What is ICD 10 for poorly controlled diabetes?
- Women in India with Gestational Diabetes Mellitus Strategy (WINGS): Methodology and development of model of care for gestational diabetes mellitus (WINGS 4)
- Difference between Diabetes Mellitus and Diabetes Insipidus
- Diabetes in Dogs (Diabetes Mellitus)
What is considered prediabetes A1c ICD 10?
What Is The Icd 10 Code For Prediabetes?
- Reimbursement And Coding For Prediabetes Screening. ...
- Icd-10 Diagnosis Code R73.03. ...
- ©october 2016 Academy Of Nutrition And Dietetics. ...
- 2017 Icd 10 Cm Diagnosis Code R73.03 Prediabetes. ...
- Prediabetes Vs Other Abnormal Glucose. ...
- 2018/2019 Icd-10-cm Diagnosis Code R73.09. ...
- Icd-10 Coding For The Undiagnosed Problem. ...
- 2018/2019 Icd-10-cm Diagnosis Code Z13.1. ...
What is the ICD 10 code for Type 1 diabetes?
Z79.84) Type 1 Excludes diabetes mellitus due to underlying condition ( E08.-) drug or chemical induced diabetes mellitus ( E09.-)
What type of diabetes requires insulin?
The objective of the trial is to assess the efficacy and safety of insulin icodec in 588 insulin-naïve people with type 2 diabetes. ONWARDS 4 is a 26-week trial comparing once-weekly insulin icodec with once-daily insulin degludec, both in combination ...
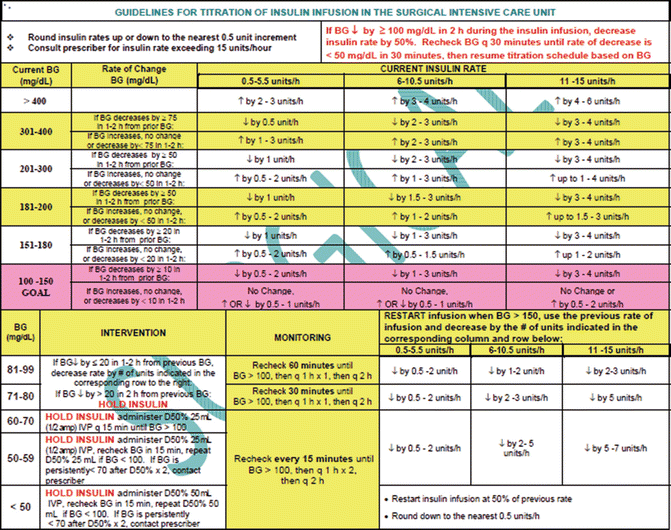
What is the ICD-10 code for insulin?
ICD-10 code Z79. 4 for Long term (current) use of insulin is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .
What is the ICD-10 code E11?
ICD-Code E11* is a non-billable ICD-10 code used for healthcare diagnosis reimbursement of Type 2 Diabetes Mellitus. Its corresponding ICD-9 code is 250. Code I10 is the diagnosis code used for Type 2 Diabetes Mellitus.
When do you code E11 8?
Type 2 diabetes mellitus with unspecified complications E11. 8 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM E11. 8 became effective on October 1, 2021.
What is the ICD-10 code for insulin dependent?
Z79. 4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM Z79.
When do you code E11 59?
ICD-10 Code for Type 2 diabetes mellitus with other circulatory complications- E11. 59- Codify by AAPC.
When do you code E11 69?
ICD-10-CM Code for Type 2 diabetes mellitus with other specified complication E11. 69.
Can you code E11 21 and E11 22 together?
21 and E11. 22 have an excludes 1 notes therefore they can be coded together as long as a separate renal manifestation is present, I would just be careful when coding the actual renal condition as there are some renal codes that are excluded when using CKD codes.
What are ICD 10 codes for diabetes?
Coding Diabetes Mellitus in ICD-10-CM: Improved Coding for Diabetes Mellitus Complements Present Medical ScienceE08, Diabetes mellitus due to underlying condition.E09, Drug or chemical induced diabetes mellitus.E10, Type 1 diabetes mellitus.E11, Type 2 diabetes mellitus.E13, Other specified diabetes mellitus.
What is the ICD 11 code for type 2 diabetes?
5A11 Type 2 diabetes mellitus - ICD-11 MMS.
Which is the insulin dependent diabetes?
Type 1 diabetes was once called insulin-dependent or juvenile diabetes. It usually develops in children, teens, and young adults, but it can happen at any age. Type 1 diabetes is less common than type 2—about 5-10% of people with diabetes have type 1.
Do you code insulin with type 1 diabetes?
Type I diabetics require the use of insulin to live. The use of insulin is implied in the diagnosis of Type I diabetes itself. Since this is the case, it is not necessary to report a Z code for long-term insulin use because it would be understood that this patient would be using insulin.
What does R73 01 mean?
ICD-10 code R73. 01 for Impaired fasting glucose is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is the proper ICD 10 code for type 2 diabetes mellitus with multiple complications?
E11. 69 - Type 2 diabetes mellitus with other specified complication. ICD-10-CM.
Which is the insulin dependent diabetes?
Type 1 diabetes was once called insulin-dependent or juvenile diabetes. It usually develops in children, teens, and young adults, but it can happen at any age. Type 1 diabetes is less common than type 2—about 5-10% of people with diabetes have type 1.
What is the ICD 10 code for diabetes?
E08. 1 Diabetes mellitus due to underlying condition... E08. 10 Diabetes mellitus due to underlying condition...
What is the ICD 10 code for type 1 diabetes?
ICD-10 code E10. 9 for Type 1 diabetes mellitus without complications is a medical classification as listed by WHO under the range - Endocrine, nutritional and metabolic diseases .
What is the ICd 10 code for diabetes?
Icd-10 Diagnosis Code E10.9. Diabetes Type 1 Also called: Insulin-dependent diabetes, Juvenile diabetes, Type I diabetes Diabetes means your blood glucose, or blood sugar, levels are too high. With type 1 diabetes, your pancreas does not make insulin. Insulin is a hormone that helps glucose get into your cells to give them energy.
What is the ICD-9 code for diabetes mellitus?
ICD-9-CM code structure classifies diabetes into a single code category, 250.
What is type 2 diabetes?
Type 2 Diabetes Mellitus E11- >. A disease in which the body does not control the amount of glucose (a type of sugar) in the blood and the kidneys make a large amount of urine. This disease occurs when the body does not make enough insulin or does not use it the way it should.
What is the name of the cell that stops producing insulin?
In this form of diabetes, specialized cells in the pancreas called beta cells stop producing insulin. Insulin controls how much glucose (a type of sugar) is passed from the blood into cells for conversion to energy. Lac Continue reading >>. Symptoms, Diagnosis & Monitoring of Diabetes.
What is the ICD-10 system?
The system is used for tracking and monitoring diseases and for health care reimbursement by countries around the world.
Where does glucose come from?
Glucose comes from the foods you eat . Insulin is a hormone that helps the glucose get into your cells to give them energy. With type 1 diabetes, your body does not make insulin. With type 2 diabetes, the more common type, your body does not make or use insulin well.
Can diabetes cause heart disease?
It can damage your eyes, kidneys, and nerves. Diabetes can also cause heart disease, stroke and even the need to remove a limb.
What is Type II diabetes?
A subclass of diabetes mellitus that is not insulin-responsive or dependent (niddm). It is characterized initially by insulin resistance and hyperinsulinemia; and eventually by glucose intolerance; hyperglycemia; and overt diabetes. Type ii diabetes mellitus is no longer considered a disease exclusively found in adults. Patients seldom develop ketosis but often exhibit obesity.
What is type 2 diabetes mellitus?
Subclass of diabetes mellitus that is not insulin responsive or dependent; characterized initially by insulin resistance and hyperinsulinemia and eventually by glucose intolerance, hyperglycemia, and overt diabetes; type ii diabetes mellitus is no longer considered a disease exclusively found in adults; patients seldom develop ketosis but often exhibit obesity.
What does it mean when your blood sugar is too high?
diabetes means your blood glucose, or blood sugar, is too high. With type 2 diabetes , the more common type, your body does not make or use insulin well. Insulin is a hormone that helps glucose get into your cells to give them energy. Without insulin, too much glucose stays in your blood.
How does diabetes affect your body?
Insulin is a hormone that helps the glucose get into your cells to give them energy. With type 1 diabetes, your body does not make insulin. With type 2 diabetes, the more common type, your body does not make or use insulin well. Without enough insulin, the glucose stays in your blood.over time, having too much glucose in your blood can cause serious problems. It can damage your eyes, kidneys, and nerves. Diabetes can also cause heart disease, stroke and even the need to remove a limb. Pregnant women can also get diabetes, called gestational diabetes.a blood test can show if you have diabetes. Exercise, weight control and sticking to your meal plan can help control your diabetes. You should also monitor your glucose level and take medicine if prescribed.
What does "type 1 excludes note" mean?
It means "not coded here". A type 1 excludes note indicates that the code excluded should never be used at the same time as E11. A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition.
Can high blood glucose cause heart problems?
Over time, high blood glucose can lead to serious problems with your heart, eyes, kidneys, nerves, and gums and teeth.you have a higher risk of type 2 diabetes if you are older, obese, have a family history of diabetes, or do not exercise.the symptoms of type 2 diabetes appear slowly.
Can diabetes cause kidney damage?
With type 2 diabetes, the more common type, your body does not make or use insulin well. Without enough insulin, the glucose stays in your blood.over time, having too much glucose in your blood can cause serious problems. It can damage your eyes, kidneys, and nerves.
What is E10.29?
E10.29 Type 1 diabetes mellitus with other diabetic ...
What is E11.618?
E11.618 Type 2 diabetes mellitus with other diabetic ...
What is the ICd 10 code for secondary diabetes?
Follow the instructions in the Tabular List of ICD-10-CM for proper sequencing of these diagnosis codes. For example, if a patient has secondary diabetes as a result of Cushing’s syndrome and no other manifestations, report code E24.9 Cushing’s syndrome, unspecified, followed by E08.9 Diabetes mellitus due to underlying condition without manifestations. If a patient is diagnosed with secondary diabetes due to the adverse effects of steroids, report codes E09.9 Drug or chemical induced diabetes without complications and T38.0X5A Adverse effect of glucocorticoids and synthetic analogues, initial encounter.
What is the code for gestational diabetes?
Codes for gestational diabetes are in subcategory O24.4. These codes include treatment modality — diet alone, oral hypoglycemic drugs, insulin — so you do not need to use an additional code to specify medication management. Do not assign any other codes from category O24 with the O24.4 subcategory codes.
How does diabetes affect blood sugar?
In patients with type 2 diabetes, problems begin when the cells in their body start to not respond to insulin as well as they should. This is called insulin resistance, which causes high blood sugar levels (hyperglycemia). The pancreas responds by making more insulin to try and manage the hyperglycemia, but eventually, the pancreas can’t keep up and blood sugar levels rise. Left uncontrolled, the disease progresses into prediabetes and, eventually, type 2 diabetes. This is the most common type of diabetes and is initially treated with lifestyle modification including a healthy diet and exercise. If these measures are not effective, treatment generally starts with an oral hypoglycemic agent. If better control is needed, injectable medications or insulin may be initiated to help manage blood sugar levels and avoid complications.
What chapter do you report diabetes?
Report encounters related to pregnancy and diabetes using codes in Chapter 15 Pregnancy, Childbirth, and the Puerperium. If a pregnant woman has pre-existing diabetes that complicates the pregnancy, Chapter 15 guidelines instruct us to assign a code from O24 first, followed by the appropriate diabetes code (s) from Chapter 4 (E08–E13). Report codes Z79.4 or Z79.84 if applicable.
What is secondary diabetes?
Secondary diabetes — DM that results as a consequence of another medical condition — is addressed in Chapter 4 guidelines. These codes, found under categories E08, E09, and E13, should be listed first, followed by the long-term therapy codes for insulin or oral hypoglycemic agents.
What is type 1.5 diabetes?
Type 1.5 diabetes is a form of diabetes in which an adult has features of both type 1 and type 2 diabetes. These patients have also been described with the terms “latent autoimmune diabetes of adults” (LADA), and “slow-progressing type 1 diabetes.” The condition has also been called “double” diabetes, because individuals demonstrate both the autoimmune destruction of beta cells of type 1 diabetes and the insulin resistance characteristic of type 2 diabetes. People with type 1.5 diabetes have autoantibodies to insulin-producing beta cells and gradually lose their insulin-producing capability, requiring insulin within 5–10 years of diagnosis.
What is the most common type of diabetes?
Left uncontrolled, the disease progresses into prediabetes and, eventually, type 2 diabetes. This is the most common type of diabetes and is initially treated with lifestyle modification including a healthy diet and exercise. If these measures are not effective, treatment generally starts with an oral hypoglycemic agent.
What is the Z79.4 for insulin?
These changes include: If the patient is treated with oral hypoglycemic medication and insulin, only assign the Z79.4 for long- term use of insulin , which is not a change for 2021. If the patient is treated with both insulin and injectable non-insulin anti-diabetic drug, assign Z79.4 and Z79.899 (other long-term drug therapy).
What type of neuropathy is cited in the 2020 Coding Clinic?
There was a Coding Clinic edition published in the first quarter of 2020 that cited a patient with a history of type 2 diabetic neuropathy and bariatric surgery. The physician documented that the patient’s diabetes had resolved after the bariatric surgery.
How many cases of diabetes were there in 1980?
According to the World Health Organization (WHO), diabetes is a chronic disease that occurs either when the pancreas does not produce enough insulin or when the body cannot effectively use the insulin it produces. The incidence of diabetes has increased from 108 million cases recorded in 1980 to 422 million in 2014.
What is the Z79.84 code?
If the patient is treated with both oral hypoglycemic medications and injectable non-insulin anti-diabetic drug, assign Z79.84 (long-term use of oral hypoglycemic drugs) and Z79.899. In 2020, the Official Coding and Reporting Guidelines indicated that if the patient was treated with insulin and oral hypoglycemic drugs, assign only Z79.84.
When to check A1C?
Remember to take time to check your A1C in the month of November.
Does diabetes cause premature death?
Diabetes also increases premature mortality. A healthy diet, regular physical activity, maintaining a normal body weight, and avoiding tobacco are all habits meant to prevent or delay the onset of Type 2 diabetes.
Popular Posts:
- 1. icd 10 code for left groin pain
- 2. icd 10 code for acute cholangitis with sirs
- 3. what icd-10-cm code is reported for post-mastectomy of the left breast
- 4. icd 10 code for left shoulder hill sachs lesion
- 5. icd-10-cm code for varicose veins, right
- 6. icd 10 code for spain due to trauma
- 7. icd 10 code for post craniotomy
- 8. icd-10-cm code for thyrotoxicosis with thyrotoxic storm
- 9. icd 10 code for post surgery care
- 10. icd 10 code for sarum ulcer