What is the ICD 10 code for sacral ulcer?
ICD-10-CM Code L89.153 Pressure ulcer of sacral region, stage 3 Billable Code L89.153 is a valid billable ICD-10 diagnosis code for Pressure ulcer of sacral region, stage 3. It is found in the 2021 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2020 - Sep 30, 2021.
What is the ICD 10 code for cellulitis?
Cellulitis of other sites. L03.818 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM L03.818 became effective on October 1, 2018. This is the American ICD-10-CM version of L03.818 - other international versions of ICD-10 L03.818 may differ.
What is the ICD 10 code for lumbar radiculopathy?
L03.818 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for warts?
L03.818 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L03.818 became effective on October 1, 2021. This is the American ICD-10-CM version of L03.818 - other international versions of ICD-10 L03.818 may differ. viral warts ( B07.-) viral warts ( B07.-)
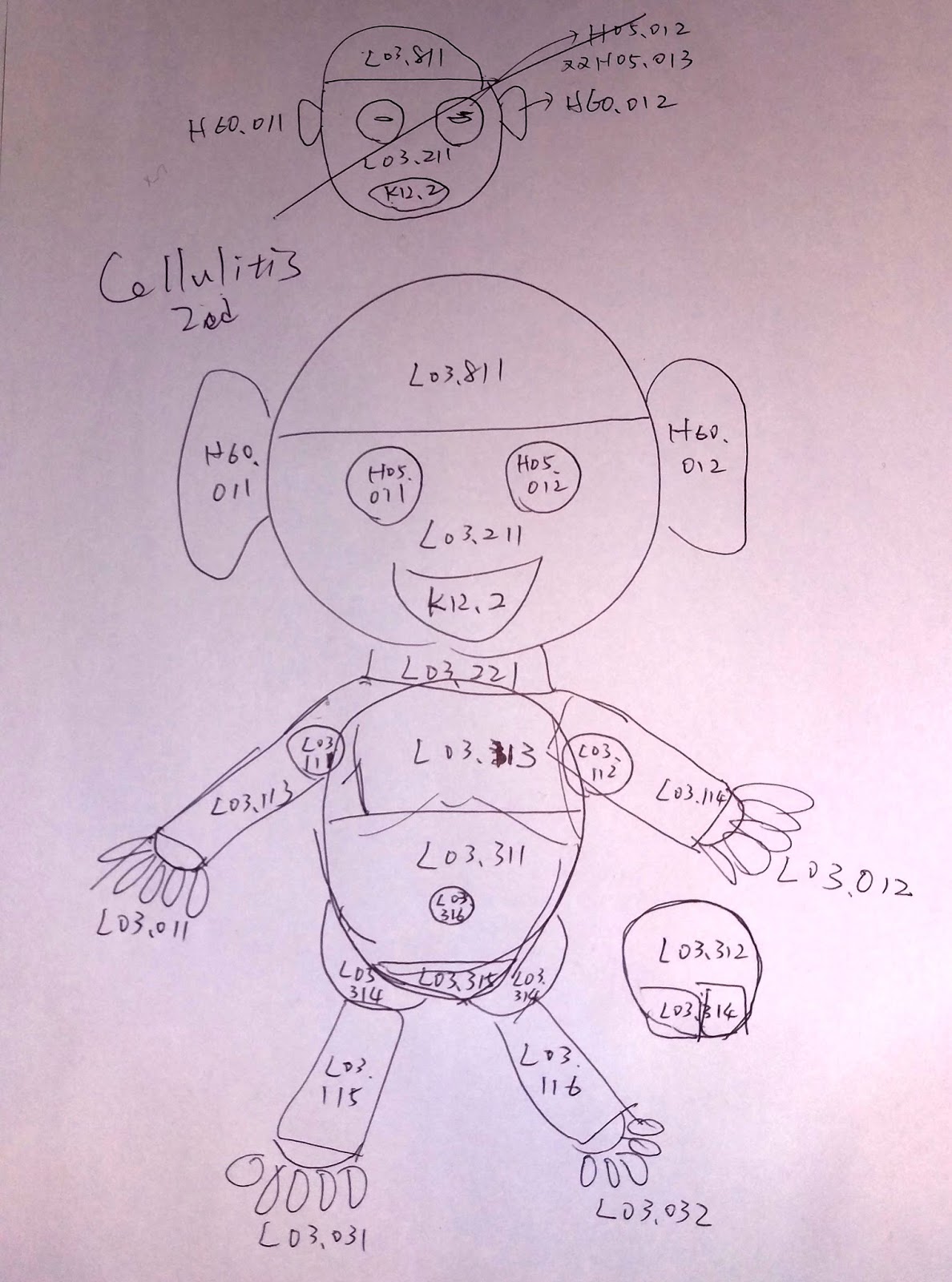
What is the ICD 10 code for Cellulitis of buttock?
ICD-10-CM Code for Cellulitis of buttock L03. 317.
What is the ICD 10 code for infected sacral wound?
ICD-10-CM Code for Pressure ulcer of sacral region, unspecified stage L89. 159.
What is the ICD 10 code for Cellulitis of lower extremity?
ICD-10 code L03. 116 for Cellulitis of left lower limb is a medical classification as listed by WHO under the range - Diseases of the skin and subcutaneous tissue .
What is the ICD 10 code for Cellulitis unspecified?
L03. 90 - Cellulitis, unspecified | ICD-10-CM.
What is the ICD-10 Code for wound infection?
L08. 9 - Local infection of the skin and subcutaneous tissue, unspecified. ICD-10-CM.
What is Pressure ulcer of sacral region?
Sacral ulcers are skin injuries that occur in the sacral region of the body, near the lower back and spine. These ulcers fall under the umbrella of pressure sores, which are more commonly referred to as bedsores.
What is the ICD-10 code for Cellulitis bilateral lower extremities?
119.
What is the diagnosis code for Cellulitis lower limb right lower?
115 Cellulitis of right lower limb.
What are the coding guidelines for Cellulitis?
L03.311 – Cellulitis of abdominal wall.L03.312 – Cellulitis of back [any part except buttock]L03.313 – Cellulitis of chest wall.L03.314 – Cellulitis of groin.L03.315 – Cellulitis of perineum.L03.316 – Cellulitis of umbilicus.L03.317 – Cellulitis of buttock.L03.319 – Cellulitis of buttock, unspecified.
What is the ICD-10 code for sepsis due to Cellulitis?
ICD-10-CM, as it does in ICD-9-CM. Septic shock is combined into code R65. 21. Example: A patient is admitted with cellulitis and abscess of the left leg, severe sepsis, septic shock, and acute renal failure and encephalopathy due to the sepsis.
What do you do for Cellulitis?
Place a cool, damp cloth on the affected area as often as needed for your comfort. Ask your health care provider to suggest a nonprescription pain medication. Elevate the affected part of the body. Ask your health care provider whether it might help to wear compression wraps or stockings.
Why does Cellulitis occur?
Cellulitis is caused when bacteria, most commonly streptococcus and staphylococcus, enter through a crack or break in the skin. The incidence of a more serious staphylococcus infection called methicillin-resistant Staphylococcus aureus (MRSA) is increasing.
What is the ICD-10 code for infected decubitus ulcer?
Pressure ulcer of unspecified site, unspecified stage The 2022 edition of ICD-10-CM L89. 90 became effective on October 1, 2021.
What is L89 154?
ICD-10 code L89. 154 for Pressure ulcer of sacral region, stage 4 is a medical classification as listed by WHO under the range - Diseases of the skin and subcutaneous tissue .
What is the ICD-10 code for sacrum Stage 3?
153.
What is the ICD-10 code for sepsis?
Septicemia – There is NO code for septicemia in ICD-10. Instead, you're directed to a combination 'A' code for sepsis to indicate the underlying infection, such A41. 9 (Sepsis, unspecified organism) for septicemia with no further detail.
What is the ICd 10 code for cellulitis?
L03.90 is a valid billable ICD-10 diagnosis code for Cellulitis, unspecified . It is found in the 2021 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2020 - Sep 30, 2021 .
Do you include decimal points in ICD-10?
DO NOT include the decimal point when electronically filing claims as it may be rejected. Some clearinghouses may remove it for you but to avoid having a rejected claim due to an invalid ICD-10 code, do not include the decimal point when submitting claims electronically. See also:
What is the ICd 10 code for pressure ulcer of sacral region?
L89.153 is a valid billable ICD-10 diagnosis code for Pressure ulcer of sacral region, stage 3 . It is found in the 2021 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2020 - Sep 30, 2021 .
Do you include decimal points in ICD-10?
DO NOT include the decimal point when electronically filing claims as it may be rejected. Some clearinghouses may remove it for you but to avoid having a rejected claim due to an invalid ICD-10 code, do not include the decimal point when submitting claims electronically.
What is the ICD code for pressure ulcer of sacral region?
L89.152 is a billable ICD code used to specify a diagnosis of pressure ulcer of sacral region, stage 2. A 'billable code' is detailed enough to be used to specify a medical diagnosis.
What is the ICd 9 code for a cranial ulcer?
Specialty: Plastic Surgery. MeSH Code: D003668. ICD 9 Code: 707.0. Classification of ulcers.
What is the ICD10 code for L89.152?
This means that while there is no exact mapping between this ICD10 code L89.152 and a single ICD9 code, 707.22 is an approximate match for comparison and conversion purposes.
What is the ICD-10 code for cellulitis?
Rationale:Documentation supports that cellulitis is the first listed diagnosis. Review of the Tabular shows that ICD-10-CM classifies the laterality of cellulitis of the lower extremity, with L03.115 being the right lower extremity. A note appears in the Tabular under the section Infections of the Skin and Subcutaneous Tissue (L00-L08) instructing to use an additional code (B95-B97) to identify infectious agent. ICD-10-CM also classifies decubitus ulcers of the buttocks both by stage and laterality. Gluteus is not listed in the classification, but it refers to the buttock region.
What is the ICd 10 code for Crohn's disease?
K50.012 Crohn’s disease –see Enteritis, regional, Enteritis (acute) (diarrheal) (hemorrhagic) (noninfective) (septic), regional (of), small intestine, with complication, intestinal obstruction Rationale:An additional code for the small bowel obstruction is not required as the combination code in ICD-10-CM identifies both the Crohn’s disease and the small bowel obstruction. Exacerbation is not a qualifier for Crohn’s disease.
What is the index for dermatitis?
This was documented as irritant contact dermatitis, but not allergic, so Index contact, irritant, due to cosmetics, L24.3. Under contact, allergic, due to cosmetics there is a different code L23.2, if documentation supported that code.
What is the instructional note code for a drug?
An instructional note appears in the Tabular, under codes L27.0 and L27.1, stating to use additional code for adverse effect, if applicable, to identify drug (T36-T50 with fifth or sixth character 5).
What stage is oSite, laterality, and severity specified in single code oSeverity identified as?
oSite, laterality, and severity specified in single code oSeverity identified as stage 1–4
How are gastric ulcers subdivided?
Rationale: Gastric ulcers are subdivided by severity and then further subdivided by hemorrhage and/or perforation.
Is cellulitis a gangrene or an abscess?
Rationale: In ICD-10-CM, there are individual categories for abscess (L02) and cellulitis (L03). In ICD-9-CM, these were combined. Note in the Index that abscess of the toe classifies to abscess of the foot, while abscess of the toe nail, classifies to cellulitis, toe. There are no “includes” or “excludes” notes that preclude the use of the abscess and gangrene code together, nor is there any sequencing guideline available.

Popular Posts:
- 1. icd 10 code for volume overload due to missed dialysis
- 2. icd 9 code for chronic headache
- 3. icd 10 code for tubulovillous adenoma of sigmoid colon
- 4. icd 10 code for injury occurring while playing handball during gym class
- 5. icd 10 cm code for retroperitoneal mass
- 6. icd 10 code for septic shock with acute kidney injury
- 7. aftercare code for incision care icd 10
- 8. icd 10 code for status post cabg x 4
- 9. icd 10 code for healed gastric ulcer
- 10. icd 9 code for z79.4