What is the ICD 10 code for chronic pain syndrome?
Chronic pain syndrome. G89.4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM G89.4 became effective on October 1, 2018.
What is the ICD 10 code for dull pain?
R52 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM R52 became effective on October 1, 2020. This is the American ICD-10-CM version of R52 - other international versions of ICD-10 R52 may differ. ... Pain may be sharp or dull. It may come and go, or it may ...
What is the ICD 10 code for headache syndromes?
G89.4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM G89.4 became effective on October 1, 2021. This is the American ICD-10-CM version of G89.4 - other international versions of ICD-10 G89.4 may differ. headache syndromes ( G44.-) abdomen pain ( R10.-)
What are the ICD-10-CM codes for spinal pain?
spine pain ( M54.-) Reimbursement claims with a date of service on or after October 1, 2015 require the use of ICD-10-CM codes.
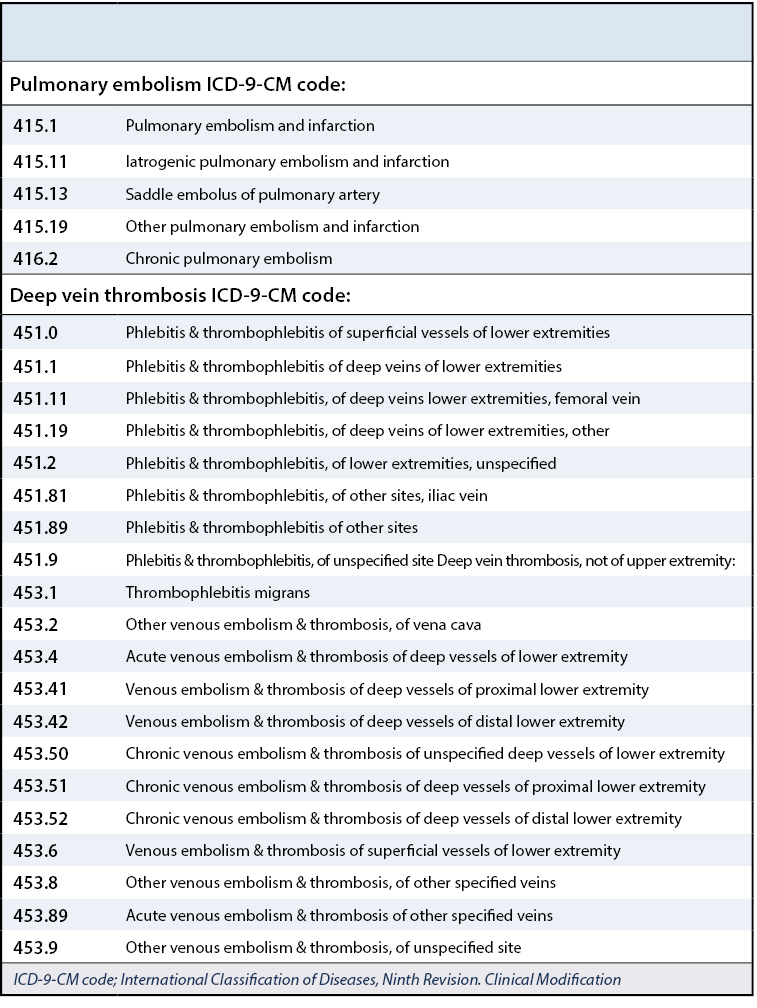
What is the ICD 9 code for pain?
ICD-9-CM (2007 Version) “PAIN (338)” Codes.
What is the ICD-10-CM code for chronic pain?
NOTE: To utilize these chronic pain diagnosis codes, the exact nature of pain should be specifically documented in the patient medical records; such as “chronic” to utilize ICD-10 code G. 89.29 or the diagnosis term “chronic pain syndrome” to utilize ICD-10 code G89. 4.
What is considered as chronic pain?
Chronic or persistent pain is pain that carries on for longer than 12 weeks despite medication or treatment. Most people get back to normal after pain following an injury or operation. But sometimes the pain carries on for longer or comes on without any history of an injury or operation.
What is the ICD 9 code?
International Classification of Diseases,Ninth Revision (ICD-9) The International Classification of Diseases (ICD) is designed to promote international comparability in the collection, processing, classification, and presentation of mortality statistics.
What is the ICD-10-CM code for pain management?
R52 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM R52 became effective on October 1, 2021. This is the American ICD-10-CM version of R52 - other international versions of ICD-10 R52 may differ.
When do you use code U09 9?
Instructions for coding COVID-19U07.1 COVID-19, virus detected.U07.2 COVID-19, virus not detected.U08.9 COVID-19 in its own medical history, unspecified.U09.9 Post-infectious condition after COVID-19, unspecified.U10.9 Multisystemic inflammatory syndrome associated with COVID-19, unspecified.More items...
What is the most common type of chronic pain?
Common types of chronic pain include:Arthritis, or joint pain.Back pain.Neck pain.Cancer pain near a tumor.Headaches, including migraines.Testicular pain (orchialgia).Lasting pain in scar tissue.Muscle pain all over (such as with fibromyalgia).More items...•
How do you prove chronic pain?
Imaging and Nerve Tests If your healthcare provider suspects your chronic pain is caused by bone, muscle or nerve damage, he may have you undergo a scan or nerve testing. These include x-rays and MRIs, which can reveal underlying bone and tissue damage.
Is chronic pain syndrome a diagnosis?
The criteria for the diagnosis of chronic pain syndrome are nonspecific. Neither term has been validated for use in determining impairment or disability. The diagnosis of pain disorder relies heavily upon a patient's self-report for its accuracy and requires that all other diagnoses be ruled out.
What does an ICD-9 code look like?
The format for ICD-9 diagnoses codes is a decimal placed after the first three characters and two possible add-on characters following: xxx. xx. ICD-9 PCS were used to report procedures for inpatient hospital services from Volume 3, which represent procedures that were done at inpatient hospital facilities.
How do you use ICD-9?
General guidelines for ICD-9 coding Carry the code to the fourth or fifth digit when possible. Link the diagnosis code (ICD-9) to the service code (CPT) on the insurance claim form to identify why the service was rendered, thereby establishing medical necessity.
What is ICD-9 and ICD-10 difference?
ICD-9 uses mostly numeric codes with only occasional E and V alphanumeric codes. Plus, only three-, four- and five-digit codes are valid. ICD-10 uses entirely alphanumeric codes and has valid codes of up to seven digits.
What are the 4 types of pain?
THE FOUR MAJOR TYPES OF PAIN:Nociceptive Pain: Typically the result of tissue injury. ... Inflammatory Pain: An abnormal inflammation caused by an inappropriate response by the body's immune system. ... Neuropathic Pain: Pain caused by nerve irritation. ... Functional Pain: Pain without obvious origin, but can cause pain.
What are the 3 types of pain?
There are 3 widely accepted pain types relevant for musculoskeletal pain: Nociceptive pain (including nociceptive inflammatory pain) Neuropathic pain. Nociplastic pain.
What is the difference between acute and chronic pain?
Acute vs. Chronic Pain. Pain is a sign that something has happened, that something is wrong. Acute pain happens quickly and goes away when there is no cause, but chronic pain lasts longer than six months and can continue when the injury or illness has been treated.
Is chronic pain a disability?
The SSA does not consider chronic pain to be a disability, so there is no listing for it in the SSA's Blue Book. Chronic pain, even if it is severe and disabling, does not qualify unless you can prove it is caused by a verifiable condition that lasts for at least 12 months.
What is the ICd 10 code for chronic pain?
Chronic pain, not elsewhere classified 1 G89.2 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. 2 The 2021 edition of ICD-10-CM G89.2 became effective on October 1, 2020. 3 This is the American ICD-10-CM version of G89.2 - other international versions of ICD-10 G89.2 may differ.
When will the ICD-10 G89.2 be released?
The 2022 edition of ICD-10-CM G89.2 became effective on October 1, 2021.
What is the meaning of pain?
Pain is a feeling triggered in the nervous system. Pain may be sharp or dull.
What is the pain of the coccyx?
Pain of coccyx greater than 3 months, chronic. Clinical Information. A disorder characterized by the sensation of marked discomfort, distress or agony. An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons.
When will the ICD-10-CM R52 be released?
The 2022 edition of ICD-10-CM R52 became effective on October 1, 2021.
How long does pain last?
Once you take care of the problem, pain usually goes away. However, sometimes pain goes on for weeks, months or even years.
How many codes are required to describe a condition?
A code also note instructs that 2 codes may be required to fully describe a condition but the sequencing of the two codes is discretionary, depending on the severity of the conditions and the reason for the encounter.
Is G89 a reimbursement code?
Pain, not elsewhere classified. G89 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. The 2021 edition of ICD-10-CM G89 became effective on October 1, 2020.

Popular Posts:
- 1. icd 10 cm code for chronic diastolic chf
- 2. what is the icd 10 code for traumatic spinal cord injry
- 3. icd 10 code for personal history of r breast cancer
- 4. icd 10 code for periorificial dermatitis
- 5. icd 10 code for speech delay without hearing loss
- 6. icd-9-cm code for tympanoplasty for repair of a tympanic membrane perforation
- 7. icd 10 code for history of heimcolectomy
- 8. icd 10 diagnosis code for multilevel degenerative changes cervical spine
- 9. icd 10 code for frostbite right hand
- 10. icd 10 code for vanco trough