What is the ICD 10 code for myopathy?
Other specified myopathies 2016 2017 2018 2019 2020 2021 Billable/Specific Code G72.89 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM G72.89 became effective on October 1, 2020.
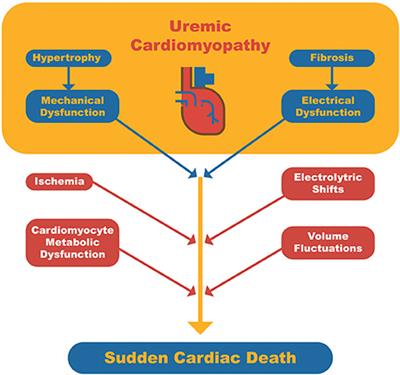
What is uremic myopathy?
Our group uses the term “uremic myopathy” to refer to the constellation of functional and occasionally structural muscle abnormalities in patients with chronic renal failure as a consequence of the uremic state itself.
What is the CPT code for hemolytic uremic syndrome?
Hemolytic uremic syndrome; code to identify associated:; E. coli infection (B96.2-); Pneumococcal pneumonia (J13); Shigella dysenteriae (A03.9)
What are the symptoms of uremic myopathy in dialysis patients?
Proximal muscle weakness and rapid-onset tiredness, common complaints in dialysis patients, are directly related to the presence of uremic myopathy. Generally, patients with chronic renal failure have about 50% of the muscle strength of their healthy counterparts Rehabilitation exercise training in chronic renal failure.
What is the diagnosis code for myopathy?
ICD-10 Code for Myopathy, unspecified- G72. 9- Codify by AAPC.
What is the ICD-10 code for autoimmune necrotizing myopathy?
The 2022 edition of ICD-10-CM G72. 49 became effective on October 1, 2021. This is the American ICD-10-CM version of G72.
What is the ICD-10 code for rhabdomyolysis?
ICD-10 code M62. 82 for Rhabdomyolysis is a medical classification as listed by WHO under the range - Soft tissue disorders .
Is U07 1 a primary diagnosis?
The diagnosis code, U07. 1, should only be billed when a patient has a confirmed diagnosis of coronavirus. This means the patient must have been tested prior and it came back positive for this diagnosis code to be used on the claim. The CDC notes that this is an exception to the hospital inpatient guideline.
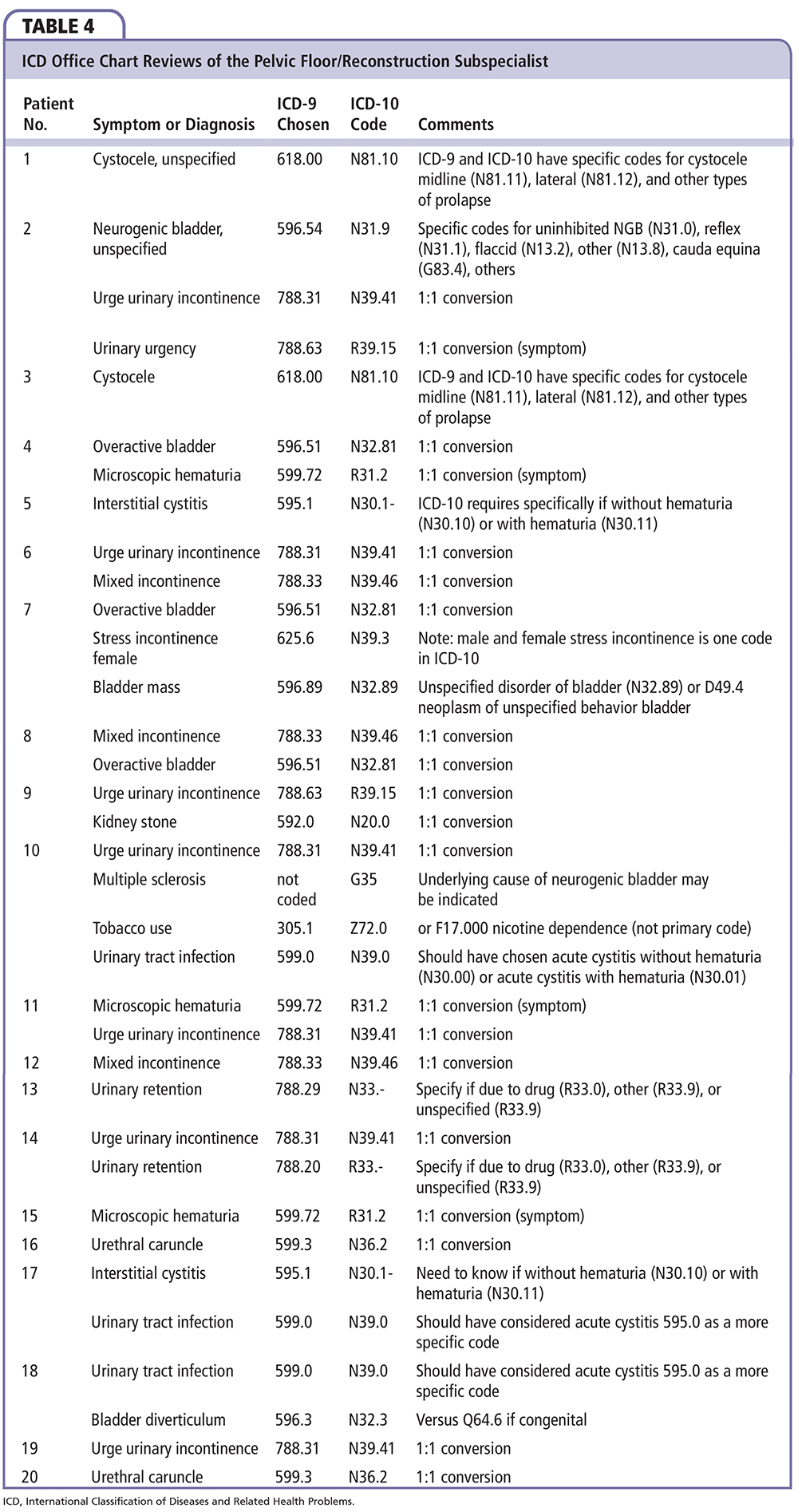
How do you code uremic myopathy?
Myopathy, unspecifiedin (due to) toxic agent NEC G72.2.toxic G72.2.
What is necrotising autoimmune myopathy?
Importance Necrotizing autoimmune myopathy (NAM) is characterized pathologically by necrotic muscle fibers with absent or minimal inflammation.
What Rhabdomyolysis means?
Rhabdomyolysis (often called rhabdo) is a serious medical condition that can be fatal or result in permanent disability. Rhabdo occurs when damaged muscle tissue releases its proteins and electrolytes into the blood. These substances can damage the heart and kidneys and cause permanent disability or even death.
Can Rhabdomyolysis be principal diagnosis?
If the doctor documented that the patient clearly would not have been admitted for the overdose and clearly was only being admitted for the Rhabdomyolysis/AKI, then you would have additional support for placing Rhabdomyolysis or AKI as the principal diagnosis.
What is traumatic rhabdomyolysis?
Abstract. Crush syndrome or traumatic rhabdomyolysis constitutes the systemic changes seen after crush injury, i.e. the damages seen after a prolonged period of pressure on a muscle group.
When do you use B94 8?
B94. 8, Sequelae of other specified infectious and parasitic diseases. Use this code for patients who are still suffering from COVID-19 complications after clearing the initial infection. It should be combined with other diagnosis codes for the patient's ongoing symptoms.
What is the diagnosis for ICD-10 code r50 9?
9: Fever, unspecified.
When do you use Z11 52?
For example, Z11. 52 will replace Z11. 59 (Encounter for screening for other viral diseases), which the CDC previously said should be used when patients being screened for COVID-19 have no symptoms, no known exposure to the virus, and test results that are either unknown or negative.
What is uremic myopathy?
For this reason, uremic myopathy has various names, most of which refer to muscle functional abnormalities.
What are the consequences of uremic myopathy?
The two main clinical consequences associated with uremic myopathy are exercise limitation and cardiomyopathy. Uremic myopathy usually is accompanied by weakness, exercise limitation, limited endurance, and rapid-onset tiredness, although the degree of clinical expression of these manifestations varies widely
When was uremia first described?
Uremic myopathy was first described by Serratrice et al in 1967, who reported a group of patients with chronic renal failure and progressive proximal muscle weakness caused by an intrinsic disorder of muscle function, presumably secondary to uremia. 2. Serratrice G. Toga M.
Does malnutrition cause uremic myopathy?
Google Scholar. . Malnutrition, especially with protein deficiency, has been clearly associated with the development of uremic myopathy, although many well-fed dialysis patients have complained of muscular weakness and exercise limitation.
Is uremic myopathy a common clinical alteration?
Nonetheless, some reports have suggested that uremic myopathy is a common clinical alteration, with an overall prevalence of approximately 50% in dialysis patients. 3. Clyne N. Physical working capacity in uremic patients.
Popular Posts:
- 1. icd 10 code for low bmi
- 2. icd 10 code for non displaced fracture l distal fibula.
- 3. icd 10 cm code for enlarged lymph nodes, cause unknown
- 4. icd 10 code for impaired nutrition
- 5. what is the icd 10 code for 403.90
- 6. icd 10 code for ddd of l spine
- 7. icd 10 code for history of h pylori
- 8. icd 10 code for bump on hand
- 9. icd 10 code for deformity of medial and lateral mallelous
- 10. icd 10 code for postprocedural hematoma