What are the common ICD 10 codes?
ICD-10-CM CODES (commonly used) These commonly used ICD-10 diagnosis codes are intended to assist physicians and other authorized ordering parties in providing correct ICD-10 codes as required by Medicare and other insurers. The codes are based on ICD-10-CM 2018, Medicare Regulations and Manuals authorized by the Centers for
What ICD 10 codes will cover vitamin D testing?
What ICD 10 codes will cover vitamin D testing?
- ICD - 10 CODE. DESCRIPTION.
- ICD - 10 CODE. DESCRIPTION.
- 2018. MEDICARE LOCAL COVERAGE DETERMINATION (LCD) - L36692.
- CPT CODES: 82306, 82652.
- Vitamin D Assay Testing.
- For services performed on or after 2-3-2017.
- DLS TEST CODE AND NAME.
What IC10 codes will cover vitamin D for Medicare?
- chronic kidney disease stage III or greater;
- osteoporosis;
- osteomalacia;
- osteopenia;
- osteogenesis imperfecta;
- osteosclerosis;
- hypocalcemia;
- hypercalcemia;
- hypoparathyroidism;
- hyperparathyroidism;
What is the diagnosis code for vitamin D deficiency?
- Only one 25 OH Vitamin D level will be reimbursed in any 24 hour period.
- Patients with conditions outlined in the indications (acute and high risk conditions associated with Vitamin D deficiency) are candidates for testing. ...
- It’s not reasonable and necessary to perform more than three tests per year.
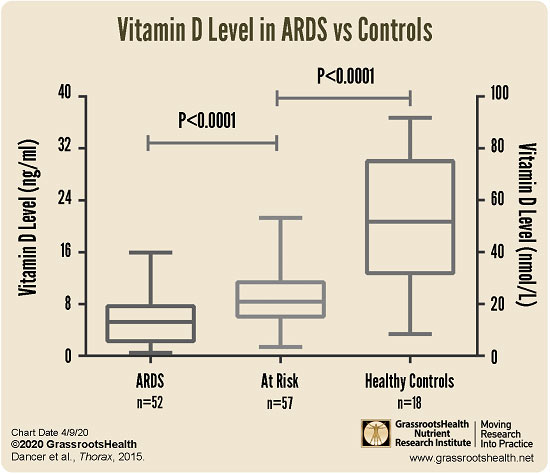
What ICD-10 codes cover vitamin D level?
4. Assays of the appropriate vitamin D levels for ICD-10 codes E55. 0, E55.
What does diagnosis E55 9 mean?
ICD-10 code: E55. 9 Vitamin D deficiency, unspecified.
What diagnosis code can be used for vitamin D?
E55. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What ICD-10 code covers vitamin D for Medicare?
2. For 82306: If more than one LCD-listed condition contributes to Vitamin D deficiency in a given patient and/or is improved by Vitamin D administration, coders should use: ICD-10 E55. 9 UNSPECIFIED VITAMIN D DEFICIENCY. This code should not be used for any other indication.
What does code E03 9 mean?
Hypothyroidism, UnspecifiedICD-9 Code Transition: 244.9 Code E03. 9 is the diagnosis code used for Hypothyroidism, Unspecified. It is a type of disorder of thyroid gland, a condition in which the production of thyroid hormone by the thyroid gland is diminished.
What is DX code I10?
ICD-Code I10 is a billable ICD-10 code used for healthcare diagnosis reimbursement of Essential (Primary) Hypertension.
How does Medicare cover vitamin D levels?
For Medicare beneficiaries, screening tests are governed by statute. Vitamin D testing may not be used for routine screening. Once a beneficiary has been shown to be vitamin D deficient, further testing is medically necessary only to ensure adequate replacement has been accomplished.
Does Medicare cover vitamin D?
Generally, Medicare Part D doesn't cover vitamin supplements, as mentioned above.
Does Medicare pay for vitamin D levels?
Do Medicare prescription drug plans cover vitamin D3? No. In general, Medicare prescription drug plans (Part D) do not cover this drug.
Does insurance cover vitamin deficiency test?
Widespread testing is associated with potentially unnecessary treatments with supplements, retesting and increased medical costs. On average, a vitamin D deficiency test can cost $50, typically covered by health insurance.
How often can you bill 82306?
25-OH Vitamin D-3 (82306) may be tested up to four times per year for Vitamin D deficiencies (268.0–268.9).
What does anemia D64 9 mean?
Code D64. 9 is the diagnosis code used for Anemia, Unspecified, it falls under the category of diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism. Anemia specifically, is a condition in which the number of red blood cells is below normal.
What causes a vitamin D deficiency?
(Rickets; Osteomalacia) Vitamin D deficiency is most commonly caused by a lack of exposure to sunlight. Some disorders can also cause the deficiency. The most common cause is lack of exposure to sunlight, usually when the diet is deficient in vitamin D, but certain disorders can also cause the deficiency.
What is ICD-10 code for vitamin B12 deficiency?
ICD-10 code D51. 9 for Vitamin B12 deficiency anemia, unspecified is a medical classification as listed by WHO under the range - Diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism .
What can you do for vitamin D deficiency?
Vitamin D deficiency is usually treated with supplements, but you may need a doctor's advice to get the right dosage. Increasing your sun exposure and eating more vitamin D-rich foods, such as fatty fish and fortified dairy products, can also help.
What is the most infamous vitamin D deficiency?
Vitamin D deficiency may lead to a variety of disorders, the most infamous of which is rickets. Evaluating patients’ vitamin D levels is accomplished by measuring the level of 25-hydroxyvitamin D. Measurement of other metabolites is generally not medically necessary.
What happens if you don't take vitamin D?
Vitamin D deficiency results in abnormalities in calcium, phosphorus, and bone metabolism. Specifically, vitamin D deficiency causes a decrease in the efficiency of intestinal calcium and phosphorus absorption of dietary calcium and phosphorus, resulting in an increase in parathyroid hormone (PTH) levels.
Why is vitamin D called a vitamin?
Vitamin D is called a “vitamin” because of its exogenous source, predominately from oily fish in the form of vitamin D2 and vitamin D3.
How long does vitamin D last in the body?
A major source of vitamin D for most humans comes from exposure of the skin to sunlight typically between 1000 hours and 1500 hours in the spring, summer, and fall. Vitamin D produced in the skin may last at least twice as long in the blood compared with ingested vitamin D.
What is the role of vitamin D in the immune system?
Vitamin D has been described as an immunomodulator targeting various immune cells, including monocytes, macrophages, T-lymphocytes, and B-lymphocytes.5 Studies have suggested that vitamin D plays an important role in maintenance of the immune system.
Where does vitamin D2 and D3 go?
Once in the blood, vitamin D2 and D3 from diet or skin bind with vitamin D binding protein and are carried to the liver where they are hydroxylated to yield calcidiol. Calcidiol then is converted in the kidney to calcitriol by the action of 1a-hydroxylase (CYP27B1).
What is vitamin D deficiency?
Clinical Information. A nutritional condition produced by a deficiency of vitamin d in the diet, insufficient production of vitamin d in the skin, inadequate absorption of vitamin d from the diet, or abnormal conversion of vitamin d to its bioactive metabolites.
When will the ICd 10 E55 be effective?
The 2021 edition of ICD-10-CM E55 became effective on October 1, 2020.
What is vitamin B12 deficiency?
Vitamin b12 deficiency. Clinical Information. A nutritional condition produced by a deficiency of folic acid in the diet. Many plant and animal tissues contain folic acid, abundant in green leafy vegetables, yeast, liver, and mushrooms but destroyed by long-term cooking.
What is vitamin B12?
A nutritional condition produced by a deficiency of vitamin b 12 in the diet, characterized by megaloblastic anemia. Since vitamin b 12 is not present in plants, humans have obtained their supply from animal products, from multivitamin supplements in the form of pills, and as additives to food preparations.
Does alcohol affect the absorption of folic acid?
Alcohol interferes with its intermedi ate metabolism and absorption. Folic acid deficiency may develop in long-term anticonvulsant therapy or with use of oral contraceptives. This deficiency causes anemia, macrocytic anemia, and megaloblastic anemia.
Popular Posts:
- 1. icd 10 diagnosis code for rotator cuff tear right
- 2. icd 9 code for status post cervical discectomy
- 3. icd 10 code for 10 weeks gestation
- 4. what is the icd-10-cm code assigned for: acute angle closure glaucoma
- 5. icd-10 code for bactrial conjunctivits
- 6. icd 10 code for young teenage mother
- 7. what is the icd 10 code for mature mediastinal teratoma
- 8. icd 10 code for left breast mass at 11 o'clock
- 9. icd 10 code for long term use of testosterone
- 10. icd-10 code for nph lesion