How to cure degenerative disc disease naturally?
Natural Treatments For Degenerative Disc Disease
- Apply Hot Or Cold Packs For Pain Relief. Applying hot or cold packs can ease pain linked to degenerative disc disease. ...
- Correct Your Posture. Poor posture can stress your spinal discs and lead to joint compression and muscular fatigue. ...
- Lose Weight If You’re Overweight. ...
- Exercise. ...
- Practice Yoga. ...
- Consume Fish Oil. ...
- Have Boswellia. ...
- Drink Ginger Tea. ...
Is degenerative disc disease the same thing as arthritis?
What is degenerative disc disease? ... Arthritis in the low back has similar symptoms and can cause pain in the back and sometimes into the buttocks. Sometimes the pain can radiate into the thighs, and if it does then it could indicate involvement of the nerves. ... The guidelines for symptoms of tingling, numbness and weakness are the same in ...
Do I have degenerative disc disease?
Symptoms of degenerative disc disease are most commonly found in the low back or neck. The pain may: • Range from mild to severe and disabling. • Primarily affect the neck and lower back. • Extend to the arms and hands. • Radiate to the buttocks and thighs. • Worsen when sitting or after bending, lifting or twisting. • Come and go.
Is my pain from degenerative disc disease?
What are the symptoms of degenerative disc disease? The most common symptoms of degenerative disc disease are neck pain and back pain. You may experience pain that: Comes and goes, lasting for weeks or months at a time. Leads to numbness or tingling in your arms or legs. Radiates down your buttocks and lower back.
What is ICD-10 code for degenerative disc disease?
ICD-10 code M51. 36 for Other intervertebral disc degeneration, lumbar region is a medical classification as listed by WHO under the range - Dorsopathies .
What is thoracic disc degeneration?
Thoracic degenerative disc disease refers to the degeneration, or breakdown, of the shock-absorbing intervertebral discs that cushion the vertebrae in the upper and middle back (called the thoracic spine). It develops most frequently in middle-aged people or young adults with active lifestyles.
How do you code degenerative disc disease?
722.51 is the correct diagnosis code for thoracic degenerative disc disease. 722.52 is the accurate diagnosis code for DDD of the lumbar or lumbosacral intervertebral disc.
Is degenerative disc disease the same as disc degeneration?
However, the term does not refer to the symptoms, but rather describes the process of the disc degenerating over time. Despite what the name suggests, degenerative disc disease is not a disease, but a condition in which natural, age-related wear-and-tear on a disc causes pain, instability, and other symptoms.
What is degenerative changes of thoracic spine?
The phrase "degenerative changes" in the spine refers to osteoarthritis of the spine. Osteoarthritis is the most common form of arthritis. Doctors may also refer to it as degenerative arthritis or degenerative joint disease. Osteoarthritis in the spine most commonly occurs in the neck and lower back.
What is degenerative thoracic spondylosis?
Spondylosis refers to the natural wear and tear that can happen in the spine. Also called spinal osteoarthritis, it can affect any region of the spine, including the cervical (neck) or lower back.
What is the ICD 10 code for degenerative changes?
According to Coding Clinic: “Assign code M16. 0—Bilateral primary osteoarthritis of hip for degenerative changes of hips”. Coding Clinic's rationale is, “ICD-10- CM's Alphabetic Index under “Degeneration, joint disease” instructs “see Osteoarthritis.”
Is degenerative disc disease a diagnosis?
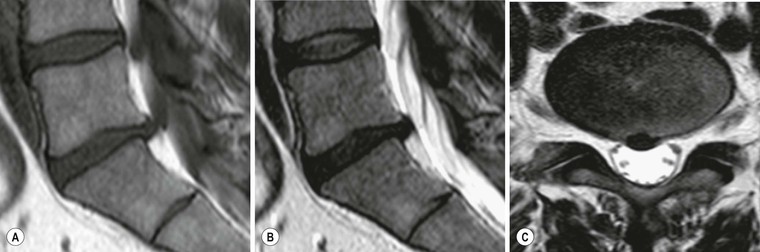
How is degenerative disc disease diagnosed? A diagnosis is based on a medical history and a physical examination, as well as the symptoms and the circumstances where the pain started. Magnetic resonance imaging can show damage to discs, but it alone cannot confirm degenerative disc disease.
What is the ICD 10 code for lumbar degenerative disc disease?
Other intervertebral disc disorders, lumbar region M51. 86 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM M51. 86 became effective on October 1, 2021.
What is the difference between spinal stenosis and degenerative disc disease?
Discs often degenerate with age causing vertebrae to sit closer together. This is part of the reason we shrink with age. Degenerative discs can lead to pain via multiple pathways. Spinal stenosis is another condition of the spine where the central canal diameter is reduced much like a pipe that becomes clogged.
How serious is degenerative thoracic spine?
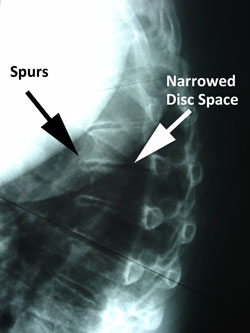
Thoracic disc degeneration can be a cause of upper or mid back pain. If the disc is severely degenerated, bone spurs can form and limit the mobility of the thoracic spine. The spurs may cause narrowing of the spinal canal and impinge on the spinal cord.
What is it called when your spine deteriorates?
Degenerative spine conditions involve the gradual loss of normal structure and function of the spine over time. They are usually caused by aging, but may also be the result of tumors, infections or arthritis. Pressure on the spinal cord and nerve roots caused by degeneration can be caused by: Slipped or herniated discs.
What character is used for disc disorders?
Only use the fourth character “9” for unspecified disc disorders if the documentation does not indicate anything more than the presence of a disc problem. But beware, payors are expected to ask for clarification if unspecified or “NOS” codes are used.
What is the 5th character of a disc?
9 = unspecified disc disorder. The fifth character provides detail about the anatomical location within the spinal region. A basic knowledge of spinal anatomy should make fifth-character selection easy, but only if it is documented properly. This includes transitionary regions.
What is the T12-L1 code?
Though it is not specifically mentioned, “thoracolumbar” likely only includes T12-L1, and “lumbosacral” probably only refers to the L5-S1 interspace. There is a strange rule for cervical disc disorders indicating that you should code to the most superior level of the disorder.
Can a spinal disc be coded?
These spinal disc codes appear to be a bit complex, but with some study and evaluation, the logic used to create them becomes clear. The provider can use the codes to guide proper documentation and the coder then can select the right codes with confidence.
Is sciatica a code for lumbar radiculopathy?
It is already included in the code. Likewise, don’t code sciatica (M54.3-) if you code for lumbar disc with radiculopathy. It would be redundant. On a side note, lumbar radiculopathy (M54.16) might be used if pain is not yet known to be due a disc, but it radiates from the lumbar spine.
Popular Posts:
- 1. icd 10 code for pvd with gangrene
- 2. icd 10 code for l lateral malleolus venous stasis ulcer
- 3. icd 10 code for long term use of oral hypoglycemics
- 4. icd 10 code for hx of gastric ulcer
- 5. icd 10 code for cellulitis abscess
- 6. icd 10 code for left shoulder sptrain
- 7. icd 10 cm code for otitis effusion
- 8. icd 10 code for acute pharyngitis
- 9. icd-10 code for long term parenteral nutrition
- 10. icd 10 code for mild hepatomegaly