What is the ICD - 10 code for fusion?
- Cervical—7
- Thoracic—12
- Lumbar—5
- Sacrum—5 (sometimes 6)
- Coccyx—4
What ICD 10 cm code(s) are reported?
What is the correct ICD-10-CM code to report the External Cause? Your Answer: V80.010S The External cause code is used for each encounter for which the injury or condition is being treated.
What is the diagnosis code for cervical fusion?
Cervical Posterior Decompression with Fusion— Single Level** 22590, 22595, 22600 Cervical Posterior Decompression (for single level fusion) 63001, 63020, 63040, 63045, 63050 Instrumentation: +22840, +22841 Bone Grafts: +20930, +20931, +20936, +20937 Cervical Posterior Decompression with Fusion— Multiple Levels **
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
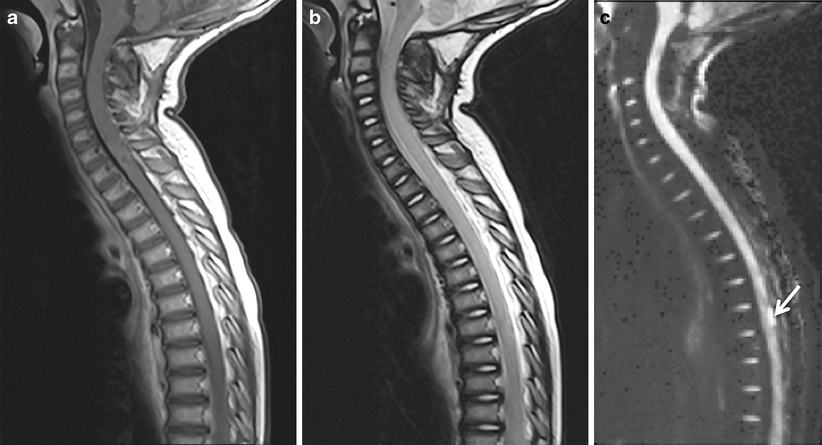
What is ICD-10 code for SP lumbar fusion?
ICD-10 code M43. 26 for Fusion of spine, lumbar region is a medical classification as listed by WHO under the range - Dorsopathies .
What is the ICD-10 code for status post spinal surgery?
Other specified postprocedural states The 2022 edition of ICD-10-CM Z98. 89 became effective on October 1, 2021.
What is the ICD-10 code for anterior cervical discectomy and fusion?
Using the International Classification of Diseases, Ninth Revision, Clinical Modification diagnosis and treatment codes, discharges were identified for those patients undergoing ACDF (defined as anterior cervical fusion (ICD-0 code=81.02) + excision of intervertebral disc (80.51)).
What is S P fusion?
Spinal fusion is surgery to permanently connect two or more vertebrae in your spine, eliminating motion between them. Spinal fusion involves techniques designed to mimic the normal healing process of broken bones.
What is the ICD 10 code for post surgery?
Encounter for other specified surgical aftercare Z48. 89 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM Z48. 89 became effective on October 1, 2021.
What is the ICD 10 code for SP laminectomy?
M96. 1 - Postlaminectomy syndrome, not elsewhere classified | ICD-10-CM.
What is the CPT code for anterior cervical discectomy and fusion?
Coders should instead report all-encompassing CPT code 22551 (arthrodesis, anterior interbody, including disc space preparation, discectomy, osteophytectomy and decompression of spinal cord and/or nerve roots; cervical below C2) for an anterior cervical discectomy and interbody fusion performed at the same level during ...
What is the ICD-10 code for status post discectomy?
2022 ICD-10-CM Diagnosis Code M96. 1: Postlaminectomy syndrome, not elsewhere classified.
How do you code spinal surgery?
The work of placing the bone graft is included in the arthrodesis/fusion codes. All spinal bone graft codes are add-on codes....3. Choose the appropriate add-on bone graft code with fusion.TypeMorselizedStructuralAllograft (donor bone)+20930+20931Autograft (patient's bone)+20936, +20937+20938Dec 9, 2021
What is spine fusion surgery?
Spinal fusion is surgery to permanently join together two or more bones in the spine so there is no movement between them. These bones are called vertebrae. Abnormal curvature in the spine is known as scoliosis, and generally begins just at the onset of puberty and progresses during the period of rapid growth.
What is spinal fusion called?
Spinal fusion, also called spondylodesis or spondylosyndesis, is a neurosurgical or orthopedic surgical technique that joins two or more vertebrae. This procedure can be performed at any level in the spine (cervical, thoracic, or lumbar) and prevents any movement between the fused vertebrae.
What are the different types of spinal fusion surgery?
Anterior/posterior spinal fusion - the procedure is done from the front and the back. Transforaminal lumbar interbody fusion (TLIF) - Similar to the PLIF, this procedure is also done from the back of the spine. Extreme Lateral Interbody Fusion (XLIF) - an interbody fusion in which the approach is from the side.
What are the codes for spinal fusion?
The codes for the anterior spinal fusion are 0SG00AJ (L4-L5) and 0SG30AJ (L5-S1) . Two codes are also assigned for the posterior spinal fusion, 0SG0071 (L4-L5) and 0SG3071 (L5-S1) . Codes 0SB20ZZ and 0SB40ZZ are also assigned for the discectomy performed at two different levels of the spine. Lastly, code 0QB20ZZ is assigned for the harvesting of the right iliac crest bone graft.
What is the code for interbody fusion?
If an interbody fusion device is used (alone or containing other material like bone graft), the procedure is coded with the device value Interbody Fusion Device (A)
What is the ICd 10 code for a right iliac crest autograft?
The code for this procedure is 0QB20ZZ, with the body part character (fourth character) being 2 for right pelvic bone. The iliac crest does not have its own distinct body part value in ICD-10-PCS, with the ICD-10-PCS Body Part Key indicating that the pelvic bone is the closest proximal branch.
What is the code for autologous tissue substitute?
If a mixture of autologous and nonautologous bone graft (with or without biological or synthetic extenders or binders) is used, the procedure is coded with device value Autologous Tissue Substitute (7)
What is the ICD-10 PCS?
The implementation of ICD-10-PCS has enhanced the skills of coding professionals as it contains many unique features that provide an opportunity to accurately reflect the complexity of the procedures being performed. The assignment of ICD-9-CM procedure codes for spinal fusions often challenged coding professionals, and this has not changed with the transition to ICD-10-PCS. As with the coding of other complex surgical procedures, coding professionals struggle with identifying which portion of the spinal fusion procedure to code or not to code.
What is the qualifier for a spine?
Qualifier: The qualifier character identifies the column of the spine being fused (anterior or posterior) and if the surgical approach is from the front or back of the body (see Figure 1 below).
Is segmental instrumentation included in spinal fusion?
As with Examples #1 and #2, the segmental instrumentation is included in the spinal fusion and is not coded separately. The lumbar decompression L4-L5 and L5-S1 bilateral foraminotomies and L3 decompression laminectomy are also considered to be integral to the spinal fusion and not coded separately.
When will the Z98.1 ICd 10 be released?
The 2022 edition of ICD-10-CM Z98.1 became effective on October 1, 2021.
What is a Z77-Z99?
Z77-Z99 Persons with potential health hazards related to family and personal history and certain conditions influencing health status
What qualifiers are used for spinal fusion?
First, denote the proper qualifier: • Anterior approach, anterior column. • Posterior approach, posterior column. • Posterior approach, anterior column.
Does spinal fusion coding affect reimbursement?
Poor coding will negatively impact data accuracy and reimbursement. Therefore, extra training in spinal fusion coding will go a long way. Make sure the coders understand spinal anatomy and keep them up to date with new devices. 6.
What is the Z in a spinal fusion?
During the Centers for Medicare & Medicaid Services (CMS) Coordination and Maintenance Committee meeting in September 2017, the topic of invalid spinal fusion codes was raised. There were spinal fusion codes which included the character “Z” for no device. According to ICD-10-PCS Official Coding and Reporting Guidelines B3.10a – B3.10c, spinal fusions require a device. In response to this observation, 87 ICD-10-PCS codes were deleted because they contained the no device character. These codes did not meet the ICD-10-PCS definitions.
What is the last step in spinal fusion?
The last step is to undergo spinal fusion education. The Official ICD-10-PCS Guidelines tell us that the physician is not expected to use the terminology of the classification system. That job belongs to the coders. The coders should understand that all spinal fusions require a device – autograft, allograft, or interbody fusion device. If a device does not exist, then a different root operation should be selected. That selection is dependent on the goal of the operation.
How much does Medicare pay for spinal fusion?
The average payment for spinal fusion (MS-DRG 460) is $28,882.77 with the average Medicare payment of $24,458.68. According to the National Summary of Inpatient Charge Data by MS-DRGs for FY16, the frequency was 79,495. The total Medicare payment for this MS-DRG is $1,944,342,766.60. Compare this number to the average payment for MS-DRG 520 which is $9,208.77 with the average Medicare payment of $6,944.51. If 10 percent of these cases were incorrectly assigned, then there would be a payback of $139,160,426.84 which is a significant chunk of change. This number is arrived at by taking 10 percent of 79,495 which is 7,945.50 and multiplying it by the difference between $24,458.88 and $6,944.51.
General Information
CPT codes, descriptions and other data only are copyright 2021 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, §1833 (e) prohibits Medicare payment for any claim lacking the necessary information to process that claim
Article Guidance
The information in this article contains billing, coding or other guidelines that complement the Local Coverage Determination (LCD) for Lumbar Spinal Fusion L37848.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
What is the most common diagnosis for spinal fusion?
Most Common Diagnoses Associated With The Need For Spinal Fusion: Degenerative disc disease (DDD) (disc degeneration)— often causes weakness, numbness and pain. DDD is age-related and is when one or more of the discs between the vertebrae of the spinal column breaks down or deteriorates. DDD is not a true disease but develops with aging.
What is pseudoarthrosis in spinal cord?
Pseudoarthrosis— this is referred to as non-union and means ‘false joint’. This is the result of a failed spinal fusion.
Why do vertebrae protect the spinal cord?
The vertebrae are stacked on top of each other and create the natural curvature of the back.
Where does spinal stenosis occur?
Spinal stenosis occurs most often in the lumbar and cervical spine. The narrowing causes pressure on the nerves throughout the spine. Most spinal stenosis diagnoses occur due to something happening to narrow the spine, but can be due to being born with a small spinal canal (not common).
Is spondylolisthesis congenital or degenerative?
There are many types of spondylolisthesis, but the most common are congenital (present at birth), isthmic (results from spondylosis) and degenerative (most common form due to aging after 40).
Is spinal fusion a hard job?
Spinal fusion coding is a tough job for coders. There are so many diseases/disorders that result in the need for spinal fusion, and even more choices in reporting the ICD-10-PCS codes. The spine has many demands as it holds up your head, shoulders and upper body.
Popular Posts:
- 1. what is the icd 10 code for abnormal mammogram
- 2. icd 10 code for healed gastric ulcer
- 3. icd 10 code for left thumb basal arthritis
- 4. 1- icd code for m25.539
- 5. what is icd code for z15.01
- 6. 2016 icd 10 code for left third metacarpal fracture
- 7. what is the icd 10 code for congenital pelviectasis
- 8. icd-10 code for digoxin
- 9. what is the icd 10 code for a routine colonoscopy
- 10. icd 10 dx code for cbc w platelet & anc