What causes a cervical protrusion disc?
What is Cervical Disc Protrusion?
- Causes of Cervical Disc Protrusion. Cervical disc protrusion generally develops in the age group of 30–50 years because of trauma to the cervical spine.
- Symptoms of Cervical Disc Protrusion. ...
- Diagnosis of Cervical Disc Protrusion. ...
- Treatment for Cervical Disc Protrusion. ...
What cervical disc affects the left arm?
- C5 radiculopathy. Tingling, numbness, and/or pain may go from the neck into the shoulder and/or down the arm and into the thumb. ...
- C6 radiculopathy. Tingling, numbness, and/or pain may radiate through the arm and into the second digit (index finger). ...
- C7 radiculopathy. ...
- C8 radiculopathy. ...
How to cure disc osteophyte complex?
Treatment options for symptomatic bone spurs in the neck could include:
- Activity modification. Perhaps a day or two of rest, or limiting strenuous activities, could help. ...
- Physical therapy. ...
- Ice and/or heat therapy. ...
- Medications or injections. ...
- Manual manipulation. ...
How is cervical disc disease diagnosed?
Sometimes headaches result from cervical degenerative disc problems. Cervical disc disorders if advanced enough are diagnosable on plain x-ray, which shows collapse or reduction in the height of the disc and possible bone spurs and bony end plate changes. An MRI is most useful diagnostic imaging for these conditions.
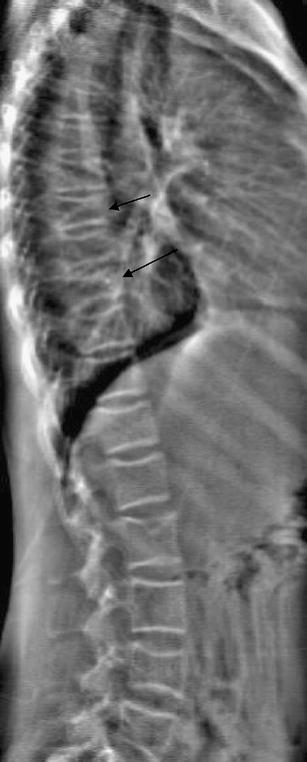
What is a cervical osteophyte?
Cervical osteophytes are bone spurs that grow on any of the seven vertebrae in the cervical spine (neck), ranging from the base of the skull, C1 vertebra, to the base of the neck, C7 vertebra.
Is an osteophyte a bone spur?
Osteophytes are bony lumps (bone spurs) that grow on the bones of the spine or around the joints. They often form next to joints affected by osteoarthritis, a condition that causes joints to become painful and stiff. Osteophytes can grow from any bone, but they're most often found in the: neck.
What is a disk osteophyte complex in the cervical spine?
Disc osteophyte complex is the development of osteophytes (bone spurs) affecting more than one intervertebral disk or spinal vertebrae. Osteophytes or bone spurs develop in the musculoskeletal system due to normal wear and tear as you age.
What is the ICD 10 code for osteoarthritis of cervical spine?
812.
What causes cervical osteophytes?
Causes of cervical osteophytes include diffuse idiopathic skeletal hyperostosis, ankylosing spondylitis, degenerative changes, and prior trauma, including surgery [5]. Anterior cervical osteophytes are generally asymptomatic; however, in rare cases, they can lead to dysphagia, dysphonia, and dyspnea [6-7].
What does osteophyte mean in medical terms?
Overview. Bone spurs are bony projections that develop along bone edges. Bone spurs (osteophytes) often form where bones meet each other — in your joints. They can also form on the bones of your spine. The main cause of bone spurs is the joint damage associated with osteoarthritis.
What is foraminal disc osteophyte?
Foraminal disc osteophyte complex: Bone spurs that develop in the foramen – the hollow archways on both sides of two adjacent vertebra, through which the spinal nerve roots run. Facet Joint Osteophytes: Bone spurs that develop surrounding the facet joints, which help connect two adjacent vertebrae together.
What is broad based disc osteophyte complex?
The disc osteophyte complex is a protruding ridge composed of chronically bulging disc encased with bony hypertrophy and granulation or scar tissue and is different from a focal or pure disc herniation, which are less common in the cervical spine.
What is neural foraminal narrowing C5 C6?
Overview. Neural foraminal stenosis, or neural foraminal narrowing, is a type of spinal stenosis. It occurs when the small openings between the bones in your spine, called the neural foramina, narrow or tighten.
What is the ICD-10 code for cervical degenerative disc disease?
ICD-10 code M50. 30 for Other cervical disc degeneration, unspecified cervical region is a medical classification as listed by WHO under the range - Dorsopathies .
What is the ICD-10 code for cervical stenosis?
ICD-10 code: M48. 02 Spinal stenosis Cervical region.
What is cervical osteoarthritis?
Cervical spondylosis is also called cervical osteoarthritis. It is a condition involving changes to the bones, discs, and joints of the neck. These changes are caused by the normal wear-and-tear of aging. With age, the discs of the cervical spine gradually break down, lose fluid, and become stiffer.
What is the diagnosis code for cervicalgia?
Code M54.2 is the diagnosis code used for Cervicalgia (Neck Pain). It is a common problem, with two-thirds of the population having neck pain at some point in their lives.
What is the ICD-10 code?
ICD-10 codes are the byproduct of that revision. This medical classification list is generated by the World Health Organization (WHO), and is used to help healthcare providers identify and code health conditions. ICD-10 is required for use by physicians and healthcare providers under the Health Insurance Portability & Accountability Act (HIPAA) ...
How long does cervical spine pain last?
Pain in cervical spine for less than 3 months. Pain in cervical spine for more than 3 months. Pain, cervical (neck) spine, acute less than 3 months. Pain, cervical (neck), chronic, more than 3 months. Chronic neck pain. Chronic neck pain for greater than 3 months. Chronic neck pain greater than 3 months.

Popular Posts:
- 1. icd 10 code for t6 compression fracture
- 2. icd 10 code for chronic pain r lower leg
- 3. icd 10 code for r10
- 4. icd 10 code for immunosuppressed status due to inhaled cyclosporine a
- 5. icd 10 code for head cancer
- 6. icd 10 code for bad cholesterol
- 7. icd 10 code for greater saphenous vein thrombosis
- 8. icd-10-cm code for abnormal cervical pap smear
- 9. icd 10 code for left foot reconstruction
- 10. icd 10 code for methamphetamine abuse