What is the best treatment for degenerative disc disease?
Billable Medical Code for Degeneration of Lumbar or Lumbosacral Intervertebral Disc Diagnosis Code for Reimbursement Claim: ICD-9-CM 722.52. Code will be replaced by October 2015 and relabeled as ICD-10-CM 722.52. The Short Description Is: Lumb/lumbosac disc degen. Known As
How to cure degenerative disc disease naturally?
Neurologic disorder due to degeneration of lumbar intervertebral disc. ICD-9-CM codes are used in medical billing and coding to describe diseases, injuries, symptoms and conditions. ICD-9-CM 722.52 is one of thousands of ICD-9-CM codes used in healthcare.
What are the side effects of degenerative disc disease?
Degeneration of intervertebral disc, site unspecified. ICD-9-CM 722.6 is a billable medical code that can be used to indicate a diagnosis on a reimbursement claim, however, 722.6 should only be used for claims with a date of service on or before September 30, 2015.
What are symptoms of degenerative disc disease?
ICD-9 Code 722.52 Degeneration of lumbar or lumbosacral intervertebral disc. ICD-9 Index; Chapter: 710–739; Section: 720-724; Block: 722 Intervertebral disc disorders; 722.52 - Lumb/lumbosac disc degen
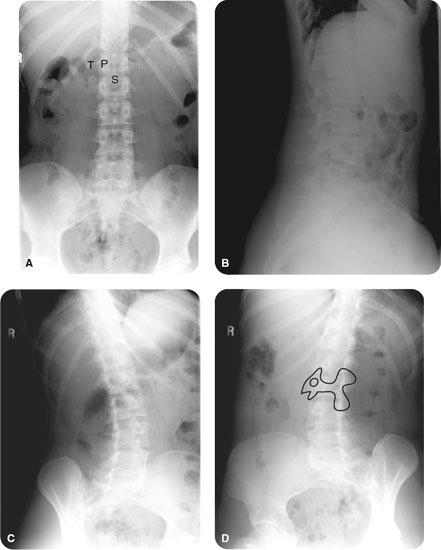
What is the ICD 9 code for degenerative disc disease?
The ICD-9 category used for this condition is dependent upon the site. 722.4 is the correct code for degenerative disease of the cervical intervertebral disc. 722.51 is the correct diagnosis code for thoracic degenerative disc disease.
How do you code degenerative disc disease?
ICD-10-CM Code for Other intervertebral disc degeneration, lumbar region M51. 36.
What is ICD-10 code for degenerative disc disease lumbar?
Other intervertebral disc degeneration, lumbar region M51. 36 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the ICD-10 code for degenerative changes of lumbar spine?
Other intervertebral disc disorders, lumbosacral region M51. 87 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM M51. 87 became effective on October 1, 2021.
Is degenerative disc disease a diagnosis?
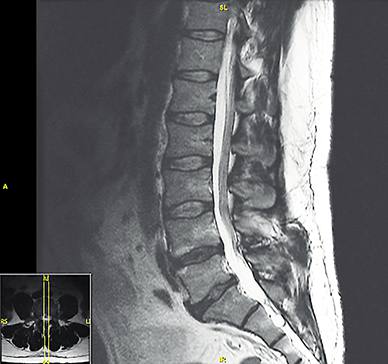
How is degenerative disc disease diagnosed? A diagnosis is based on a medical history and a physical examination, as well as the symptoms and the circumstances where the pain started. Magnetic resonance imaging can show damage to discs, but it alone cannot confirm degenerative disc disease.
Is degenerative disc disease and degenerative joint disease the same thing?
Degenerative Joint Disease is most commonly know as Osteoarthritis. Similar to Degenerative Disc Disease, with Degenerative Joint Disease, the 'cushion' of cartilage between the joints beings to deteriorate. The joints most commonly affected by DJD are the knees, followed by the hips, hands and spine.May 10, 2019
What is ICD-10 code for multilevel degenerative disc disease?
ICD-10-CM Diagnosis Code G31 G31.
What is lumbar disc disease?
Lumbar disk disease may occur when a disc in the low back area of the spine bulges or herniates from between the bony area of the spine. Lumbar disk disease causes lower back pain and leg pain and weakness that is made worse by movement and activity.
What is the ICD-10 code for chronic back pain?
5 – Low Back Pain. ICD-Code M54. 5 is a billable ICD-10 code used for healthcare diagnosis reimbursement of chronic low back pain.
What is degenerative lumbar spine?
Degenerative disc disease in the lumbar spine, or lower back, refers to a syndrome in which age-related wear and tear on a spinal disc causes low back pain.
What is diagnosis code M5136?
icd10 - M5136: Other intervertebral disc degeneration, lumbar region.
What is the ICd 10 code for lumbar disc degeneration?
722.52 is a legacy non-billable code used to specify a medical diagnosis of degeneration of lumbar or lumbosacral intervertebral disc. This code was replaced on September 30, 2015 by its ICD-10 equivalent.
What are the bones that make up the spine?
Your backbone, or spine, is made up of 26 bone discs called vertebrae. The vertebrae protect your spinal cord and allow you to stand and bend. A number of problems can change the structure of the spine or damage the vertebrae and surrounding tissue. They include. Infections. Injuries.
What causes pain in the spine?
Conditions, such as ankylosing spondylitis and scoliosis. Bone changes that come with age, such as spinal stenosis and herniated disks. Spinal diseases often cause pain when bone changes put pressure on the spinal cord or nerves. They can also limit movement.
What is a code note?
Code also note - A "code also" note instructs that two codes may be required to fully describe a condition, but this note does not provide sequencing direction. Code first - Certain conditions have both an underlying etiology and multiple body system manifestations due to the underlying etiology.
What does excludes2 mean?
An excludes2 note indicates that the condition excluded is not part of the condition represented by the code, but a patient may have both conditions at the same time. When an Excludes2 note appears under a code, it is acceptable to use both the code and the excluded code together, when appropriate.
What is the 7th character in a code?
The 7th character must always be the 7th character in the data field. If a code that requires a 7th character is not 6 characters, a placeholder X must be used to fill in the empty characters.
Known As
Degenerative disc disease is also known as degeneration of intervertebral disc, and intervertebral disc degeneration. This applies to degenerative disc disease NOS and narrowing of intervertebral disc or space NOS.
Degenerative Disc Disease Definition and Symptoms
Degenerative disc disease is a term used for a condition in which a damaged vertebral disc causes chronic pain. Symptoms include back or neck pain, lower back pain, and pain that gets worse with movements.
What is a DDD code?
Degenerative Disc Disease (DDD) is a gradual process that may compromise the spine. It is a relatively common disorder. Degenerative changes to a spinal disc often refer to those changes that cause the loss of normal structure and/or function.
What is intervertebral disc?
The intervertebral disc is one structure prone to the degenerative changes associated with wear and tear such as aging, weight bearing, injury as well as misuse (e.g. smoking). These changes are linked and may lead to the disc’s inability to handle mechanical stress.
Is there a cure for osteoarthritis?
There is no cure for osteoarthritis, but medications can relieve the symptoms.
Popular Posts:
- 1. icd 10 code for procedure inserts an anterior nasal packing into left nostril
- 2. icd 10 code for hiv screening patient is asymptomatic
- 3. icd-10 code for cellulitis of left knee
- 4. what is icd 10 code for high risk sexual practices
- 5. give 2 examples for when an external cause icd code is not required
- 6. the icd 10 cm code for accidental puncture of adrenal gland during kidney biopsy.
- 7. icd 10 code for contusion of right elbow
- 8. icd 10 code for liver tumor of unknown etiology
- 9. icd-10-pcs code for picc line placement
- 10. 2016 icd 10 code for lesion hepatic lobe