What is the ICD 9 code for gangrene?
2015 ICD-9-CM Diagnosis Code 785.4 Gangrene 2015 Billable Thru Sept 30/2015 Non-Billable On/After Oct 1/2015 ICD-9-CM 785.4 is a billable medical code that can be used to indicate a diagnosis on a reimbursement claim, however, 785.4 should only be used for claims with a date of service on or before September 30, 2015.
How do you code diabetic foot ulcers with gangrene?
Gangrene ICD-9-CM 785.4 is a billable medical code that can be used to indicate a diagnosis on a reimbursement claim, however, 785.4 should only be used for claims with a date of service on or before September 30, 2015. For claims with a date of service on or after October 1, 2015, use an equivalent ICD-10-CM code (or codes).
What are the symptoms of gangrene in feet?
785.4 is a legacy non-billable code used to specify a medical diagnosis of gangrene. This code was replaced on September 30, 2015 by its ICD-10 equivalent. ICD-9:
What is the ICD 10 code for inguinal hernia with gangrene?
ICD-10-CM Diagnosis Code I73.01 [convert to ICD-9-CM] Raynaud's syndrome with gangrene. Gangrene due to raynaud disease; Gangrene due to secondary raynaud phenomenon; Raynaud disease with gangrene; Raynauds disease with gangrene; Raynauds syndrome with gangrene; Secondary raynaud phenomenon with gangrene.
What is the ICD-10 code for right foot gangrene?
Atherosclerosis of native arteries of extremities with gangrene, right leg. I70. 261 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD-10 code for gangrene of left foot?
262.
Does necrosis code to gangrene?
Necrosis is commonly documented in the patient records with traumatic wounds, burns, pressure sores etc. Necrosis due to lack of oxygen such as with a MI would be considered part of the MI code as would any necrosis with infection in pneumonia. Gangrene would seem to be a complication of necrotic tissue.
What is the code for gangrene?
ICD-10 code I96 for Gangrene, not elsewhere classified is a medical classification as listed by WHO under the range - Diseases of the circulatory system .
Is gangrene and necrosis the same thing?
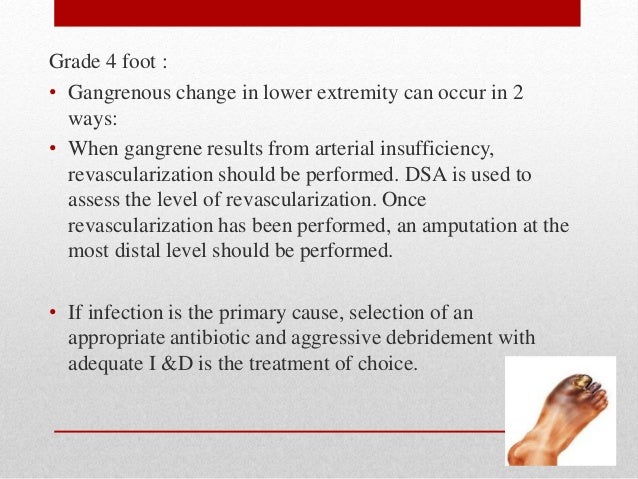
Gangrene is dead tissue (necrosis) consequent to ischemia. In the image above, we can see a black area on half of the big toe in a diabetic patient. This black area represents necrosis—dead tissue—in fact, gangrene of the big toe.
What causes gangrene in feet?
Gangrene of the hand and foot Gangrene results when blood flow to a certain area of your body is interrupted, causing tissue decay and death. Gangrene often affects the fingers or toes. Causes of gangrene include: Lack of blood supply.
What is the ICD-10 code for necrotic tissue?
0: Necrosis of skin and subcutaneous tissue, not elsewhere classified.
Which type of gangrene occurs in diabetes?
Wet gangrene typically occurs in people who have frostbite or experience a severe burn. People with diabetes may unknowingly develop wet gangrene after experiencing a minor toe or foot injury.
Is gangrene a disease?
Dry gangrene is a form of coagulative necrosis that develops in ischemic tissue, where the blood supply is inadequate to keep tissue viable. It is not a disease itself, but a symptom of other diseases.
What is the ICD-10 code for diabetes with gangrene?
E11. 52 Type 2 diabetes mellitus with diabetic peripheral angiopathy with gangrene.
What is gangrene not elsewhere classified?
Gangrene, not elsewhere classified I96- A type 1 excludes note is for used for when two conditions cannot occur together, such as a congenital form versus an acquired form of the same condition. gangrene in atherosclerosis of native arteries of the extremities (
What is the ICD-10 code for peripheral arterial disease?
Provider's guide to diagnose and code PAD Peripheral Artery Disease (ICD-10 code I73. 9) is estimated to affect 12 to 20% of Americans age 65 and older with as many as 75% of that group being asymptomatic (Rogers et al, 2011).
What is the ICd 10 code for gangrene?
785.4 is a legacy non-billable code used to specify a medical diagnosis of gangrene. This code was replaced on September 30, 2015 by its ICD-10 equivalent.
How to tell if you have gangrene?
If the gangrene is internal, you may run a fever and feel unwell, and the area may be swollen and painful.
What is the treatment for gangrene?
Gangrene is a serious condition. It needs immediate attention. Treatment includes surgery, antibiotics, and oxygen therapy. In severe cases an amputation may be necessary.
What does NOS mean in a syllable?
NOS "Not otherwise specified" - This abbreviation is the equivalent of unspecified.
What is the diabetes code for gangrene?
mitchellde. The only diabetes code that states with gangrene is for peripheral angiopathy with gangrene. If the patient has this condition and the diabetic foot ulcers, then code both conditions and you may use the peripheral angiopathy with gangrene first listed.
What is the code for gangrene ulcers?
However if that is not the diagnosis and it states only dues ethic foot ulcers with gangrene, then you code the with foot ulcers code and add the L97 code that applies which will probably be the one that indicates with necrosis of muscle or necrosis of bone.
Does DM gangrene have higher DRG?
DM gangrene has higher DRG when coded but there's a confusing statement on the coding handbook for DM complications that foot ulcer code should be assigned first with additional code for the ulcer site and, if gangrene is present, it should be assigned as an additional code.
Can you code L97 with diabetes?
You are correct it is an exclude 1 exclusion and cannot be coded with the diabetes code. This will over ride the note at L97 to code first the I96. I would speak with whomever you took the class thru and point out that this is incorrect.
How to treat gangrene on foot?
Restoring Blood Flow to Treat Gangrene on the Foot. Gangrene is a severe form of poor circulation and restoring blood flood must be done immediately to saved toes or the foot from amputation. For patients with gangrene due to Peripheral Artery Disease, a minimally invasive procedure called Lumivascular Atherectomy is an option.
Why is gangrene more likely to develop in patients with diabetes?
Patients with Peripheral Artery Disease due to smoking or diabetes are more susceptible to developing gangrene because their arteries may be blocked or obstructed.
Is gangrene a risk to diabetics?
Another risk of gangrene is that amputation may be the only way to remove the dead tissue and prevent further spread. Amputation is a risk to a patient in and of itself. In fact, research has that diabetic patients with foot disease fear leg or foot amputation more than they fear death.
Can gangrene cause inability to move?
When the gangrene becomes very severe you may have an inability to move your foot due to tissue death. Risks of Gangrene Foot. Gangrene can become potentially fatal if not treated in time.
Can you walk on gangrene?
Additionally, you may notice that walking on or touching the gangrene affected area on your foot is very painful initially. However, as gangrene develops you will notice a loss of sensation in your foot. When the gangrene becomes very severe you may have an inability to move your foot due to tissue death. Risks of Gangrene Foot.
Does gangrene turn your feet dark?
The affected foot will typically look “decayed” and as it progresses the skin will begin to turn dark and dry out. The skin of the foot may also become much shinier in appearance before it starts shedding. This shedding will make a clear distinction on your foot between the healthy skin and the gangrene affected area.
Why do PAD patients have gangrene?
Patients with PAD are more likely to have gangrene on their feet because the poor circulation leads to tissue death and gangrene. Symptoms of Gangrene on the Foot. Some of the major symptoms of gangrene include, a discoloration in the foot or toes. The affected foot will typically look “decayed” and as it progresses the skin will begin ...
Does gangrene affect diabetes?
However, I strongly object to the characterization that the “gangrene is associated with the pressure ulcer rather than the diabetes mellitus.”. Gangrene has to affect a body part (e.g., musculoskeletal system, intestine portion, gallbladder, etc.); it does not occur diffusely, i.e., directly due to diabetes.
Does I96 have gangrene?
Not only does it not make clinical sense, but it doesn’t adhere to coding rules, either. I96 has an Excludes 2 for gangrene in diabetes mellitus, and the Alphabetic Index instructs us that Type 2 diabetes “with gangrene” goes to E11.52, according to the assumptive rule. The coding guidelines remind us of the “basic rule ...
Is a diabetic foot ulcer considered a pressure ulcer?
In the first article in this series, I compared pressure ulcers and diabetic foot ulcers (the latter are considered non-pressure chronic ulcers in ICD-10-CM). My conclusion was that there is significant overlap, but heel ulcers are prime candidates to be classified as pressure injuries by providers. Ultimately, their documentation will determine whether an ulcer on the foot of a diabetic will be considered a “diabetic foot ulcer” or a pressure ulcer. This article will explore whether they are mutually exclusive conditions.

Popular Posts:
- 1. icd 10 code for hemosis
- 2. icd 10 diagnosis code for ambulatory dysfunction
- 3. icd 10 code for abnormal heart sounds
- 4. icd 10 code for pregnancy dehydration
- 5. icd 10 code for administrative exam
- 6. icd 10 code for left chest injury
- 7. icd-10 code for fetal tachycardia in pregnancy
- 8. icd 10 code for oh
- 9. icd-10 code for flu vaccine administration
- 10. icd 10 code for herp cyst