. icd 10 code for sob with exertion
- 3. icd-10 code for hypertonicity
- 4. icd 10 code for cellulitis right finger
- 5. icd 9 code for lap band complication
- 6. icd 10 cm code for inflamation of sacroiliac joint
- 7. icd code for pruritus
- 8. icd-10 code for failed medication treatment
- 9. what is the icd-10 code for eye pain
- 10. icd 10 code for intolerenace to trazadone