What is the ICD 10 code for retinopathy of the eye?
proliferative E11.359. ICD-10-CM Codes Adjacent To E11.359. E11.354 Type 2 diabetes mellitus with proliferative diabetic retinopathy with combined traction retinal detachment and rhegmatogenous retinal detachment.
What is the ICD 10 for diabetic retinopathy without macular edema?
Type 2 diabetes mellitus with proliferative diabetic retinopathy without macular edema. The 2019 edition of ICD-10-CM E11.359 became effective on October 1, 2018. This is the American ICD-10-CM version of E11.359 - other international versions of ICD-10 E11.359 may differ. All neoplasms, whether functionally active or not,...
What is the latest ICD 10 for type 2 diabetes mellitus?
Type 2 diabetes mellitus with proliferative diabetic retinopathy without macular edema. The 2019 edition of ICD-10-CM E11.359 became effective on October 1, 2018. This is the American ICD-10-CM version of E11.359 - other international versions of ICD-10 E11.359 may differ.
What is the new ICD 10 for neoplasm?
The 2022 edition of ICD-10-CM E11.359 became effective on October 1, 2021. This is the American ICD-10-CM version of E11.359 - other international versions of ICD-10 E11.359 may differ. All neoplasms, whether functionally active or not, are classified in Chapter 2.
What is PDR of the eye?
PDR (proliferative diabetic retinopathy) PDR is the more advanced stage of diabetic eye disease. It happens when the retina starts growing new blood vessels. This is called neovascularization. These fragile new vessels often bleed into the vitreous.
What is NPDR and PDR?
As the disease progresses, it may evolve into proliferative diabetic retinopathy (PDR), which is defined by the presence of neovascularization and has a greater potential for serious visual consequences. NPDR – Hyperglycemia results in damage to retinal capillaries.
Does NPDR progress to PDR?
A total of 4,617 beneficiaries with NPDR were eligible for the study. Of those eligible, 307 (6.7%) progressed from NPDR to PDR. The median length of time enrollees were followed from the index date was 1.7 years.
What is background retinopathy?
Stage 1: background retinopathy This means that tiny bulges (microaneurysms) have appeared in the blood vessels in the back of your eyes (retina), which may leak small amounts of blood. This is very common in people with diabetes.
What is PDR surgery?
The role of vitrectomy in the management of proliferative diabetic retinopathy (PDR) is complex and may include several of the following goals: removal of visually significant vitreous opacities, release of anteroposterior or tangential traction, removal of fibrovascular proliferation (FVP), and use of endolaser ...
Is diabetic retinopathy bilateral?
Diabetic retinopathy usually affects both eyes.
What is clinically significant macular edema?
Clinically-significant macular edema (CSME) [3] is defined as one or more of the following: retinal thickening at or within 500 μm of the center of the macula; hard exudates at or within 500 μm of the center of the macula, if associated with adjacent retinal thickening; or a zone or zones of retinal thickening one disc ...
What is prolific diabetic retinopathy?
What is proliferative diabetic retinopathy (PDR)? ANSWER. If you continue to have high blood sugar over several years, you could go on to have a more severe eye disease known as proliferative diabetic retinopathy. It's called "proliferative" because new blood vessels start to grow on the surface of the retina.
What does NPDR stand for in ophthalmology?
Non-Proliferative Diabetic Retinopathy (NPDR) Vision Simulator - American Academy of Ophthalmology.
What is the ICD 10 code for background diabetic retinopathy?
362.01 - Background diabetic retinopathy | ICD-10-CM.
What is the difference between maculopathy and retinopathy?
The macula helps you see color, fine details, and distant objects. It sends information to the brain that gets interpreted into images. It's needed for everything from recognizing faces to reading. Diabetic retinopathy causes DME when the retina can no longer absorb the fluids from those leaky blood vessels.
Is background diabetic retinopathy the same as nonproliferative?
Background diabetic retinopathy, also known as non-proliferative diabetic retinopathy (NPDR), is the early stage of diabetic retinopathy. This occurs when diabetes damages the small blood vessels and nerves in the retina. The retina acts like the film of the eye.
What does NPDR stand for?
Definition: Non-proliferative diabetic retinopathy (NPDR) is the most common form of diabetic retinopathy. Early stages consist of edema and hard exudates, lipid that has leaked from abnormal blood vessels, in the central retina, resulting in blurred central vision.
What is diabetic macular edema DME?
Diabetic macular edema (DME) is manifested as retinal thickening caused by the accumulation of intraretinal fluid, primarily in the inner and outer plexiform layers. It is believed to be a result of hyperpermeability of the retinal vasculature. DME can be present with any level of diabetic retinopathy.
Why is vitrectomy performed?
Vitrectomy is a surgical procedure undertaken by a specialist where the vitreous humor gel that fills the eye cavity is removed to provide better access to the retina. This allows for a variety of repairs, including the removal of scar tissue, laser repair of retinal detachments and treatment of macular holes.
Can NPDR be reversed?
Can DR be treated/reversed? Fortunately, diabetic retinopathy is preventable and also treatable. Maintaining blood sugar at an optimal level can help to prevent this serious condition. As controlled diabetes can also lead to diabetic retinopathy, it is advised to have your eyes examined regularly.
When did the ICD-10 code for diabetic retinopathy go into effect?
On Oct. 1, thousands of new and revised ICD-10 codes go into effect, including 368 that are relevant to ophthalmology. This article focuses on changes to the diabetic retinopathy and age-related macular degeneration (AMD) codes.
What is the code for diabetes mellitus?
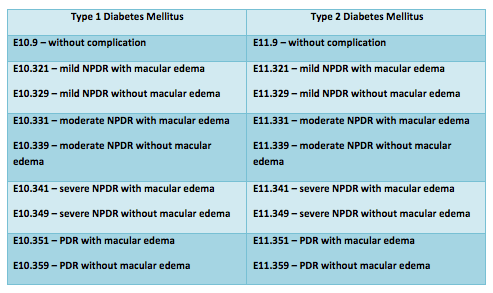
And you still use the same codes to indicate diabetes mellitus with no complications—E10.9 for type 1 and E11.9 for type 2 —and those 2 codes don’t have laterality.
When is laterality required for AMD?
After Oct. 1, laterality is required when coding for AMD, in addition to staging. Unlike diabetes, the eye indicator is in the sixth position (see red numerals in Tables 3 and 4) and staging is in the seventh position (see green numerals in Tables 3 and 4 ).
Is ophthalmology a transition to ICD-9?
Based on feedback from physicians and practice managers at Academy Codequest Coding Courses, ophthalmology seems to have been well prepared for the initial transition from ICD-9. As ICD-10 evolves, the Academy and AAOE will continue to support their members with a comprehensive range of resources, including:

Popular Posts:
- 1. icd 10 code for pikloderma
- 2. icd 10 code for dermatitis buttocks
- 3. icd 9 code for acute non st segment elevation myocardial infarction
- 4. what is the icd-9-cm code for a closed fracture of the wrist?
- 5. what is the icd 10 code for sebaceous epithelioma
- 6. icd 10 code for need for assistance
- 7. icd 10 code for open wound left middle finger
- 8. icd 10 code for medically refractory epilepsy
- 9. icd-10-pcs 2017 code for median sternotomy incision
- 10. icd-9-cm code for hypokalemia