What is the ICD 10 code for injection of trigger points?
Compliance with the provisions in LCD L33912, Injection of Trigger Points may be monitored and addressed through post payment data analysis and subsequent medical review audits. The following ICD-10-CM codes support medical necessity and provide limited coverage for CPT codes: 20552 and 20553.
What is the ICD 10 code for trigger thumb?
Trigger thumb of right thumb ICD-10-CM M65.311 is grouped within Diagnostic Related Group (s) (MS-DRG v38.0): 557 Tendonitis, myositis and bursitis with mcc 558 Tendonitis, myositis and bursitis without mcc
What is the CPT code for trigger finger injection?
What CPT code is used for trigger finger injection? Utilizing CPT codes for the injection of the tendon sheath (20550) and tendon sheath incision (26055) it was determined whether a patient was treated with injection or surgery. Click to see full answer. Considering this, what is the CPT code for trigger finger release?
What is trigger point injection (TPI)?
Trigger point injection (TPI) therapy involves injection of medications directly into the trigger points or knots that form when muscles do not relax.
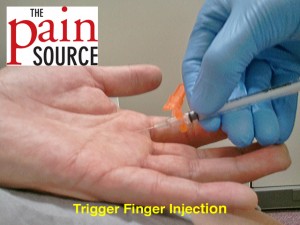
What is the ICD-10 code for trigger point injection?
20552-Injection(s); single or multiple trigger point(s), 1 or 2 muscle(s)
What is the ICD-10 code for right thumb trigger?
ICD-10 | Trigger thumb, right thumb (M65. 311)
What is the ICD-10 code for left thumb trigger?
ICD-10 code M65. 312 for Trigger thumb, left thumb is a medical classification as listed by WHO under the range - Soft tissue disorders .
How do you document a trigger point injection?
When coding for trigger point injections, the documentation must include the site of the injection, the total number of injections and the number of muscles involved. In addition, documentation must also support that various conservative therapies have been tried and failed.
What is the CPT code for trigger finger injection?
CPT code 20550 is frequently used for a trigger finger injection, where the injection is administered to the tendon sheath.
What is the CPT code for trigger thumb release?
26055Patients who have undergone trigger finger release without any concurrent procedures were identified from 2017-2018 using cpt code 26055.
What is the ICD-10 code for trigger finger?
ICD-10 code M65. 30 for Trigger finger, unspecified finger is a medical classification as listed by WHO under the range - Soft tissue disorders .
What is the ICD-10 code for right hand Pain?
M79. 641 - Pain in right hand. ICD-10-CM.
Is trigger finger a disease?
Trigger finger is a condition that causes pain, stiffness, and a sensation of locking or catching when you bend and straighten your finger. The condition is also known as “stenosing tenosynovitis.” The ring finger and thumb are most often affected by trigger finger, but it can occur in the other fingers, as well.
What diagnosis covers trigger point injections?
A Medicare beneficiary must be diagnosed with myofascial pain syndrome (MPS), which is a chronic pain disorder, in order for Medicare to cover trigger point injections. A doctor or provider will review the beneficiary's medical history and complete an exam of the patient to make this diagnosis.
Are trigger point injections the same as nerve blocks?
Trigger point injections are not truly nerve blocks; rather they are muscle blocks. Muscles that are chronically tense or in spasm become tender and painful.
Is a trigger point injection the same as a cortisone injection?
Trigger point injections are the second treatment option, and these injections contain either a steroid (cortisone) or plant-based medicine (sarapin) to loosen the trigger point and reduce pain.
What is trigger point injection?
Trigger point injection therapy is a common procedure performed by pain management specialists, orthopedic surgeons, physical medicine and rehab and other specialties. Trigger point injection therapy is used for the treatment of myofascial pain syndrome (MPS). According to the American Society of Regional Anesthesia and Pain Medicine.
What is the CPT code for MPS?
There are two CPT ® codes for Trigger point injections: 20552-Injection (s); single or multiple trigger point (s), 1 or 2 muscle (s) ...
How many sets of injections are needed for pain?
Up to 4 sets of injections are considered medically necessary to diagnose the origin of the patient’s pain and to achieve a therapeutic effect; additional sets of trigger point injections are not considered medically necessary if not clinical response is achieved.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, §1862 (a) (1) (A). Allows coverage and payment for only those services that are considered to be medically reasonable and necessary. Title XVIII of the Social Security Act, §1833 (e). Prohibits Medicare payment for any claim which lacks the necessary information to process the claim.
Article Guidance
The following coding and billing guidance is to be used with its associated Local coverage determination.
ICD-10-CM Codes that Support Medical Necessity
These are the only covered ICD-10-CM codes that support medical necessity. This A/B MAC will assign the following ICD-10-CM codes to indicate the diagnosis of a trigger point. Claims without one of these diagnoses will always be denied.
ICD-10-CM Codes that DO NOT Support Medical Necessity
All ICD-10-CM codes not listed in this policy under ICD-10-CM Codes That Support Medical Necessity above.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
Article Guidance
This First Coast Billing and Coding Article for Local Coverage Determination (LCD) L33912 Injection of Trigger Points provides billing and coding guidance for diagnosis limitations that support diagnosis to procedure code automated denials.
ICD-10-CM Codes that Support Medical Necessity
The following ICD-10-CM codes support medical necessity and provide limited coverage for CPT codes: 20552 and 20553.
ICD-10-CM Codes that DO NOT Support Medical Necessity
All those not listed under the “ICD-10-CM Codes that Support Medical Necessity” section of this article.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
What is the ICD 10 code for trigger finger?
Trigger finger, unspecified finger M65. 30 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2020 edition of ICD-10-CM M65. 30 became effective on October 1, 2019.
What is a1 pulley?
The pulley at the base of the finger is called the “A1 pulley.” This is the pulley that is most often involved in trigger finger. The tendon sheath attaches to the finger bones and keeps the flexor tendon in place as it moves. The A1 pulley is near the opening of the tendon sheath.
What is the ICD 10 code for right trigger thumb?
Trigger thumb, right thumb M65. 311 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
How do you bill a 20553?
Effective March 1, 2017, Any combination of trigger point injections, CPT codes 20552 (Injection (s); single or multiple trigger point (s), 1 or 2 muscle (s)) and 20553 (Injection (s); single or multiple trigger point (s), 3 or more muscles), when billed >3 times in a 90-day period, for the same anatomic site, without
Does 20552 need a modifier?
Modifier 50 is not a valid modifier with this code. Example # 3: 20552 = Injection (s); single or multiple trigger point (s), one or two muscle (s) Modifiers LT or RT are not valid for 20552 because trigger points and muscles exist throughout the body, not in only two paired locations.
How do you code multiple trigger point injections?
There continues to be a lot of confusion on proper coding for trigger-point injections. Two CPT4 codes can be used: 20552—Injection (s); single or multiple trigger point (s), one or two muscle (s); and. 20553—Injection (s); single or multiple trigger point (s), three or more muscle (s).
Can you bill for lidocaine injection?
This means that code 90772 [Therapeutic, prophylactic or diagnostic injection (specify substance or drug); subcutaneous or intramuscular] is the correct code. To bill for lidocaine, report J3490 [Unclassified drugs]. Lidocaine would be included as a supply with code 58999 and therefore not separately billable.
Document Information
CPT codes, descriptions and other data only are copyright 2021 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
This LCD supplements but does not replace, modify or supersede existing Medicare applicable National Coverage Determinations (NCDs) or payment policy rules and regulations for trigger point injections. Federal statute and subsequent Medicare regulations regarding provision and payment for medical services are lengthy.
Coverage Guidance
Compliance with the provisions in this LCD may be monitored and addressed through post payment data analysis and subsequent medical review audits. History/Background and/or General Information Trigger point injection is one of many modalities utilized in the management of chronic pain.
General Information
CPT codes, descriptions and other data only are copyright 2021 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, Section 1833 (e) states that no payment shall be made to any provider of services or other person under this part unless there has been furnished such information as may be necessary in order to determine the amounts due such provider or other person under this part for the period with respect to which the amounts are being paid or for any prior period..
Article Guidance
This Billing and Coding Article provides billing and coding guidance for Local Coverage Determination (LCD) L35010, Trigger Point Injections. Please refer to the LCD for reasonable and necessary requirements.
ICD-10-CM Codes that Support Medical Necessity
It is the provider’s responsibility to select codes carried out to the highest level of specificity and selected from the ICD-10-CM code book appropriate to the year in which the service is rendered for the claim (s) submitted. The following ICD-10 CM codes support medical necessity and provide coverage for CPT/HCPCS codes 20552 and 20553:
ICD-10-CM Codes that DO NOT Support Medical Necessity
All those not listed under the “ICD-10 Codes that Support Medical Necessity” section of this policy.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.

Popular Posts:
- 1. icd 10 code for pinky fracture
- 2. what icd-10-pcs code is used for open repair of laceration of large intestine
- 3. icd 10 code for sensation of foreign body in eye
- 4. icd 10 code for fracture of dental restoration
- 5. icd 10 code for infection post back surgery
- 6. icd 10 code for dolphon
- 7. icd-10-cm code for reporting sepsis due to mrsa?
- 8. 2017 icd 10 code for ect
- 9. icd 10 code for hot flashes in male
- 10. icd 10 cm code for pathological fracture of pelvis dur to osteoporosis