How to code ischial ulcer ICD 10?
Pressure ulcer of sacral region, stage 4
- L89.154 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM L89.154 became effective on October 1, 2021.
- This is the American ICD-10-CM version of L89.154 - other international versions of ICD-10 L89.154 may differ.
What is the diagnosis code for diabetic foot ulcer?
diabetic, it is considered a diabetic foot ulcer, and therefore should be coded using an L97- code. This is true even if arterial disease and/or pressure played a role in the develop-ment of this ulcer. ICD-10 Coding
How do you code a diabetic foot ulcer with osteomyelitis?
most commonly used codes for di-abetic foot ulcers are E10.621 (Type 1 diabetes mel-litus with foot ulcer) and E11.621 (Type 2 diabetes mellitus with foot ulcer). “Code first” indicates that an additional code is required, the orders matter, and you should list this code first. Therefore, E10.621 or E11.621 should precede the L97-
Do you have a foot ulcer?
The ulcer can develop anywhere on your foot or toes. Ulcers usually develop on the bottom of the foot. You may not know you have an ulcer until you notice drainage on your sock. Drainage is fluid that may be yellow, brown, or red. The fluid may also contain pus or blood.
How do you code a DM ulcer?
Of these options, the most commonly used codes for diabetic foot ulcers are E10. 621 (Type 1 diabetes mellitus with foot ulcer) and E11. 621 (Type 2 diabetes mellitus with foot ulcer). “Code first” indicates that an additional code is required, and it must be listed first.
What is the ICD-10 code for diabetic foot ulcer left foot?
Non-pressure chronic ulcer of other part of left foot with unspecified severity. L97. 529 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L97.
What is ICD-10 code for diabetic wound infection?
Type 2 diabetes mellitus with other skin ulcer The 2022 edition of ICD-10-CM E11. 622 became effective on October 1, 2021. This is the American ICD-10-CM version of E11.
What is the ICD-10 code for type 2 diabetes with foot ulcer?
Step 5: E11. 621 is a combination code describing “type 2 diabetes mellitus with foot ulcer.”
What is the difference between a pressure ulcer and a diabetic ulcer?
While diabetic patients can get pressure ulcers due to abuse or neglect in a nursing home, diabetic ulcers may appear in areas that are not typically subject to extended pressure—such as the bottoms of the feet when a resident has been lying down. In these cases, a diagnosis of a diabetic ulcer is more apt.
What is the ICD-10 code for foot ulcer?
Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity. L97. 509 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L97.
What is the ICD-10 code for diabetes with foot infection?
Type 2 diabetes mellitus with foot ulcer E11. 621 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM E11. 621 became effective on October 1, 2021.
How do you code a diabetic foot infection?
Wiki Diabetic foot infection???Code: E11.621.Code Name: ICD-10 Code for Type 2 diabetes mellitus with foot ulcer.Block: Diabetes mellitus (E08-E13)Details: Type 2 diabetes mellitus with foot ulcer. ... Excludes1: diabetes mellitus due to underlying condition (E08.-)More items...•
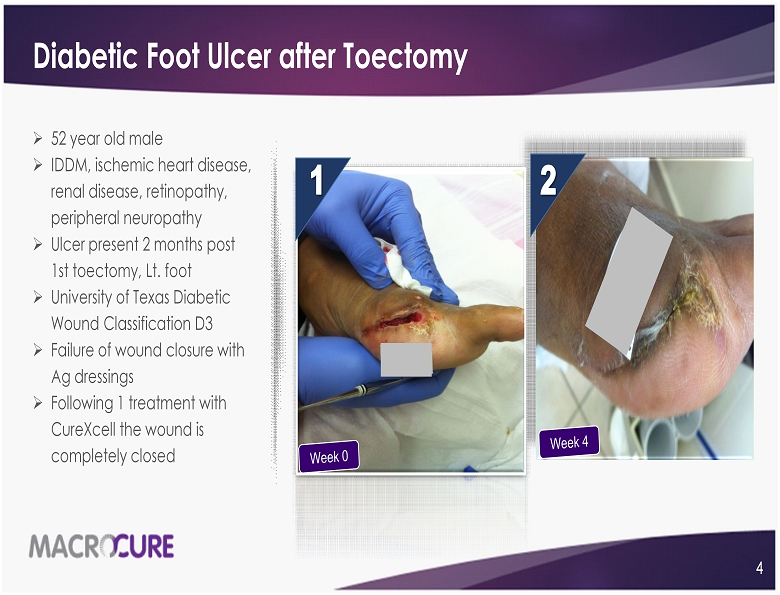
What is diabetic foot ulcer?
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
What is the difference between pressure ulcer and non-pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
What is the ICd 10 code for ulcers?
Non-pressure chronic ulcer of right heel and midfoot 1 L97.41 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. 2 The 2021 edition of ICD-10-CM L97.41 became effective on October 1, 2020. 3 This is the American ICD-10-CM version of L97.41 - other international versions of ICD-10 L97.41 may differ.
When will ICD-10 L97.41 be released?
The 2022 edition of ICD-10-CM L97.41 became effective on October 1, 2021.
What causes diabetic foot ulcers?
A “diabetic foot ulcer,” which is caused exclusively by hyperglycemia, in the absence of neuropathy or ischemia, is a rarity. That term almost always refers to an ulcer on the foot of a diabetic that derives from neuro/ischemic etiology, as opposed to being strictly and principally due to pressure injury.
Why do diabetics get ulcers on their feet?
The American Podiatric Medical Association adds that “ (diabetic foot) ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation (such as friction or pressure), and trauma, as well as duration of diabetes.” They go on to note that “vascular disease can complicate a foot ulcer, reducing the body’s ability to heal and increasing the risk for an infection.”
What is a malum perforans pedis ulcer?
Neuropathy results in malum perforans pedis (a.k.a. bad perforating foot) ulcers. These are painless, non-necrotic, circular lesions circumscribed by hyperkeratosis. They often overlie a metatarsal head. Ischemic wounds manifest local signs of ischemia such as thin, shiny, hairless skin with pallor and coldness. These are often found at areas of friction and may be painful.
Why are pressure ulcers considered a patient safety indicator?
Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.
What is the most common site of ulceration?
The plantar surface is the most common site of ulceration, especially at areas of bony prominence.”.
Why should we specifically carve out pressure ulcers?
Why should we specifically carve out pressure ulcers? Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.
What is non pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
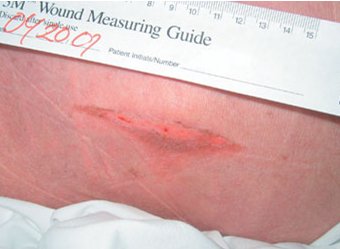
How are foot ulcers defined?
Typically, foot ulcers are defined by the appearance of the ulcer, the ulcer location, and the way the borders and surrounding skin of the ulcer look. There are different types of diabetic foot ulcers –
How many parts are there in the podiatry billing process?
9 Parts of The Podiatry Billing Process
What are the risk factors for ulcers?
The most common risk factors for ulcer formation include – diabetic neuropathy, structural foot deformity, kidney disease, obesity and peripheral arterial occlusive disease. The condition can be effectively prevented if the underlying conditions causing it are diagnosed early and treated correctly.
What is a diabetic foot ulcer?
Regarded as the most common reason for hospital stays among people with diabetes, a diabetic foot ulcer (DFU) is an open sore caused by neuropathic (nerve) and vascular (blood vessel) complications of the disease. Typically located on the plantar surface, or bottom/top of toes, pad of foot, or heel of foot, these complex, ...
What is the most common foot injury leading to lower extremity amputation?
Diabetic ulcers are the most common foot injuries leading to lower extremity amputation. The blog provides a detailed overview of the condition with the ICD-10 codes.
Why is it important to remove dead skin?
This procedure is important because dead skin hampers the development of healthy new tissues, and also makes the affected area more vulnerable to infections. Removal of the dead skin will promote quick and easy healing. Debridement will be done surgically, enzymatically, biologically, or through autolysis.
How many amputations are there for diabetics?
The risk of foot ulceration and limb amputations increases with age and duration of diabetes. In the United States, about 82,000 amputations are performed each year on persons with diabetes; half of those ages 65 years or older. Treatment for diabetic foot ulcers varies depending on their causes.
Popular Posts:
- 1. icd 10 code for spine surgery
- 2. icd 10 code for cll/sll
- 3. icd 10 cm code for rabies shot
- 4. icd 10 code for hx lymphoma
- 5. icd 9 code for e9556
- 6. icd 10 code for personal history of portal vein thrombosis
- 7. icd 10 code for lowe syndrome
- 8. icd-10 code for cholelithiasis
- 9. icd 10 code for singulair
- 10. what is the icd 10 code for hypocalcemia