What is the ICD 10 code for transient acantholytic dermatosis?
Transient acantholytic dermatosis [Grover] L11.1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM L11.1 became effective on October 1, 2018. This is the American ICD-10-CM version of L11.1 - other international versions of ICD-10 L11.1 may differ.
What is the ICD 10 code for melanin hyperpigmentation?
Other melanin hyperpigmentation 2016 2017 2018 2019 2020 2021 Billable/Specific Code L81.4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM L81.4 became effective on October 1, 2020.
What is the ICD 10 code for subcorneal pustular dermatitis?
2018/2019 ICD-10-CM Diagnosis Code L13.1. Subcorneal pustular dermatitis. L13.1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD 10 code for viral warts?
L81.4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM L81.4 became effective on October 1, 2021. This is the American ICD-10-CM version of L81.4 - other international versions of ICD-10 L81.4 may differ. viral warts ( B07.-)
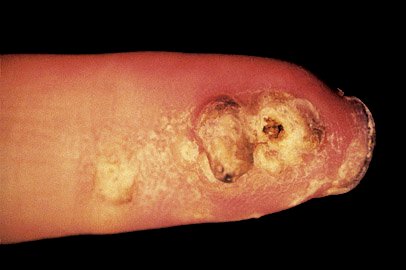
What is the ICD-10 code for pustular melanosis newborn?
Condition of the integument specific to newborn, unspecified The 2022 edition of ICD-10-CM P83. 9 became effective on October 1, 2021. This is the American ICD-10-CM version of P83.
What is transient neonatal pustular melanosis?
Transient neonatal pustular melanosis (TNPM) is an idiopathic pustular eruption that heals with brown pigmented macules. TNPM is more common in black neonates, and is probably the reason for the so-called lentigines neonatorum noted in 15% of black newborns.
Is pustular melanosis normal?
Transient neonatal pustular melanosis (TNPM) is a normal and harmless skin condition that affects newborns. Infants with TNPM have skin bumps called pustules that are noticeable at birth. These pus-filled bumps rupture, causing white-encircled dark spots on the skin. These spots eventually fade.
What causes pustular melanosis in infants?
What causes transient neonatal pustular melanosis? The cause of transient neonatal pustular melanosis is unknown. Some authors have suggested it may be a variant of toxic erythema of the newborn [4].
How is pustular melanosis treated?
No treatment is indicated. Reassure parents that neonatal pustular melanosis is a benign finding and that it disappears.
How long can pustular melanosis last?
The prognosis for transient neonatal pustular melanosis is good. The vesicles and pustules usually resolve within 48 hours, while the brown macules usually fade over 3-4 weeks but may persist for several months.
What is Pustulosis?
Pustulosis is highly inflammatory skin condition resulting in large fluid-filled blister-like areas - pustules. Pustulosis typically occurs on the palms of the hands and/or the soles of the feet. The skin of these areas peels and flakes (exfoliates).
Does psoriasis cause pustules?
This type of psoriasis causes reddish, scaly, pus-filled bumps. Anyone who has pus-filled bumps over much of the body needs immediate medical care. When widespread, pustular psoriasis can be life-threatening. The pus-filled bumps are called pustules.
What is transitory dermatosis?
NEONATAL. DERMATOSIS. “Sucking blister” These erosions (missing patches of skin), a result of vigorous sucking during fetal life, are typically located on the outer aspect of hands and resolve without specific treatment within days to weeks.
What causes infantile acne?
Infantile acne is thought to be a result of testosterone temporarily causing an over-activity of the skin's oil glands. In susceptible children this may stimulate the development of acne. Most children are however otherwise healthy with no hormonal problem. The acne reaction usually subsides within 2 years.
How long does neonatal cephalic Pustulosis last?
The term "benign cephalic pustulosis" is increasingly used for this condition. The lesions may appear within the first 2 to 4 weeks of life and can last up to 6 months. Neonatal acne occurs primarily on the face; back and chest involvement is less common. Often patients have a family history of severe acne.
How do you treat baby acne?
These tips are useful for caring for your baby's skin while he or she has acne:Keep your baby's face clean. Wash your baby's face daily with warm water and mild baby soap.Dry your baby's face gently. Simply pat your baby's skin dry.Don't pinch or scrub the acne. ... Avoid using lotions or oils on your baby's face.
What causes Acropustulosis?
The cause of acropustulosis is unknown. Sometimes it develops before or after a child has a similar skin condition called scabies. A child can have an allergic reaction to the type of burrowing mite that gets into their skin and causes scabies. Acropustulosis may occur without scabies too.
What causes neonatal cephalic Pustulosis?
What is the cause of neonatal cephalic pustulosis? Neonatal cephalic pustulosis is related to malassezia colonisation, which may be found on mycology (microscopy and culture) of smears from facial pustules.
What causes infantile acne?
Infantile acne is thought to be a result of testosterone temporarily causing an over-activity of the skin's oil glands. In susceptible children this may stimulate the development of acne. Most children are however otherwise healthy with no hormonal problem. The acne reaction usually subsides within 2 years.
What are Craniotabes?
Craniotabes is a softening of the skull bones.
What is a small circumscribed melanose?
Small circumscribed melanoses resembling, but differing histologically from , freckles. The concept includes senile lentigo ('liver spots') and nevoid lentigo (nevus spilus, lentigo simplex) and may also occur in association with multiple congenital defects or congenital syndromes (e.g., peutz-jeghers syndrome).
When will the ICD-10-CM L81.4 be released?
The 2022 edition of ICD-10-CM L81.4 became effective on October 1, 2021.
What is transient neonatal pustular melanosis?
Transient neonatal pustular melanosis is an uncommon benign pustular condition presenting in newborn infants [1]. It is also known as transient neonatal pustular dermatosis and transient neonatal pustulosis.
What causes pustular melanosis in neonates?
The cause of transient neonatal pustular melanosis is unknown. Some authors have suggested it may be a variant of toxic erythema of the newborn [4].
How common is pustular melanosis in African American babies?
It is more common in African American babies than white American babies, affecting 4.4% of African American [3].
How long does it take for pustules to heal?
The pustules can rupture and crust, resolving within several days [1].
Do pustules develop after birth?
The pustules are present at birth and evolve; new lesions usually do not develop after birth [1].
Is pustular melanosis clinical?
The diagnosis of transient neonatal pustular melanosis is clinical. No investigations are required.

Popular Posts:
- 1. icd 10 code for history of gastrointestinal bleeding
- 2. icd 10 code for ramseys hunt syndrome
- 3. icd-10 code for history of aaa
- 4. icd code 10 code for large kidney stones with hydronephrosis
- 5. icd 10 code for possible hernia vaginal
- 6. icd 10 code for right sided hydronephrosis
- 7. icd 10 cm code for blepharitis
- 8. icd 9 code for iliac atherosclerosis
- 9. icd 10 code for cut mid side of toe nail left side
- 10. icd 10 code for upper back muscle spasm