Non-pressure chronic ulcer of other part of left foot with fat layer exposed. L97.522 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2019 edition of ICD-10-CM L97.522 became effective on October 1, 2018.
What is the ICD 10 code for foot ulcer?
Pressure ulcer L89-
- bed sore
- decubitus ulcer
- plaster ulcer
- pressure area
- pressure sore
What is non - pressure ulcer?
Non-pressure chronic ulcers are similar to pressure ulcers in that they require documentation of the site, severity, and laterality. Category L97 and L98 are for Non-pressure ulcers, and have an instructional note to code first any associated underlying condition, such as: Associated gangrene.
What is the ICD 9 code for pressure ulcer?
- Bedsore (see also Ulcer, pressure) 707.00 with gangrene 707.00 [ 785.4]
- Decubiti (see also Ulcer, pressure) 707.00
- Decubitus (ulcer) (see also Ulcer, pressure) 707.00 with gangrene 707.00 [ 785.4] ankle 707.06 back lower 707.03 upper 707.02 buttock 707.05 coccyx 707.03 elbow 707.01 head 707.09 heel 707.07 hip ...
What does non - pressure Chronic ulcer mean?
What is a non pressure ulcer? Non-pressure chronic ulcers are similar to pressure ulcers in that they require documentation of the site, severity, and laterality. Category L97 and L98 are for Non-pressure ulcers, and have an instructional note to code first any associated underlying condition, such as: Associated gangrene.
How do you code a non-pressure ulcer?
Non-pressure chronic ulcer of skin of other sites with unspecified severity. L98. 499 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD-10 code for unspecified foot ulcer?
ICD-10-CM Code for Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity L97. 509.
What is a non-pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
What is the ICD-10 code for non healing ulcer?
Non-pressure chronic ulcer of skin of other sites limited to breakdown of skin. L98. 491 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L98.
What is the ICD-10 code for foot lesion?
Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity. L97. 509 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L97.
Whats the code for a non-pressure chronic ulcer of the right foot with a breakdown of the skin?
ICD-10-CM Code for Non-pressure chronic ulcer of other part of right foot limited to breakdown of skin L97. 511.
How do you code a foot ulcer?
Of these options, the most commonly used codes for diabetic foot ulcers are E10. 621 (Type 1 diabetes mellitus with foot ulcer) and E11. 621 (Type 2 diabetes mellitus with foot ulcer).
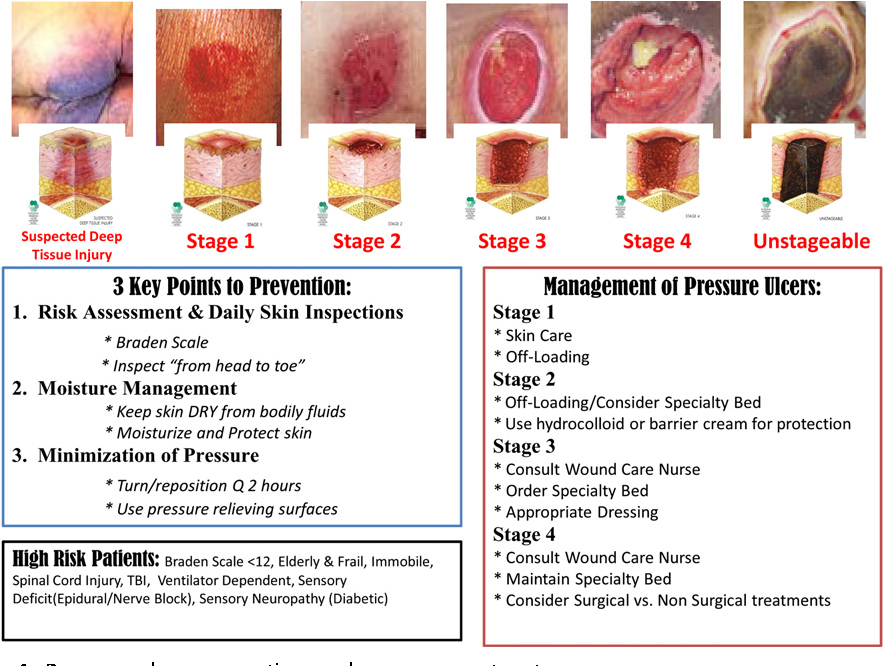
Are Non pressure ulcers stages?
Possible stages are 1-4 and unstageable. Unstageable: Based on clinical documentation the stage cannot be determined clinically (e.g., the wound is covered with eschar) or for ulcers documented as deep tissue injury without evidence of trauma.
What is pressure ulcer and non pressure ulcer?
Non-pressure chronic ulcers are similar to pressure ulcers in that they require documentation of the site, severity, and laterality. Category L97 and L98 are for Non-pressure ulcers, and have an instructional note to code first any associated underlying condition, such as: Associated gangrene.
What is the ICD-10 code for non-healing surgical wound?
998.83 - Non-healing surgical wound is a topic covered in the ICD-10-CM.
What is ICD-10 code for leg wound?
Unspecified open wound, unspecified lower leg, initial encounter. S81. 809A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM S81.
What is a superficial ulcer?
ulcer, a lesion or sore on the skin or mucous membrane resulting from the gradual disintegration of surface epithelial tissue. An ulcer may be superficial, or it may extend into the deeper layer of the skin or other underlying tissue.
What are the different types of ulcers?
Non-pressure chronic ulcer of lower limb, not elsewhere classified L97- 1 chronic ulcer of skin of lower limb NOS 2 non-healing ulcer of skin 3 non-infected sinus of skin 4 trophic ulcer NOS 5 tropical ulcer NOS 6 ulcer of skin of lower limb NOS
What is a type 2 exclude note?
A type 2 excludes note indicates that the condition excluded is not part of the condition it is excluded from but a patient may have both conditions at the same time. When a type 2 excludes note appears under a code it is acceptable to use both the code ( L97) and the excluded code together.
What causes ulcers in the body?
Ulceration caused by prolonged pressure in patients permitted to lie too still for a long period of time; bony prominences of the body are the most frequently affected sites; ulcer is caused by ischemia of the underlying structures of the skin, fat, and muscles as a result of the sustained and constant pressure. Codes.
What is pressure sore?
Pressure sores are areas of damaged skin caused by staying in one position for too long. They commonly form where your bones are close to your skin, such as your ankles, back, elbows, heels and hips. You are at risk if you are bedridden, use a wheelchair, or are unable to change your position.
What does type 2 exclude note mean?
A type 2 excludes note represents "not included here". A type 2 excludes note indicates that the condition excluded is not part of the condition it is excluded from but a patient may have both conditions at the same time. When a type 2 excludes note appears under a code it is acceptable to use both the code ( L89) and the excluded code together.
What is the ICD-10 code for ulcers on the left foot?
L97.52 is a non-billable ICD-10 code for Non-pressure chronic ulcer of other part of left foot. It should not be used for HIPAA-covered transactions as a more specific code is available to choose from below.
What is a billable L97.525?
Billable - L97.525 Non-pressure chronic ulcer of other part of left foot with muscle involvement without evidence of necrosis
What is non pressure ulcer?
The term “non-pressure ulcer” was coined to designate a primary mechanism other than shear or pressure. If there is poor circulation, such as that caused by venous or arterial insufficiency or excessive moisture or trauma, a patient may develop a non-pressure ulcer.
Why are pressure ulcers considered a patient safety indicator?
Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.
What causes diabetic foot ulcers?
A “diabetic foot ulcer,” which is caused exclusively by hyperglycemia, in the absence of neuropathy or ischemia, is a rarity. That term almost always refers to an ulcer on the foot of a diabetic that derives from neuro/ischemic etiology, as opposed to being strictly and principally due to pressure injury.
Why do diabetics get ulcers on their feet?
The American Podiatric Medical Association adds that “ (diabetic foot) ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation (such as friction or pressure), and trauma, as well as duration of diabetes.” They go on to note that “vascular disease can complicate a foot ulcer, reducing the body’s ability to heal and increasing the risk for an infection.”
What is a malum perforans pedis ulcer?
Neuropathy results in malum perforans pedis (a.k.a. bad perforating foot) ulcers. These are painless, non-necrotic, circular lesions circumscribed by hyperkeratosis. They often overlie a metatarsal head. Ischemic wounds manifest local signs of ischemia such as thin, shiny, hairless skin with pallor and coldness. These are often found at areas of friction and may be painful.
What is pressure injury?
Shear and pressure are the mechanisms that lead to what are known as “pressure injuries.” In 2016, the National Pressure Ulcer Advisory Panel (NPUAP) recommended transitioning to the terminology of “pressure injury” because although underlying tissue may be damaged, overlying skin may appear intact. Pressure injuries with skin breakdown are considered pressure ulcers. An additional L89 code specifies the stage (depth of tissue injury) and the anatomical site.
Why should we specifically carve out pressure ulcers?
Why should we specifically carve out pressure ulcers? Pressure ulcers are deemed patient safety indicators and hospital acquired conditions because a concerted program for prevention and treatment can prevent them and protect our patients from iatrogenic harm. The diagnosis of a “pressure ulcer” may trigger prevalence and incident reporting.

Popular Posts:
- 1. icd 10 code for natal teeth
- 2. icd 10 code for history of ra
- 3. icd 10 code for personal history of hormone therapy
- 4. icd 10 cm code for dvt prophylaxis
- 5. icd-10 code for depression with anxiety
- 6. icd code for pre-op testing
- 7. icd 9 code for shingels
- 8. icd 10 code for parkinson's dz
- 9. icd 10 code for transmetatarsal amputation of food at right big toe
- 10. icd 9 code for abdominal swelling mass and lump