What is the prognosis of ovarian cancer?
Overall, epithelial ovarian cancers have a five-year relative survival rate of 48 percent. This means that on average, people with epithelial ovarian tumors are about half as likely as people without this cancer to live at least five years. However, a person’s prognosis also depends on how far cancer has spread.
What were your first symptoms of ovarian cancer?
The most common symptoms include:
- Bloating
- Pelvic or abdominal (belly) pain
- Trouble eating or feeling full quickly
- Urinary symptoms such as urgency (always feeling like you have to go) or frequency (having to go often)
What are some of the symptoms of ovarian cancer?
Signs and symptoms of ovarian cancer may include:
- Abdominal bloating or swelling
- Quickly feeling full when eating
- Weight loss
- Discomfort in the pelvic area
- Fatigue
- Back pain
- Changes in bowel habits, such as constipation
- A frequent need to urinate
What is my personal risk of ovarian cancer?
What is my Personal Risk of Ovarian Cancer?
- Average Ovarian Cancer Risk. You don’t have any family history of breast or ovarian cancer. ...
- Slightly Increased Risk. Do you have a history of infertility (difficulty getting pregnant)? ...
- Moderately Increased Risk. Has your mother, sister or daughter had ovarian cancer? ...
- Very Increased Risk. ...
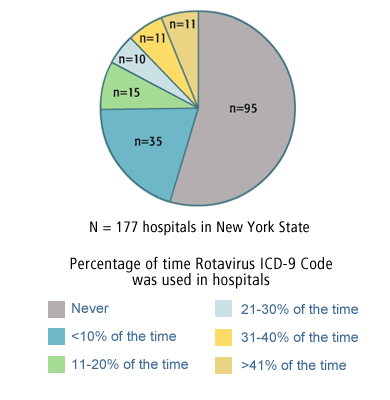
How do you code Family history of ovarian cancer?
41.
What is the code for ovarian cancer?
Malignant neoplasm of unspecified ovary C56. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM C56. 9 became effective on October 1, 2021.
What is c44 42 diagnosis?
42 for Squamous cell carcinoma of skin of scalp and neck is a medical classification as listed by WHO under the range - Malignant neoplasms .
What is ICD-10 code for history of endometrial cancer?
ICD-10-CM Code for Personal history of malignant neoplasm of other parts of uterus Z85. 42.
What is the ICD-10 code for history of ovarian cancer?
ICD-10 code Z85. 43 for Personal history of malignant neoplasm of ovary is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .
What diagnosis is code C56 9?
C56. 9, Malignant neoplasm of unspecified ovary.
What is ICD-10 code for basal cell carcinoma?
Basal cell carcinoma of skin, unspecified C44. 91 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM C44. 91 became effective on October 1, 2021.
How do ICD-10 code atypical squamous cells of undetermined significance?
610 for Atypical squamous cells of undetermined significance on cytologic smear of cervix (ASC-US) is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is metastatic squamous cell carcinoma?
Squamous cell carcinoma - a very common form of nonmelanoma skin cancer that originates in the squamous cells - becomes metastatic when it spreads (metastasizes) beyond the primary cancer site and affects other areas of the body.
What is the ICD-10 code for history of endometriosis?
N80. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM N80.
What is the ICD-10 code for endometrial cancer?
ICD-10 Code for Malignant neoplasm of endometrium- C54. 1- Codify by AAPC.
What is the ICD-10 code for history of hysterectomy?
Z90. 710 - Acquired absence of both cervix and uterus | ICD-10-CM.
What is the ICD-10 code for ovarian mass?
Unspecified ovarian cyst, left side N83. 202 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM N83. 202 became effective on October 1, 2021.
How do you code an ovarian mass?
ICD-10 code N83. 20 for Unspecified ovarian cysts is a medical classification as listed by WHO under the range - Diseases of the genitourinary system .
What is diagnosis code Z51 11?
ICD-10 code Z51. 11 for Encounter for antineoplastic chemotherapy is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .
What are the symptoms of ovarian cyst cancer?
Signs and symptoms of ovarian cancer may include:Abdominal bloating or swelling.Quickly feeling full when eating.Weight loss.Discomfort in the pelvic area.Fatigue.Back pain.Changes in bowel habits, such as constipation.A frequent need to urinate.
What is the ICd 10 code for cancer?
For more context, consider the meanings of “current” and “history of” (ICD-10-CM Official Guidelines for Coding and Reporting; Mayo Clinic; Medline Plus, National Cancer Institute):#N#Current: Cancer is coded as current if the record clearly states active treatment is for the purpose of curing or palliating cancer, or states cancer is present but unresponsive to treatment; the current treatment plan is observation or watchful waiting; or the patient refused treatment.#N#In Remission: The National Cancer Institute defines in remission as: “A decrease in or disappearance of signs or symptoms of cancer. Partial remission, some but not all signs and symptoms of cancer have disappeared. Complete remission, all signs and symptoms of cancer have disappeared, although cancer still may be in the body.”#N#Some providers say that aromatase inhibitors and tamoxifen therapy are applied during complete remission of invasive breast cancer to prevent the invasive cancer from recurring or distant metastasis. The cancer still may be in the body.#N#In remission generally is coded as current, as long as there is no contradictory information elsewhere in the record.#N#History of Cancer: The record describes cancer as historical or “history of” and/or the record states the current status of cancer is “cancer free,” “no evidence of disease,” “NED,” or any other language that indicates cancer is not current.#N#According to the National Cancer Institute, for breast cancer, the five-year survival rate for non-metastatic cancer is 80 percent. The thought is, if after five years the cancer isn’t back, the patient is “cancer free” (although cancer can reoccur after five years, it’s less likely). As coders, it’s important to follow the documentation as stated in the record. Don’t go by assumptions or averages.
What is the ICd 10 code for primary malignancy?
According to the ICD-10 guidelines, (Section I.C.2.m):#N#When a primary malignancy has been excised but further treatment, such as additional surgery for the malignancy, radiation therapy, or chemotherapy is directed to that site, the primary malignancy code should be used until treatment is complete.#N#When a primary malignancy has been excised or eradicated from its site, there is no further treatment (of the malignancy) directed to that site, and there is no evidence of any existing primary malignancy, a code from category Z85, Personal history of malignant neoplasm, should be used to indicate the former site of the malignancy.#N#Section I.C.21.8 explains that when using a history code, such as Z85, we also must use Z08 Encounter for follow-up examination after completed treatment for a malignant neoplasm. This follow-up code implies the condition is no longer being actively treated and no longer exists. The guidelines state:#N#Follow-up codes may be used in conjunction with history codes to provide the full picture of the healed condition and its treatment.#N#A follow-up code may be used to explain multiple visits. Should a condition be found to have recurred on the follow-up visit, then the diagnosis code for the condition should be assigned in place of the follow-up code.#N#For example, a patient had colon cancer and is status post-surgery/chemo/radiation. The patient chart notes, “no evidence of disease” (NED). This is reported with follow-up code Z08, first, and history code Z85.038 Personal history of other malignant neoplasm of large intestine, second. The cancer has been removed and the patient’s treatment is finished.
What is a follow up code?
This follow-up code implies the condition is no longer being actively treated and no longer exists. The guidelines state: Follow-up codes may be used in conjunction with history codes to provide the full picture of the healed condition and its treatment. A follow-up code may be used to explain multiple visits.
Is cancer history?
History of Cancer: The record describes cancer as historical or “history of” and/or the record states the current status of cancer is “cancer free,” “no evidence of disease,” “NED,” or any other language that indicates cancer is not current. According to the National Cancer Institute, for breast cancer, the five-year survival rate ...
Does history of cancer affect relative value units?
The fear is, history of will be seen as a less important diagnosis, which may affect relative value units . Providers argue that history of cancer follow-up visits require meaningful review, examinations, and discussions with the patients, plus significant screening and watching to see if the cancer returns.
What is the ICD-10 code for ovarian cancer?
ICD-10 requires you to code to the greatest degree of specificity. If you have bilateral ovarian cancer, you should use BOTH the right ovarian cancer (C56.1) and the left ovarian cancer (C56.2) codes. The unspecified code (C56.9) might be appropriate for a patient diagnosed on biopsy if it is impossible to determine a site of origin.
What are the codes for metastatic cancer?
For example, a stage 4 ovarian cancer may be coded using 3 codes: C56.1 (malignant neoplasm of the right ovary), C78.6 (secondary malignancy of the peritoneum and retroperitoneum, and J91.0 (malignant pleural effusion). How do you code for borderline ovarian tumors ...
What is CPT code 38573?
In 2018, the CPT code 38573 (Laparoscopy, surgical ; with bilateral total pelvic lymphadenectomy and peri-aortic lymph node sampling, peritoneal washings, peritoneal biopsy (ies), omentectomy, and diaphragmatic washings, including diaphragmatic and other serosal biopsy (ies), when performed.) was created to address situation where a Gyn Onc is asked to perform staging where another surgeon has performed the laparoscopic BSO ± hysterectomy.
What is the CPT code for a laparoscopic BSO?
For a laparoscopic BSO with staging (for a patient with prior hysterectomy, for instance), you can use the CPT code 38573 (Laparoscopy, surgical; with bilateral total pelvic lymphadenectomy and peri-aortic lymph node sampling, peritoneal washings, peritoneal biopsy (ies), omentectomy, and diaphragmatic washings, including diaphragmatic and other serosal biopsy (ies), when performed) with a -22 modifier. That would be billed with the laparoscopic BSO CPT code 58661 with the -59 modifier for a second surgery. With any -22 modifier, you would need to have an operative note and letter requesting increased reimbursement with the rationale, in this case the extra time and effort for “debulking”.
What is the CPT code for a hysterectomy?
This code specifically excludes hysterectomy codes. If you perform a laparoscopic hysterectomy, BSO, debulking, the proper CPT code would be 58575 (Laparoscopy, surgical, total hysterectomy for resection of malignancy (tumor debulking), with omentectomy including salpingo-oophorectomy, unilateral or bilateral, when performed).
What is the ICd code for appendectomy?
The operative report documentation should clearly describe the procedure and the reason for performing it. You should also append a distinct ICD code, such as C78.5, secondary malignant neoplasm of the large bowel.
What is the ICd10 code for peritoneal malignancy?
The series 58950-58952 can only be used with ICD10 codes for ovarian, tubal or primary peritoneal malignancy. 58953-58954 may be used with any diagnosis. All describe various combinations of procedures commonly performed for advanced gynecologic cancers.

Section 1.C.2 Provides Guidance
- According to the ICD-10 guidelines, (Section I.C.2.m): When a primary malignancy has been excised but further treatment, such as additional surgery for the malignancy, radiation therapy, or chemotherapy is directed to that site, the primary malignancy code should be used until treatment is complete. When a primary malignancy has been excised or era...
Defining Terms with Care
- For more context, consider the meanings of “current” and “history of” (ICD-10-CM Official Guidelines for Coding and Reporting; Mayo Clinic; Medline Plus, National Cancer Institute): Current: Cancer is coded as current if the record clearly states active treatment is for the purpose of curing or palliating cancer, or states cancer is present but unresponsive to treatment; the curr…
Active Treatment vs. Preventative Care
- What if a patient with breast cancer is status post-surgery/chemotherapy/radiation and is currently on tamoxifen for five years? If the patient is on tamoxifen or an aromatase inhibitor, such as Arimidex®, is that active treatment or preventive care (to inhibit returning cancer). Ultimately, what determines active treatment versus preventive care is how the drug is used. For example: 1. Ne…
The Provider Perspective
- Do providers agree with the above guidelines, or are the clinical and coding worlds at odds? According to a presentation by James M. Taylor, MD, CPC, providers look at cancer at a cellular level; whereas, coding guidelines look more at the organ level. In his opinion, common concerns among providers are: 1. Some neoplasms may not be active but remain at a cellular level, and c…
“History Of” Doesn’T Mean A Lesser Service
- I’ve heard providers worry about the level of medical decision-making assigned to a history of diagnosis, versus a current status diagnosis. The fear is, history of will be seen as a less important diagnosis, which may affect relative value units. Providers argue that history of cancer follow-up visits require meaningful review, examinations, and discussions with the patients, plus …
Popular Posts:
- 1. icd 9 code for dry eyes
- 2. icd 10 code for hydronephrosis with obstruction
- 3. icd code for ppd test placement
- 4. icd 10 code for urinary incomtience
- 5. icd 9 cm code for ileostomy
- 6. icd 10 code for infalmation of surgical site
- 7. which icd 10 code is for a history of tobacco use
- 8. icd 10 code for thoracolumbar fusion
- 9. icd 10 code for ascus
- 10. icd 10 diagnosis code for history of ectopic pregnancy