What are the ICD 10 codes for stroke?
- Code: I63.
- Code Name: ICD-10 Code for Cerebral infarction.
- Block: Cerebrovascular diseases (I60-I69)
- Excludes 1: transient cerebral ischemic attacks and related syndromes (G45.-)
- Details: Cerebral infarction.
- Includes: occlusion and stenosis of cerebral and precerebral arteries, resulting in cerebral infarction.
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
What is the diagnosis code for stroke?
- Acute cerebrovascular insufficiency
- Acute stroke
- Autosomal recessive leukoencephalopathy, ischemic stroke, retinitis pigmentosa syndrome
- Brainstem stroke syndrome
- Cerebellar infarction
- Cerebellar stroke
- Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy
- Cerebral infarction
What are ICD 10 codes?
Why ICD-10 codes are important
- The ICD-10 code system offers accurate and up-to-date procedure codes to improve health care cost and ensure fair reimbursement policies. ...
- ICD-10-CM has been adopted internationally to facilitate implementation of quality health care as well as its comparison on a global scale.
- Compared to the previous version (i.e. ...
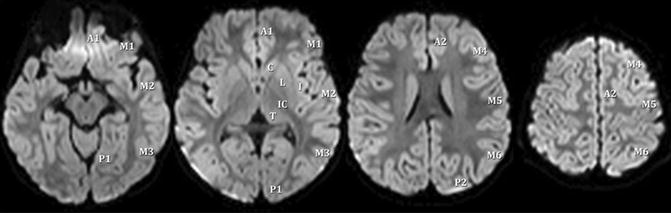
What is the ICD-10 code for a stroke?
ICD-10 | Cerebral infarction, unspecified (I63. 9)
What is the ICD-10 code for recent CVA?
When a patient has a history of cerebrovascular disease without any sequelae or late effects, ICD-10 code Z86. 73 should be assigned.
What is the ICD-10-CM code for ischemic stroke?
ICD-10-CM I67. 81 is grouped within Diagnostic Related Group(s) (MS-DRG v39.0): 061 Ischemic stroke, precerebral occlusion or transient ischemia with thrombolytic agent with mcc.
What is the code for stroke?
For ischaemic stroke, the main codes are ICD-8 433/434 and ICD-9 434 (occlusion of the cerebral arteries), and ICD-10 I63 (cerebral infarction).
Is CVA and stroke the same thing?
A stroke, also referred to as a cerebral vascular accident (CVA) or a brain attack, is an interruption in the flow of blood to cells in the brain. When the cells in the brain are deprived of oxygen, they die.
How do you code late effects of stroke?
Other sequelae of cerebral infarctionI69. 398 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.The 2022 edition of ICD-10-CM I69. 398 became effective on October 1, 2021.This is the American ICD-10-CM version of I69.
How can you diagnose stroke?
Strokes are usually diagnosed by doing physical tests and studying images of the brain produced during a scan.A blood test to find out your cholesterol and blood sugar level.checking your pulse for an irregular heartbeat.taking a blood pressure measurement.
What is the ICD-10 code for history of CVA with residual deficits?
Cognitive deficits following cerebral infarction The 2022 edition of ICD-10-CM I69. 31 became effective on October 1, 2021. This is the American ICD-10-CM version of I69. 31 - other international versions of ICD-10 I69.
What is the ICD-10 code for stroke?
Explicitly document findings to support diagnoses of › Stroke sequela codes (ICD-10 category I69.-) should acute stroke, stroke and subsequent sequela of be used at the time of an ambulatory care visit stroke, and personal history of stroke without sequela, oce, which is considered subsequent to any acute
What is the term for a stroke that occurs when there is disruption of blood flow to brain tissue?
stroke occurs when there is disruption of blood flow to brain tissue, this leads to ischemia (deprivation of oxygen) and potentially infarction (dysfunctional scar tissue). Strokes can be either hemorrhagic, or embolic/thrombotic. Hemorrhagic strokes occur as a result of a ruptured cerebral blood vessel. Embolic/thrombic strokes occur as a result of an obstructed cerebral vessel.
When will the ICd 10-CM Z03.89 be released?
The 2022 edition of ICD-10-CM Z03.89 became effective on October 1, 2021.
What is a Z00-Z99?
Categories Z00-Z99 are provided for occasions when circumstances other than a disease, injury or external cause classifiable to categories A00 -Y89 are recorded as 'diagnoses' or 'problems'. This can arise in two main ways:
What is a brief attack of cerebral dysfunction of vascular origin?
A brief attack (from a few minutes to an hour) of cerebral dysfunction of vascular origin, with no persistent neurological deficit. A disorder character ized by a brief attack ( less than 24 hours) of cerebral dysfunction of vascular origin, with no persistent neurological deficit.
How long does a cerebral ischemia attack last?
Recurring, transient episodes of neurologic dysfunction caused by cerebral ischemia; onset is usually sudden, often when the patient is active; the attack may last a few seconds to several hours; neurologic symptoms depend on the artery involved.
When will the ICD-10 G45.9 be released?
The 2022 edition of ICD-10-CM G45.9 became effective on October 1, 2021.
How long does focal ischemic dysfunction last?
Brief reversible episodes of focal, nonconvulsive ischemic dysfunction of the brain having a duration of less than 24 hours, and usually less than one hour, caused by transient thrombotic or embolic blood vessel occlusion or stenosis.
How to identify stroke symptoms?
Identify signs and symptoms of possible stroke and activate emergency response. Observe the patient for signs of a stroke. Use F-A-S-T to remember the warning signs: facial drooping, arm weakness, speech difficulties, and time. Call 911 immediately, or have someone else call, to activate the emergency response system.
Can fibrinolytic therapy be used for ischemic stroke?
Probable acute ischemic stroke; consider fibrinolytic therapy. If the CT scan shows no sign of hemorrhage, it is probable that the patient experienced an ischemic stroke and is a candidate for fibrinolytic therapy. Check for fibrinolytic exclusions such as significant head trauma or stroke in the previous 3 months, history of intracranial hemorrhage, elevated blood pressure, active internal bleeding, or a blood glucose concentration less than 50 milligrams per deciliter. Then repeat the neurologic exam.

Popular Posts:
- 1. icd 10 code for hx of basal cell carcinoma
- 2. icd 9 code for vit b def
- 3. icd 10 code for batten disease
- 4. icd-10 code for seizure activity
- 5. icd 10 code for umbilical hernia with sbo
- 6. icd 9 code for tibial fracture
- 7. icd-10 code for dizziness
- 8. icd 10 code for acute lymphangitis of right forearm
- 9. icd 10 cm code for ganglion tendon sheath of the right wrist
- 10. icd code for foreign body removal