What is the ICD 10 code for stenosis?
Stenosis of other vascular prosthetic devices, implants and grafts, initial encounter. T82.858A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for stenosis of other vascular prosthesis?
Stenosis of other vascular prosthetic devices, implants and grafts, initial encounter 2016 2017 - Revised Code 2018 2019 2020 2021 Billable/Specific Code T82.858A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. Short description: Stenosis of other vascular prosth dev/grft, init
What is the ICD 10 code for vascular implants and grafts?
Presence of other vascular implants and grafts. Z95.828 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for vascular angioplasty?
Peripheral vascular angioplasty status with implants and grafts. Z95.820 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM Z95.820 became effective on October 1, 2018.
What is the ICD-10 code for occlusion of bypass graft?
Note: As of October 1, 1994, coronary artery bypass graft occlusions due to atherosclerosis are coded to 414.02 or 414.03.
What is the ICD-10 code for clotted AV graft?
T82.868AICD-10-CM Code for Thrombosis due to vascular prosthetic devices, implants and grafts, initial encounter T82. 868A.
What is the ICD-10 code for infected AV graft?
T82. 7XXA - Infection and inflammatory reaction due to other cardiac and vascular devices, implants and grafts [initial encounter] | ICD-10-CM.
What is a dialysis graft?
The dialysis machine is connected to your blood vessels using an access such as a fistula or graft. A graft is created by connecting a vein to an artery using tubing. Grafts are not used as often for dialysis access as fistula because they don't last as long and tend to have higher rates of infection.
What is the ICD 10 code for AVF malfunction?
ICD-10 code T82. 590A for Other mechanical complication of surgically created arteriovenous fistula, initial encounter is a medical classification as listed by WHO under the range - Injury, poisoning and certain other consequences of external causes .
What is the CPT code for percutaneous thrombectomy of forearm AV graft that was inserted for dialysis treatment?
36831 is for open thrombectomy of AV graft without graft revision.
What is the diagnosis for ICD-10 code r50 9?
9: Fever, unspecified.
What is the CPT code for removal of arteriovenous graft?
Vein Patch After Removal of AV Graft I reported code 35903 for removal of the infected graft.
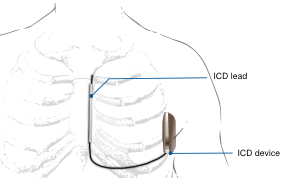
What is the ICD-10 code for AICD?
Z95.810ICD-10-CM code Z95. 810 is used to report the presence of an AICD without current complications.
Is AV fistula and AV graft the same?
AV fistula is considered the most preferred vascular access method for dialysis treatment. Although AV graft offers an alternative to fistula for patients with small or weak veins, it increases the risk of blood clotting, aneurysms and infections.
Is a graft the same as a fistula?
a fistula, which is made by joining together an artery and vein to make a bigger high-flow blood vessel. a graft, in which a soft plastic tube is placed between an artery and a vein, creating an artificial high-flow blood vessel.
What's the difference between AV fistula and grafts?
An AV graft requires the patient to take good care of the access point, as it might be prone to complications otherwise. The third option is the arteriovenous fistula, deemed the best option by most doctors. Rather than using a plastic tube, a fistula is created by connecting an artery directly to a vein.
What is a dialysis graft made of?
Most commonly used material for making AV fistula are polytetrafluorethylene, Dacron, silicon, and polyurethane. Polytetrafluoroethylene (PTFE) grafts are preferred over biological and other synthetic grafts due to low thrombosis risk, longer patency, ease of implantation, and low risk of disintegration with infection.
Why do you need AV graft for dialysis?
An AV fistula causes extra pressure and extra blood to flow into the vein, making it grow large and strong. The larger vein provides easy, reliable access to blood vessels. Without this kind of access, regular hemodialysis sessions would not be possible.
What is the purpose of an AV graft?
An arteriovenous or AV graft is made when the veins are not suitable for an AV fistula. The AV graft is a form of vascular access which is created by inserting a synthetic tube to connect a vein to an artery. Two dialysis needles are inserted into the AV graft on each hemodialysis treatment.
What is the most common cause of death in dialysis patients?
Patients with end-stage renal disease (ESRD) on long-term dialysis therapy have very high mortality due to predominantly cardiovascular causes1 (Figure 1). Sudden cardiac death (SCD) is the single most common form of death in dialysis patients, accounting for 20% to 30% of all deaths in this cohort.
Popular Posts:
- 1. icd 10 code for blood alcohol level of 60-79 mg/100 ml
- 2. icd 10 cm code for compression of the l1 vertebrae due to trauma
- 3. icd 9 code for abscess of breast during pregnancy
- 4. icd 10 code for ghtn
- 5. icd 10 code for personal history of lymph node cancer
- 6. icd 10 code for secondary neoplasm of lung
- 7. icd 10 code for right finger mcp joint pain and swelling
- 8. icd 10 code for vomiting in pregnancy
- 9. icd 10 code for muscle strain inguinal
- 10. icd 10 code for abnormal wbc count