What is the ICD 9 code for cellulitis of the foot?
most severe category for which they had an ICD-9-CM code. Our presumptive order was Gangrene > Osteo-myelitis > Foot ulcer > Cellulitis/abscess of foot > Cellu-litis/abscess of toe > Paronychia. This was based on clinical judgment, but corresponds in part to Wagner’s classification system for diabetic foot ulcers, which
What is the ICD 10 code for diabetic foot ulcer?
Jul 06, 2010 · We determined which ICD-9-CM codes served to identify patients with different types of diabetic foot infections and ranked them in declining order of severity: Gangrene, Osteomyelitis, Ulcer, Foot cellulitis/abscess, Toe cellulitis/abscess, Paronychia.
Are cellulitis and diabetes linked in ICD-10-CM?
DEpiC contains computerized VA and Medicare patient-level data for patients with diabetes since 1998. We determined which ICD-9-CM codes served to identify patients with different types of diabetic foot infections and ranked them in declining order of severity: Gangrene, Osteomyelitis, Ulcer, Foot cellulitis/abscess, Toe cellulitis/abscess ...
Is there a classification system for diabetic foot infections in ICD-9?
ICD-9-CM 250.80 is a billable medical code that can be used to indicate a diagnosis on a reimbursement claim, however, 250.80 should only be used for claims with a date of service on or before September 30, 2015. For claims with a date of service on or after October 1, 2015, use an equivalent ICD-10-CM code (or codes).
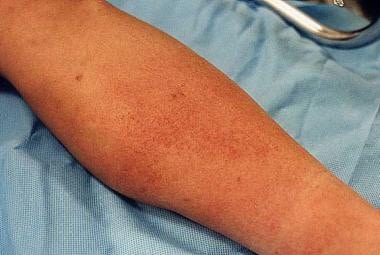
Is diabetic foot ulcer cellulitis?
In patients with diabetes, any foot infection is potentially serious. Diabetic foot infections range in severity from superficial paronychia to deep infection involving bone. Types of infection include cellulitis, myositis, abscesses, necrotizing fasciitis, septic arthritis, tendinitis, and osteomyelitis.Jul 1, 2008
How do you code an infected diabetic foot ulcer?
622).” Of these options, the most commonly used codes for diabetic foot ulcer are E10. 621 (Type 1 diabetes mellitus with foot ulcer) and E11. 621 (Type 2 diabetes mellitus with foot ulcer). “Code first” indicates that an additional code is required and you should list this first.
What is the ICD 10 code for infected diabetic foot ulcer?
ICD-10-CM Code for Type 2 diabetes mellitus with foot ulcer E11. 621.
What is ICD 10 code for diabetic wound infection?
E11. 621 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM E11. 621 became effective on October 1, 2021.
What is the ICD-10 code for foot ulcer?
ICD-10 code L97. 509 for Non-pressure chronic ulcer of other part of unspecified foot with unspecified severity is a medical classification as listed by WHO under the range - Diseases of the skin and subcutaneous tissue .
What are diabetic ulcers?
Diabetic ulcers are open wounds or sores usually found on the bottom of feet. These ulcers affect many people with diabetes and experts suggest that about 15 percent of diabetics will develop one or more at some point in their lifetime.
What is the ICD-10 code for foot infection?
X7 for Direct infection of ankle and foot in infectious and parasitic diseases classified elsewhere is a medical classification as listed by WHO under the range - Arthropathies .
What is the icd10 code for diabetes?
E08, Diabetes mellitus due to underlying condition. E09, Drug or chemical induced diabetes mellitus. E10, Type 1 diabetes mellitus. E11, Type 2 diabetes mellitus.
How do you code a diabetic foot exam?
CPT codes 11055, 11056, and 11057 will also be covered when billed with one of the diabetes, neurological or vascular disease diagnosis codes listed below any one of the following routine foot care diagnosis codes: B35. 3, L60.Apr 1, 2018
What is the ICD-10 code for skin infection?
ICD-10 code: L08. 9 Local infection of skin and subcutaneous tissue, unspecified - gesund.bund.de.
What is a Wagner ulcer?
The most widely accepted classification system for diabetic foot ulcers and lesions is the Wagner ulcer classification system, which is based on the depth of penetration, the presence of osteomyelitis or gangrene, and the extent of tissue necrosis (Table 2).Nov 1, 2002
What is the ICD-10 code for gangrene?
I96ICD-10 code I96 for Gangrene, not elsewhere classified is a medical classification as listed by WHO under the range - Diseases of the circulatory system .
What is the ICd 10 code for diabetes?
Icd-10 Diagnosis Code E11.628. If you have diabetes, your blood glucose, or blood sugar, levels are too high. Over time, this can cause problems with other body functions, such as your kidneys, nerves, feet, and eyes. Having diabetes can also put you at a higher risk for heart disease and bone and joint disorders.
How many people have diabetes mellitus?
With more than 23 million Americans diagnosed with diabetes mellitus , thecondition where the body either cant respond to insulin correctly or just cant produce it, codersneed to know changes to diabetic coding guidelines for ICD-10.
What are the long term complications of diabetes?
Other long-term complications of diabetes include skin problems, digestive problems, sexual dysfunction, and problems with your teeth and gums. Very high or very low blood sugar levels can also lead to emergencies in people with diabetes.
What happens to bone when you have a sequestra?
As the disease progresses, areas of bone may become isolated by the infection and lack of circulation, forming islands or segments of necrotic bone that remain infected (sequestra). These areas become a source of recurrent episodes of acute infection and possible draining wounds.
Does diabetes cause cellulitis?
However, diabetes in and of itself does not cause cellulitis.
Can high blood glucose cause heart problems?
Over time, high blood glucose can lead to serious problems with your heart, eyes, kidneys, nerves, and gums and teeth. You have a higher risk of type 2 diabetes if you are older, obese, have a family history of diabetes, or do not exercise. Having prediabetes also increases your risk.
Can you link cellulitis and diabetes?
NO, the link is not assumed when patients have cellulitis and diabetes documented. The physician would need to document the cellulitis as a diabetic skin complication or link the two conditions with verbiage such as due to, associated with or similar terms.
What is the I96 code for gangrene?
I96 has an Excludes 2 for gangrene in diabetes mellitus, and the Alphabetic Index instructs us that Type 2 diabetes “with gangrene” goes to E11.52, according to the assumptive rule. The coding guidelines remind us of the “basic rule of coding…that further research must be done when the title of the code suggested by the Alphabetic Index clearly ...
Does diabetes cause ulcers?
There is an obvious clinical relationship. Peripheral vascular disease and peripheral neuropathy, also more common in diabetes, contribute to the development and severity of ulcers and gangrene.
Does gangrene affect diabetes?
However, I strongly object to the characterization that the “gangrene is associated with the pressure ulcer rather than the diabetes mellitus.”. Gangrene has to affect a body part (e.g., musculoskeletal system, intestine portion, gallbladder, etc.); it does not occur diffusely, i.e., directly due to diabetes.

Popular Posts:
- 1. icd 10 cm code for elevated bs
- 2. icd 10 code for deconditioning unspecified
- 3. icd 9 code for cryptogenic stroke
- 4. icd 10 code for nerve stimulator implant
- 5. 2047 icd 10 code for projectile vomiting
- 6. icd code for rosacea
- 7. icd 10 cm code for chest pain
- 8. icd 10 code for fall from roof
- 9. icd 10 code for breast lump right
- 10. icd-10 code for radiology