Full Answer
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
What is the ICD 10 code for aortoiliac atherosclerosis?
The ICD-10-CM code I70.0 might also be used to specify conditions or terms like abdominal aortic atherosclerosis, aortic arch atherosclerosis, aortoiliac atherosclerosis, arteriosclerosis of abdominal aorta, arteriosclerosis of aorta , arteriosclerosis of thoracic aorta, etc.
What is the ICD 10 code for aortic stenosis?
Other nonrheumatic aortic valve disorders
- I35.8 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM I35.8 became effective on October 1, 2021.
- This is the American ICD-10-CM version of I35.8 - other international versions of ICD-10 I35.8 may differ.
What is the CPT code for right iliac venogram?
I82.521 Chronic embolism and thrombosis of right iliac vein I82.522 Chronic embolism and thrombosis of left iliac vein I82.523 Chronic embolism and thrombosis of iliac vein, bilateral Postthrombotic Syndrome I87.001 Postthrombotic syndrome without complications of right lower extremity I87.002
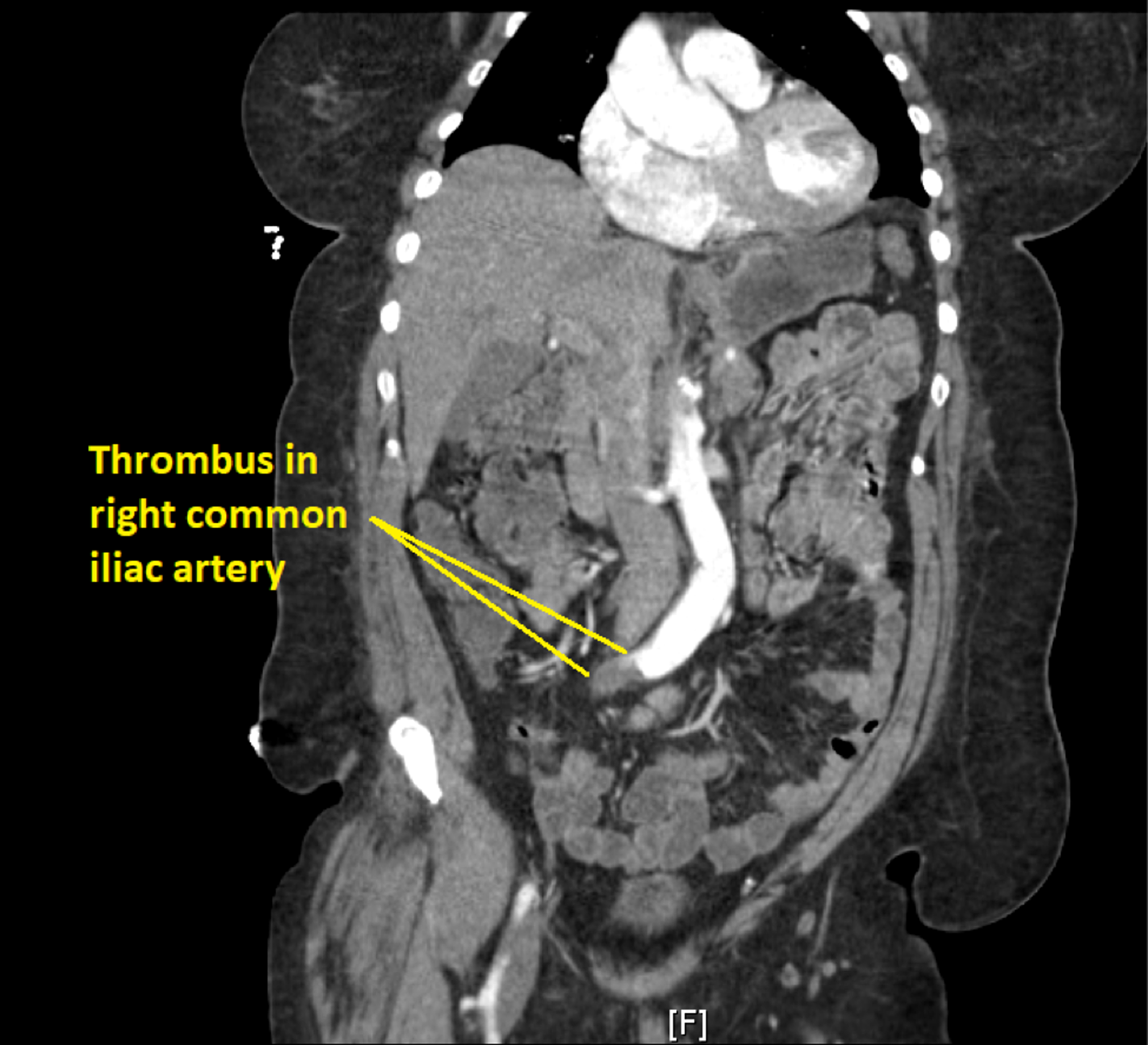
What is the ICD 10 code for common iliac artery stenosis?
5 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM I74. 5 became effective on October 1, 2021. This is the American ICD-10-CM version of I74.
What is the ICD 10 code for arterial stenosis?
ICD-10 code I65. 2 for Occlusion and stenosis of carotid artery is a medical classification as listed by WHO under the range - Diseases of the circulatory system .
What is the ICD 9 code for hip pain?
ICD-9-CM 719.45 converts approximately to: 2022 ICD-10-CM M25. 559 Pain in unspecified hip.
What is the ICD 10 code for subclavian stenosis?
The 2022 edition of ICD-10-CM I65. 22 became effective on October 1, 2021. This is the American ICD-10-CM version of I65.
What is iliac artery stenosis?
It occurs when the iliac artery that brings blood to your legs becomes narrow or blocked by plaque. Symptoms can include pain, numbness, or cramping in the lower limbs, gangrene in the feet, and erectile dysfunction (ED) in men.
What is the ICD-10 code for right common femoral artery stenosis?
213.
What are ICD-9 and ICD-10 codes?
Code Structure: Comparing ICD-9 to ICD-10ICD-9-CMICD-10-CMConsists of three to five digitsConsists of three to seven charactersFirst character is numeric or alpha ( E or V)First character is alphaSecond, Third, Fourth and Fifth digits are numericAll letters used except U3 more rows•Aug 24, 2015
What is the ICD-10 diagnosis code for hip pain?
ICD-10 Code for Pain in unspecified hip- M25. 559- Codify by AAPC.
What are ICD-9 procedure codes?
ICD-9-CM is the official system of assigning codes to diagnoses and procedures associated with hospital utilization in the United States. The ICD-9 was used to code and classify mortality data from death certificates until 1999, when use of ICD-10 for mortality coding started.
What is stenosis of left subclavian artery?
In subclavian stenosis, the artery is simply narrowed, leading to decreased blood flow beyond the area of blockage. When the subclavian blockage is severe, or if the artery is completely blocked, a condition called 'subclavian steal' can occur (Figure 4).
What is the ICD-10 code for aortic stenosis?
ICD-10 Code for Nonrheumatic aortic (valve) stenosis- I35. 0- Codify by AAPC.
What is proximal subclavian artery stenosis?
The pathophysiology of subclavian steal syndrome is severe stenosis or occlusion of the proximal subclavian artery, leading to retrograde flow through the vertebral artery. 2. Coronary subclavian steal syndrome is a similar phenomenon occurring in patients after CABG, utilizing an in situ left or right IMA.
Incidence and Prevalence of IIAS
Incidence and prevalence of IIAS have not been established in general population. Although isolated IIAS is probably rare, IIAS is often associated with common iliac artery stenosis.
Symptoms and Functional Impairment
The main symptom is the lower back, hip, buttock, or thigh claudication defining the proximal claudication, a fatigue, discomfort, or pain occurring in specific muscle groups alimenting by IIA during effort due to exercise-induced ischemia and which is relieved with rest ( 2, 6 ).
Strategies and Evidences
Patients typically report a gradual decrease of their walking capacity, which is evaluated by the maximal walking distance ( 2 ). Claudication traditionally stops within 10 min after the end of walking ( 22, 23 ).
Areas of Uncertainties
To date, no algorithm has been proposed to perform the IIAS diagnosis taking account the cost of the exams and their possible results to help for the diagnosis. Studies are lacking about the sensitivity and specificity of several exams such as ultrasound exam, CTA, or MRA on the specific IIAS evaluation.
Guidelines
An expert multidisciplinary committee organized by the ACC and the AHA have reported comprehensive guidelines for the management of LEAD in 2013 ( 11 ). Surprisingly, neither this committee nor the TASC II working group mentioned the way of managing IIAS ( 4, 11 ).
Conclusion
This review shows that when a patient has a proximal walking pain, physician should look for IIAS. We also found that literature is very sparse and that guidelines and recommendations have to be addressed to know how to manage IIAS.
Conflict of Interest Statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.

Popular Posts:
- 1. icd 10 pcs code for repair of skin, right hand
- 2. icd 10 code for foot drop left
- 3. icd 10 code for mediastinoscopy?
- 4. icd 10 code for hematocolpos
- 5. icd 10 code for broncho laryngomalacia
- 6. icd 10 cm code for pain right thumb
- 7. icd 9 code for status post lung transplant
- 8. free testosterone icd 10 for labcorp test code
- 9. icd 10 code for diverticulosis left colon
- 10. icd 10 code for total knee replacement left