Acute on chronic diastolic (congestive) heart failure. I50.33 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2019 edition of ICD-10-CM I50.33 became effective on October 1, 2018.
How to manage CHF exacerbations?
- Monitor your symptoms. Heart failure worsens over time, so you need to be familiar with changes in your body. ...
- Monitor your health. Keep track of blood pressure, weight and other vital signs as your doctor advises. ...
- Try to keep a positive attitude. ...
- Don’t be shy about asking questions. ...
How is a CHF exacerbation treated?
- Oral medication regimen for heart failure has been established for 24 h
- No intravenous vasodilator or inotropic agent for at least 24 h
- Ambulation before discharge to evaluate the beneficial effect of therapy and restoration of functional capacity
What is treatment of diastolic dysfunction?
With the high prevalence of hypertension and its associated complications, treatment of diastolic dysfunction in hypertension is an important and desirable goal. Angiotensin converting enzyme inhibitors and angiotensin receptor blockers have been shown to be effective in improvement of measures of diastolic function and are recommended as first-line agents in the control of hypertension in patients with diastolic heart failure.
What is Grade 3 left ventricular diastolic dysfunction?
What is Grade 3 left ventricular diastolic dysfunction? Grade III – This is a severe form of diastolic dysfunction characterized by restrictive filling of the heart that leads to symptoms of advanced heart failure. When the patient is asked to perform the Valsalva manoeuvre during echocardiography, the diastolic abnormalities seem to reverse.
What is the ICD-10 code for Acute on chronic CHF exacerbation?
23 for Acute on chronic systolic (congestive) heart failure is a medical classification as listed by WHO under the range - Diseases of the circulatory system .
What is Acute on chronic diastolic heart failure?
Acute heart failure can result from an event such as a viral infection or blockage affecting an artery around the heart. Doctors may call this “de novo” acute heart failure. It may instead result from damage in the heart, which may have developed over time. Doctors may call this “acute on chronic” heart failure.
What is ICD-10 code for diastolic heart failure?
ICD-10 Code for Diastolic (congestive) heart failure- I50. 3- Codify by AAPC.
How do you code CHF exacerbation?
Assign code I50. 9, heart failure NOS for a diagnosis of congestive heart failure. “Exacerbated” or “Decompensated” heart failure – Coding guidelines advise that “exacerbation” and “decompensation” indicate an acute flare-up of a chronic condition.
Is diastolic heart failure the same as congestive heart failure?
There is growing recognition that congestive heart failure (CHF) caused by a predominant abnormality in diastolic function (ie, diastolic heart failure) is both common and causes significant morbidity and mortality.
What is the difference between congestive heart failure and diastolic heart failure?
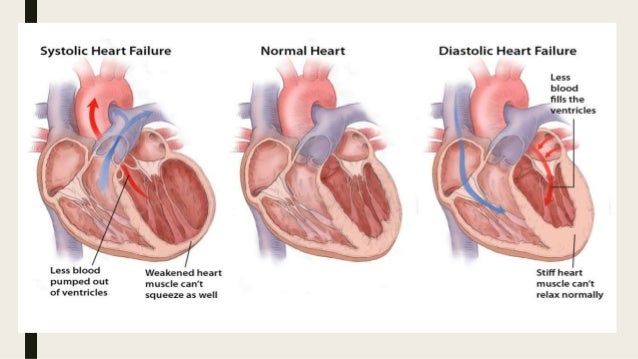
If you have systolic heart failure, it means your heart does not contract effectively with each heartbeat. If you have diastolic heart failure, it means your heart isn't able to relax normally between beats.
What are ICD-10 codes for heart failure?
9 – Heart Failure, Unspecified. Code I50. 9 is the diagnosis code used for Heart Failure, Unspecified.
How do you code chronic heart failure?
When the provider has linked either diastolic or systolic dysfunction with acute or chronic heart failure, it should be coded as 'acute/chronic diastolic or systolic heart failure. ' If there is no provider documentation linking the two conditions, assign code I50. 9, Heart failure, unspecified.”
What is the ICD-10 code for Acute respiratory failure?
00 for Acute respiratory failure, unspecified whether with hypoxia or hypercapnia is a medical classification as listed by WHO under the range - Diseases of the respiratory system .
What is the life expectancy of someone with diastolic heart failure?
Diastolic HF is associated with high mortality comparable with that of HF with depressed ejection fraction with a five year survival rate after a first episode of 43% and a higher excess mortality compared with the general population.
How serious is chronic diastolic failure?
If you have DD, you have an increased risk of death — even if your systolic function is normal and you have no other problems with how your heart is functioning, according to a study co-authored by Dr. Jaber.
Is diastolic heart failure a death sentence?
Although it can be a severe disease, heart failure is not a death sentence, and treatment is now better than ever. When this happens, blood and fluid may back up into the lungs (congestive heart failure), and some parts of the body don't get enough oxygen-rich blood to work normally.
What does acute on chronic systolic heart failure mean?
Systolic heart failure happens when your left ventricle cannot squeeze (contract) strongly enough. This means it can no longer pump out blood to your body very well. It's also called heart failure with reduced ejection fraction.
What is heart failure accompanied by?
Heart failure accompanied by edema, such as swelling of the legs and ankles and congestion in the lungs.
What is the clinical sign of heart failure?
Clinical symptoms of heart failure include: unusual dyspnea on light exertion, recurrent dyspnea occurring in the supine position, fluid retention or rales, jugular venous distension, pulmonary edema on physical exam, or pulmonary edema on chest x-ray presumed to be cardiac dysfunction.
What are the symptoms of a heart failure?
Signs and symptoms include shortness of breath, pitting edema, enlarged tender liver, engorged neck veins, and pulmonary rales.
What is the term for a condition in which the heart is unable to pump out enough blood to meet the metabolic?
A heterogeneous condition in which the heart is unable to pump out sufficient blood to meet the metabolic need of the body. Heart failure can be caused by structural defects, functional abnormalities (ventricular dysfunction), or a sudden overload beyond its capacity. Chronic heart failure is more common than acute heart failure which results from sudden insult to cardiac function, such as myocardial infarction.
When will ICD-10-CM I50.9 be released?
The 2022 edition of ICD-10-CM I50.9 became effective on October 1, 2021.
What does a type 2 exclude note mean?
A type 2 excludes note represents "not included here". A type 2 excludes note indicates that the condition excluded is not part of the condition it is excluded from but a patient may have both conditions at the same time. When a type 2 excludes note appears under a code it is acceptable to use both the code ( I50.9) and the excluded code together.
What is the ICd 10 code for fluid overload?
There are many types of HF, and CHF is just one type. There is a code in ICD-10-CM for fluid overload: E87.70, Fluid over, unspecified. This is also where hypervolemia would be coded.
What is HF code assignment?
Euvolemic is a medical term that implies the patient appears to have normal circulatory or blood fluid volume. Hypervolemia or fluid overload is the medical condition where there is too much fluid in the blood, because not every patient is in fluid overload or hypervolemia at the time of admission, many physicians are now use HF (heart failure) versus congestive heart failure (CHF) in their documentation.
What is the medical term for a patient with too much fluid in their blood?
Hypervolemia or fluid overload is the medical condition where there is too much fluid in the blood, because not every patient is in fluid overload or hypervolemia at the time of admission, many physicians are now use HF (heart failure) versus congestive heart failure (CHF) in their documentation.
What is an acute exacerbation?
According to ICD-10-CM guidelines (I.C.10.a.1), an acute exacerbation is a worsening or a decompensation of a chronic condition. An acute exacerbation is not equivalent to an infection superimposed on a chronic condition, although an exacerbation may be triggered by an infection. Status asthmaticus is an acute exacerbation of asthma that remains unresponsive to initial treatment with bronchodilators.
Why is it important to review the ICD-10 code?
It’s important to review these issues with your physicians and other providers to ensure documentation in the medical record supports the more specific code assignment possibilities in ICD-10-CM. You must also understand the differences in verbiage in ICD-10-CM to assign the correct codes. Working in cooperation with your peers will allow you to piece together the ICD-10-CM puzzle.
What is an example of an asthmatic patient?
Example: An asthmatic patient presents for a check-up. The patient states that she uses her rescue inhaler daily; her asthma awakens her a few nights per week; and she has some limitations to normal activities. She has been coughing and running a fever. She is found to have pneumonia.
How often does a patient use a rescue inhaler?
Mild persistent: The patient is symptomatic more than two days per week; awakens at night three to four times per month; uses a rescue inhaler more than two days per week, but not daily; has minor limitation with normal activity; and has greater than 80 percent predicted lung function.
Is heart failure life threatening?
Acute heart failure is life threatening. Chronic heart failure happens slowly and is typically due to an underlying condition, such as hypertension or heart disease. Acute on chronic is seen when a patient has chronic heart failure and suffers an acute exacerbation.
Is heart failure a chronic disease?
Heart failure can also be acute, chronic, or acute on chronic. In this case, acute heart failure is heart failure that happens when there has been sudden damage to the heart—for example, due to an MI, thrombus in the heart, or severe infection. Acute heart failure is life threatening.
Is heart failure systolic or diastolic?
Heart failure can be systolic, diastolic, or combined systo lic and diastolic: When the left ventricle can’t contract enough, it’s systolic heart failure. When the left ventricle can’t fill with enough blood, it’s diastolic heart failure. Heart failure can also be acute, chronic, or acute on chronic.
What is the code for systolic heart failure?
These terms can be used to clarify the type of heart failure for code assignment. Systolic (congestive) heart failure being coded to I50.2; with Diastolic (congestive) heart failure coded to I50.3 and I50.4 for combined systolic/diastolic heart failure in ICD-10-CM.
When will there be new codes for heart failure?
Now, having said all of this, there will be new codes in 2018 for heart failure, including a code for right-sided failure.
What is left ventricular heart failure?
With left-sided heart failure or left ventricular (LV) heart failure, you may have either systolic and/or diastolic heart failure. Diastolic failure occurs when the muscle becomes stiff and loses its ability to relax normally. Documentation of heart failure with preserved EF (HFpEF), heart failure with preserved systolic function is also called ...
What is the term for the right ventricle failure?
When the right ventricle fails, we call it right-heart failure. In this case, fluid backs up into the peripheral circulation, into the legs, head, and the liver. Right-sided or right ventricular (RV) heart failure usually occurs as a result of left-sided failure.
What is the ICD-10 code for right sided heart failure?
Right-sided heart failure is coded in ICD-10-CM to the default code I50.9 heart failure, unspecified. This code is not affected by documentation of the acuity of the condition. The code maps to the MS-DRGs 291-293, Heart Failure and Shock.
Can heart failure be coded?
Before we can code heart failure, though, we need to review the medical record to determine the underlying cause. I would suggest querying the physician regarding whether the “right-heart failure” is due to an underlying pulmonary process or right failure related to left-sided failure (CHF—systolic versus diastolic).

Popular Posts:
- 1. icd 10 code 2019 for hammer toe
- 2. icd 10 code for didelphys
- 3. icd 10 code for long term use of oral hypoglycemics
- 4. icd 10 code for g tube feedings
- 5. icd 10 code for posterior cul de sac
- 6. icd-10 code for overinflation of left lingula
- 7. icd 10 code for abnormal ct of chest
- 8. icd 10 code for growth hormone deficiency
- 9. icd-10-pcs code for monitoring
- 10. what is the icd 10 code for hypoxia