What is a stage 4 ulcer?
Oct 01, 2021 · 2022 ICD-10-CM Diagnosis Code L89.154 2022 ICD-10-CM Diagnosis Code L89.154 Pressure ulcer of sacral region, stage 4 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code L89.154 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the treatment for Stage 4 pressure ulcer?
L89.39 Stage IV decubitus ulcer Other and unspecified sites Information In outpatient care, the ICD code on medical documents is always appended with a diagnostic confidence indicator (A, G, V or Z): A (excluded diagnosis), G (confirmed diagnosis), V (tentative diagnosis) and Z (condition after a confirmed diagnosis).
What is the cure for a decubitus ulcer?
Oct 01, 2021 · Pressure ulcer of other site, stage 4. 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code. L89.894 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L89.894 became effective on October 1, 2021.
What is pressure ulcer Stage 4?
L89.35: Stage IV decubitus ulcer Ischium. Skin on your buttocks has been damaged by pressure. As a result, an open wound has formed. This skin damage often occurs when the body is very weak. The person is then often unable to move unaided.
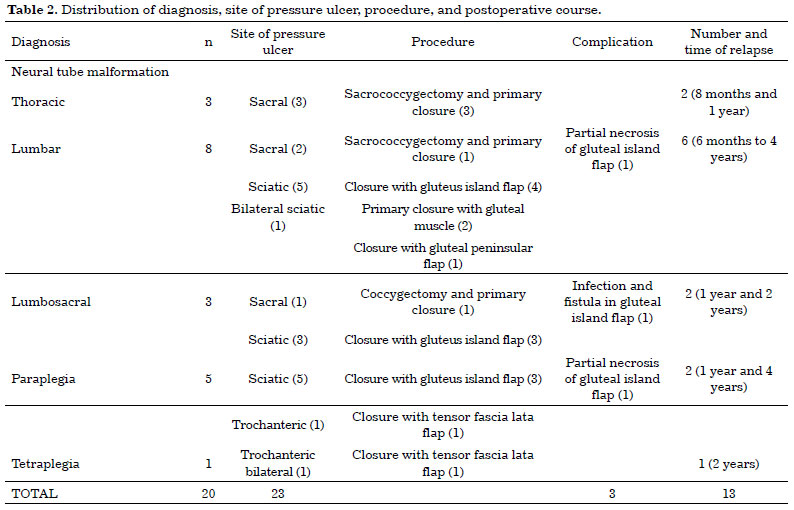
What is a stage 4 ulcer?
Stage 4 bedsores are the most severe form of bedsores, also called pressure sores, pressure ulcers, or decubitus ulcers. A stage 4 bedsore is characterized by a deep wound that reaches the muscles, ligaments, or even bone. They often cause residents to suffer extreme pain, infection, invasive surgeries, or even death.May 5, 2021
What is L89 154?
ICD-10 | Pressure ulcer of sacral region, stage 4 (L89. 154)
What is the ICD-10 code for coccyx pressure ulcer 4?
L89.1542022 ICD-10-CM Diagnosis Code L89. 154: Pressure ulcer of sacral region, stage 4.
What is the correct code for a stage IV decubitus ulcer on the left ankle?
2022 ICD-10-CM Diagnosis Code L89. 524: Pressure ulcer of left ankle, stage 4.
How are decubitus ulcers formed?
A decubitus ulcer is also known as a pressure ulcer, pressure sore, or bedsore. It's an open wound on your skin caused by a long period of constant pressure to a specific area of the body. Decreased blood flow to these areas leads to tissue damage and death. Decubitus ulcers often occur on the skin covering bony areas.
What is the ICD-10 code for HX of CVA?
When a patient has a history of cerebrovascular disease without any sequelae or late effects, ICD-10 code Z86. 73 should be assigned.
What is the ICD-10 code for chronic sacral decubitus ulcer?
L89.159159 for Pressure ulcer of sacral region, unspecified stage is a medical classification as listed by WHO under the range - Diseases of the skin and subcutaneous tissue .
What is coccyx and sacrum?
The sacrum, sometimes called the sacral vertebra or sacral spine (S1), is a large, flat triangular shaped bone nested between the hip bones and positioned below the last lumbar vertebra (L5). The coccyx, commonly known as the tailbone, is below the sacrum.Mar 12, 2020
What is the ICD-10 code for coccyx Stage 2 pressure ulcer?
L89.1522022 ICD-10-CM Diagnosis Code L89. 152: Pressure ulcer of sacral region, stage 2.
What is the ICD 10 code for decubitus ulcer?
L89.90Pressure ulcer of unspecified site, unspecified stage L89. 90 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L89. 90 became effective on October 1, 2021.
How do you code an ulcer with gangrene?
When there is documentation of necrotic or gangrenous ulcer, so stated, then Gangrenous ulcer = R02, L97 in that order by index. Necrotic ulcer = L97, R02 (As there is no exclusion for 'necrosis under L97 only gangrene –L97 must be coded first.)Jan 1, 2014
When gangrene is present with a skin ulcer code?
The appropriate ICD-10-CM codes for this patient, as per ICD-10-CM guidelines, are E086. 621 and L97. 413. Gangrene at the Site of Ulcer: The gangrene should be coded first, followed by the code for the ulcer.Sep 3, 2019
Information
In outpatient care, the ICD code on medical documents is always appended with a diagnostic confidence indicator (A, G, V or Z): A (excluded diagnosis), G (confirmed diagnosis), V (tentative diagnosis) and Z (condition after a confirmed diagnosis).
Source
Provided by the non-profit organization “Was hab’ ich?” gemeinnützige GmbH on behalf of the Federal Ministry of Health (BMG).
Bei Ihnen wurde Haut am Gesäß durch Druck geschädigt. Dadurch hat sich eine offene Stelle gebildet
Häufig entstehen diese Hautschäden, wenn der Körper sehr geschwächt ist. Man hat dann oft keine Kraft, sich alleine zu bewegen. Wenn man viel und lange liegt, wirkt über längere Zeit ein Druck auf die gleiche Stelle. Wenn länger Druck auf die Haut einwirkt, dann wird die Haut weniger durchblutet und kann geschädigt werden.
Information
This information is not intended for self-diagnosis and does not replace professional medical advice from a doctor.
Source
Provided by the non-profit organization “Was hab’ ich?” gemeinnützige GmbH on behalf of the Federal Ministry of Health (BMG).
What is an unstageable ulcer?
An unstageable ulcer is when the base of the ulcer is covered in eschar or slough so much that it cannot be determined how deep the ulcer is. This diagnosis is determined based on the clinical documentation. This code should not be used if the stage is not documented.
What is the sequence of a pressure ulcer?
The sequence depends on the pressure ulcer being treated. If all the pressure ulcers are being treated, sequence the code for the most severe pressure ulcer first. Example: A patient with a stage 3 pressure ulcer on her left heel and a stage 2 pressure ulcer of her left hip is scheduled for debridement.
What is pressure ulcer?
Pressure ulcers are areas of damaged skin and tissue developing as a result of compromised circulation. When a patient stays in one position without movement, the weight of the bones against the skin inhibits circulation and causes an ulceration of the tissue. Pressure ulcers usually form near the heaviest bones (buttocks, hips, and heels).
Where do pressure ulcers form?
Pressure ulcers usually form near the heaviest bones (buttocks, hips, and heels). There are stages of pressure ulcers that identify the extent of the tissue damage. Stage 1—Persistent focal erythema. Stage 2—Partial thickness skin loss involving epidermis, dermis, or both.
Can a pressure ulcer get worse?
If the pressure ulcer is healed completely , a code is not reported for the pressure ulcer. There are some cases where the pressure ulcer will get worse during the course of the admission. For example, the patient is admitted for treatment of a stage 2 ulcer that progresses to stage 3.
What is the stage of an unstageable ulcer?
However, unstageable ulcers can only be Stage 3 or 4, by definition (“full-thickness skin and tissue loss in which the extent of tissue damage within the ulcer cannot be confirmed because it is obscured by slough or eschar. If slough or eschar is removed, a Stage 3 or Stage 4 pressure injury will be revealed”).
How many codes are needed for pressure ulcers?
If a patient is admitted to an inpatient hospital with a pressure ulcer at one stage and it progresses to a higher stage, two separate codes should be assigned: one code for the site and stage of the ulcer on admission and a second code for the same ulcer site and the highest stage reported during the stay.
What is pressure ulcer?
A pressure injury is now described as “localized damage to the skin and/or underlying soft tissue, usually over a bony prominence or related to a medical or another device .”. The injury can present as intact skin or an open ulcer ...
Popular Posts:
- 1. icd 10 code for chronic deep vein thrombosis (dvt) of other vein of right upper extremity
- 2. icd 10 code for distention renal pelvis
- 3. icd 10 code for lower extremity arterial insufficiency
- 4. icd 10 code for otits media
- 5. icd 10 code for bypass graft infection right leg
- 6. icd 10 diagnosis code for angroedenia of tongue
- 7. icd 10 code for sleep exhaustion
- 8. icd 10 cm code for strangulated 4th-degree hemorrhoids
- 9. icd 10 code for breast lumpectomy
- 10. icd 9 code for excessive eating