What is the ICD 10 code for slow response time?
2018/2019 ICD-10-CM Diagnosis Code R46.4. Slowness and poor responsiveness. R46.4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
How do you code therapy time in a code?
When codes are ranked in sequential typical times, and the actual time is between two typical times, use the code with the typical time closest to the actual time. Let’s look at psychotherapy codes to illustrate the second rule. In this example, the actual psychotherapy time with the patient is 37 minutes.
What Z codes are applicable to the ICD 10?
Possible applicable Z codes include: Z59.0-, Homelessness ICD-10-CM Official Guidelines for Coding and Reporting FY 2022 Page 19 of 115 Z59.1, Inadequate housing Z59.5, Extreme poverty Z75.1, Person awaiting admission to adequate facility elsewhere
How do you list ICD 10 codes on a resume?
List first the ICD-10-CM code for the diagnosis, condition, problem, or other reason for encounter/visit shown in the medical record to be chiefly responsible for the services provided. List additional codes that describe any coexisting conditions.

How do you bill on time?
A sample billable hours chart For example, if you worked for 15 minutes at a rate of $100 per hour, you could use the chart to see that the time increment is 0.3. So, 0.3 x $100 = $30 to bill. You can also use a billable hours calculator to help expedite the process.
How do you document time?
You still must spend more than 50 percent of your time on counseling or coordination. To properly document your time, use statements like these: “I spent 30 minutes face-to-face with the patient, over half in discussion of the diagnosis and the importance of compliance with the treatment plan.”
How do you code time in 2021?
For longer visits there is a prolonged visit code, 99417, that should be reported with 99205/99215 for every 15 minutes that total time exceeds the ranges for those codes....Tips for using total time to code E/M office visits in 2021.ActivityTime (minutes)Phone call with family member (POA)13 (recorded by phone)6 more rows•Nov 23, 2020
What is a time based code?
Under time-based coding, more than half of the face-to-face time (in the office or other outpatient setting) or more than half of the floor/unit time (in the hospital or nursing facility) must be spent on counseling or coordinating care.
Can you bill for documentation time?
You can't bill for documentation. Documentation takes time—there's no denying that. Even if you have an EMR system that streamlines the process, there's still a lot of effort that goes into creating notes that are complete, correct, and compliant.
What should be documented for time based coding?
The following must be documented in the patient's medical record in order to report an E/M service based on time: The total length of time of the E/M visit; Evidence that more than half of the total length of time of the E/M visit was spent in counseling and coordinating of care; and.
What is the time requirement for 99213?
CPT® code 99213: Established patient office or other outpatient visit, 20-29 minutes.
How is time counted under CPT em code and guideline changes 2021?
Under CPT® rules you start counting based on the minimum time required for the code. For instance, 99205 represents 60-74 minutes in 2021. You may add +99417 as soon as the encounter reaches 75 minutes, which is 15 minutes beyond the minimum required time of 60 minutes.
What is the time requirement for 99215?
40-54 minutesThe total time corresponding to CPT ® codes 99202-99215 have been defined as specific intervals. For example, in order to report 99215, 40-54 minutes of total time must be spent on the date of the encounter. Currently, the time requirement for 99215 is “typically” 40 minutes. Medical decision-making elements.
Can you bill 97110 for 10 minutes?
For example, a patient under a PT plan of care receives skilled treatment consisting of 20 minutes of therapeutic exercise (CPT 97110) and 20 minutes of gait training (CPT 97116). The total “Timed Code Treatment Minutes” documented will be 40 minutes.
Is 99214 a time based code?
The 99214 time allotment is between 30-39 minutes. Providers must record exact beginning and end times in the patient record. Although coding is now mainly determined by time and medical decision making, health care professionals should still document patient history and perform examinations when appropriate.
What is the CPT time rule?
The CPT midpoint rule, which says that “a unit of time is attained when the midpoint is passed,” applies to codes that specify a time basis for code selection. Though not accepted by all payers, even Medicare allows the midpoint rule for some services.
How many minutes is 99214?
30-39 minutesCPT® code 99214: Established patient office or other outpatient visit, 30-39 minutes.
How do you em code?
Total time may be used alone to select the appropriate code level for office visit E/M services (99202-99205, 99212-99215). A key change in the new guidelines is the updated definition of time....Selecting E/M Codes by Total Time.CPT CodeTime Range9921320-29 minutes9921430-39 minutes9921540-54 minutes5 more rows
Is 99214 a time based code?
The 99214 time allotment is between 30-39 minutes. Providers must record exact beginning and end times in the patient record. Although coding is now mainly determined by time and medical decision making, health care professionals should still document patient history and perform examinations when appropriate.
How do I use CPT 99417?
CPT ® code 99417 may only be reported in conjunction with 99205 or 99215 if the codes were selected based on the time alone and not medical decision making. A service of less than 15 minutes should not be reported.
How many codes are needed for late effects?
Coding for a late effect usually requires two codes.
Which code is always sequenced second?
Appears in the Official Guidelines at I.A.7. Codes that are in brackets in the Alphabetic Index are always sequenced second.
What is the code for underlying neoplasm?
When you look up this code in the Tabular List, you’ll find the instructional note “Code first underlying neoplasm (C00-D49).”
What is the code for adrenal adenoma?
When you look up this code in the Tabular List, you’ll find an instructional note to “Code also” adrenal adenoma (D35.0-).
What is the meaning of sequencing in medical billing?
When we select diagnosis codes for billing, we are telling the story of a patient’s healthcare encounter. Patients often present with multiple conditions — some related, some not. Medical coders are tasked with selecting the most specific codes and putting them in the right order. This code arrangement is called “sequencing,” and it is an essential step to correct coding.
Does the coding convention provide sequencing direction?
This convention instructs that two codes may be required, but it does not provide sequencing direction.
What is the Medicare code for prolonged visits?
For longer visits there is a prolonged visit code, 99417 , that should be reported with 99205/99215 for every 15 minutes that total time exceeds the ranges for those codes. CMS, however, has decided to allow physicians and other qualified health care professional to bill for prolonged services only when they have exceeded the maximum time for a Level 5 visit by 15 minutes or more (at least 69 minutes for an established patient and 89 minutes for a new patient), rather than the minimum time. Because of the discrepancy, Medicare has its own code, G2212, for reporting prolonged services.
What is the extended visit code for a monitor?
For longer visits there is a prolonged visit code, 99417 , that should be reported with 99205/99215 for every 15 minutes that total time exceeds the ranges for those codes.
What is total time?
Total time includes all of the time the physician or QHP spend on that visit on the date of service. That means it includes prepping for the visit (e.g. chart review) and anything done after the visit (e.g. calling other clinicians and ordering tests or procedures) after the face-to-face portion of the visit. But it does not include staff time or time spent by the physician or QHP outside the date of the visit.
Can you record a task in less than a certain amount of time?
Some common tasks may be physically impossible for you to complete in less than a certain amount of time, which makes it easier to record. For example, my state requires physicians to check the Prescription Drug Monitoring Program (PDMP) when we prescribe controlled substances.
Do EHRs have timers?
But those minutes can add up. Some EHRs have timers that automatically track when you’re logged in to a patient's chart, which is imperfect, but helpful. If your system has this feature, make sure the EHR chart is open while you’re reviewing records (and take some notes about that review in the chart) before the visit, and make sure it’s open during the visit as well.
What is the CPT code for critical care?
CPT® provides a chart for critical care codes 99291 Critical care, evaluation and management of the critically ill or critically injured patient; first 30-74 minutes and +99292 Critical care, evaluation and management of the critically ill or critically injured patient; each additional 30 minutes (List separately in addition to code for primary service). Use this chart to determine which code (s) is appropriate for the total critical care time on a given day.
When is time the controlling factor in a patient's visit?
When time is the controlling factor in a patient’s visit, be sure to capture the appropriate time-based service code.#N#Per CPT®, unless there are code or code-range-specific guidelines, parenthetical instructions, or code descriptors to the contrary, the following standards apply to time measurement:#N#A unit of time is attained when the midpoint is passed. For example, an hour is attained when 31 minutes have elapsed (more than midway between zero and 60 minutes). A second hour is attained when 91 minutes have elapsed.#N#When codes are ranked in sequential typical times, and the actual time is between two typical times, use the code with the typical time closest to the actual time.
How many minutes are in a second hour?
A second hour is attained when 91 minutes have elapsed. When codes are ranked in sequential typical times, and the actual time is between two typical times, use the code with the typical time closest to the actual time.
Is time spent performing separately reportable procedures or services included in the time reported as critical care?
Time spent performing separately reportable procedures or services should not be included in the time reported as critical care . Example: A patient involved in a fire at home suffers multiple third-degree burns of the face, neck, and arms. The patient also suffers from smoke inhalation.
What is CPT billing?
In other Current Procedural Terminology (CPT®) E&M guidelines and for previous office/outpatient visits, time-based billing has a “typical time” specified, and there is a requirement that the provider must exceed that typical time, and greater than 50 percent of the time must be spent in counseling and/or coordination of care. Best-practice documentation has the provider attesting to exactly these specifications and giving some points as to what was discussed or addressed in the counseling or coordination of care.
What time does Chuck Buck talk on 10 Tuesdays?
Programming Note: Listen to Dr. Erica Remer when she co-hosts Talk Ten Tuesdays with Chuck Buck, Tuesdays at 10 a.m. Eastern.
Is time a guesstimated time?
Although time is often guesstimated, as opposed to formally being clocked in and out with a stopwatch, the provider should try to be accurate . If they were to get audited and the cumulative time claimed in a day exceeded the workday (or, even worse, 24 hours), there would be serious repercussions.
Does time have to be sequential?
The time is added over the course of the calendar day, and it does not need to be sequential. Here’s what time encompasses: Preparation to see the patient, such as reviewing tests done prior to the visit; The provider obtaining their own history and/or reviewing history obtained by someone else, like a medical assistant;
Does social time count as medical time?
Finally, social time doesn’t count, either . There is no medical necessity to make small talk about the patient’s family member’s wedding or the patient’s newfound love of birding during the pandemic. Although discussing niceties may be endearing and increase patient satisfaction, there is no associated reimbursement.
Does total time include face to face time?
To indicate billing based on time, the provider could develop an attestation that has a field to enter a specific amount of time, and note that the total time includes face-to-face and non-face-to-face time (including, but not limited to…). Here they could list a few of the activities that count toward total time, as bulleted above. It does not have to be comprehensive, but should support the amount of time being claimed.
How to eliminate time based coding?
As coders we can eliminate the confusion surrounding time-based coding by following these three easy steps: 1. Get in the habit of reviewing the code descriptors for the key terms that differentiate the specific rules; 2. Understand how and when to apply the rules; and. 3.
When did CPT start using time based coding?
Since 1992 , time-based coding for most of the E/M categories, as well as many other CPT® codes, has evolved. Today, we use terms such as total time, total visit time, face-to-face and non-face-to-face time, greater than 50 percent, CPT® midpoint rule, and rounding.
How long is 99401?
Take, for example, code 99401 Preventive medicine counseling and/or risk factor reduction intervention (s) provided to an individual (separate procedure); approximately 15 minutes: Eight minutes is past the midpoint of 15 minutes. If the time spent was less than eight minutes, then no code should be billed. If at least eight minutes is documented, however, you can report 99401.
What was the problem with the CPT code book prior to 1992?
This was a big problem. Physicians struggled with determin ing what E/M level to report, and payers could not assess the clinical documentation and reported E/M levels objectively.
What is face to face time?
Face-to-face time is defined as the time a provider spends directly interacting with the patient and/or family or caregiver and includes tasks such as obtaining a history, examination, and counseling. In 2008, the AMA introduced codes for Counseling Risk Factor Reduction and Behavior Change Intervention. These codes can be used when counseling patients on specific behaviors that may lead to illness or exacerbate an existing condition.
What is total time?
Total time is defined as the overall time on the day of the encounter during which a provider provides services related to patient care, even if the times are not consecutive. The time spent over the course of the day is totaled, with the day starting at 12:01 am and ending at midnight. The time calculation includes a provider’s face-to-face and non-face-to-face time. A provider’s total time may be calculated based on their start and stop times or simply a statement of total time.
How long can you report 99401?
If at least eight minutes is documented, however, you can report 99401. Another example is 99358 Prolonged evaluation and management service before and/or after direct patient care; first hour: For encounters lasting 31-60 minutes, you may bill this code. For encounters lasting less than 31 minutes, you cannot.
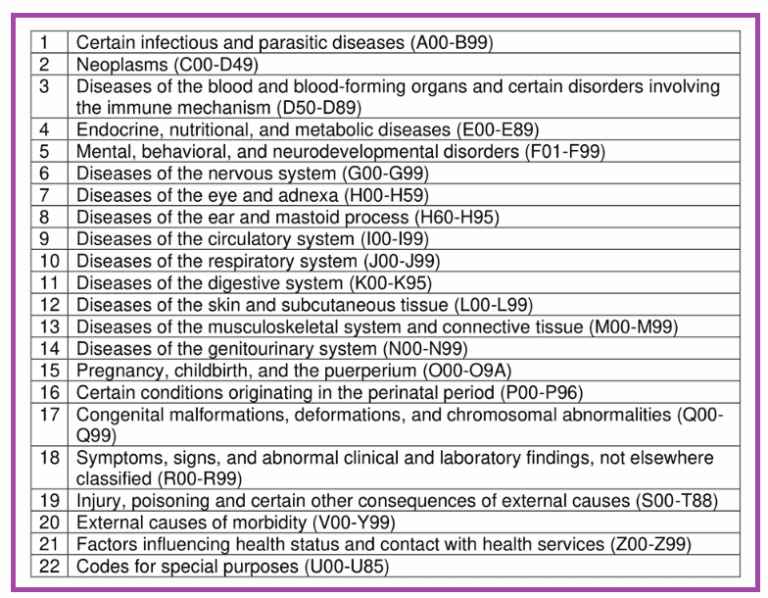
in Diseases Classified Elsewhere
sequela
- A sequela condition is one that results from a previous disease or injury. 1. Coding for a late effect usually requires two codes. 2. Sequencing comes directly from the Official Guidelines at I.B.10. Example: Keloid scar as a late effect of third-degree burn to the chest wall L91.0Hypertrophic scar T21.31XSBurn of third degree of chest wall, sequel...
Use Additional Code
- This convention instructs you to “Code first” the underlying condition, followed by etiology and/or manifestations. 1. Appears in the Official Guidelinesat I.A.13. 2. The “Use additional” code note is found below the underlying condition code. Example: Type 2 diabetes with stage three chronic kidney disease E11.22 Type 2 diabetes mellitus with diabetic chronic kidney disease When you l…
Code Also
- This convention instructs that two codes may be required, but it does not provide sequencing direction. 1. Appears in the Official Guidelinesat I.A.17. 2. The circumstances of the encounter will determine the sequencing. Example 1: Secondary pulmonary arterial hypertension in HIV (reason for the encounter is for HIV) B20Human immunodeficiency virus [HIV] disease I27.21Secondary …
Brackets
- This type of punctuation appears in both the Alphabetic Index and Tabular List. 1. Appears in the Official Guidelinesat I.A.7. Codes that are in brackets in the Alphabetic Index are always sequenced second. 2. Brackets are used in the Tabular List to enclose synonyms, alternative words, or explanatory phrases. Example: Exanthema epidemic with meningitis – Alphabetic Inde…
Popular Posts:
- 1. 2016 icd 10 code for gallbladder polyps
- 2. what is the icd 10 code for soft tissue radionecrosis
- 3. icd 10 code for toe ulcer left
- 4. icd code for dermatits of bilateral arms
- 5. what is the correct icd 10 code for bilateral epistaxis
- 6. icd 10 cm code for well child
- 7. icd 10 dx code for infiltration of iv
- 8. icd 10 code for personal history of hodgkin's lymphoma
- 9. icd-10-cm code for pityriasis rubra pilaris
- 10. icd 10 cm code for mrsa