What are symptoms of viral URI?
Oct 01, 2021 · J06.9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM J06.9 became effective on October 1, 2021. This is the American ICD-10-CM version of J06.9 - other international versions of ICD-10 J06.9 may differ. Applicable To Upper respiratory disease, acute
What does viral URI mean?
ICD-10-CM Diagnosis Code M01.X8 [convert to ICD-9-CM] Direct infection of vertebrae in infectious and parasitic diseases classified elsewhere. Direct infct of verteb in infec/parastc dis classd elswhr; Arthritis of vertebra due to viral infection; Viral arthirits of vertebra. ICD-10-CM Diagnosis Code M01.X8.
What is diagnosis of Uri?
Mar 02, 2020 · What is the ICD 10 code for viral upper respiratory infection? Acute upper respiratory infection, unspecified. J06. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. Click to see full answer.
What does acute Uri mean?
Oct 01, 2021 · Viral infection, unspecified 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code B34.9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM …
How do you code a viral upper respiratory infection?
Viral URTI should be coded:J06.9 Acute upper respiratory infection, unspecified.B97.8 Other viral agents as the cause of diseases classified to other chapters.
What is the ICD-10 code for unspecified URI?
J06.9ICD-10 code: J06. 9 Acute upper respiratory infection, unspecified - gesund.bund.de.
What is URI unspecified?
A viral upper respiratory infection, or URI, is a condition that affects your upper air passages. The most well-known type is the common cold. An infection caused by a virus, it typically enters your body through your nose or mouth.Nov 9, 2021
What are viral URI symptoms?
What are the symptoms of acute URI? Symptoms of the common cold typically include stuffy and runny nose, scratchy or sore throat, watery eyes, sneezing, mild cough, achy muscles and bones, headaches, low-grade fever, watery discharge from the nose that thickens and turns yellow or green, mild tiredness.
What is the ICD 10 code for viral illness?
9.
What is the ICD 10 code for anemia?
Code D64. 9 is the diagnosis code used for Anemia, Unspecified, it falls under the category of diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism.
What is a URI medical?
Upper Respiratory Infection (URI or Common Cold)
Is a viral URI contagious?
Yes, upper respiratory infections are contagious. They pass from person to person through respiratory droplets or hand-to-hand contact. People who have an upper respiratory infection can pass it to others through: Sneezing or coughing without covering their nose and mouth.May 25, 2021
Is a viral infection of the upper respiratory tract?
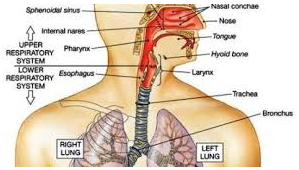
An acute URI is a contagious infection of your upper respiratory tract. Your upper respiratory tract includes the nose, throat, pharynx, larynx, and bronchi. Without a doubt, the common cold is the most well-known URI. Other types of URIs include sinusitis, pharyngitis, epiglottitis, and tracheobronchitis.
Is a URI the same as a cold?
An upper respiratory infection (URI), also known as the common cold, is one of the most common illnesses, leading to more primary care provider visits and absences from school and work than any other illness every year.
What is a viral infection of the upper respiratory tract caused by many different viruses?
Common viral respiratory diseases are illnesses caused by a variety of viruses that have similar traits and affect the upper respiratory tract. The viruses involved may be the influenza viruses, respiratory syncytial virus (RSV), parainfluenza viruses, or respiratory adenoviruses.
What are 4 types of respiratory infections?
Four of the most common types of respiratory infections are COVID-19, the flu, pneumococcal disease, and colds.Jan 27, 2021
What is the ICd 10 code for naso pharyngitis?
Ready for some good news? The common cold is still the common cold and has a simple, three-digit ICD-10 code: J00, “Acute naso-pharyngitis.” ICD-10 even includes “common cold” in the description.
What is the J00 code for rhinitis?
Infective rhinitis defaults to the “Acute naso-pharyngitis” (common cold) J00 code, discussed earlier. However, chronic rhinitis gets its own code, J31.0. Vasomotor and allergic rhinitis also have their own code series (J30). (See “Rhinitis
What is the ICD-10 code for emphysema?
For these conditions, ICD-10 uses two base code catego-ries: J43 for emphysema and J44 for chronic obstructive pulmonary disease (COPD). All codes require a fourth digit. However, without additional testing, it is unlikely that a primary care physician can clearly differentiate emphysema from chronic bronchitis. Per the National Heart, Lung, and Blood Institute (NHLBI) of the National Institutes of Health, “Most people who have COPD have both emphysema and chronic bronchitis. Thus, the general term ‘COPD’ is more accurate.”1 In
What is the ICd 10 code for nasopharyngitis?
Ready for some good news? The common cold is still the common cold and has a simple, three-digit ICD-10 code: J00, “Acute nasopharyngitis.” ICD-10 even includes “common cold” in the description.
What is the ICd 10 code for allergic rhinitis?
However, if in your clinical judgment the condition is caused by pollen, you need to document that judgment in the record and then assign code J30.1, “Allergic rhinitis due to pollen.”. Remember that ICD-10 does not prohibit you from using your clinical judgment, but your documentation must support your judgment.
What are the causes of pharyngitis?
(See “ Pharyngitis codes .”) Three additional causes of acute pharyngitis that may be identified in the primary care office are excluded from this category: gonococcus (A54.5), herpes (B00.2), and mononucleosis (B27.-). These codes are typically used for a follow-up visit after the results of previously ordered labs are available.
Can you use a diagnostic code for influenza?
As we move further down the respiratory tract, the likelihood of a primary care physician using diagnostic codes that specify the causative organism decreases, particularly in the office setting. When you make a clinical diagnosis of influenza in the office, coding will reflect an unidentified influenza virus. Therefore, depending on the presence of any additional findings, you will likely use one of several codes for “Influenza due to unidentified influenza virus.” (See “ Influenza codes .”)
What is the code for a cold nose?
Infective rhinitis defaults to the “Acute nasopharyngitis” (common cold) J00 code, discussed earlier. However, chronic rhinitis gets its own code, J31.0. Vasomotor and allergic rhinitis also have their own code series (J30). (See “ Rhinitis and other codes related to the nose .”)
What is the ICD-10 code for COPD?
For these conditions, ICD-10 uses two base code categories: J43 for emphysema and J44 for chronic obstructive pulmonary disease (COPD). All codes require a fourth digit. However, without additional testing, it is unlikely that a primary care physician can clearly differentiate emphysema from chronic bronchitis. Per the National Heart, Lung, and Blood Institute (NHLBI) of the National Institutes of Health, “Most people who have COPD have both emphysema and chronic bronchitis. Thus, the general term ‘COPD’ is more accurate.” 1 In that case, J44.9, “COPD, unspecified,” should be used. (See “ Emphysema/COPD codes .”)
What is the classification of asthma?
Classification of asthma is based on the NHLBI's “Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma” published in 2007. Coding is based on the classification level and the presence of an acute exacerbation or status asthmaticus. (See “ Asthma codes .”)

Popular Posts:
- 1. icd 10 code for prosthetic knee infection
- 2. icd 10 code for old cva non dominant weakness
- 3. icd 10 code for achilles tendon tendinopathy
- 4. what is the icd 10 code for epiglottis with tonsillitis
- 5. icd 10 code for secondary osteoarthritis
- 6. what is the icd 10 code for gram negative sepsis
- 7. icd 10 code for respiratory conditions due to smoke inhalation
- 8. icd 10 code for hiatal hernia with reflux esophagitis
- 9. icd 9 code for discogenic upper back pain
- 10. icd-10-pcs code for cystoscopy with stent placement