What is the ICD 10 code for depression in remission?
2018/2019 ICD-10-CM Diagnosis Code F32.5. Major depressive disorder, single episode, in full remission. F32.5 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for alcohol dependence in remission?
Alcohol dependence, in remission. F10.21 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2020 edition of ICD-10-CM F10.21 became effective on October 1, 2019.
What is the ICD 10 code for attention deficit hyperactivity disorder?
Attention-deficit hyperactivity disorder, unspecified type. 2016 2017 2018 2019 Billable/Specific Code. F90.9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM F90.9 became effective on October 1, 2018.
What is the ICD 10 code for adjustment disorder with depressed mood?
Adjustment disorder with depressed mood 1 F43.21 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. 2 The 2019 edition of ICD-10-CM F43.21 became effective on October 1, 2018. 3 This is the American ICD-10-CM version of F43.21 - other international versions of ICD-10 F43.21 may differ.
What is ADHD in remission?
Results: Remission in ADHD should be defined as a loss of diagnostic status, minimal or no symptoms, and optimal functioning when individuals are being treated with or without medication. Symptomatic remission can be operationalized as a mean total score of S1 on most standardized questionnaires.
What is partial remission ADHD?
In partial remission: When full criteria were previously met, fewer than the full criteria have been met for the past 6 months, and the symptoms still result in impairment in social, academic, or occupational functioning.
What is the ICD-10 diagnosis code for ADHD disorder?
F90. 8, Attention-deficit hyperactivity disorder, other type. F90. 9, Attention-deficit hyperactivity disorder, unspecified type.
What does ADHD F90 mean?
ICD-10 code: F90.0. Attention-Deficit/Hyperactivity Disorder (ADHD) is a neurobehavioral disorder that usually first becomes apparent in childhood. Approximately 5% of adults in the U.S. have some form of ADHD.
Why is ADD no longer a diagnosis?
People sometimes use the term ADHD interchangeably with attention deficit disorder (ADD), to refer to ADHD without hyperactivity. However, the American Psychiatric Association (APA) only recognizes only ADHD. The Diagnostic and Statistical Manual of Mental Disorders (DSM-5) does not provide criteria for ADD.
What are the three types of ADHD differentiate one from the other?
Three major types of ADHD include the following:ADHD, combined type. This, the most common type of ADHD, is characterized by impulsive and hyperactive behaviors as well as inattention and distractibility.ADHD, impulsive/hyperactive type. ... ADHD, inattentive and distractible type.
What is the ICD-10 code for adult ADHD?
9 – Attention-Deficit Hyperactivity Disorder, Unspecified Type. ICD-Code F90. 9 is a billable ICD-10 code used for healthcare diagnosis reimbursement of Attention-Deficit Hyperactivity Disorder, Unspecified Type.
What is the ICD-10 code for ADHD without hyperactivity?
ICD-10 code: F98. 80 Attention deficit disorder without hyperactivity with onset usually occurring in childhood and adolescence.
What does diagnosis Z79 899 mean?
ICD-10 Code for Other long term (current) drug therapy- Z79. 899- Codify by AAPC. Factors influencing health status and contact with health services. Persons with potential health hazards related to family and personal history and certain conditions influencing health status.
Is R41 840 the same as ADHD?
In case ADHD is suspected but not yet diagnosed, symptoms such as attention and concentration deficit (R41. 840) should be reported. If signs and symptoms of ADHD are absent, screening for ADHD can be reported using code Z13. 4, encounter for screening for certain developmental disorders in childhood.
What does F43 23 mean?
ICD-Code F43. 23 is a billable ICD-10 code used for healthcare diagnosis reimbursement of Adjustment Disorder with Mixed Anxiety and Depressed Mood. Its corresponding ICD-9 code is 309.28.
What does F41 8 mean?
ICD-10 code: F41. 8 Other specified anxiety disorders.
What is the prognosis of ADHD?
Prognosis of Attention Deficit Hyperactivity Disorder (ADHD) There really is no cure for ADHD. Most children with this condition continue with its symptoms into adulthood. 80% of the children who require medication for ADHD will need them as teenagers. Over 50% need medication as adults.
Can you recover from ADHD?
While there is no cure for ADHD, individuals with ADHD can experience mental health recovery. For these individuals, recovery can best be understood as the ongoing management of ADHD symptoms.
What percent of children with ADHD will remit in adulthood?
It is estimated that childhood attention deficit hyperactivity disorder (ADHD) remits by adulthood in approximately 50% of cases; however, this conclusion is typically based on single endpoints, failing to consider longitudinal patterns of ADHD expression.
What is the frequency of ADHD?
The overall prevalence of current adult ADHD is 4.4%. Prevalence was higher for males (5.4%) versus females (3.2%). The non-Hispanic white group (5.4%) had a higher prevalence than all other race/ethnicity groups.
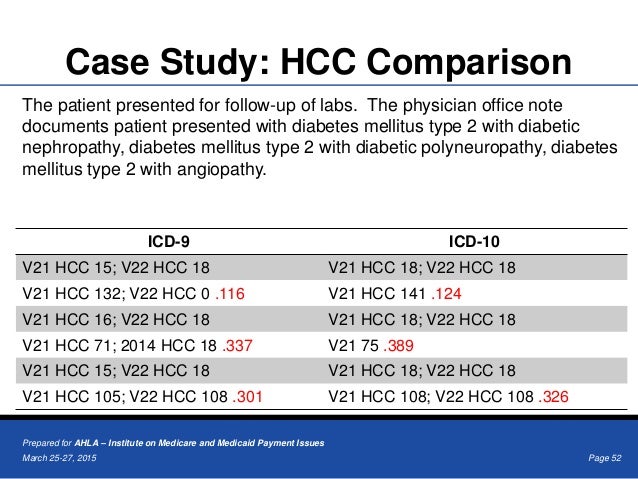
What is ADHD coding?
Attention-Deficit/Hyperactivity Disorder ( ADHD) is a chronic neurobehavioral disorder and often associated with serious areas of impairment and comorbidities over a life span. Physician practice coding professionals are at the forefront to ensure quality ICD-10-CM coded data across a life span for ADHD. In ICD-10-CM, ADHD coding over a life span requires clinical coding expertise across multi-physician specialties including but not limited to psychiatry, pediatrics, internal medicine, and family practice. This article summarizes how complete and accurate ADHD ICD-10-CM coding results in complete and quality coded data for the physician office provider setting.
What is the DSM-5 for ADHD?
In addition to the ADHD presentation, DSM-5 further classifies the ADHD severity of the present symptoms as “mild,” “moderate,” or “severe.”
How many visits does ADHD take?
The ADHD diagnosis is not established at the time of the initial physician office visit. Therefore, it may take two or more visits before the diagnosis is confirmed or ruled out. ICD-10-CM outpatient coding guidelines specify not to assign a diagnosis code when documented as “rule out,” “working diagnosis,” or other similar terms indicating uncertainty. Instead, the outpatient coding guidelines specify to code the condition (s) to the highest degree of certainty for that encounter/visit, which may require using symptoms, signs, or another reason for the visit.
What are the coexisting conditions of ADHD?
2 Across a life span, some coexisting conditions with ADHD include conduct disorder, depression, and anxiety, which may occur during both childhood and adulthood life stages.
What is ADHD evaluation?
ADHD is a clinical diagnosis based on symptomatology and evidence that the symptoms are interfering with social, academic, or occupational functioning. A comprehensive evaluation is required to diagnose ADHD and consists of a thorough diagnostic interview, information obtained from independent sources such as family members or teachers, diagnostic symptom checklists, standardized behavior rating scales for ADHD, and other types of clinical assessment testing as defined by the clinician.
Why was ADHD moved to the neurodevelopmental disorders chapter?
ADHD was moved to the neurodevelopmental disorders chapter to better reflect how brain development correlates with ADHD. Thus, with the introduction of DSM-5, ADHD is no longer classified as a childhood disorder but as a chronic lifelong disorder.
What is the best treatment for ADHD?
Effective treatment examples include long-term medication therapy, academic intervention, and cognitive behavioral therapy. Medication (stimulant and non-stimulant) often provides the first line of treatment for many individuals with ADHD, but not all.
How long does Adhd last?
Nearly everyone shows some of these behaviors at times, but adhd lasts more than 6 months and causes problems in school, at home and in social situations. Adhd is more common in boys than girls. It affects 3-5 percent of all american children.the main features of adhd are. inattention. hyperactivity.
What is a behavioral disorder?
A behavior disorder originating in childhood in which the essential features are signs of developmentally inappropriate inattention, impulsivity, and hyperactivity. Although most individuals have symptoms of both inattention and hyperactivity-impulsivity, one or the other pattern may be predominant. The disorder is more frequent in males ...
What is the age of inattention?
At home and at school). At least some of the symptoms must be present before the age of 7 years.
When will the ICD-10-CM F15.21 be released?
The 2022 edition of ICD-10-CM F15.21 became effective on October 1, 2021.
What are the synonyms for amphetamines?
Approximate Synonyms. Amphetamine dependence (moderate use disorder), in early remission. Amphetamine dependence (moderate use disorder), in sustained remission. Amphetamine dependence (severe use disorder), in early remission. Amphetamine dependence (severe use disorder), in sustained remission.
What is the ICd 10 code for attention deficit?
Attention and concentration deficit 1 R41.840 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. 2 The 2021 edition of ICD-10-CM R41.840 became effective on October 1, 2020. 3 This is the American ICD-10-CM version of R41.840 - other international versions of ICD-10 R41.840 may differ.
When will ICD-10 R41.840 be available?
The 2022 edition of ICD-10-CM R41.840 became effective on October 1, 2021.
How long does ADHD last?
The symptoms have lasted longer than six months, and they impair school, work, home life, or relationships in more than one setting. Clinical documentation requirements for ADHD. Clinical documentation must clearly differentiate ADHD from the following conditions: Hyperkinesia. Hyperkinetic syndrome.
How many symptoms are there for ADHD?
Combined: These individuals have symptoms of inattention, hyperactivity, and impulsivity. For a clinical diagnosis of ADHD, an individual must exhibit six or more symptoms of one of the types of ADHD and also meet each of the following three criteria: The symptoms caused problems before the age of 7.
How many children with ADHD receive psychological services?
Only 40-50 percent of young children with ADHD receive psychological services. Many parents resort immediately to stimulant or non-stimulant medication, which could have detrimental side effects. The CDC provides many resources for parents as well as clinical guidelines for providers.
What happens if you leave ADHD untreated?
Children with the condition may fall behind in school, have difficulty maintaining friendships, find themselves unable to accomplish basic tasks, or have conflicts with others.
What are the three types of ADHD?
It’s important for parents, providers, and teachers to be able to recognize the three types of ADHD: Inattentive: Individuals with this type of ADHD fail to pay close attention to details and make careless mistakes in schoolwork and other activities.
How to learn more about ADHD?
To learn more about ADHD, visit the CDC’s website as well as CHADD, the national resource on ADHD.
Is behavior therapy effective for ADHD?
It has been shown to be as effective as medicine, but without the risk of side effects.”. Unfortunately, the recommended first line of treatment for ADHD (i.e., behavior therapy) is often underused, according to the CDC. Only 40-50 percent of young children with ADHD receive psychological services.
Popular Posts:
- 1. identify the icd-10-cm code for ventricular diastolic dysfunction.
- 2. icd-10 code for pneumothorax traumatic
- 3. icd 10 code for skin tear left knee
- 4. icd 10 code for peritoneal dialysis
- 5. icd 10 code for ajovy injection
- 6. icd 10 code for chronic lymphocytic arm
- 7. icd-10 code for falling onto walker
- 8. icd-10-cm code for pharyngeal cancer that has spread to lymph nodes
- 9. icd 10 code for ductal carcinoma right breast
- 10. icd 9 code for spitting up infant