Pancreatic steatorrhea
- K90.3 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2021 edition of ICD-10-CM K90.3 became effective on October 1, 2020.
- This is the American ICD-10-CM version of K90.3 - other international versions of ICD-10 K90.3 may differ.
What is the ICD 10 diagnosis code for?
Disclosures: Kuwahara reports serving as a CMS fellow and previously served as a fellow at the Association of Asian Pacific Community Health Organizations. Disclosures: Kuwahara reports serving as a CMS fellow and previously served as a fellow at the Association of Asian Pacific Community Health Organizations.
What is the diagnosis code for pancreatic cancer?
- CT scan (88.01);
- MRI (88.87); • endoscopic retrograde cholangiopancreatiogaphy (51.10); • endoscopic ultrasound (88.74 and a code for the endoscopy—code assignment will depend on location) • percutaneous transhepatic cholangiography (87.51); • biopsy of ...
- Respectable — all tumor nodules can be removed.
What is the ICD 10 code for chronic pancreatitis?
Personal history of other diseases of the digestive system
- Z87.19 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM Z87.19 became effective on October 1, 2021.
- This is the American ICD-10-CM version of Z87.19 - other international versions of ICD-10 Z87.19 may differ.
What is the ICD 10 code for pancreatic cancer?
- C7A.020 Malignant carcinoid tumor of the appendix
- C7A.021 Malignant carcinoid tumor of the cecum
- C7A.022 Malignant carcinoid tumor of the ascending colon
- C7A.023 Malignant carcinoid tumor of the transverse colon
- C7A.024 Malignant carcinoid tumor of the descending colon
- C7A.025 Malignant carcinoid tumor of the sigmoid colon
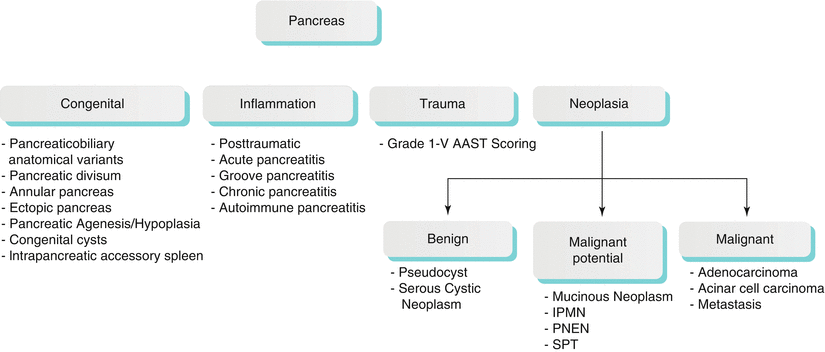
What is K86 89 diagnosis?
ICD-10 code K86. 89 for Other specified diseases of pancreas is a medical classification as listed by WHO under the range - Diseases of the digestive system .
What is pancreatic Steatorrhea?
Steatorrhea is one of the clinical features of fat malabsorption and noted in many conditions such as exocrine pancreatic insufficiency (EPI), celiac disease, and tropical sprue. An increase in the fat content of stools results in the production of pale, large volume, malodorous, loose stools.
What is the ICD-10 code for pancreatitis unspecified?
ICD-10 Code for Acute pancreatitis, unspecified- K85. 9- Codify by AAPC.
What is the ICD-10 code for pancreatic Steatorrhea?
K90. 3 - Pancreatic steatorrhea | ICD-10-CM.
What does thickening of pancreas mean?
Thickening of the pancreatic juices may result in clogging of the pancreatic ducts and pancreatic stones which, along with damage to the ducts themselves can result in aggravation of the pancreatitis due to obstruction.
What is steatorrhea caused by?
Although several conditions can lead to impaired lipid absorption and steatorrhea (excess fat in the feces), the most common causes of steatorrhea are related to bile salt deficiency, pancreatic enzyme deficiency, defective CM synthesis, or lymphatic obstruction.
What is the ICD 10 code for acute on chronic pancreatitis?
ICD-10 Code for Other chronic pancreatitis- K86. 1- Codify by AAPC.
What is acute pancreatitis?
Acute pancreatitis is a condition where the pancreas becomes inflamed (swollen) over a short period of time. The pancreas is a small organ, located behind the stomach, that helps with digestion. Most people with acute pancreatitis start to feel better within about a week and have no further problems.
What is chronic pancreatitis?
Chronic pancreatitis causes severe damage to your pancreas. This means that your body won't be able to make needed enzymes and hormones. This can result in malnutrition, because you won't be able to digest foods. Chronic pancreatitis can also cause diabetes. This happens because your pancreas can't make insulin.
What is fatty pancreas?
Fatty pancreas is a fatty‐infiltrated pancreas where adipocytes infiltrate the parenchyma with a scattered pattern (intralobular fat) and/or accumulate in the peri‐lobular space; this pattern is mainly observed around large vessels (interlobular fat).
Is the pancreas part of the digestive system?
During digestion, your pancreas makes pancreatic juices called enzymes. These enzymes break down sugars, fats, and starches. Your pancreas also helps your digestive system by making hormones. These are chemical messengers that travel through your blood.
What is the ICD 10 code for elevated lipase?
ICD-10-CM Code for Abnormal levels of other serum enzymes R74. 8.
Is steatorrhea serious?
Mild to moderate steatorrhea may only cause minor dehydration and discomfort but these symptoms can lead to serious conditions, including heart attack and organ failure, if left untreated. Steatorrhea can also be a sign of underlying medical conditions that require treatment.
What does steatorrhea poop look like?
What does steatorrhea stool look like? Steatorrhea, or fatty stools, are foul-smelling and may be loose and bulkier than usual. They will float and may appear to be filled with mucus, froth, or foam, and will be lighter in color.
What causes high Steatocrit?
This generally results from pancreatic exocrine insufficiency but can also occur with severe small bowel disease i.e. celiac disease, liver diseases such as Primary Biliary Cirrhosisor medications that inhibit fat absorption such as orlistat.
What are the symptoms of acute pancreatitis?
Acute pancreatitis signs and symptoms include:Upper abdominal pain.Abdominal pain that radiates to your back.Tenderness when touching the abdomen.Fever.Rapid pulse.Nausea.Vomiting.
What are the problems with the pancreas?
Problems with the pancreas can lead to many health problems. These include. pancreatitis, or inflammation of the pancreas: this happens when digestive enzymes start digesting the pancreas itself. pancreatic cancer. cystic fibrosis, a genetic disorder in which thick, sticky mucus can also block tubes in your pancreas.
What is the function of the pancreas?
It produces juices that help break down food and hormones that help control blood sugar levels. Problems with the pancreas can lead to many health problems.
Why does the pancreas no longer make insulin?
In type 1 diabetes, the beta cells of the pancreas no longer make insulin because the body's immune system has attacked them. In type 2 diabetes, the pancreas loses the ability to secrete enough insulin in response to meals.
Coding Notes for K86.8 Info for medical coders on how to properly use this ICD-10 code
Inclusion Terms are a list of concepts for which a specific code is used. The list of Inclusion Terms is useful for determining the correct code in some cases, but the list is not necessarily exhaustive.
MS-DRG Mapping
DRG Group #438-440 - Disorders of pancreas except malignancy with MCC.
ICD-10-CM Alphabetical Index References for 'K86.8 - Other specified diseases of pancreas'
The ICD-10-CM Alphabetical Index links the below-listed medical terms to the ICD code K86.8. Click on any term below to browse the alphabetical index.
Equivalent ICD-9 Code GENERAL EQUIVALENCE MAPPINGS (GEM)
This is the official approximate match mapping between ICD9 and ICD10, as provided by the General Equivalency mapping crosswalk. This means that while there is no exact mapping between this ICD10 code K86.8 and a single ICD9 code, 577.8 is an approximate match for comparison and conversion purposes.
What is the cause of inflammation of the pancreas?
Acute or chronic inflammation of the pancreas due to autodigestion of pancreatic tissue by its own enzymes. An acute inflammatory process that leads to necrosis of the pancreatic parenchyma. Signs and symptoms include severe abdominal pain, nausea, vomiting, diarrhea, fever, and shock.
What is subcutaneous nodular fat necrosis?
Pancreatitis, hereditary. Subcutaneous nodular fat necrosis in pancreatitis. Clinical Information. A disorder characterized by inflammation of the pancreas. Acute or chronic inflammation of the pancreas due to autodigestion of pancreatic tissue by its own enzymes.
How long does it take for pancreatitis to go away?
Pancreatitis can be acute or chronic. Either form is serious and can lead to complications.acute pancreatitis occurs suddenly and usually goes away in a few days with treatment.
Is pancreatitis an acute condition?
Pancreatitis is classified as acute unless there are computed tomographic or endoscopic retrograde cholangiopancreatographic findings of chronic pancreatitis (international symposium on acute pancreatitis, atlanta, 1992).

Popular Posts:
- 1. icd 10 code for history of gait instability
- 2. icd 10 code for v02.61
- 3. icd 10 code for prophylasic fo phst herpatic neralgia
- 4. icd 10 code for postorperative adhesions
- 5. icd-9-cm code for symbolic dysfunction
- 6. icd 10 code for onychomycosis
- 7. what was the payment for icd 9 code 410.9
- 8. icd 10 code for aseptic necrosis of scaphoid
- 9. icd 10 code for unspecified hand pain
- 10. icd 10 code for candidal of the colon