What is the difference between primary and secondary hypercoagulable state?
Most often, primary hypercoagulable state will be reported as these don’t go away. For the secondary hypercoagulable state, if the acquired disorder resolves, so may the hypercoagulable state in most patients. Documentation shows that the patient has a venous thrombosis. Does this support coding the thrombosis and also the hypercoagulable state?
What is the ICD 10 code for hypercoagulable thrombophilia?
Hypercoagulable state, secondary; Thrombophilia; ICD-10-CM D68.69 is grouped within Diagnostic Related Group(s) (MS-DRG v 38.0): 814 Reticuloendothelial and immunity disorders with mcc; 815 Reticuloendothelial and immunity disorders with cc; 816 Reticuloendothelial and immunity disorders without cc/mcc; Convert D68.69 to ICD-9-CM. Code History
Is the diagnosis of hypercoagulable state documented?
The diagnosis of hypercoagulable state is documented, is it coded? That all depends on if it meets one of the criteria for reporting a diagnosis in ICD-10-CM. Chances are, the patient is under medical treatment for the condition or monitoring and follow up is normally required.
What is the most common cause of hypercoagulability?
The most common cause of inherited hypercoagulable state is activated protein C resistance (factor V Leiden) Malignancy/cancer is the second most common cause of hypercoagulable state and accounts for 10% to 20% of spontaneous venous thromboses
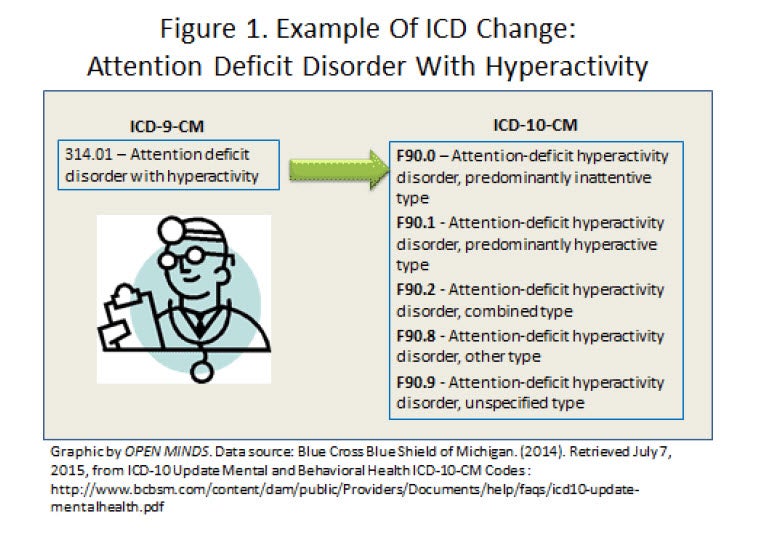
What is the ICD 10 code for secondary hypercoagulable state?
Yes, ICD 10 code D68. 69 (Other thrombophilia) groups multiple ICD 9 code descriptors within this category including secondary hypercoagulable state (previously 289.82).
What is secondary hypercoagulable state?
Secondary hypercoagulable states are primarily acquired disorders that. predispose to thrombosis through complex and multifactorial mechanisms. These involve blood flow abnormalities or defects in blood composition and of. vessel walls.
What is the ICD-10-CM code for hypercoagulable state?
59.
How do you code secondary thrombocytosis?
Other secondary thrombocytopenia D69. 59 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM D69. 59 became effective on October 1, 2021.
How is hypercoagulable state diagnosis?
Tests used to help diagnose inherited hypercoagulable states include: Genetic tests, including factor V Leiden (Activated protein C resistance) and prothrombin gene mutation (G20210A)* Antithrombin activity. Protein C activity.
What is acquired hypercoagulable state?
Abstract. Acquired hypercoagulable states comprise a diverse group of clinical conditions that are associated with an increased risk of thrombosis.
What is the ICD-10 code for long term anticoagulation?
01 Long term (current) use of anticoagulants.
What is the ICD-10 code for prothrombotic state?
D68. 59 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD-10 code for CVA?
I63. 9 - Cerebral infarction, unspecified | ICD-10-CM.
What is the difference between primary & secondary thrombocytosis?
Primary thrombocytosis is a myeloproliferative disease, caused by monoclonal or polyclonal abnormalities of haematopoietic cells or by abnormalities in the biology of Tpo. Secondary thrombocytosis is caused by stimulated megakaryopoiesis because of various haematological or non-haematological disorders.
How do primary and secondary thrombocytosis differ?
Even though the platelet count is elevated for a short time (or even indefinitely after splenectomy), secondary thrombocytosis does not typically lead to abnormal blood clotting. Primary thrombocytosis, or essential thrombocythemia, can cause serious bleeding or clotting complications.
What causes secondary thrombocytosis?
The pathophysiology of secondary thrombocytosis may differ, depending on the cause of thrombocytosis. Thrombocytosis is driven by overproduction of thrombopoietin, interleukin-6, other cytokines, or catecholamines in inflammatory, infectious, or neoplastic conditions or in situations of stress.
What is a hypercoagulable state?
Hypercoagulable states are blood disorders that increase the risk of deep vein thrombosis or embolic disease. The state is either inherited or acquired. About 80% of patients with blood clots have been found to have either an inherited or acquired clotting disorder. These blood clots can be lethal and some require life-long therapy. Hypercoagulable state is also known as thrombophilia. The patients that fall into one of these disorders have an increased tendency to develop blood clots. This is due to the presence of either an inherited factor or an acquired factor.
What is the second most common cause of hypercoagulable state?
Malignancy/cancer is the second most common cause of hypercoagulable state and accounts for 10% to 20% of spontaneous venous thromboses
What are the disorders that affect coagulation?
These include the disorders such as protein C and S, heparin cofactor, antithrombin III, fibrinogen, factor XIII, prothrombin, and plasminogen
Does a venous thrombosis need to be documented before coding?
Does this support coding the thrombosis and also the hypercoagulable state? NO! Since there is a thrombus wouldn’t that mean that the patient has a hypercoagulable state? NO! The physician must document the diagnosis before it can be coded. No assumptions can be made. Not all patients with a thrombosis have a hypercoagulable state or disorder.
Which mutation is most common in hypercoagulopathy?
Factor V Leiden mutation—this is the most common inherited factor associated hypercoagulopathy
Can a coder determine if a patient has primary or secondary hypercoagulation?
If only hypercoagulable state is diagnosed, can the coder look at the patient’s other diseases/diagnoses and determine by that if they have primary or secondary? NO! Only the physician can make the link between the cause/effect.
Is hypercoagulable state documented?
The diagnosis of hypercoagulable state is documented, is it coded? That all depends on if it meets one of the criteria for reporting a diagnosis in ICD-10-CM. Chances are, the patient is under medical treatment for the condition or monitoring and follow up is normally required. If documentation is unclear, a query would be needed to clarify if this was clinically significant on the current admission. Most often, primary hypercoagulable state will be reported as these don’t go away. For the secondary hypercoagulable state, if the acquired disorder resolves, so may the hypercoagulable state in most patients.
What are some examples of hypercoagulable states?
Examples are antithrombin III deficiency, protein C and S deficiencies, and dysfibrinogenemias. The checks and balances of clotting don’t work, so the patient clots excessively.
What is the code for D68.69?
Ronald Hirsch were having a lively discussion on LinkedIn regarding atrial fibrillation and the diagnosis of D68.69, Other thrombophilia which is the code used for “secondary hypercoagulable state.”.
Is thrombosis a hypercoagulable state?
My opinion is just having a propensity for developing a clot, especially in a specific location, does not constitute a hypercoagulable state. Thrombogenic, yes, hypercoagulable, no.
Is atrial fibrillation a secondary hypercoagulable state?
My vote is atrial fibrillation is not a “secondary hypercoagulable state.” There is literature that refers to it this way but prepare yourself for a denial appeal unless there are extenuating circumstances.

Popular Posts:
- 1. icd 10 code for pneumonia due to hemophilus influenzae
- 2. icd 10 cm code for abdominal discomfort.
- 3. icd 10 code for m47.812
- 4. icd-10 code for lumbar disc herniation with radiculopathy
- 5. what is the correct icd 10 code for c71.9
- 6. icd 10 code for ankylosing
- 7. icd 10 code for personal history of covid vaccine
- 8. icd 10 code for abcess on neck
- 9. icd 10 code for endometrial curettings
- 10. icd 10 code for exacerbation of ocd