What is the ICD 10 code for Neurologic diagnosis?
S06.330A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM S06.330A became effective on October 1, 2020. This is the American ICD-10-CM version of S06.330A - other international versions of ICD-10 S06.330A may differ.
What is the ICD 10 code for diagnosis?
2022 ICD-10-CM Diagnosis Code S06.330A S06.330A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM S06.330A became effective on October 1, 2021. This is the American ICD-10-CM version of S06.330A - other international versions of ICD-10 S06.330A may differ.
What is the ICD 10 code for Senile degeneration of brain?
Senile degeneration of brain, not elsewhere classified 2016 2017 2018 2019 2020 2021 Billable/Specific Code G31.1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM G31.1 became effective on October 1, 2020.
What are the ICD 10 codes for brain disorders?
Other specified disorders of brain. Ependymopathy G93.89 ICD-10-CM Diagnosis Code J96.90 Fistula (cutaneous) L98.8 ICD-10-CM Diagnosis Code L98.8 Gliosis (cerebral) G93.89 Paralysis, paralytic (complete) (incomplete) G83.9 ICD-10-CM Diagnosis Code G83.9 ICD-10-CM Diagnosis Code R06.81 Pneumatocele (lung)...
What is ICD-10 code for parenchymal volume loss?
9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM E86. 9 became effective on October 1, 2021. This is the American ICD-10-CM version of E86.
What is cerebral volume loss?
What is brain atrophy? People with brain atrophy, also called cerebral atrophy, lose brain cells (neurons), and connections between their brain cells and brain volume often decreases. This loss can lead to problems with thinking, memory and performing everyday tasks.
What is the ICD-10 code for cerebral atrophy?
2022 ICD-10-CM Diagnosis Code G31. 1: Senile degeneration of brain, not elsewhere classified.
What is diagnosis code R90 89?
ICD-10 code R90. 89 for Other abnormal findings on diagnostic imaging of central nervous system is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
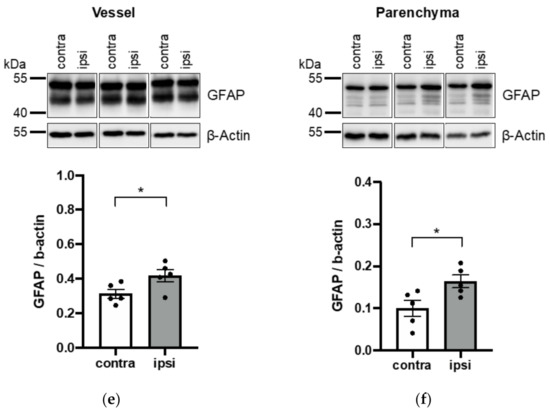
What is brain parenchymal volume?
The brain parenchymal fraction, defined as the ratio of brain parenchymal volume to the total volume within the brain surface contour, was used to measure whole brain atrophy. The relationship between disease features and brain atrophy and effect of interferon beta-1a were determined.
What is cerebral parenchyma?
The brain parenchyma is the functional tissue in the brain. It's comprised of two types of cells that are used specifically for cognition and controlling the rest of the body. The remaining brain tissue is known as stroma, which is the supportive or structural tissue.
What is parenchymal volume loss?
Cerebral atrophy is the morphological presentation of brain parenchymal volume loss that is frequently seen on cross-sectional imaging. Rather than being a primary diagnosis, it is the common endpoint for a range of disease processes that affect the central nervous system.
What is the ICD-10 code for CVA?
I63. 9 - Cerebral infarction, unspecified | ICD-10-CM.
What is the ICD-10 code for white matter changes?
ICD-10 code R90. 82 for White matter disease, unspecified is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
Is the brain part of the central nervous system?
The central nervous system (CNS) is made up of the brain and spinal cord. It is one of 2 parts of the nervous system. The other part is the peripheral nervous system, which consists of nerves that connect the brain and spinal cord to the rest of the body.
What is the ICD-10 code for brain MRI?
The matching ICD-10-PCS code is B030ZZZ, Magnetic Resonance Imaging (MRI) of Brain.
What is the ICD-10 code for dizziness?
ICD-10 Code: R42 – Dizziness and Giddiness.
What causes cerebral volume loss?
Diseases that cause cerebral atrophy include: stroke and traumatic brain injury. Alzheimer's disease, Pick's disease, and fronto-temporal dementia. cerebral palsy, in which lesions (damaged areas) may impair motor coordination.
What is cerebral and cerebellar volume loss?
Cerebral volume loss and cerebellar volume loss (i.e., atrophy) are usually apparent on imaging because of the prominence of the subarachnoid spaces (SASs) with associated widening of the sulci, along with mild, progressive enlargement of the ventricles, particularly the lateral ventricles.
How long can you live with cerebral atrophy?
Life expectancy among patients with brain atrophy can be influenced by the condition that caused the brain shrinkage. People with Alzheimer's disease live an average of four to eight years after their diagnosis.
Can cerebral atrophy cause death?
Cerebral atrophy occurs naturally in all humans. But cell loss can be accelerated by a variety of causes, including injury, infection, and medical conditions such as dementia, stroke, and Huntington's disease. These latter cases sometimes culminate in more severe brain damage and are potentially life-threatening.
What is progressive nervous system dysfunction?
Hereditary and sporadic conditions which are characterized by progressive nervous system dysfunction. These disorders are often associated with atrophy of the affected central or peripheral nervous system structures. Neurologic disorders characterized by progressive nervous system dysfunction and loss of neural tissue.
What is cerebral atrophy?
Degenerative brain disorder. Paraneoplastic cerebellar degeneration. Clinical Information. A disorder of the central nervous system characterized by gradual and progressive loss of neural tissue and neurologic function.
What causes cerebral edema?
Conditions that cause cerebral edema include traumatic brain injuries, ischemic and hemorrhagic strokes, brain tumors, infection, altitude sickness, electrolyte derangements, and toxins. However, the development of cerebral edema isn’t invariable; for instance, not all brain tumors have surrounding vasogenic edema.
Can a coder code exclusively from a radiology report?
The coder is not permitted to code exclusively from a radiology report.
Can cerebral edema be woven into notes?
Have cerebral edema be woven into the notes repeatedly, not just once in a single note. They should link the treatment and monitoring with the condition (e.g., “will start on Decadron for the cerebral edema and get repeat MRI in two weeks.”). It should also be present in the discharge summary.
Is decompressive surgery urgent?
The patient is undergoing an urgent decompressive surgery – and maybe it wouldn’t have been as urgent if the cerebral edema hadn’t been present. It is easier to identify when the treatment is Decadron or mannitol, because those are specifically targeted for edema.
Is traumatic cerebral edema a MCC?
If there is any loss of consciousness, in addition to those two diagnoses, there are 337 traumatic conditions, which exclude traumatic cerebral edema as a MCC. These conditions include facial and skull fractures and other types of injuries, traumatic brain injuries and hemorrhages, suicide attempts, and traumatic compartment syndromes.
Can a patient have non-traumatic cerebral edema?
It often magnifies or complicates the clinical features of the primary underlying condition. The only Excludes 1 instructions are that a patient can’t have non- traumatic and traumatic cerebral edema concomitantly.
Is cerebral edema a valid diagnosis?
It is easier to fix it on the front end than to rework it on the basis of a clinical validation denial. Cerebral edema is a legitimate, valid, important diagnosis. Get it documented in a codable format and code it.
Popular Posts:
- 1. icd 10 code for left lower skin tear leg
- 2. icd 10 code for right side neck nodule
- 3. icd 10 code for manic exacerbation
- 4. icd 10 code for pedestrian hit by pickup truck
- 5. icd 10 code for comminuted displaced neck humeral fracture left side
- 6. icd 10 code for burn of unspecified degree of arm
- 7. icd 9 code for tonsils hypertrophy
- 8. icd 10 code for mixed hearing loss bilateral
- 9. what is the icd 10 code for increased blood sugar
- 10. icd 10 code for closed head injury