How exactly do you tear your ACL?
Torn anterior cruciate ligament (ACL) definition and facts
- The anterior cruciate ligament is one of the four ligaments in the knee that provides stabilization for the knee joint.
- Torn ACLs are a common knee injury.
- An ACL tear or sprain occurs with a sudden change in direction or pivot against a locked knee.
- A pop, followed by pain and swelling of the knee are the most common symptoms of an ACL tear.
What can be done for an ACL tear?
model of self-care at home:
- Rest. General rest is necessary for healing and limits weight bearing on your knee.
- Ice. When you're awake, try to ice your knee at least every two hours for 20 minutes at a time.
- Compression. Wrap an elastic bandage or compression wrap around your knee.
- Elevation. Lie down with your knee propped up on pillows.
What to do after an ACL tear?
- Chesterfield's Manny Oyeleke is set to face boyhood club Chelsea in the FA Cup
- The midfielder was on the Blues' books but they released him for being too small
- Six years ago, Oyeleke was unemployed with an injured ACL and no income
- Oyeleke has come a long way since asking for Universal Credit during his injury
How to protect yourself from an ACL tear?
- Jog the 50 yards (45.7 m). Jog slowly and easily to allow your muscles to engage.
- Jog sideways. Start with your knees bent and side step your way across the 50 yards. At 25 yards, turn around so that you are leading with the other leg. ...
- Jog backwards. Land on your toes while you run backwards. Keep your knees slightly bent so that they will not lock. ...
What is the ACL in the knee?
What is the VAS scale for pain?
About this website
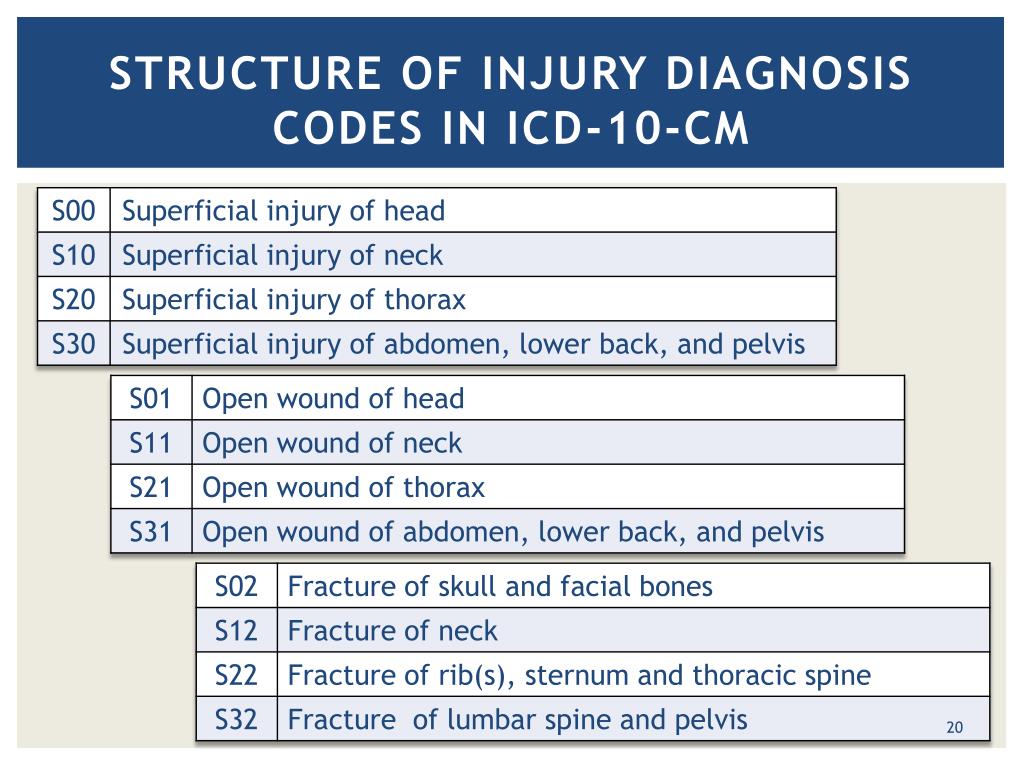
What is the ICD-10 code for ACL tear?
ICD-10 code S83. 512A for Sprain of anterior cruciate ligament of left knee, initial encounter is a medical classification as listed by WHO under the range - Injury, poisoning and certain other consequences of external causes .
What is the ICD-10 code for ACL tear left knee?
S83. 512A - Sprain of anterior cruciate ligament of left knee [initial encounter]. ICD-10-CM.
What is the ICD-10 code for status post ACL reconstruction?
ICD-10: Z96. 651, Status (post), organ replacement, by artificial or mechanical device or prosthesis of, joint, knee-see presence of knee joint implant.
What is the medical code for knee pain?
M25. 569 - Pain in unspecified knee. ICD-10-CM.
What's an ACL injury?
If you tear the anterior cruciate ligament (ACL) in your knee, you may need to have reconstructive surgery. The ACL is a tough band of tissue joining the thigh bone to the shin bone at the knee joint. It runs diagonally through the inside of the knee and gives the knee joint stability.
What is ACL medical term?
The two ligaments inside the knee that “cross” each other are called the anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL). Both ligaments attach on one side to the end of the thighbone (femur) and on the other to the top of the shinbone (tibia).
What is diagnosis code Z98 89?
Other specified postprocedural statesICD-10 code Z98. 89 for Other specified postprocedural states is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .
What is the difference between subsequent and sequela?
D (subsequent encounter) describes any encounter after the active phase of treatment, when the patient is receiving routine care for the injury during the period of healing or recovery. S (sequela) indicates a complication or condition that arises as a direct result of an injury.
What is the ICD 10 code for right knee pain?
M25. 561 Pain in right knee - ICD-10-CM Diagnosis Codes.
What is the ICD-10 code for knee injury?
Superficial injury of knee and lower leg ICD-10-CM S80. 912A is grouped within Diagnostic Related Group(s) (MS-DRG v39.0):
What is the ICD-10 DX code for knee injury?
Superficial injury of knee and lower leg ICD-10-CM S80. 911A is grouped within Diagnostic Related Group(s) (MS-DRG v39.0):
What is the ICD-10 code for both knee pain?
Bilateral primary osteoarthritis of knee M17. 0 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM M17. 0 became effective on October 1, 2021.
When will the ICD-10-CM S83.512A be released?
The 2022 edition of ICD-10-CM S83.512A became effective on October 1, 2021.
What is the secondary code for Chapter 20?
Use secondary code (s) from Chapter 20, External causes of morbidity, to indicate cause of injury. Codes within the T section that include the external cause do not require an additional external cause code. Type 1 Excludes.
What is the ICd 10 code for a failed ACL tear?
If a patient has a failed ACL tear of the left knee and ends up having an ACL revision done.... do we use the ICD 10 code S83.512D or T84.410A or both? Any help or input would be greatly appreciated.
What is S83.512A?
The patient at one time had a traumatic ACL Tear (S83.512A) which was treated by ACL Reconstruction. Some time after the original procedure, it was found that the "Reconstruction" had failed, but the reason for this is not given.
What is the ACL in the knee?
tissue which courses from the femur to the tibia. The ACL is a key structure in the knee joint, as it resists anterior tibial translation and rotational loads. When the knee is extended, the ACL has a mean length of 32 mm and a width of 7-12 mm. There are two components of the ACL, the anteromedial bundle (AMB) and the posterolateral bundle (PLB). They are not isometric with the main change being lengthening of the AMB and shortening of the PLB during flexion. The ACL has a microstructure of collagen bundles of multiple types (mostly type I) and a matrix made of a network of proteins, glycoproteins, elastic systems, and glycosaminoglycans with multiple functional interactions. The complex ultrastructural organization and abundant elastic system of the ACL allow it to withstand multiaxial stresses and varying tensile strains. The ACL is innervated by the posterior articular branches of the tibial nerve and is vascularized by branches of the middle genicular artery.2
What is the VAS scale for pain?
Pain: Pain is typically measured on a visual analogue scale (VAS) from 0 to 10 with 0 representing no pain and 10 representing the worst pain. Information should be gathered on the patient’s current, worst, and least pain level. Aggravating and alleviating factors should be identified.

Popular Posts:
- 1. icd 9 code for external otitis media
- 2. icd 9 code for history of small bowel ostomy
- 3. icd 10 code for j pouch
- 4. what is the icd 10 code for scarring of nerve of foot
- 5. icd 10 code for low vitamin b
- 6. icd code for delivery of baby
- 7. icd 10 code for squamous cell cancer of skin
- 8. icd 10 code for wisdom teeth removal
- 9. icd code for complete heart block
- 10. icd 10 code for bartholin cyst removal