How does doctor check for deviated septum?
When to visit the ENT doctor in case of a deviated nasal septum?
- nasal congestion or blockage on either one side or both sides of the nose
- postnasal drip
- nose bleeds
- nasal infections
- facial pain
- sinusitis or sinus infections
- dry nose due to drying out of mucous membranes
- noisy breathing
- snoring
- headaches
How to detect if you have a deviated nasal septum?
If you have a severely deviated septum causing nasal obstruction, it can lead to:
- Dry mouth, due to chronic mouth breathing
- A feeling of pressure or congestion in your nasal passages
- Disturbed sleep, due to the unpleasantness of not being able to breathe comfortably through the nose at night
Is surgery necessary for a deviated septum?
The answer primarily depends upon your symptoms. Deviated Septum Surgery Is Not Always Necessary Often, a deviation in the septum is discovered incidentally during a routine examination. Patients may not be aware they have this condition if they haven’t experienced any symptoms.
Which treatment is best for deviated nasal septum?
Treatments for a Deviated Septum
- Decongestants. Available orally or by spray, nasal decongestants can significantly reduce the swelling in your nasal cavity.
- Antihistamines. Antihistamines work by relieving symptoms like postnasal drip, runny nose, or chronic sneezing. ...
- Corticosteroid Sprays. ...
- Surgery. ...
What is ICD-10 code for deviated nasal septum?
ICD-10 code: J34. 2 Deviated nasal septum | gesund.bund.de.
What is the CPT code for deviated nasal septum?
What is a CPT® code? The Current Procedural Terminology (CPT®) codes offer doctors and health care professionals a uniform language for coding medical services and procedures to streamline reporting, increase accuracy and efficiency.
What is J34 89 diagnosis?
J34. 89 - Other specified disorders of nose and nasal sinuses | ICD-10-CM.
What is a deviated septum or whatever it is?
A deviated septum occurs when your nasal septum is significantly displaced to one side, making one nasal air passage smaller than the other. A deviated septum occurs when the thin wall (nasal septum) between your nasal passages is displaced to one side.
What is the CPT code 90834?
CPT® code 90834: Psychotherapy, 45 minutes.
Is CPT code the same as ICD 10?
CPT codes refer to the treatment being given, while ICD codes refer to the problem that the treatment is aiming to resolve. The two work hand-in-hand to quickly provide payors specific information about what service was performed (the CPT code) and why (the ICD code).
What is DX R05?
ICD-10-CM Code for Cough R05.
What is the ICD-10-CM code for nasal obstruction?
ICD-10-CM Code for Nasal congestion R09. 81.
What is the ICD-10 code for nasal septal perforation?
ICD-10 Code for Congenital perforated nasal septum- Q30. 3- Codify by AAPC.
Is deviated septum the same as a crooked septum?
A deviated septum occurs when the septum is severely shifted away from the midline. The most common symptom from a badly deviated or crooked septum is difficulty breathing through the nose. The symptoms are usually worse on one side, and sometimes actually occur on the side opposite the bend.
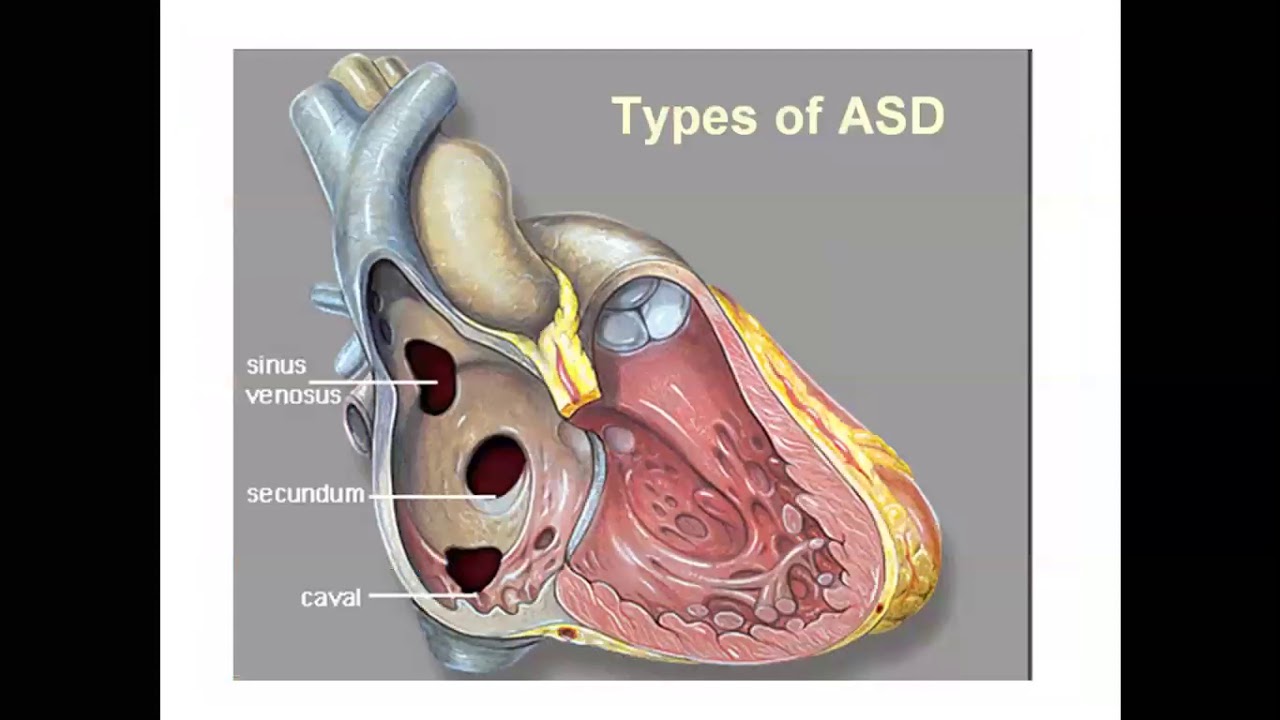
What are the types of deviated nasal septum?
Baumann classified types of septal deviation into 6 types, where each type has several additional features: Type 1: septal crest, Type 2: cartilaginous deviated nose, Type 3: high septal crest deviation, Type 4: caudally inclined septum, Type 5: septal crest, and Type 6: caudally inclined septum [25].
Who diagnoses deviated septum?
Your general physician may look at your nose to diagnose a deviated septum. However, when treatment is needed, an otolaryngologist (ear, nose, and throat doctor) will likely be recommended. An ear, nose, and throat doctor can diagnose and treat a deviated septum.
The ICD code J342 is used to code Nasal septum deviation
Nasal septum deviation or deviated nasal septum (DNS) is a physical disorder of the nose, involving a displacement of the nasal septum. Some displacement is common, affecting 80% of people, most unknowingly.
Coding Notes for J34.2 Info for medical coders on how to properly use this ICD-10 code
Inclusion Terms are a list of concepts for which a specific code is used. The list of Inclusion Terms is useful for determining the correct code in some cases, but the list is not necessarily exhaustive.
MS-DRG Mapping
DRG Group #011-013 - Tracheostomy for face, mouth and neck diagnoses with MCC.
ICD-10-CM Alphabetical Index References for 'J34.2 - Deviated nasal septum'
The ICD-10-CM Alphabetical Index links the below-listed medical terms to the ICD code J34.2. Click on any term below to browse the alphabetical index.
Equivalent ICD-9 Code GENERAL EQUIVALENCE MAPPINGS (GEM)
This is the official exact match mapping between ICD9 and ICD10, as provided by the General Equivalency mapping crosswalk. This means that in all cases where the ICD9 code 470 was previously used, J34.2 is the appropriate modern ICD10 code.
How many passageways are there in the nasal cavity?
Each nasal cavity is divided into 3 passageways (the superior, middle and inferior meati) by the projection of the 4 nasal turbinates (inferior, middle, superior and supreme) from the lateral walls of the internal nose. The inferior turbinate is a separate bone, while the other 3 are part of the ethmoid bone.
Where are the nasal valves located?
The nasal valves or vestibules are the areas just inside the nostrils comprised of cartilage and are structured to work together to keep the nasal airway open by facilitating airflow resistance during breathing. The internal valves are located in each side of the nose at the upper edge of the hair bearing area, while the outer (external) valves are at the edge of the nostril rim. Aging, congenital abnormality or prior nasal surgery may cause nasal valve impairment such as nasal valve collapse, also referred to as vestibular stenosis. Nasal valves may narrow, weaken or collapse resulting in symptoms of nasal obstruction.
Is septal surgery a clean contaminated procedure?
The authors concluded that septal surgery with early removal of nasal packing is a clean-contaminated procedure and does not require routine antibiotic prophylaxis because of the low infection risk. Karaman et al (2012) examined the effect of antibiotic prophylaxis and septoplasty on nasal flora.
Is nasal packing effective after septoplasty?
However, it was since found that not only is nasal packing ineffective in this regard, it can actually cause these complications. In a prospective, randomized, comparison study, Awan and Iqbal (2008) compared nasal packing versus no packing after septoplasty (n = 88). These investigators examined the incidence of a variety of post-operative signs and symptoms in patients (15 years of age and older), who did (n = 44) and did not (n = 44) undergo nasal packing following septoplasty. They found that patients who underwent packing experienced significantly more post-operative pain, headache, epiphora, dysphagia, and sleep disturbance on the night of surgery. Oral and nasal examinations 7 days post-operatively revealed no significant difference between the 2 groups in the incidence of bleeding, septal hematoma, adhesion formation, and local infection. Finally, subjects in the packing group reported a moderate-to-high level of pain during removal of the packing. These findings confirmed that nasal packing after septoplasty is not only unnecessary, it is actually a source of patient discomfort and other signs and symptoms.
Is septoplasty cosmetic enhancement?
Because the septum is deviated in most adults, the potential exists for over-utilization of septoplasty in asymptomatic individuals. The primary indication for surgical treatment of a deviated septum is nasal airway obstruction.
Is septoplasty necessary for Aetna?
Aetna considers septoplasty medically necessary when any of the following clinical criteria is met: Asymptomatic septal deformity that prevents access to other intranasal areas when such access is required to perform medical necessary surgical procedures (e.g., ethmoidectomy); or.
Does septoplasty increase S. aureus colonization?
The authors concluded that septoplasty increases S. aureus colonization and decreases normal flora. Antibiotics do not protect against S. aureus colonization and contribute to a decrease in normal flora.

Popular Posts:
- 1. icd 10 code for neural foraminal narrowing cervical
- 2. icd 10 code for left breast cyst
- 3. icd 10 code for ventricular ectopics
- 4. icd-10 code for history of cva
- 5. icd 10 code for left eye mild conjunctivitis
- 6. icd 9 code for compression fracture of l3
- 7. icd-10-pcs code for open approach for vaginal suspension of uterus
- 8. icd-10 code for migranes
- 9. icd-10-cm code for prostate cancer
- 10. icd 10 code for filling up paperwork