Table 1: Dry Age-Related Macular Degeneration (AMD)
| Right Eye | Left Eye | Bilateral | |
| Dry (nonexudative) AMD, early dry stage | H35.31 11 | H35.31 21 | H35.31 31 |
| Dry (nonexudative) AMD, intermediate dry ... | H35.31 12 | H35.31 22 | H35.31 32 |
| Dry (nonexudative) AMD, advanced atrophi ... | H35.31 13 | H35.31 23 | H35.31 33 |
| Dry (nonexudative) AMD, advanced atrophi ... | H35.31 14 | H35.31 24 | H35.31 34 |
How do you cure macular degeneration?
Oct 01, 2021 · This is the American ICD-10-CM version of H35.30 - other international versions of ICD-10 H35.30 may differ. ICD-10-CM Coding Rules H35.30 is applicable to adult patients aged 15 - 124 years inclusive. Applicable To Age-related macular degeneration The following code (s) above H35.30 contain annotation back-references
Is it possible to cure macular degeneration?
6 rows · When you use the codes for dry AMD (H35.31xx) and wet AMD (H35.32xx), you must use the sixth ...
Would macular degeneration be considered legally blind?
Oct 01, 2021 · 2022 ICD-10-CM Diagnosis Code H35.3112 Nonexudative age-related macular degeneration, right eye, intermediate dry stage 2017 - New Code 2018 2019 2020 2021 2022 Billable/Specific Code Adult Dx (15-124 years) H35.3112 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
Can an optometrist treat macular degeneration?
Oct 01, 2021 · Nonexudative age-related macular degeneration, right eye, advanced atrophic with subfoveal involvement. H35.3114 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM H35.3114 became effective on October 1, 2021.
What is the ICD-10-CM code for cystoid macular degeneration bilateral eyes?
ICD-10 code H35. 35 for Cystoid macular degeneration is a medical classification as listed by WHO under the range - Diseases of the eye and adnexa .
What is the ICD-10 code for blind right eye?
2022 ICD-10-CM Diagnosis Code H54. 0X5: Blindness right eye, category 5.
What is the ICD-10 code for blind in left eye?
2022 ICD-10-CM Diagnosis Code H54. 12: Blindness, left eye, low vision right eye.
What is exudative age related macular degeneration?
Exudative macular degeneration is a progressive eye disease that affects the macula or central part of the retina. It causes the eye to develop leaky blood vessels behind the macula, the part of the eye that enables us to see what is straight in front of us.Nov 29, 2021
What is the ICD-10 code for macular degeneration?
H35.30Unspecified macular degeneration H35. 30 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is blindness right eye Category 5?
Table 1Category of visual impairmentVisual acuity with best possible correctionClassified as26/60 1/10 (0.1) 20/200Low vision33/60 1/20 (0.05) 20/400Blindness41/60 (finger counting at 1 metre) 1/50 (0.02) 5/300Blindness5No light perceptionBlindness4 more rows•Mar 16, 2006
What is the ICD-10 code for blind in both eyes?
2022 ICD-10-CM Diagnosis Code H54. 0: Blindness, both eyes.
What is Category 3 blindness?
If “blindness” or “low vision” in one eye is documented but the visual impairment category is not documented, assign a code from H54. 6-, Unqualified visual loss, one eye....Looking at new ICD-10-CM Codes for Blindness.CategoryWorse than:Equal to or better than:Blindness 33/60 1/20 (0.5) 20/4001/60* 1/50 (0.02) 5/300 (20/1200)6 more rows•Sep 25, 2017
What is the diagnosis code for blindness?
H54.0ICD-10-CM Code for Blindness, both eyes H54. 0.
What is the difference between exudative and Nonexudative age-related macular degeneration?
Greater than 90% of patients diagnosed with AMD have nonexudative (dry) AMD; nonexudative AMD is generally associated with much slower (over decades), progressive visual loss compared with exudative (wet) AMD, which is generally associated with more rapid (over months) visual loss.Jul 16, 2021
What is non exudative?
The hallmark of the dry, or nonexudative form, is the deposition of extracellular material beneath the retinal pigment epithelium (RPE) that leads to the formation of drusen. Both atrophic and hypertrophic changes occur in the RPE underlying the central macula and can lead to the loss of retinal photoreceptors.Jun 24, 2021
What causes Metamorphopsia?
[1] suggested that metamorphopsia is not only caused by displacement of retinal layers resulting in mislocation of light on the retina, but also by the combination of retinal changes with cortical processing, mainly after long-standing maculopathy or after treatment of macular disorders (as neovascular AMD).Nov 11, 2015
Coding For Laterality in AMD
When you use the codes for dry AMD (H35.31xx) and wet AMD (H35.32xx), you must use the sixth character to indicate laterality as follows:1 for the...
Coding For Staging in Dry AMD
The codes for dry AMD—H35.31xx—use the seventh character to indicate staging as follows:H35.31x1 for early dry AMD—a combination of multiple small...
Defining Geographic Atrophy
When is the retina considered atrophic? The Academy Preferred Practice Pattern1 defines GA as follows:The phenotype of central geographic atrophy,...
Coding For Geographic Atrophy
The Academy recommends that when coding, you indicate whether the GA involves the center of the fovea: Code H35.31x4 if it does and H35.31x3 if it...
Coding For Staging in Wet AMD
The codes for wet AMD—H35.32xx—use the sixth character to indicate laterality and the seventh character to indicate staging as follows:H35.32x1 for...
What is bilateral designation?
If the same disease stage is present in both eyes, use the bilateral designation (3) regardless of whether 1 or both eyes are being treated. The treatment code should indicate which eye is being treated.
What is central geographic atrophy?
The phenotype of central geographic atrophy, the advanced form of non-neovascular AMD, will have 1 or more zones of well- demarcated RPE and/or choriocapillaris atrophy. Drusen and other pigmentary abnormalities may surround the atrophic areas.
Can an inactive scar be a CNV?
Similarly, an eye that has an inactive scar could have active CNV after the diagnosis of an inactive scar, and treatment can be considered at the time of active CNV. 1 American Academy of Ophthalmology Retina/Vitreous Panel. Preferred Practice Pattern Guidelines: Age-Related Macular Degeneration.
Does GA affect the fovea?
GA often spares the fovea until late in the course of the disease. It may first present as 1 or more noncontiguous patches of atrophy around the fovea. These patches enlarge and coalesce and may be associated with a dense paracentral scotoma, thereby limiting tasks such as reading.
What is the ICd code for macular degeneration?
Code is only used for patients 15 years old or older. H35.30 is a billable ICD code used to specify a diagnosis of unspecified macular degeneration. A 'billable code' is detailed enough to be used to specify a medical diagnosis.
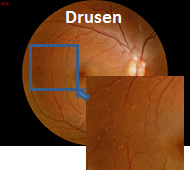
What is the ICd code for drusen?
The ICD code H353 is used to code Drusen. Drusen (singular, "druse") are tiny yellow or white accumulations of extracellular material that build up between Bruch's membrane and the retinal pigment epithelium of the eye. The presence of a few small ("hard") drusen is normal with advancing age, and most people over 40 have some hard drusen.
Is it normal to have a few hard drusen?
The presence of a few small ("hard") drusen is normal with advancing age, and most people over 40 have some hard drusen. However, the presence of larger and more numerous drusen in the macula is a common early sign of age-related macular degeneration (AMD).

Popular Posts:
- 1. icd 10 code for ovarian follicles
- 2. icd 10 code for epipen
- 3. icd-10-cm code for cataract of right eye
- 4. icd 10 code for chronic paranoia
- 5. icd 10 code for asthmatic breathing
- 6. icd 10 code for side effects of medication
- 7. icd 10 code for brachial neuritis or radiculitis
- 8. what is the icd-10 code for av dialysis fistula
- 9. icd 10 code for dressing wound
- 10. icd 10 code for leg cramping unspecified