What are the new ICD 10 codes?
The new codes are for describing the infusion of tixagevimab and cilgavimab monoclonal antibody (code XW023X7), and the infusion of other new technology monoclonal antibody (code XW023Y7).
What ICD 10 cm code(s) are reported?
What is the correct ICD-10-CM code to report the External Cause? Your Answer: V80.010S The External cause code is used for each encounter for which the injury or condition is being treated.
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
What does ICD 10 mean?
ICD-10 is the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD), a medical classification list by the World Health Organization (WHO). It contains codes for diseases, signs and symptoms, abnormal findings, complaints, social circumstances, and external causes of injury or diseases.
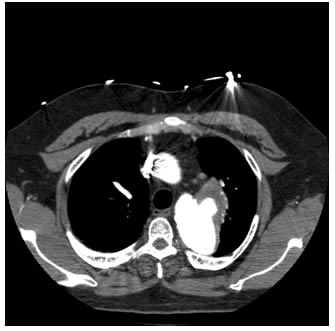
How do you code pseudoaneurysm?
It is important to note that if treating a rupture that is considered chronic, and if contained would be considered a pseudoaneurysm. As such, codes 34701, 34703, 34705, or 34707 would be assigned instead of the codes for “rupture.”
What is a ruptured pseudoaneurysm?
A rupture carries a risk of internal bleeding that can be life-threatening. A pseudoaneurysm is due to an artery injury that pierces the wall of a blood vessel. The opening in the blood vessel allows blood to leak out and pool in the surrounding tissue.
What is the difference between an aneurysm and a pseudoaneurysm?
A saccular-shaped aneurysm bulges or balloons out only on one side. A pseudoaneurysm, or false aneurysm, is not an enlargement of any of the layers of the blood vessel wall. A false aneurysm may be the result of a prior surgery or trauma. Sometimes, a tear can occur on the inside layer of the vessel.
What is a pseudoaneurysm?
A pseudoaneurysm, or pseudoaneurysm of the vessels, occurs when a blood vessel wall is injured and the leaking blood collects in the surrounding tissue. It is sometimes called a false aneurysm. In a true aneurysm, the artery or vessel weakens and bulges, sometimes forming a blood-filled sac.
What is the difference between a pseudoaneurysm and a hematoma?
By definition a pseudoaneurysm communicates with the feeding artery. In contrast a hematoma does not have a "neck.” "Yin-Yang” sign – indicates bidirectional flow within the lesion from arterial blood flowing into the lesion, which may resemble its namesake.
What is a femoral artery pseudoaneurysm?
The femoral artery pseudoaneurysm (FAP) is a troublesome groin complication related to the femoral arterial access site used for invasive cardiovascular procedures. 1. FAP occur in 0.1% to 0.2% of diagnostic angiograms and 0.8% to 2.2% following interventional procedures. 2.
Is a pseudoaneurysm a hematoma?
A pseudoaneurysm, also known as a false aneurysm, is a locally contained hematoma outside an artery or heart due to damage to the vessel wall. The injury goes through all the three layers of the arterial wall causing a leak, which is contained by a new weak wall formed by the products of the clotting cascade.
What are the three types of aneurysms?
The three types of cerebral aneurysms are: berry (saccular), fusiform and mycotic. The most common, "berry aneurysm," occurs more often in adults. It can range in size from a few millimeters to more than two centimeters. A family history of aneurysms may increase your risk.
What is a pseudoaneurysm of the aorta?
Pathology. Aortic pseudoaneurysms are contained ruptures of the aorta in which the majority of the aortic wall has been breached, and luminal blood is held in only by a thin rim of the remaining wall or adventitia.
What are the causes of pseudoaneurysm?
What causes a pseudoaneurysm?Cardiac catheterization. ... Trauma. ... Surgical complication. ... Infections. ... Existing aneurysms: Ruptures of existing aneurysms have also been known to cause pseudoaneurysms to develop.
What is a radial artery pseudoaneurysm?
A radial artery pseudoaneurysm represents a rare, potentially catastrophic complication of arterial cannulation that has been reported after cardiac catheterization. Treatment options are limited to chemical, mechanical, and combined approaches to obliterate the radial artery pseudoaneurysm and tract.
What is hepatic artery pseudoaneurysm?
Hepatic artery pseudoaneurysm (HAP) is a rare complication of acute or chronic surgical injury to the hepatic artery. Sethi et al. [1] reported that 19% of pseudoaneurysms due to pancreatitis occur in the hepatic artery.
How long can you live with a pseudoaneurysm?
Methods: 10 patients with postinfarction left ventricular pseudoaneurysm were followed up over a mean (SD) period of 3.8 (5.2) years. Results: In those treated conservatively (n = 9), cumulative survival was 88.9 (10.5)% and 74.1 (16.1)% at one and four years, respectively.
Can a pseudoaneurysm heal on its own?
Some pseudoaneurysms resolve themselves, though others require treatment to prevent hemorrhage, an uncontrolled leak or other complications. An ultrasound study in the Vascular Laboratory may be requested to evaluate a puncture site if swelling, pain or extensive bruising suggests a pseudoaneurysm may have developed.
How long does it take pseudoaneurysm to heal?
How is a pseudoaneurysm diagnosed and treated? Your healthcare provider will use an ultrasound to check the artery for leaking blood. A small pseudoaneurysm may close on its own in about 4 weeks.
What does a pseudoaneurysm look like?
swelling or tenderness in a particular area, especially if you've recently undergone a procedure. a painful mass or lump. a whooshing noise called a bruit that your healthcare provider can hear with a stethoscope, which may suggest a blockage of blood flow through the artery or a narrowing of the blood vessel.
What are the two main treatments for aneurysms?
Medicines and surgery are the two main treatments for aneurysms. Bulging or ballooning in an area of an artery secondary to arterial wall weakening. Pathological outpouching or sac-like dilatation in the wall of any blood vessel (arteries or veins) or the heart (heart aneurysm).
What is the meaning of "G45.-"?
transient cerebral ischemic attacks and related syndromes ( G45.-) aneurysm (of) aorta ( I71.-) An aneurysm is a bulge or "ballooning" in the wall of an artery. Arteries are blood vessels that carry oxygen-rich blood from the heart to other parts of the body.
What is an aneurysm?
Aneurysms are classified by location, etiology, or other characteristics. Pathological, blood-filled distension of blood vessel. Protruding sac in the wall of a vein, artery, or heart, frequently caused by microbial infection; may present as pain, pressure on nearby organs, or cardiac weakening.
Where do aneurysms occur?
Most aneurysms occur in the aorta, the main artery traveling from the heart through the chest and abdomen. Aneurysms also can happen in arteries in the brain, heart and other parts of the body. If an aneurysm in the brain bursts, it causes a stroke. Aneurysms can develop and become large before causing any symptoms.
Popular Posts:
- 1. icd 10 code for dissecting abdominal aortic aneurysm
- 2. icd 10 code for running and fell
- 3. icd 10 code for prophylasix diarrh
- 4. icd-9-cm code for pre-eclampsia complicating pregnancy delivered this admission
- 5. icd-10 code for multiple maxillary incisor fractures avulsion
- 6. icd 10 code for contact lens wearer
- 7. icd 10 code for mild intermittent asthma,
- 8. what is the correct icd-10-cm diagnosis code for impetigo, unspecified?
- 9. icd 10 code for hypertension in newborn
- 10. icd-10 code for bilateral aphakia