What is the ICD 10 code for right knee pain?
Right knee pain ICD-10-CM M25.561 is grouped within Diagnostic Related Group (s) (MS-DRG v38.0): 555 Signs and symptoms of musculoskeletal system and connective tissue with mcc 556 Signs and symptoms of musculoskeletal system and connective tissue without mcc
What is the ICD 10 code for total knee replacement?
The appropriate codes for this scenario, according to this presentation, would be: ICD-10: Z96.651, Status (post), organ replacement, by artificial or mechanical device or prosthesis of, joint, knee-see presence of knee joint implant
What is the ICD 10 code for presence of right artificial knee?
Presence of right artificial knee joint. Z96.651 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2019 edition of ICD-10-CM Z96.651 became effective on October 1, 2018.
What is the ICD-10 code for postoperative gait following knee replacement surgery?
The appropriate codes for this scenario, according to this presentation, would be: 1 ICD-10: Z47.1, aftercare following surgery for joint replacement 2 ICD-10: Z96.651, Status (post), organ replacement, by artificial or mechanical device or prosthesis of, joint, knee-see presence of knee joint implant 3 ICD-10: R26.9 Abnormality, gait
What is the ICD-10 code for post surgical Pain?
18.
What is the ICD-10-CM code for right knee pain?
M25. 561 Pain in right knee - ICD-10-CM Diagnosis Codes.
What is the ICD-10 code for aftercare following orthopedic surgery?
ICD-10-CM Code for Encounter for other orthopedic aftercare Z47. 89.
What is the ICD-10 code for knee surgery?
Presence of artificial knee joint, bilateral The 2022 edition of ICD-10-CM Z96. 653 became effective on October 1, 2021. This is the American ICD-10-CM version of Z96.
What is the ICD 9 code for right knee pain?
Convert ICD-9-CM Diagnosis 719.46 to ICD-10-CM.
What is the ICD-10 code for injury to knee?
Superficial injury of knee and lower leg ICD-10-CM S80. 912A is grouped within Diagnostic Related Group(s) (MS-DRG v39.0):
What is the ICD-10 code for status post surgery?
ICD-10-CM Code for Encounter for surgical aftercare following surgery on specified body systems Z48. 81.
What is considered orthopedic aftercare?
Z aftercare codes are used in office follow-up situations in which the initial treatment of a disease is complete and the patient requires continued care during the healing or recovery phase or for long-term consequences of the disease.
What is the ICD-10 code for orthopedic?
Encounter for other orthopedic aftercare Z47. 89 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM Z47. 89 became effective on October 1, 2021.
What is the ICD-10 code for status post total knee arthroplasty?
ICD-10: Z96. 651, Status (post), organ replacement, by artificial or mechanical device or prosthesis of, joint, knee-see presence of knee joint implant.
What is right total knee arthroplasty?
Knee replacement, also called knee arthroplasty or total knee replacement, is a surgical procedure to resurface a knee damaged by arthritis. Metal and plastic parts are used to cap the ends of the bones that form the knee joint, along with the kneecap.
What is the ICD-10 code for right knee arthroscopy?
In ICD-10-PCS, arthroscopy goes to the root operation “inspection,” which is defined as visually and/or manually exploring a body part. Therefore, an arthroscopy of the right knee is classified to code 0SJC4ZZ, and arthroscopy of the left knee is classified to code 0SJD4ZZ.
Symptoms and Causes
Knee pain can be mild, moderate or severe. The reasons for pain can vary such as injury, overuse, infection and inflammation. Sometimes there may be swelling and redness depends on the cause. We need to visit doctor as per the severity and as per how long the pain lasts.
Tests and Diagnosis
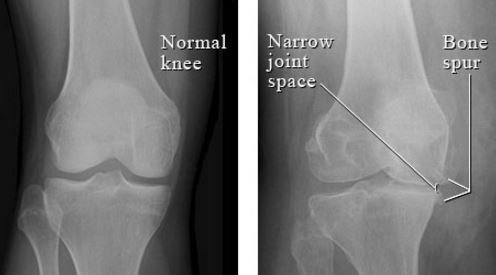
Physician will do extremity examination to check if there is any swelling, inflammation or injury. There may be need of radiological tests (X-ray, CT, MRI, ultrasound) or arthrocentesis (lab analysis of knee joint fluid) for further evaluation to check for infections or injury to tendon or ligament.
ICD 10 Code for Knee Pain and guidelines
ICD 10 Code for knee pain is found in chapter 13 of ICD-10 CM manual – diseases of musculoskeletal system and connective tissue, code range M00 – M99
What is the code for postoperative pain?
Postoperative pain not associated with a specific postoperative complication is reported with a code from Category G89, Pain not elsewhere classified, in Chapter 6, Diseases of the Nervous System and Sense Organs. There are four codes related to postoperative pain, including:
Is postoperative pain a part of recovery?
Postoperative pain typically is considered a normal part of the recovery process following most forms of surgery. Such pain often can be controlled using typical measures such as pre-operative, non-steroidal, anti-inflammatory medications; local anesthetics injected into the operative wound prior to suturing; postoperative analgesics;
Is postoperative pain normal?
Determining whether to report postoperative pain as an additional diagnosis is dependent on the documentation, which, again, must indicate that the pain is not normal or routine for the procedure if an additional code is used. If the documentation supports a diagnosis of non-routine, severe or excessive pain following a procedure, it then also must be determined whether the postoperative pain is occurring due to a complication of the procedure – which also must be documented clearly. Only then can the correct codes be assigned.
Is postoperative pain a reportable condition?
Only when postoperative pain is documented to present beyond what is routine and expected for the relevant surgical procedure is it a reportable diagnosis. Postoperative pain that is not considered routine or expected further is classified by whether the pain is associated with a specific, documented postoperative complication.
What is the ICd 10 code for post thoracotomy pain?
Category G89 contains four codes for acute and chronic post-thoracotomy pain (G89.12, G89.22) and other postprocedural pain (G89.18, G89.28). The ICD-10-CM guidelines state that you should not code “routine or expected postoperative pain immediately after surgery.” Additionally, in order to assign these codes, the physician must document that the patient’s pain is a complication of the surgery.
What is R07.81 pain?
Pleurodynia (R07.81): Spasms of pain in the intercostal muscles, which can be a sign of pleurisy (inflammationof the pleural membranes). Intercostal pain (R07.82): This is pain originating in the intercostal nerves, which run between pairs of adjacent ribs.
What is the ICD-10 code for chest pain?
The ICD-10-CM Index refers you to the code for angina (I20.9) when the patient’s chest pain is described as “ischemic.” However, other types of chest pain are reported with codes from category R07 (Pain in throat and chest). There is an exception for post-thoracotomy pain, which we’ll discuss later.
What is the code for flank pain?
You must code flank pain as unspecified abdominal pain (R10.9) unless the physician provides additional information about the location of the pain, such as whether it is in the upper or lower portion of the abdomen. Pelvic pain is classified to code R10.2 (Pelvic and perineal pain).
What is the code for abdominal pain?
In addition to the codes for pain in the various parts of the abdomen, there are codes for: Acute abdomen (R10.0): This is sudden, severe abdominal pain, often accompanied by rigidity of the abdomen.
What is the G89 code?
For example, you can assign a G89 code to indicate that the pain is acute or chronic. You should assign the site-specific pain code first unless the purpose of the encounter is pain management, in which case the G89 code is first. For example, a patient is referred for ankle x-rays for chronic right ankle pain.
Do you need a re-evaluation after surgery?
In many cases, yes; a patient who undergoes surgery mid-plan of care should receive a re-evaluation. However, per the above-linked article, "some commercial payers may consider the post-op treatment period a new episode of care, in which case you’d need to use an evaluation code.".
Can you use aftercare codes with injury codes?
Essentially, you are indicating that the patient is receiving aftercare for the injury. Thus, you should not use aftercare codes in conjunction with injury codes, because doing so would be redundant. 3. You can use Z codes to code for surgical aftercare.
Do therapists use ICD-10 aftercare codes?
Even so, therapists should only use ICD-10 aftercare codes to express patient diagnoses in a very select set of circumstances.
Popular Posts:
- 1. icd 10 code for nasal septum abrasion
- 2. icd code 10 for aki
- 3. icd 10 code for traumatic effusion left elbow joint
- 4. what is the icd 10 code for diabetic neuropathy
- 5. assign the icd-10-cm code for self-defeating personality disorder.
- 6. icd 10 code for peritoneal dialysis associated peritonitis
- 7. icd 9 code for hepatitis c
- 8. icd 10 code for alcohol induced gastritis
- 9. icd 10 code for hypercotoidilim
- 10. icd 10 procedure code for thoractomy with resection of left lower lobe of lung