What is treatment for infected ulcers?
Treatment
- Treatment team
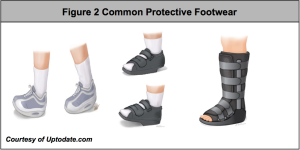
- Reducing pressure. The first step in treating a bedsore is reducing the pressure and friction that caused it. ...
- Cleaning and dressing wounds. Care for pressure ulcers depends on how deep the wound is. ...
- Removing damaged tissue. To heal properly, wounds need to be free of damaged, dead or infected tissue. ...
- Other interventions. ...
- Surgery. ...
What is toe ulcer?
What Is an Ulcer?
- Leg and Foot Ulcers. These can be painful and may take months to heal. ...
- Bedsores. Also called pressure ulcers or pressure sores, at first they just look like off-color skin. ...
- Genital Ulcers. These are painful sores on the penis, vagina, or anus. ...
- Corneal Ulcers. These show up on the cornea, which is the surface of your eye. ...
- Stomach Ulcers. ...
- Mouth Ulcers. ...
What causes a foot ulcer?
You’re also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
- Heart disease.
- Obesity.
- A foot deformity like a bunion or hammertoe.
- Kidney disease.
- Wounded feet.
- Use tobacco.
- Use alcohol.
What is the ICD 10 code for impacted tooth?
- DRG 011 - TRACHEOSTOMY FOR FACE,MOUTH & NECK DIAGNOSES OR LARYNGECTOMY WITH MCC
- DRG 012 - TRACHEOSTOMY FOR FACE,MOUTH & NECK DIAGNOSES OR LARYNGECTOMY WITH CC
- DRG 013 - TRACHEOSTOMY FOR FACE,MOUTH & NECK DIAGNOSES OR LARYNGECTOMY WITHOUT CC/MCC
What is the ICD 10 code for right toe ulcer?
519 for Non-pressure chronic ulcer of other part of right foot with unspecified severity is a medical classification as listed by WHO under the range - Diseases of the skin and subcutaneous tissue .
What is the ICD 10 code for ulcer left toe?
L97. 529 - Non-pressure chronic ulcer of other part of left foot with unspecified severity. ICD-10-CM.
What is the ICD 10 code for unspecified foot ulcer?
ICD-10-CM Code for Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity L97. 509.
What is the ICD-10 for diabetic foot ulcer?
ICD-10 code E11. 621 for Type 2 diabetes mellitus with foot ulcer is a medical classification as listed by WHO under the range - Endocrine, nutritional and metabolic diseases .
How do you code a foot ulcer?
Of these options, the most commonly used codes for diabetic foot ulcers are E10. 621 (Type 1 diabetes mellitus with foot ulcer) and E11. 621 (Type 2 diabetes mellitus with foot ulcer).
What is a hallux ulcer?
In conclusion, hallux ulceration is common in patients with diabetes mellitus and is usually preceded by a blister. Neuropathy, foot deformity, and wearing new shoes are common causative factors; and ischemia, osteomyelitis, any form of wound infection, and the size of the ulcer are main outcome determinants.
What is the ICD-10 code for foot lesion?
Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity. L97. 509 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L97.
Whats the difference between a pressure ulcer and a diabetic ulcer?
While diabetic patients can get pressure ulcers due to abuse or neglect in a nursing home, diabetic ulcers may appear in areas that are not typically subject to extended pressure—such as the bottoms of the feet when a resident has been lying down. In these cases, a diagnosis of a diabetic ulcer is more apt.
What is the difference between a pressure ulcer and a non-pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
What is ICD-10 code for diabetic wound infection?
Type 2 diabetes mellitus with other skin ulcer The 2022 edition of ICD-10-CM E11. 622 became effective on October 1, 2021.
How do you code a diabetic foot infection?
Wiki Diabetic foot infection???Code: E11.621.Code Name: ICD-10 Code for Type 2 diabetes mellitus with foot ulcer.Block: Diabetes mellitus (E08-E13)Details: Type 2 diabetes mellitus with foot ulcer. ... Excludes1: diabetes mellitus due to underlying condition (E08.-)More items...•
What is diabetic foot ulcer?
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
What is the ICD-10 code for diabetic foot ulcer left foot?
Non-pressure chronic ulcer of other part of left foot with unspecified severity. L97. 529 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L97.
What is a non-pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
What is the ICD-10 code for foot infection?
X7 for Direct infection of ankle and foot in infectious and parasitic diseases classified elsewhere is a medical classification as listed by WHO under the range - Arthropathies .
What is the ICD-10 code for peripheral arterial disease?
Provider's guide to diagnose and code PAD Peripheral Artery Disease (ICD-10 code I73. 9) is estimated to affect 12 to 20% of Americans age 65 and older with as many as 75% of that group being asymptomatic (Rogers et al, 2011).
What is a grade 1 foot?
The Grade 1 foot has a superficial ulcer without penetration to deeper layers. The base may be necrotic or may be viable with early granulation tissue
What is ulcer depth?
Ulcer depth: with necrosis of muscle. with muscle involvement without evidence of necrosis. The Grade 3 foot has ulcer with deep abscess, osteitis or osteomyelitis, pyarthrosis, plantar space abscess, or infection of the tendon and tendon sheaths.
What are the tables 1A, 1B and 2?
Tables 1A, 1B and 2 below correlate the Wagner and UT classification systems with the specific terminology medical coders need in order to correctly code the encounter.
What classification system is used for UT?
The UT system is based on the Wagner classification system, and describes the presence of infection and ischemia better than Wagner. Despite its widespread use, it does not reference either neuropathy or ulcer area, which is considered to be one of the main determinants of time to healing.
Which scale assesses ulcer depth and the presence of osteomyelitis or gangrene?
Sabet pointed out the Wagner Scale assesses ulcer depth and the presence of osteomyelitis or gangrene by using the following grades:
Can ulcers be cultured?
Clinically uninfected ulcers should not be cultured, as the recovered organisms will contain only colonizing flora. “Empirical antibiotic therapy should be started and revised, if necessary, once culture results are obtained.”
How are foot ulcers defined?
Typically, foot ulcers are defined by the appearance of the ulcer, the ulcer location, and the way the borders and surrounding skin of the ulcer look. There are different types of diabetic foot ulcers –
What is a diabetic foot ulcer?
Regarded as the most common reason for hospital stays among people with diabetes, a diabetic foot ulcer (DFU) is an open sore caused by neuropathic (nerve) and vascular (blood vessel) complications of the disease. Typically located on the plantar surface, or bottom/top of toes, pad of foot, or heel of foot, these complex, ...
How many parts are there in the podiatry billing process?
9 Parts of The Podiatry Billing Process
What are the risk factors for ulcers?
The most common risk factors for ulcer formation include – diabetic neuropathy, structural foot deformity, kidney disease, obesity and peripheral arterial occlusive disease. The condition can be effectively prevented if the underlying conditions causing it are diagnosed early and treated correctly.
What is the most common foot injury leading to lower extremity amputation?
Diabetic ulcers are the most common foot injuries leading to lower extremity amputation. The blog provides a detailed overview of the condition with the ICD-10 codes.
How many people with diabetes have foot ulcers?
According to the American Podiatric Medical Association (APMA), approximately 15 percent of people with diabetes suffer from foot ulcers. Of those who develop a foot ulcer, about 6 percent will be hospitalized due to serious infections or other ulcer-related complications.
Where does neuropathic ulcer occur?
Neuropathic ulcers– occur where there is peripheral diabetic neuropathy, but no ischemia caused by peripheral artery disease. This type of foot infection generally occurs on the plantar aspect of the foot under the metatarsal heads or on the plantar aspects of the toes.
What is a grade 1 wound?
Grade 1 – superficial wound not involving tendon, capsule, or bone
What are the different types of ulcers?
The Wagner diabetic foot ulcer classification system assesses ulcer depth and the presence of osteomyelitis or gangrene by using the following grades: 1 Grade 0 – intact Skin 2 Grade 1 – superficial ulcer of skin or subcutaneous tissue 3 Grade 2 – ulcers extend into tendon, bone, or capsule 4 Grade 3 – deep ulcer with osteomyelitis, or abscess 5 Grade 4 – partial foot gangrene 6 Grade 5 – whole foot gangrene
Is there a universal system for diabetic ulcers?
At the present time no specific system has been universally accepted. Even so, most clinicians use one of the available systems when assessing and documenting a diabetic ulcer.
What is non pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
Why are pressure ulcers considered a patient safety indicator?
Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.
What causes diabetic foot ulcers?
A “diabetic foot ulcer,” which is caused exclusively by hyperglycemia, in the absence of neuropathy or ischemia, is a rarity. That term almost always refers to an ulcer on the foot of a diabetic that derives from neuro/ischemic etiology, as opposed to being strictly and principally due to pressure injury.
Why do diabetics get ulcers on their feet?
The American Podiatric Medical Association adds that “ (diabetic foot) ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation (such as friction or pressure), and trauma, as well as duration of diabetes.” They go on to note that “vascular disease can complicate a foot ulcer, reducing the body’s ability to heal and increasing the risk for an infection.”
What is a malum perforans pedis ulcer?
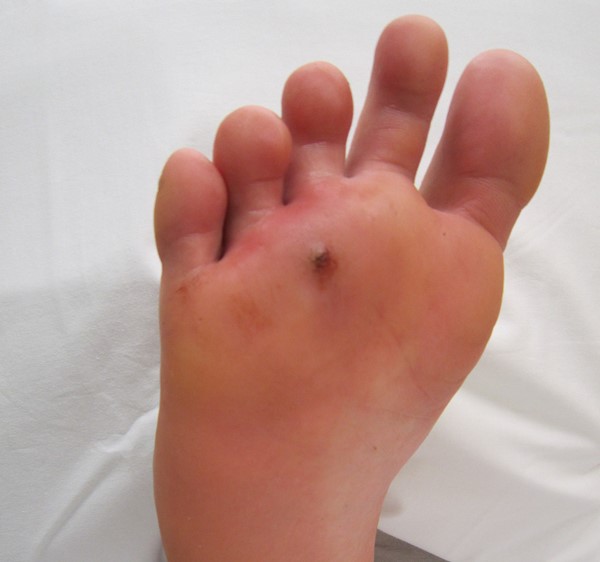
Neuropathy results in malum perforans pedis (a.k.a. bad perforating foot) ulcers. These are painless, non-necrotic, circular lesions circumscribed by hyperkeratosis. They often overlie a metatarsal head. Ischemic wounds manifest local signs of ischemia such as thin, shiny, hairless skin with pallor and coldness. These are often found at areas of friction and may be painful.
What is the most common site of ulceration?
The plantar surface is the most common site of ulceration, especially at areas of bony prominence.”.
Why should we specifically carve out pressure ulcers?
Why should we specifically carve out pressure ulcers? Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.
How deep is the dermis of ulcer?
Ulcer is 6cm x 5cm to depth of dermis and you debride 4cm x 4cm of tissue to dermis:
How many ulcers are there in the human body?
Two ulcers: first 2cm x 2cm, second 4cm x 4cm both debrided to dermis
How big is an ulcer debride?
One ulcer debride 2cm x 2cm to dermis and another debride 6cm x 6cm to muscle. 97 597 – 59 mod
How many square centimeters are needed for debridement of wound?
Debridement of open wound to level of epidermis / dermis each additional 20 square centimeters
Popular Posts:
- 1. icd 10 code for osteoarthrosis left shoulder
- 2. icd-10 code for 6 month follow up mammogram
- 3. icd 10 code for osteoarthritis of toe joint, left
- 4. icd 9 code for abnormal ct scan
- 5. icd 9 code for intvrt disc disorders with radiculopathy
- 6. icd 10 code for lupus
- 7. icd-10-pcs code for excision of peritoneum, open approach, diagnostic
- 8. icd 10 cm code for fall from skateboard
- 9. icd 10 code for hfref
- 10. icd 10 code for diabetic ulcer of left great toe