The ablation procedure is directed at the pathway for electrical impulses rather the muscular wall of the heart itself. The atrium is not being destroyed. This procedure can be reported with the following ICD-10-PCS codes: 02580ZZ, Destruction of conduction mechanism, open approach; 02583ZZ, Destruction of conduction mechanism, percutaneous ...
Full Answer
What is the diagnosis code for cardiac arrest?
adjustment or management of cardiac device ( Z45.0-) adjustment or management of cardiac pacemaker ( Z45.0) presence of automatic (implantable) cardiac defibrillator with synchronous cardiac pacemaker ( Z95.810) ICD-10-CM Diagnosis Code I49.9 [convert to ICD-9-CM] Cardiac arrhythmia, unspecified.
What is the CPT code for cardiac ablation?
Dec 03, 2020 · CODES . ICD-10-CM. 1 . Diagnosis Codes that May Support Cardiac Catheter Ablation Procedures . The following is a list of diagnosis codes that may be associated with VT, SVT, and PVI ablation procedures. The list is for illustrative purposes only.
How many codes in ICD 10?
ICD-10-CM Diagnosis Code I97.190 Other postprocedural cardiac functional disturbances following cardiac surgery 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code
What does ICD stand for in cardiac in medical category?
Cardiac ICD-10-PCS Procedure Code 5A02 Cardiac ICD-10-PCS Procedure Code 5A12 Cardiac ICD-10-PCS Procedure Code 5A22 Cardiac ICD-10-CM Diagnosis Code T82.598A [convert to ICD-9-CM] Other mechanical complication of other cardiac …
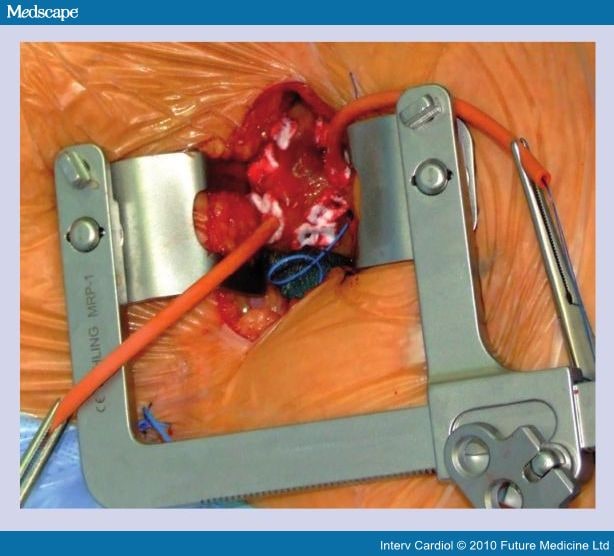
What is catheter ablation?
Catheter ablation is a therapeutic technique using a tripolar electrode catheter to eliminate conduction defects, which cause tachycardia. This technique involves a high level of current, which is channeled through a catheter to destroy the arrhythmic area of the heart. It treats supraventricular tachycardia by ablating or modulating the atrio-ventricular (AV) node or ablating accessory conduction pathways; it treats ventricular tachycardia by ablating the arrhythmogenic focus (as an alternative to open heart surgical techniques). Catheter ablation is an acceptable alternative to long-term drug therapy. The role of catheter ablation as primary therapy for several arrhythmias has been described in position papers or technology assessments by the American Medical Association, the American College of Cardiology, and the North American Society of Pacing and Electrophysiology.
How long does it take to follow up after index ablation?
The follow-up duration is 12 months. The primary end-point is the rate of documented atrial tachycardia arrhythmias of greater than 30 seconds, without any anti-arrhythmic drugs, in 12 months after the index ablation procedure (excluding a blanking period of 3 months).
Can EI-VOM be used for PMF?
Takigawa and colleagues (2020) hypothesized that an epicardial approach using EI-VOM may improve the result of ablation for peri-mitral flutter (PMF). These researchers studied 103 consecutive patients with PMF undergoing high-resolution mapping. The first 71 were treated with RFA alone (RF-group), and the next 32 underwent EI-VOM followed by RFA on the endocardial and epicardial mitral isthmus (EI-VOM/RF-group). Contact force was not measured during ablation; acute and 1-year outcomes were compared. Flutter termination rates were similar between the RF-group (63/71, 88.7 %) and EI-VOM/RF-group (31/32, 96.8 %, p = 0.27). Atrial tachycardia (AT) terminated with EI-VOM alone in 22/32 (68.6 %) in the EI-VOM/RF-group. Bi-directional block of mitral isthmus was always achieved in the EI-VOM/RF-group, but significantly less frequently achieved in the RF-group (62/71, 87.3 %; p = 0.05). Median RF duration for AT termination/conversion was shorter [0 s (0 to 6) in the EI-VOM/RF-group than 312 s (55 to 610) in the RF-group, p < 0.0001], as well as for mitral isthmus block in the EI-VOM/RF-group [246 s (0 to 663)] than in the RF-group [900 s (525 to 1,310), p < 0.0001]. Pericardial effusion was observed in 1/32 (3.2 %) in EI-VOM/RF-group and 5/71 (7.0 %) in RF-group (p = 0.66); 2 in RF-group required drainage and 1 of them developed subsequent ischemic stroke. One-year follow-up showed fewer recurrences in the EI-VOM/RF-group [6/32 (18.8 %)] than in the RF-group [29/71 (40.8 %), p = 0.04]. By multi-variate analysis, only EI-VOM was significantly associated with less AT recurrence (HR = 0.35, p = 0.018). The authors concluded that EI-VOM may reduce RF duration needed for PMF termination as well as for mitral isthmus block without severe complications, and the mid-term outcome may be improved by this approach. This was a relatively small study (n = 32 in the EI-VOM/RF-group) with mid-term results. These preliminary findings need to be validated by well-designed studies with larger sample size and long-term follow-up.
What is RA in medical terms?
Krug and associates (2020) noted that single-session cardiac stereotactic body radiotherapy, called cardiac radiosurgery (CRS) or radioablation (RA), may offer a potential therapeutic option for patients with refractory VT and electrical storm who are otherwise ineligible for catheter ablation.
What is a STSF catheter?
Gonna and associates (2017) stated that the Biosense Webster ThermoCool SmartTouch Surround Flow (STSF) catheter (STSFc) is a recently developed ablation catheter incorporating Surround Flow (SF) technology to ensure efficient cooling and force sensing to quantify tissue contact. In the authors’ unit, it superseded the ThermoCool SF catheter (STc) from the time of its introduction in May 2015. Procedure-related data were collected prospectively for the first 100 ablation procedures carried out in the authors’ department using the STSFc. From a data-base of 654 procedures performed in the authors’ unit using the SF catheter, these investigators selected one to match each STSF procedure, matching for procedure type, operator experience, patient age, and gender. The groups were well-matched for patient age, gender, and procedure type. Procedure duration was similar in both groups (mean of 225.5 versus 221.4 mins, inter-quartile range [IQR] 106.5 versus 91.5, p = 0.55), but fluoroscopy duration was shorter in the STSF group (mean of 25.8 versus 30.0, IQR 19.6 versus 18.5, p = 0.03). No complication occurred in the STSF group. Complications occurred in 2 cases in the SF group (1 peri-cardial effusion requiring drainage and 1 need for permanent pacing). Complete procedural success was achieved in 98 cases in the STSF group and 94 cases in the SF group (p = 0.15). The composite end-point of procedure failure or acute complication was less common in the STSF group (2 versus 8, p = 0.05). The authors concluded that the STSFc was safe and effective in treating a range of arrhythmias. Compared with the SF catheter, it showed a trend towards improved safety-efficacy balance.
What is asymptomatic pre-excitation?
Asymptomatic members with ventricular pre-excitation whose livelihood or profession, important activities, insurability, or mental well being or the public safety would be affected by spontaneous tachyarrhythmias or the presence of the electrocardiographic abnormality; or
What is VOM in dogs?
Valderrabano et al (2009a) noted that vein of Marshall (VOM) is an attractive target during ablation of atrial fibrillation (AF) due to its autonomic innervation, its location anterior to the left pulmonary veins and drainage in the coronary sinus. These researchers studied 17 dogs. A coronary sinus venogram showed a VOM in 13, which was successfully cannulated with an angioplasty wire and balloon. In 5 dogs, electro-anatomical maps of the left atrium were performed at baseline and after ethanol infusion in the VOM, which demonstrated a new crescent-shaped scar, extending from the annular left atrium towards the posterior wall and left pulmonary veins. In 4 other dogs, effective refractory periods (ERP) were measured at 3 sites in the left atrium, before and after high-frequency bilateral vagal stimulation. The ERP decreased from 113.6 +/- 35.0 ms to 82.2 +/- 25.4 ms (p < 0.05) after vagal stimulation. After VOM ethanol infusion, vagally-mediated ERP decrease was eliminated (from 108.6 +/- 24.1 ms to 96.4 +/- 16.9 ms, p = NS). The abolition of vagal effects was limited to sites near the VOM (ERP: 104 +/- 14 ms, versus 98.6 +/- 12.2 ms post-vagal stimulation, p = ns), as opposed to sites remote to VOM (ERP: 107.2 +/- 14.9 ms, versus 78.6 +/- 14.7ms post-vagal stimulation, p < 0.05). To test feasibility in humans, 5 patients undergoing pulmonary vein antral isolation had successful VOM cannulation and ethanol infusion: left atrial voltage maps demonstrated new scar involving the infero-posterior left atrial wall extending towards the left pulmonary veins. The authors concluded that ethanol infusion in then VOM achieved significant left atrial tissue ablation, abolished local vagal responses and was feasible in humans.
Popular Posts:
- 1. icd 10 code for axillary sebaceous cyst
- 2. icd 10 code for lumbar spine instability
- 3. each icd-10-pcs code for whole body musculoskeletal pt, therapeutic exercise
- 4. icd 10 cm code for epidermoid cyst)
- 5. icd-10 code for kidney injury
- 6. icd 10 code for abnormal uterine bleeding in pregnancy
- 7. icd 9 cpt code for right ring finger bourchards noe
- 8. icd 10 code for personal history surgery left shoulder
- 9. icd 10 code for right calcaneus fracture
- 10. icd 10 code for lowerabdominal pain unspecified