What is the ICD 10 code for gangrene?
2021 ICD-10-CM Diagnosis Code I96 Gangrene, not elsewhere classified 2016 2017 2018 2019 2020 2021 Billable/Specific Code I96 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for left foot ulcer?
2016 2017 2018 2019 2020 Billable/Specific Code. L97.529 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. Short description: Non-pressure chronic ulcer oth prt left foot w unsp severity. The 2020 edition of ICD-10-CM L97.529 became effective on October 1, 2019.
What is the ICD 10 code for fused toes of bilateral feet?
Fused toes of bilat feet; Fused toes of bilateral feet; Syndactyly of toes of bilateral feet ICD-10-CM Diagnosis Code Q70.33 [convert to ICD-9-CM]
What is the ICD 10 code for chronic ulcer of toe?
L97.5 ICD-10-CM Diagnosis Code L97.5. Non-pressure chronic ulcer of other part of foot 2016 2017 2018 2019 Non-Billable/Non-Specific Code. Applicable To Non-pressure chronic ulcer of toe.

How do you code gangrene?
A: The coder would report ICD-10-CM code I96 (gangrene, not elsewhere classified) as the principal diagnosis because of the “code first” note under code category L89. - (pressure ulcer).
What is the ICD-10 for gangrene?
ICD-10 code I96 for Gangrene, not elsewhere classified is a medical classification as listed by WHO under the range - Diseases of the circulatory system .
What is the ICD 10 code for gangrene of right foot?
261.
Is necrosis the same as gangrene?
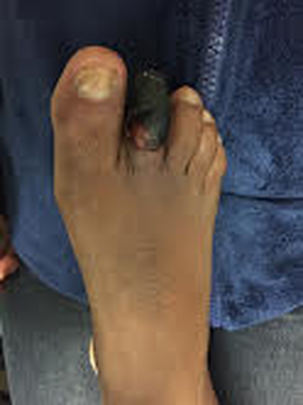
Gangrene is dead tissue (necrosis) consequent to ischemia. In the image above, we can see a black area on half of the big toe in a diabetic patient. This black area represents necrosis—dead tissue—in fact, gangrene of the big toe.
What is gangrene?
Gangrene is a serious condition where a loss of blood supply causes body tissue to die. It can affect any part of the body but typically starts in the toes, feet, fingers and hands. Gangrene can occur as a result of an injury, infection or a long-term condition that affects blood circulation.
What is code e11621?
ICD-10 code E11. 621 for Type 2 diabetes mellitus with foot ulcer is a medical classification as listed by WHO under the range - Endocrine, nutritional and metabolic diseases .
What is the ICD-10 code for right lower extremity gangrene?
I70. 261 - Atherosclerosis of native arteries of extremities with gangrene, right leg. ICD-10-CM.
Does necrosis code to gangrene?
Necrosis is commonly documented in the patient records with traumatic wounds, burns, pressure sores etc. Necrosis due to lack of oxygen such as with a MI would be considered part of the MI code as would any necrosis with infection in pneumonia. Gangrene would seem to be a complication of necrotic tissue.
Is gangrene an infection?
Overview. Gangrene is death of body tissue due to a lack of blood flow or a serious bacterial infection. Gangrene commonly affects the arms and legs, including the toes and fingers.
What are the three types of gangrene?
Types of gangrenedry gangrene – where the blood flow to an area of the body becomes blocked.wet gangrene – caused by a combination of an injury and bacterial infection.gas gangrene – where an infection develops deep inside the body and the bacteria responsible begin releasing gas.More items...
What is necrosis of the foot?
Avascular necrosis (AVN) involving the bones of the foot and ankle is an uncommon condition that can lead to significant disability and loss of function. AVN occurs due to the loss of blood supply to an area of bone, which can lead to destruction of the involved bone and surrounding joint cartilage.
How many different types of gangrene are there?
There are two major types of gangrene, wet gangrene and dry gangrene. Dry gangrene can result from conditions that reduce or block arterial blood flow such as diabetes, arteriosclerosis, and tobacco addiction as well as from trauma, frostbite, or injury.
When do you code E11 69?
ICD-10-CM Code for Type 2 diabetes mellitus with other specified complication E11. 69.
Why does diabetes cause gangrene?
Diabetes. People with diabetes have an increased risk of developing gangrene. This is because the high blood sugar levels associated with the condition can damage your nerves, particularly those in your feet, which can make it easy to injure yourself without realising.
What is the ICD-10 code for skin necrosis?
ICD-10 code: R02. 0 Necrosis of skin and subcutaneous tissue, not elsewhere classified.
What is the ICD-10 code for diabetic neuropathy?
ICD-10 Code for Type 2 diabetes mellitus with diabetic neuropathy, unspecified- E11. 40- Codify by AAPC.
Does gangrene affect diabetes?
However, I strongly object to the characterization that the “gangrene is associated with the pressure ulcer rather than the diabetes mellitus.”. Gangrene has to affect a body part (e.g., musculoskeletal system, intestine portion, gallbladder, etc.); it does not occur diffusely, i.e., directly due to diabetes.
Is a diabetic foot ulcer considered a pressure ulcer?
In the first article in this series, I compared pressure ulcers and diabetic foot ulcers (the latter are considered non-pressure chronic ulcers in ICD-10-CM). My conclusion was that there is significant overlap, but heel ulcers are prime candidates to be classified as pressure injuries by providers. Ultimately, their documentation will determine whether an ulcer on the foot of a diabetic will be considered a “diabetic foot ulcer” or a pressure ulcer. This article will explore whether they are mutually exclusive conditions.
Popular Posts:
- 1. icd 10 code for history of diabetic ulcer
- 2. what is the icd 10 code for stemi of inferior wall
- 3. icd 10 code for shorness of breath
- 4. icd 10 code for burn to left foot initial encounter for fracture
- 5. icd 10 code for asthmatic bronchitis
- 6. icd 10 cm code for reactive depression
- 7. icd 10 code for teres minor strain right
- 8. icd 10 code for spinal cord injury cervical
- 9. icd 10 code for annual labs
- 10. icd 10 code for intraperitoneal abscesses