ICD 10 Code for Back Pain/Backache 724.5 back pain only (Converts to M54.9 ICD-10 Code) 724.1 Upper/Middle back pain (Converts to M54.6 ICD-10 Code) 724.2 Lower back pain or lumbago (Converts to M54.5 ICD-10 Code)
What does pain in the lower back indicate?
What Does Lower Back Pain Mean? At its most basic level, lower back pain means that you are having an inflammatory response to some sort of injury within the lower portion of your back. Sometimes it happens if you’ve strained a muscle after a workout, or maybe you’ve picked something up that’s too heavy and there’s a twinge that turns ...
What is the ICD 10 code for low back pain?
- M54.5 is a billable/specific ICD-10-CM code that can be used to for reimbursement purposes.
- Low back pain ICD-10-CM M54.5 became effective on October 1, 2020.
- This is the American ICD-10-CM version of M54.5 – other international versions of ICD-10 M54.5 may differ.
What is the diagnosis code for lower back pain?
What are some common causes of lower back pain?
- Arthritis of the Spine. Arthritis of the spine — the slow degeneration of the spinal joints — is the most frequent cause of lower back pain.
- Back Injuries. A bad fall or a car accident can cause a lower back injury. ...
- Herniated Discs. A herniated, or bulging, disc is a disc that has “spilled out” of its lining. ...
Do you have mid back pain?
What is it? Mid-back pain can be a sign of pancreatic cancer. The pain can be caused by a tumour invading nerves or organs that lie near the pancreas. Some people also report that they feel pain in their shoulder or under their shoulder blade. Other people feel pain in their back and abdomen (tummy) at the same time.
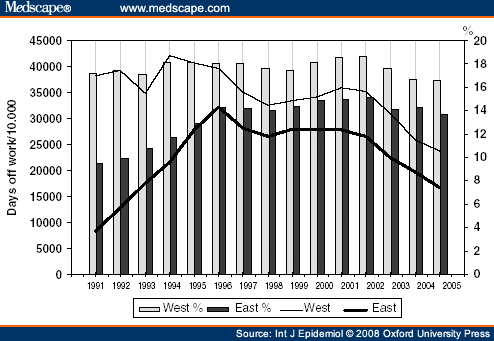
What is the ICD 10 code for middle back pain?
ICD-10 code M54. 6 for Pain in thoracic spine is a medical classification as listed by WHO under the range - Dorsopathies .
What is ICD 10 code for chronic midline low back pain without sciatica?
5 - Low back pain is a sample topic from the ICD-10-CM. To view other topics, please log in or purchase a subscription. ICD-10-CM 2022 Coding Guide™ from Unbound Medicine.
What code can I use instead of M54 5?
Here are some potential code replacements that you can use beginning October 1: S39. 012, Low back strain. M51.
Is M54 5 and M54 50 the same?
The current code, M54. 5 (Low back pain), will be expanded into three more specific codes: M54. 50 (Low back pain, unspecified)
When do you use M54 51?
The new diagnosis code – M54. 51 – went into effect on October 1, 2021. This code will be applied to patients meeting indications for treatment with basivertebral nerve radiofrequency neurotomy.
What does diagnosis code M54 9 mean?
9: Dorsalgia, unspecified.
What is M54 5 low back pain?
ICD-Code M54. 5 is a billable ICD-10 code used for healthcare diagnosis reimbursement of chronic low back pain. Its corresponding ICD-9 code is 724.2. Code M54.
What is diagnosis code M54 6?
6: Pain in thoracic spine.
Is M54 50 a valid diagnosis code?
M54. 50 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
When do you use M54 59?
M54. 59, other low back pain is used for lower back pain that can be attributed to a specific reason but there is not an applicable code available that describes or defines it. (You can name it but it is does not have its own specific code (i.e. facet syndrome.)
What does diagnosis code M54 2 mean?
ICD-9 Code Transition: 723.1 Code M54. 2 is the diagnosis code used for Cervicalgia (Neck Pain). It is a common problem, with two-thirds of the population having neck pain at some point in their lives.
Is M54 2 still valid?
M54. 2 is a billable/specific ICD-10-CM code used for Cervicalgia (Neck Pain). The 2021 edition of ICD-10-CM M54. 2 became effective on October 1, 2020.
What is the ICD-10 for chronic low back pain?
5 – Low Back Pain. ICD-Code M54. 5 is a billable ICD-10 code used for healthcare diagnosis reimbursement of chronic low back pain.
What is the ICD-10-CM code for chronic back pain?
M54. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What does diagnosis code M54 2 mean?
ICD-9 Code Transition: 723.1 Code M54. 2 is the diagnosis code used for Cervicalgia (Neck Pain). It is a common problem, with two-thirds of the population having neck pain at some point in their lives.
Can M54 50 be a primary diagnosis code?
M54. 50 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the term for pain in the lower back?
Sciatica – Pain which radiates down to one or both the legs from the lower back caused due to compression of the sciatic nerve by a herniated disk or a bone spur. Lumbago- The medical term for low back pain.
What is back pain called?
Back pain, medically called Dorsalgia is a very common physical discomfort affecting 8 out of 10 people both young and the old. The pain can be in the cervical, cervicothoracic, thoracic, thoracolumbar, Lumbar or lumbosacral regions. It can be felt as a dull, persistent ache or a sudden sharp pain.
Which region of the spine is curved slightly inwards and made of 5 vertebrae?
Lumbar region – The lower back region of the spine which is curved slightly inwards and made of 5 vertebrae (L1-L5). Lumbosacral region – The region connecting the last lumbar vertebrae to the sacrum which is made of 5 bones fused together.
How long does back pain last?
Chronic back pain – Back pain is said to be chronic if it is a constant nagging pain usually lasting for more than 3-6 months duration, which begins to affect the daily routine of the person.
Which region of the spine extends from the base of the neck to the abdomen?
Thoracic region – The longest region of the spine which extends from the base of the neck to the abdomen. It comprises of 12 vertebrae (T1 to T12).
Is back pain a symptom of a disease?
Back pain being a symptom of an underlying disease in most cases is coded only in the absence of a confirmed diagnosis of an underlying condition like intervertebral disc disorders, traumatic disc fracture, muscle strain etc..
What is the ICd 10 code for back pain?
The ICD 10 code M545 is used to define conditions connected with acute back pain (C & O lumbar pain, C & O back pain, or chronic back pain) or complaints about back pain or facet or joint pain. This code is used in common practice, internal medicine, and orthopedic works to define clinical ideas such as neck pain. Like the billable ICD 10 code, M545 is also used for medical diagnosis and compensation of chronic back pain.
Why does my back hurt?
The main cause of back pain may be an issue with the back itself or a problem with a different part of the body. Degenerative arthritis is a wear and tear method compared with age, injury, or genetic choice. Infection of intervertebral disc space within bones (osteomyelitis) in the abdomen or pelvis or bloodstream.
Can you code lumbar radiculopathy as M5416?
The instruction for ICD 10 CM states that if the problem of pain is known, the code is committed to the underlying diagnosis, not the pain code if the problem is known. For instance, if we encode lumbar radiculopathy as M5416, you can not allow M545 (lumbar pain) to this code. Although we report Radicullopathy as an ICD 10 code, we do not report the code for back pain.
What does it mean when you feel a bad feeling in your back?
Sensation of unpleasant feeling indicating potential or actual damage to some body structure felt in the back.
How long does back pain last?
Acute back pain comes on suddenly and usually lasts from a few days to a few weeks. Back pain is called chronic if it lasts for more than three months. most back pain goes away on its own, though it may take awhile.
How long does it take for back pain to go away?
If your back pain is severe or doesn't improve after three days, you should call your health care provider. You should also get medical attention if you have back pain following an injury.treatment for back pain depends on what kind of pain you have, and what is causing it.
When will the ICd 10-CM M54.9 be released?
The 2022 edition of ICD-10-CM M54.9 became effective on October 1, 2021.
Where is chronic pain located?
Acute or chronic pain located in the posterior regions of the thorax, lumbosacral region, or the adjacent regions.
What is the ICd 9 code for back pain?
ICD-9CM codes are used in medical billing and coding to describe diseases, injuries, symptoms and conditions. ICD-9CM 724.5 for backpain is one of the thousands of ICD-9 codes used in healthcare documentation.
What is the medical term for back pain?
Low back pain, backache, lumbago or lumbar pain is a common disorder involving the muscles and bones of the back. Low back pain is often abbreviated as LBP.
How long does back pain last?
Acute back pain comes on suddenly and usually lasts from a few days to a few weeks. The clinical definition of back pain is: A backache (back pain) is a disorder characterized by marked discomfort sensation in the back region. Back pain is called chronic if it lasts for more than three months. It can be an acute or chronic pain located in ...
How to treat back pain?
It might incorporate hot or cool packs, exercise, pharmaceuticals, infusions, reciprocal medicines, and in some cases surgery.
How long can you stay in bed with back pain?
Be that as it may, staying in bed for more than 1 or 2 days can aggravate it. In the event that your back pain is serious or doesn't enhance following three days, you ought to call your medicinal services supplier.
Where is back pain located?
It can be an acute or chronic pain located in the posterior regions of the thorax, lumbosacral region, or the adjacent regions. Most back pain leaves all alone, however, it might take a little while. Assuming control over-the-counter pain relievers and resting can offer assistance.
When to use ICD-10 code 724.5?
However, 724.5 should only be used for claims with a date of service on or before September 30, 2015. For claims with a date of service on or after October 1, 2015, use an equivalent ICD-10CM code.
When did the ICd 10 change to M54.5?
This August, CMS published its latest round of ICD-10 changes—including the deletion of ICD-10 code M54.5, low back pain, effective October 1, 2021.
Why is CMS deleting M54.5?
So, here’s the real question: How the heck can CMS justify deleting such a commonly used code? Well, CMS has explained that it’s deleting M54.5 because it lacks specificity (and we all know how important coding specificity is to ICD-10). To supplement this low back coding deletion, CMS suggested that providers use other, more specific codes—some which you may recognize, and some of which are totally new. Here are some potential code replacements that you can use beginning October 1:
Is the BCBS diagnosis a primary diagnosis?
No, oddly enough it was mainly Medicare and BCBS... It wasn't the primary diagnosis so I just deleted the code from the claim.
Popular Posts:
- 1. icd 10 code for decreased fine motor skills
- 2. icd 9 code for fractured leg
- 3. icd 10 code for macular thickness
- 4. icd 10 code for right radial artery thrombosis
- 5. icd-10 code for pvd with claudisma
- 6. icd 10 code for herpetic pharyngotonsillitis
- 7. icd 10 code for fracture right hand
- 8. icd 10 code for dm with macular edema
- 9. diagnosis icd-10 code for patellofemoral chondromalaleftcia.
- 10. icd 10 code for abnormal mch