What is the diagnosis code for body aches?
- Able to cope
- Able to cope with pain
- Aching pain
- Acute pain
- Alimentary tract pain due to vascular insufficiency
- Alteration in comfort: chronic pain
- Alteration in comfort: pain
- Application site pain
- Burning pain
- Catch
What does it mean when your whole body aches?
Muscle pain that affects a small part of your body is usually caused by overuse -- sore arms from lifting boxes all day, for example. Or it could be a minor injury, like a bruised shoulder after a fall. But when you ache all over your body, it’s more likely caused by an infection, illness, or medicine you’ve taken.
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
What is ICD 10 code for severe persistent asthma?
Severe persistent asthma, uncomplicated. J45.50 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM J45.50 became effective on October 1, 2021.
What is the diagnosis code for chronic pain?
ICD-10 code G89. 4 for Chronic pain syndrome is a medical classification as listed by WHO under the range - Diseases of the nervous system .
What does R52 mean?
Pain, unspecified (R52)
What is the ICD-10 code for acute on chronic pain?
The ICD-10-CM guidelines also state you can assign the G89 codes in conjunction with codes from other categories and chapters to provide more detail about acute or chronic pain or neoplasm-related pain. For example, you can assign a G89 code to indicate that the pain is acute or chronic.
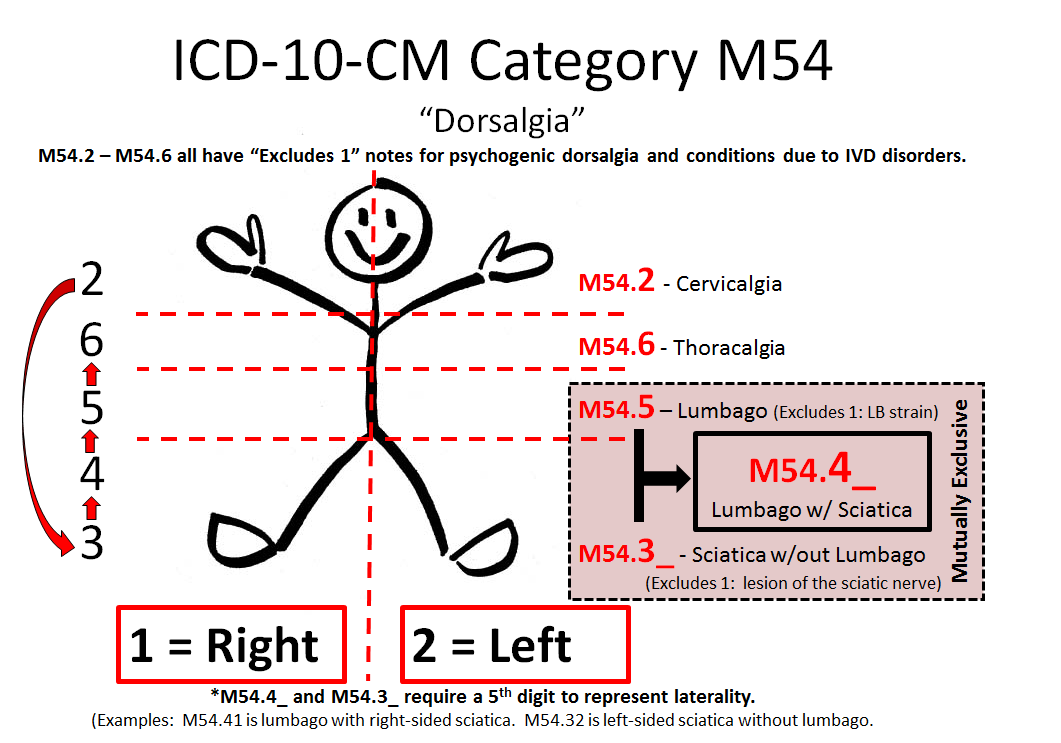
What is the ICD-10 for chronic back pain?
ICD-10 Code M54. 5 for Chronic Low Back Pain | CareCloud.
How do you code chronic low back pain?
ICD-10 code M54. 5, low back pain, effective October 1, 2021.
What is the ICD 10 code for joint pain?
Code M25. 50 is the diagnosis code used for Pain in the Unspecified Joint. It falls under the category of Diseases of the musculoskeletal system and connective tissue.
What is time frame defining when pain becomes chronic?
Chronic pain is pain that is ongoing and usually lasts longer than six months. This type of pain can continue even after the injury or illness that caused it has healed or gone away. Pain signals remain active in the nervous system for weeks, months or years.
What means dorsalgia?
For starters, dorsalgia is severe back pain, which could be coming from different parts of the spine. Depending on the specific section of the spine where the pain is coming from, there are six types of dorsalgia.
What does intractable pain mean?
When a health care practitioner certifies a patient for intractable pain, they are certifying the patient meets this definition, "pain whose cause cannot be removed and, according to generally accepted medical practice, the full range of pain management modalities appropriate for this patient has been used without ...
What is the ICD 10 code for acute low back pain?
5: Low back pain.
What is the pain of the coccyx?
Pain of coccyx greater than 3 months, chronic. Clinical Information. A disorder characterized by the sensation of marked discomfort, distress or agony. An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons.
What does it mean when you feel a sensation?
Sensation of unpleasant feeling indicating potential or actual damage to some body structure felt all over, or throughout the body. Severe pain of limited duration. The sensation of discomfort, distress, or agony, resulting from the stimulation of specialized nerve endings.
What does "type 1 excludes note" mean?
It means "not coded here". A type 1 excludes note indicates that the code excluded should never be used at the same time as R52. A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition.
What is the meaning of pain?
Pain is a feeling triggered in the nervous system. Pain may be sharp or dull.
How long does pain last?
Once you take care of the problem, pain usually goes away. However, sometimes pain goes on for weeks, months or even years.
What is nonarticular rheumatic?
A common nonarticular rheumatic condition that is characterized by muscle pain, tenderness, and stiffness. A common nonarticular rheumatic syndrome characterized by myalgia and multiple points of focal muscle tenderness to palpation (trigger points).
What is the medical term for pain in the neck, shoulders, back, hips, and legs?
M60.-) (my-al-juh) pain in a muscle or group of muscles. A chronic disorder of unknown etiology characterized by pain, stiffness, and tenderness in the muscles of neck, shoulders, back, hips, arms, and legs. Other signs and symptoms include headaches, fatigue, sleep disturbances, and painful menstruation.
What causes a muscle to feel tired?
An acute, subacute, or chronic painful state of muscles, subcutaneous tissues, ligaments, tendons, or fasciae caused by a number of agents such as trauma, strain, occupation, exposure, posture, infection, or arthritis. Fibromyalgia makes you feel tired and causes muscle pain and "tender points.".
What is a thoracic myofascial pain syndrome?
Clinical Information. (my-al-juh) pain in a muscle or group of muscles. A chronic disorder of unknown etiology characterized by pain, stiffness, and tenderness in the muscles of neck, shoulders, back, hips, arms, and legs.
What is a type 1 exclude note?
A type 1 excludes note is a pure excludes. It means "not coded here". A type 1 excludes note indicates that the code excluded should never be used at the same time as M79.1. A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition.
What is the ICd 10 code for chronic pain?
G89.29 is a valid billable ICD-10 diagnosis code for Other chronic pain . It is found in the 2021 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2020 - Sep 30, 2021 .
What is tabular list?
When a specific code is not available for a condition, the Tabular List includes an NEC entry under a code to identify the code as the “other specified” code. This abbreviation is the equivalent of unspecified. This note further define, or give examples of, the content of the code or category.
What does "excludes" mean in a note?
An Excludes1 note indicates that the code excluded should never be used at the same time as the code above the Excludes1 note. An Excludes1 is used when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition. A type 2 Excludes note represents 'Not included here'.
What is a list of terms?
List of terms is included under some codes. These terms are the conditions for which that code is to be used. The terms may be synonyms of the code title, or, in the case of “other specified” codes, the terms are a list of the various conditions assigned to that code.
When an excludes2 note appears under a code, is it acceptable to use both the code and the excluded code
When an Excludes2 note appears under a code it is acceptable to use both the code and the excluded code together. A “code also” note instructs that two codes may be required to fully describe a condition, but this note does not provide sequencing direction. The sequencing depends on the circumstances of the encounter.
Do you include decimal points in ICD-10?
DO NOT include the decimal point when electronically filing claims as it may be rejected. Some clearinghouses may remove it for you but to avoid having a rejected claim due to an invalid ICD-10 code, do not include the decimal point when submitting claims electronically. See also: Pain (s) R52 see also Painful.
What is the ICd 10 code for post thoracotomy pain?
Category G89 contains four codes for acute and chronic post-thoracotomy pain (G89.12, G89.22) and other postprocedural pain (G89.18, G89.28). The ICD-10-CM guidelines state that you should not code “routine or expected postoperative pain immediately after surgery.” Additionally, in order to assign these codes, the physician must document that the patient’s pain is a complication of the surgery.
What is the G89 code?
For example, you can assign a G89 code to indicate that the pain is acute or chronic. You should assign the site-specific pain code first unless the purpose of the encounter is pain management, in which case the G89 code is first. For example, a patient is referred for ankle x-rays for chronic right ankle pain.
What is R07.81 pain?
Pleurodynia (R07.81): Spasms of pain in the intercostal muscles, which can be a sign of pleurisy (inflammationof the pleural membranes). Intercostal pain (R07.82): This is pain originating in the intercostal nerves, which run between pairs of adjacent ribs.
What is a pain that does not point to a specific body system?
Pain that does not point to a specific body system is classified in the Symptoms and Signs chapter. For example, abdominal pain is classified to category R10. Certain specific types of pain are classified to category G89 (Pain, not elsewhere classified) in the Nervous System chapter.
What is Category G89?
Category G89 contains codes for acute (G89.11) and chronic (G89.21) pain due to trauma. You should not assign these codes if a cause for the pain (i.e., a specific injury) has been identified, except in the unlikely event that the purpose of the encounter is pain management.
What is the ICD-10 code for chest pain?
The ICD-10-CM Index refers you to the code for angina (I20.9) when the patient’s chest pain is described as “ischemic.” However, other types of chest pain are reported with codes from category R07 (Pain in throat and chest). There is an exception for post-thoracotomy pain, which we’ll discuss later.
What causes central pain syndrome?
Central pain syndrome can occur as a result of stroke, multiple sclerosis, neoplasm, epilepsy, CNS trauma, or Parkinson’s disease. Patients with central pain syndrome may experience localized pain, burning, and/or numbness in specific parts of the body, or throughout the body.
Why is G89 not reported?
The reason for the service is for pain control or pain management . Do not report codes from category G89 as the first-listed diagnosis if you know the underlying (definitive) diagnosis and the reason for the service is to manage/treat the underlying condition.
What is the ICd 10 code for pain?
The ICD-10-CM Official Guidelines for Coding and Reporting provide extensive notes and instruction for coding pain (category G89). Review these guidelines in full. The following summary identifies key points.#N#When seeking a pain diagnosis, identify as precisely as possible the pain’s location and/or source. If pain is the primary symptom and you know the location, the Alphabetic Index generally will provide all the information you need.#N#Only report pain diagnosis codes from the G89 category as the primary diagnosis when: 1 The acute or chronic pain and neoplasm pain provide more detail when used with codes from other categories; or 2 The reason for the service is for pain control or pain management.
Why use the Alphabetic Index?
If pain is the primary symptom and you know the location, the Alphabetic Index generally will provide all the information you need. The acute or chronic pain and neoplasm pain provide more detail when used with codes from other categories; or. The reason for the service is for pain control or pain management.
How long does chronic pain last?
Chronic pain may last for months or years, and may persist even after the underlying injury has healed or the underlying condition has been treated. There is no specific timeframe identifying when you can define the pain as chronic. Determine the code assignment based on provider documentation.
How long does a syringe last?
It can range from mild to severe and may last a few minutes or a few months. Acute pain typically does not last longer than six months and usually disappears when the physician identifies and treats the underlying cause or condition.
Who is John Verhovshek?
John Verhovshek, MA, CPC, is a contributing editor at AAPC. He has been covering medical coding and billing, healthcare policy, and the business of medicine since 1999. He is an alumnus of York College of Pennsylvania and Clemson University.
Popular Posts:
- 1. icd 10 code for klippel feil syndrome
- 2. icd 10 code for heart murmer
- 3. icd 10 code for long term use of seroquel
- 4. icd 10 code for personal history of seizure
- 5. icd 10 code for acute lymphocytic leukemia
- 6. icd-10-pcs code for incidental appendectomy, opem
- 7. icd 9 code for whipple proceedure
- 8. icd 10 code for pm secondary to a. fib
- 9. icd 10 code for lesion of hard palate
- 10. icd 10 code for procedure clearance