What are my options for squamous cell carcinoma treatment?
Treating Squamous Cell Carcinoma of the Skin
- Surgery. Different types of surgery can be used to treat squamous cell skin cancers. ...
- Radiation therapy. Radiation therapy is often a good option for patients with large cancers, especially in areas where surgery would be hard to do (such as the eyelids, ears, or ...
- Cryotherapy. ...
- Treating advanced squamous cell cancers. ...
Does squamous cell carcinoma have a high recurrence rate?
There was a 20% incidence of recurrence in 86 patients with invasive squamous cell carcinoma. The presence of solar changes in the skin did not obviate recurrence. The larger, less differentiated lesions had a greater probability of recurrence.
Is basaloid squamous cell carcinoma serious?
Though this form of skin cancer is not usually life-threatening, one major difference between basal cell and squamous cell cancers is that squamous cell cancer are more likely to grow deeper into the layers of your skin and spread to other parts of the body.
What are the symptoms of squamous cell carcinoma (SCC)?
You may see one of the following on your skin:
- Rough, reddish scaly patch
- Open sore (often with a raised border)
- Brown spot that looks like an age spot
- Firm, dome-shaped growth
- Wart-like growth
- Tiny, rhinoceros-shaped horn growing from your skin
- Sore developing in an old scar
What is the ICD 10 code for vulvar cancer?
C51. 9 - Malignant neoplasm of vulva, unspecified | ICD-10-CM.
What is the ICD 10 code for squamous cell carcinoma?
ICD-10 Code for Squamous cell carcinoma of skin, unspecified- C44. 92- Codify by AAPC.
What is vulvar intraepithelial neoplasia squamous cell carcinoma?
Having a history of precancerous conditions of the vulva. Vulvar intraepithelial neoplasia is a precancerous condition that increases the risk of vulvar cancer. Most instances of vulvar intraepithelial neoplasia will never develop into cancer, but a small number do go on to become invasive vulvar cancer.
Is vulvar carcinoma in situ cancer?
Abnormal cells are found on the surface of the vulvar skin. These abnormal cells may become cancer and spread into nearby tissue. Also called VIN and vulvar intraepithelial neoplasia.
What is squamous cell carcinoma?
Squamous cell carcinoma of the skin is a common form of skin cancer that develops in the squamous cells that make up the middle and outer layers of the skin. Squamous cell carcinoma of the skin is usually not life-threatening, though it can be aggressive.
What is the ICD 10 code for metastatic squamous cell carcinoma?
Squamous cell carcinoma of skin, unspecified C44. 92 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM C44. 92 became effective on October 1, 2021.
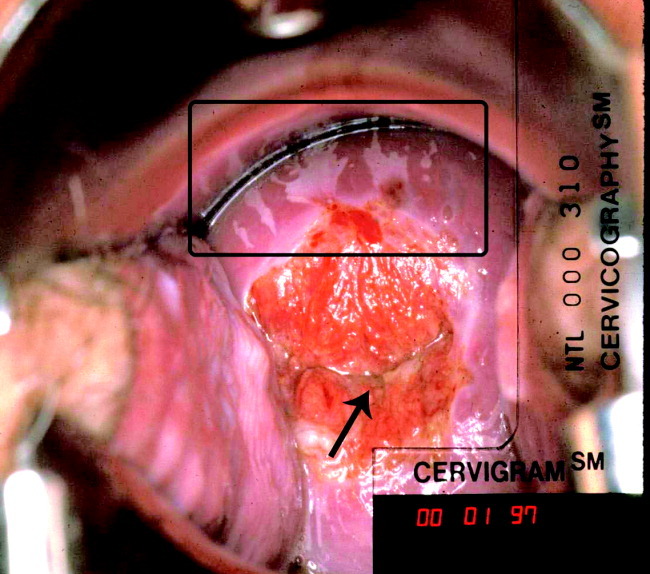
What does vulvar squamous cell carcinoma look like?
Invasive squamous cell cancer of the vulva An area on the vulva that looks different from normal – it could be lighter or darker than the normal skin around it, or look red or pink. A bump or lump, which could be red, pink, or white and could have a wart-like or raw surface or feel rough or thick.
Where is vulvar carcinoma most commonly located?
Cancer of the vulva (also known as vulvar cancer) most often affects the inner edges of the labia majora or the labia minora. It starts in the clitoris or in the Bartholin glands less often.
What is vulvar squamous mucosa?
INTRODUCTION. The vulva contains both keratinizing, hair-bearing skin; and non-keratinizing squamous mucosa, as well as subcutaneous soft tissues. Neoplastic disease of the vulva most commonly involves the epidermal layer or squamous mucosal lining, and most of these neoplasms are of squamous origin.
What is the first stage of vulvar cancer?
Stage I: The cancer has formed but has not moved beyond the vulva or perineum (the area between the rectum and the vagina.) Stage Ia: The cancer is 2 cm or smaller and has spread no more than 1 mm into the vulva's tissue. The cancer has not reached the lymph nodes.
What does vulvar cancer smell like?
Does vulvar cancer smell a particular way? Since vulvar cancer develops on the surface of the vulva, it may have a particular smell. However, during the initial stages of vulvar cancer, you may not experience any symptoms. In advanced stages, you may experience vaginal discharge with a foul smell.
Do you need chemo for vulvar cancer?
In more advanced disease, chemo might be given with radiation therapy before surgery. Chemotherapy helps the radiation work better, and this may shrink the tumor so it's easier to remove with surgery. At this time, chemo is most often used for vulvar cancers that have spread or have come back after surgery.
Is squamous cell carcinoma malignant?
The vast majority of skin cancers are basal cell carcinomas and squamous cell carcinomas. While malignant, these are unlikely to spread to other parts of the body if treated early. They may be locally disfiguring if not treated early.
How do ICD-10 code atypical squamous cells of undetermined significance?
610 for Atypical squamous cells of undetermined significance on cytologic smear of cervix (ASC-US) is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is metastatic squamous cell carcinoma?
Squamous cell carcinoma - a very common form of nonmelanoma skin cancer that originates in the squamous cells - becomes metastatic when it spreads (metastasizes) beyond the primary cancer site and affects other areas of the body.
What is atypical squamous proliferation of skin?
ATYPICAL SQUAMOUS PROLIFERATION – abnormal growth of squamous cells which could be cause by Squamous Cell Carcinoma or warts – can become Squamous Cell skin cancer. Page 2. SQUAMOUS CELL CARCINOMA – In-situ - the second most common type of skin cancer caused from sun exposure, warts, or areas of old wounds.
Where does vulva cancer form?
It forms in a woman's external genitals, called the vulva. The cancer usually develops slowly over several years. First, precancerous cells grow on vulvar skin. This is called vulvar intraepithelial neoplasia (vin), or dysplasia. Not all vin cases turn into cancer, but it is best to treat it early.
What are the risks of vulva cancer?
being older and having a human papillomavirus infection are risk factors for vulvar cancer. Treatment varies, depending on your overall health and how advanced the cancer is. It might include laser therapy, surgery, radiation or chemotherapy. nih: national cancer institute. Codes. C51 Malignant neoplasm of vulva.
What is a type 1 exclude note?
A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition. Primary or metastatic malignant neoplasm involving the vulva. Vulvar cancer is a rare type of cancer. It forms in a woman's external genitals, called the vulva.
What is the synonym for cancer of the vagina?
Includes. malignant neoplasm of skin of female genital organs. Malignant neoplasms of female genital organs. Approximate Synonyms. Cancer of the vagina, adenocarcinoma. Cancer of the vagina, primary. Cancer of the vagina, recurrent to primary site. Cancer of the vagina, squamous cell. Malignant melanoma of vagina.
What is the code for a primary malignant neoplasm?
A primary malignant neoplasm that overlaps two or more contiguous (next to each other) sites should be classified to the subcategory/code .8 ('overlapping lesion'), unless the combination is specifically indexed elsewhere.
What is a malignant neoplasm?
Malignant neoplasms of ectopic tissue are to be coded to the site mentioned, e.g., ectopic pancreatic malignant neoplasms are coded to pancreas, unspecified ( C25.9 ). A primary or metastatic malignant tumor involving the vagina. Representative examples include carcinomas and sarcomas.
What is a type 1 exclude note?
A type 1 excludes note is a pure excludes. It means "not coded here". A type 1 excludes note indicates that the code excluded should never be used at the same time as D07.1. A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition.
What chapter is neoplasms classified in?
All neoplasms are classified in this chapter, whether they are functionally active or not. An additional code from Chapter 4 may be used, to identify functional activity associated with any neoplasm. Morphology [Histology] Chapter 2 classifies neoplasms primarily by site (topography), with broad groupings for behavior, malignant, in situ, benign, ...
What is the correct coding for SCC?
Example 1: A patient returns to the dermatologist to discuss removal of his SCC on his lower lip. Proper coding is C44.02 Squamous cell carcinoma of skin of lip.
What are the risk factors for squamous cell carcinoma?
Squamous cell carcinoma is most commonly seen in fair-skinned people who have spent extended time in the sun. Other risk factors for SCC include: 1 Blue or green eyed people with blond or red hair 2 Long-term daily sun exposure, as with people that work outdoors with no sun protection or covering up 3 Many severe sunburns early in life 4 Older age. The older a person, the longer sun exposure they have had 5 Overexposure or long-term exposure to X-rays 6 Chemical exposures, such as arsenic in drinking water, tar, or working with insecticides or herbicides. 7 Tanning bed use. According to the Skin Cancer Foundation, 170,000 cases of non-melanoma skin cancer in the US each year are associated with indoor tanning. Use of indoor UV tanning equipment increases a person’s risk of developing squamous cell carcinoma by 67 percent.
What is the second most common type of skin cancer?
by John Verhovshek, MA, CPC. Squamous cell carcinoma (SCC) is the second most common type of skin cancer. It begins in the squamous cells, which comprise most of the skin’s epidermis.
What is chapter 2 of ICd 10?
ICD-10-CM chapter 2 contains codes for most benign and malignant neoplasms. As in ICD-9-CM, there is a separate Table of Neoplasms. Codes should be selected from the table. It is important to remember when accessing the Neoplasm Table, to look under the main term Skin, first, then drop to the body part, to locate the appropriate code.
What is the code for a primary malignant neoplasm?
A primary malignant neoplasm that overlaps two or more contiguous (next to each other) sites should be classified to the subcategory/code .8 ('overlapping lesion'), unless the combination is specifically indexed elsewhere.
When will the ICd 10 C44.92 be released?
The 2022 edition of ICD-10-CM C44.92 became effective on October 1, 2021.
What chapter is neoplasms classified in?
All neoplasms are classified in this chapter, whether they are functionally active or not. An additional code from Chapter 4 may be used, to identify functional activity associated with any neoplasm. Morphology [Histology] Chapter 2 classifies neoplasms primarily by site (topography), with broad groupings for behavior, malignant, in situ, benign, ...
What is the code for a primary malignant neoplasm?
A primary malignant neoplasm that overlaps two or more contiguous (next to each other) sites should be classified to the subcategory/code .8 ('overlapping lesion'), unless the combination is specifically indexed elsewhere.
When will the ICD-10 C51.0 be released?
The 2022 edition of ICD-10-CM C51.0 became effective on October 1, 2021.
What chapter is neoplasms classified in?
All neoplasms are classified in this chapter, whether they are functionally active or not. An additional code from Chapter 4 may be used, to identify functional activity associated with any neoplasm. Morphology [Histology] Chapter 2 classifies neoplasms primarily by site (topography), with broad groupings for behavior, malignant, in situ, benign, ...
Popular Posts:
- 1. icd code for major depression recurrent moderate
- 2. icd 10 code for post nasal drainage
- 3. icd 10 code for reveals proximal transverse fracture of humerus
- 4. icd 10 code for s p right foot fracture
- 5. icd 10 code for hip dislocation
- 6. icd code for bell's palsy
- 7. icd 10 code for fibrosis
- 8. icd 10 code for trustissl
- 9. icd 10 code for heart muscle disorder
- 10. icd 10 code for chnages inthe liver