What is diagnosis covers B12?
Covered Indications. Vitamin B 12 injection will be considered medically reasonable and necessary under the following circumstances: Vitamin B 12 administration by injection is a covered benefit accepted as medically necessary when the beneficiary has a history of a low serum B 12 or conditions causing or caused by a low serum B 12.
How do you Bill B12 injections?
“Body stores of vitamin B12 are in the region of two to three milligrams, which is sufficient to last for two to four years.” B12 injections are often used in the treatment of severe deficiencies, allowing the body to fully recover within the space of 12 months.
What is the CPT code for B12 injection?
Vitamin B-12 Injections / Vitamin Therapy
- Adachi S, Kawamoto T, Otsuka M, Fukao K. ...
- Albert CM, Cook NR, Gaziano JM, et al. ...
- Allos Therapeutics, Inc. ...
- Almeida OP, Ford AH, Flicker L. ...
- Andres E, Noel E, Kaltenbach G. ...
- Andres E, Vogel T, Federici L, et al. ...
- Auger RR, Burgess HJ, Emens JS, et al. ...
- Bajwa ZH, Ortega E. ...
- Balk E, Chung M, Raman G, et al. ...
- Balk EM, Raman G, Tatsioni A, et al. ...
What is the diagnosis code for vitamin B12 deficiency?
- ICD-10-CM Codes
- D50-D89 Diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism
- D50-D53 Nutritional anemias
- D51- Vitamin B12 deficiency anemia
- 2022 ICD-10-CM Diagnosis Code D51.9
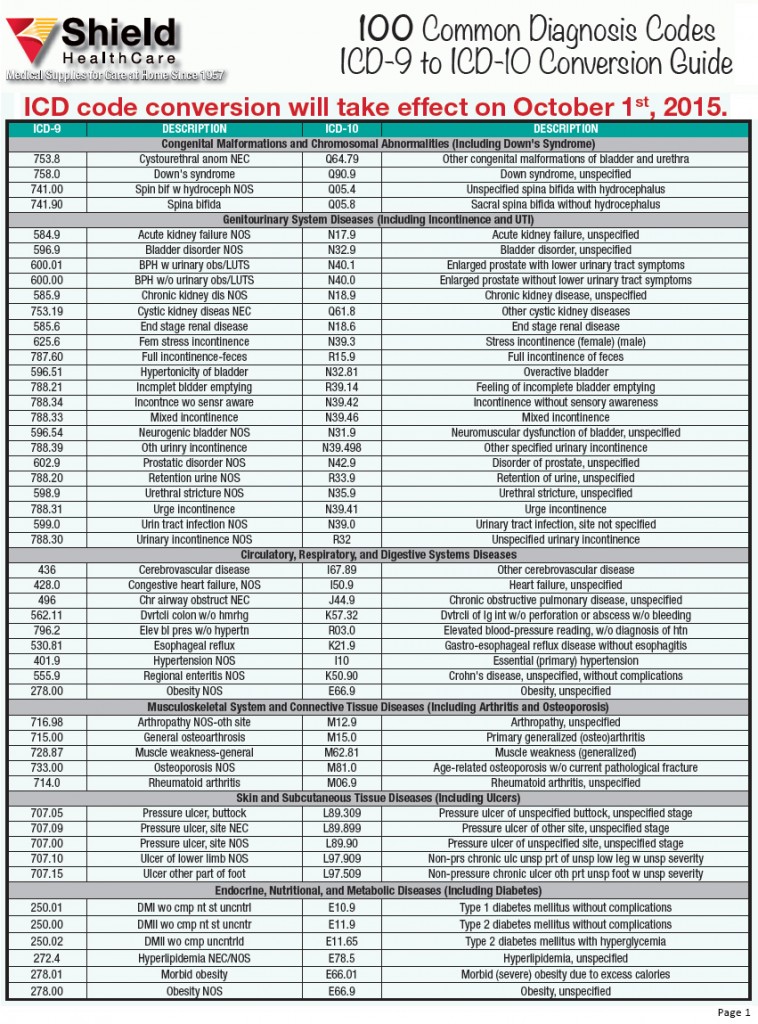
What ICD-10 codes cover B12?
Vitamin B12 deficiency anemia, unspecified D51. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM D51. 9 became effective on October 1, 2021.
What ICD-10 codes cover B12 and folate?
Vitamin B-12 (82607) and folate (82746) can be tested up to four times per year for malabsorption syndromes (K90. 9) or deficiency disorders (D81. 818, D81.
What diagnosis covers a B12 injection?
ICD-10-CM codes T50. 995A, T50. 995D, and T50. 995S apply to administration of Vitamin B12 as adjunct to Alimta®....Group 1.CodeDescriptionD51.8Other vitamin B12 deficiency anemiasD51.9Vitamin B12 deficiency anemia, unspecifiedD52.0Dietary folate deficiency anemiaD52.1Drug-induced folate deficiency anemia37 more rows
How do you bill B12 injections?
Coding a B12 injection Is 90782, “Therapeutic, prophylactic or diagnostic injection (specify material injected); subcutaneous or intramuscular,” the proper code for administering a vitamin B12 injection in the office if the patient provides the medication?
What is CPT code for vitamin B12?
CPT-4 code 82607 (cyanocobalamin [vitamin B-12]) is reimbursable only when billed in conjunction with one or more of the following ICD-10-CM codes.
Does Medicare cover B12 blood test?
The Centers for Medicare & Medicaid Services also do not provide coverage for routine testing for vitamin B12 deficiency. There is agreement within the literature that serum vitamin B12 testing should be used to diagnose vitamin B12 deficiency in symptomatic and high-risk populations.
What is the ICD 10 code for injection?
ICD-10 code T80 for Complications following infusion, transfusion and therapeutic injection is a medical classification as listed by WHO under the range - Injury, poisoning and certain other consequences of external causes .
Is B12 shots covered by insurance?
If you have been formally admitted into a hospital, reside in a skilled nursing facility, or hospice and your physician orders a B12 shot as medically necessary treatment, Part A (hospital insurance) may help cover the costs.
Is vitamin B12 test covered by insurance?
Insurance will usually cover the cost of vitamin B12 testing if your health care provider orders it to diagnose or monitor a medical condition. You can check with your doctor or nurse, the lab, or your health insurance company to learn more about what, if any, testing costs you are responsible for.
How do you code an injection?
CPT® code 96372: Injection of drug or substance under skin or into muscle.
What diagnosis code goes with 96372?
The Current Procedural Terminology (CPT®) code 96372 as maintained by American Medical Association, is a medical procedural code under the range - Therapeutic, Prophylactic, and Diagnostic Injections and Infusions (Excludes Chemotherapy and Other Highly Complex Drug or Highly Complex Biologic Agent Administration).
What is the CPT code for therapeutic injection?
The CPT code 96372 should be used–Therapeutic, prophylactic, or diagnostic injection.
What is vitamin B12 injection given for?
Vitamin B12 shots are injections that a doctor may prescribe to treat a vitamin B12 deficiency, especially if a person's body has difficulty absorbing the vitamin. A deficiency in vitamin B12 can lead to various health problems, ranging from fatigue to permanent neurological changes.
What do you have B12 injections for?
Vitamin B-12 is also added to some foods and is available as a dietary supplement. Vitamin B-12 injections are commonly prescribed to help prevent or treat pernicious anemia and B-12 deficiency.
What are you lacking if you need B12 injections?
Vitamin B12 deficiency anaemia is usually treated with injections of vitamin B12. There are 2 types of vitamin B12 injections: hydroxocobalamin.
What causes a vitamin B12 deficiency?
Some people can develop a vitamin B12 deficiency as a result of not getting enough vitamin B12 from their diet. A diet that includes meat, fish and dairy products usually provides enough vitamin B12, but people who do not regularly eat these foods can become deficient.
What is D50-D89?
D50-D89 Diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism
Is D51 a reimbursement code?
Vitamin B12 deficiency anemia. D51 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. The 2021 edition of ICD-10-CM D51 became effective on October 1, 2020.
What is the name of the condition where the body cannot absorb B12?
A type of anemia (low red blood cell count) caused by the body's inability to absorb vitamin b12. Anemia due to poor intestinal absorption of vitamin b12 caused by defective production of intrinsic factor (a carrier protein) by the gastric mucosa. Megaloblastic anemia caused by vitamin b-12 deficiency due to impaired absorption.
What is B20 in medical terms?
human immunodeficiency virus [HIV] disease ( B20) injury, poisoning and certain other consequences of external causes ( S00-T88) neoplasms ( C00-D49) symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified ( R00 - R94) Diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism.
What is the cause of megaloblastic anemia?
Megaloblastic anemia caused by vitamin b-12 deficiency due to impaired absorption. The impaired absorption of vitamin b-12 is secondary to atrophic gastritis and loss of gastric parietal cells.
When will the ICd 10 D51.0 be released?
The 2022 edition of ICD-10-CM D51.0 became effective on October 1, 2021.
What is the synonym for anemia?
Approximate Synonyms. Anemia, pernicious. Pernicious anemia. Clinical Information. A decrease in red blood cells that occurs when the body cannot absorb vitamin b12. A megaloblastic anemia occurring in children but more commonly in later life, characterized by histamine-fast achlorhydria, in which the laboratory and clinical manifestations are ...
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
Article Guidance
This First Coast Billing and Coding Article for Local Coverage Determination (LCD) L33967 Vitamin B 12 Injections provides billing and coding guidance for frequency limitations as well as diagnosis limitations that support diagnosis to procedure code automated denials.
ICD-10-CM Codes that Support Medical Necessity
The following ICD-10-CM codes support medical necessity and provide limited coverage for CPT code: J3420
ICD-10-CM Codes that DO NOT Support Medical Necessity
All those not listed under the “ICD-10 Codes that Support Medical Necessity” section of this article.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
Document Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
This LCD supplements but does not replace, modify or supersede existing Medicare applicable National Coverage Determinations (NCDs) or payment policy rules and regulations for Vitamin B 12 Injections. Federal statute and subsequent Medicare regulations regarding provision and payment for medical services are lengthy.
Coverage Guidance
Compliance with the provisions in this LCD may be monitored and addressed through post payment data analysis and subsequent medical review audits.

Popular Posts:
- 1. icd 10 code for exposure to influ
- 2. icd 10 cm code for outer ear infection right
- 3. icd 10 code for hcg blood test
- 4. icd 10 code for acute dehydration
- 5. icd 10 code for open wounds on legs
- 6. icd 10 code for leg spasm
- 7. icd 10 code for hepatitis a positive
- 8. icd 10 code for ankle sprain left
- 9. icd 10 code for gait deficit
- 10. icd-10-pcs code book updates for 2020