ICD-9-CM procedure codes are two numeric digits followed by a decimal, which is then followed by another one or two digits. The codes begin with 00.01, to describe a therapeutic ultrasound of vessels in the head and neck, and they end with 99.99, which describes other miscellaneous procedures.
| 00.01 | ‑ | 0. PROCEDURES AND INTERVENTIONS , NOT ELSEWHERE CLASSIFIED (00) |
|---|---|---|
| 06.01 | ‑ | 2. OPERATIONS ON THE ENDOCRINE SYSTEM (06-07) |
| 08.01 | ‑ | 3. OPERATIONS ON THE EYE (08-16) |
| 17.11 | ‑ | 3A. OTHER MISCELLANEOUS DIAGNOSTIC AND THERAPEUTIC PROCEDURES (17) |
| 18.01 | ‑ | 4. OPERATIONS ON THE EAR (18-20) |
How ICD 10 is different from ICD 9 codes?
- Similar to the diagnosis code set, the alpha characters in ICD 10 code sets are not case-sensitive.
- The letters “O” and “I” are not in the code set. ...
- The 7 characters in the procedure code set help in providing very precise details. ...
- The fourth character identifies the part of the body. ...
How to assign ICD 9 diagnosis codes?
Types of Pain
- Traumatic:
- Psychological:
- Postoperative:
- Site Specific:
- Pain as a Symptom: The pain is a symptom of a confirmed diagnosis (e.g., abdominal pain due to an ulcer; ulnar pain due to a fracture).
What is ICD 9 coding used for?
The ICD-9 was used to code and classify mortality data from death certificates until 1999, when use of ICD-10 for mortality coding started. The ICD-9-CM consists of: a tabular list containing a numerical list of the disease code numbers in tabular form; an alphabetical index to the disease entries; and
What is the ICD - 9 code for routine medical exam?
ICD-9 V70.0 is routine general medical examination at a health care facility (V700). This code is grouped under diagnosis codes for supplementary classification of factors influencing health status and contact with health services.
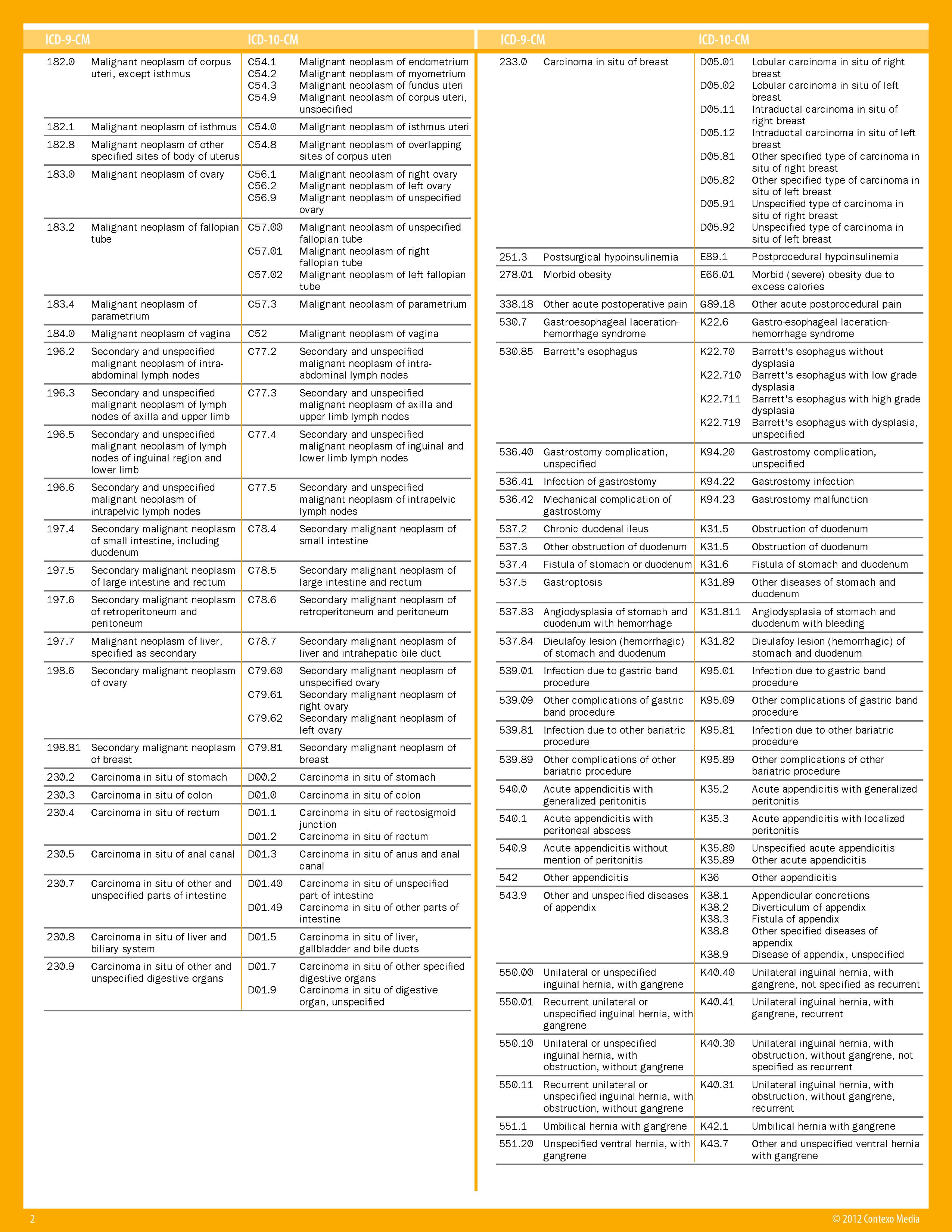

What are ICD-9 procedure codes?
ICD-9-CM is the official system of assigning codes to diagnoses and procedures associated with hospital utilization in the United States. The ICD-9 was used to code and classify mortality data from death certificates until 1999, when use of ICD-10 for mortality coding started.
What codes are used for procedures?
For some types of care, procedures are billed using CPT (Current Procedural Terminology) /HCPCS (Healthcare Common Procedure Coding System) codes, rather than ICD. CPT codes, also called Level I HCPCS codes, are used to bill physician services and they are copyrighted by the American Medical Association (AMA).
Is ICD-10 used for coding procedures?
The U.S. developed a Clinical Modification (ICD-10-CM) for medical diagnoses based on WHO's ICD-10 and CMS developed a new Procedure Coding System (ICD-10-PCS) for inpatient procedures. ICD-10-CM replaces ICD-9-CM, volumes 1 and 2, and ICD-10-PCS replaces ICD-9-CM, volume 3.
What is the difference between CPT and ICD-9 procedure codes?
In a concise statement, ICD-9 is the code used to describe the condition or disease being treated, also known as the diagnosis. CPT is the code used to describe the treatment and diagnostic services provided for that diagnosis.
What is a medical procedure code?
CPT codes, or procedural codes, describe what kind of procedure a patient has received while ICD codes, or diagnostic codes, describe any diseases, illnesses or injuries a patient may have.
What is primary procedure code?
PRIMARY PROCEDURE (OPCS) is the same as attribute CLINICAL CLASSIFICATION CODE. PRIMARY PROCEDURE (OPCS) is the OPCS Classification of Interventions and Procedures code which is used to identify the primary Patient Procedure carried out.
What is the difference between diagnosis code and procedure code?
2. The CPT code describes what was done to the patient during the consultation, including diagnostic, laboratory, radiology, and surgical procedures while the ICD code identifies a diagnosis and describes a disease or medical condition. 3. CPT codes are more complex than ICD codes.
What is the difference between ICD-9 and ICD-10?
ICD-9 uses mostly numeric codes with only occasional E and V alphanumeric codes. Plus, only three-, four- and five-digit codes are valid. ICD-10 uses entirely alphanumeric codes and has valid codes of up to seven digits.
How do you code outpatient procedures?
How will ICD-10 Codes Help Outpatient Procedures?ICD-10-CM codes will be used for all inpatient and outpatient diagnoses.ICD-10-PCS will only be used by hospitals for inpatient procedures.CPT will be used by all healthcare providers for outpatient procedures.
What is an example of an ICD-9 code?
Most ICD-9 codes are three digits to the left of a decimal point and one or two digits to the right of one. For example: 250.0 is diabetes with no complications. 530.81 is gastroesophageal reflux disease (GERD).
What is an ICD code used for?
ICD stands for the International Classification of Disease. The ICD provides a method of classifying diseases, injuries, and causes of death.
How do I find ICD codes?
A Five-Step ProcessStep 1: Search the Alphabetical Index for a diagnostic term. ... Step 2: Check the Tabular List. ... Step 3: Read the code's instructions. ... Step 4: If it is an injury or trauma, add a seventh character. ... Step 5: If glaucoma, you may need to add a seventh character.
What is the ICD-9-CM?
The Health Insurance Portability and Accountability Act of 1996 (HIPAA) mandates that Volume 3 of the International Classification of Diseases, 9th Revision, Clinical Modification ( ICD-9-CM) be used to code inpatient services on medical claims.
What is the ICd 9 code for leech therapy?
The codes begin with 00.01, to describe a therapeutic ultrasound of vessels in the head and neck, and they end with 99.99, which describes other miscellaneous procedures. ICD-9-CM indicates that leech therapy falls under 99.99. Being able to read and understand the code manual is an asset for hospitals to submit accurate claims for accurate reimbursement.
Why are HCPCS codes used?
Any services these patients receive are described by the use of HCPCS codes because they do are not in an inpatient treatment status. All procedure codes are attached to specific charges that a hospital has determined represents its reasonable cost to perform the service.
Why are medical coders important?
Being able to bear all the code variations in mind while reviewing medical records and assembling claims, professional medical coders and medical billers reduce fraud and abuse of the healthcare reimbursement system , limiting a hospital’s legal exposure to charges of the same.
What is volume 3 code?
CMS states that hospitals can use Volume 3 codes for internal tracking purposes, but the HIPAA standard is to use Healthcare Common Procedure Coding System (HCPCS) codes in every other setting when financial transactions take place with third-party payers.
What is an inpatient patient?
Inpatients are patients who are admitted to the hospital and stay at least overnight.
Do medical billers use code sets?
Medical billers and medical coders who do not use these code sets regularly have still been trained in their use. A solid, well-rounded education is what professional medical coders and billers bring to their jobs, applying a consistent philosophy to coding that governs every medical claim for payment.
When was the ICd 9-CM code set adopted?
ICD-9-CM (Clinically Modified) was adopted in United States in 1979. The code set is updated at least once a year, based on the input of providers, payers, and other key stakeholders. A new generation and much larger code set, ICD-10, will replace ICD-9 codes on Oct 1, 2015.
When was the ICD-9-CM standard established?
Already the standard for diagnostic and inpatient hospital coding in the United States, ICD-9-CM was mandated in 2003 by the Health Insurance Portability and Accountability Act of 1996 (HIPAA).
When was the ICD-9-CM first used?
ICD-9-CM (Clinically Modified) was adopted in United States in 1979.
When did Medicare start using ICD-9 codes?
Medicare began requiring the use of ICD 9 diagnosis codes on claims in the 1980's and was soon followed by commercial insurance providers. These codes are a 5 digit number which has 3 digits followed by a decimal and then a 2 digit number. ICD-9 Codes Organization. Here's a categorical listing of IDC 9 codes:
What does ICD stand for in medical billing?
ICD stands for International Classification of Diseases.
What is the ICD code for health?
The International Statistical Classification of Diseases and Related Health Problems (commonly known as the ICD) provides alpha-numeric codes to classify diseases and a wide variety of signs, symptoms, abnormal findings, complaints, social circumstances and external causes of injury or disease. Nearly every health condition can be assigned ...
Who is the author of the AHA coding handbook?
The handbook is authored by Nelly Leon-Chisen, RHIA , Director of Coding and Classification at the AHA.
Organization of ICD-9-CM Volume 3
- ICD-9-CM procedure codes are two numeric digits followed by a decimal, which is then followed by another one or two digits. The codes begin with 00.01, to describe a therapeutic ultrasound of vessels in the head and neck, and they end with 99.99, which describes other miscellaneous procedures. ICD-9-CM indicates that leech therapy falls under 99.99...
Uses of ICD-9-CM Procedure Codes
- The Center for Medicare and Medicaid Services (CMS) which administrates the implementation of HIPAA, has offered clear guidance that Volume 3 procedure codes are only to be used in the inpatient setting to obtain reimbursement. CMS states that hospitals can use Volume 3 codes for internal tracking purposes, but the HIPAA standard is to use Healthcare Common Procedure Co…
Appropriate Use of ICD-9-CM Volume 3
- In the medical office setting, most billing software is loaded with a database of the complete set of ICD-9-CM codes, both diagnostic and procedural. Even if they are not appropriate, Volume 3 codes are available to medical billers and medical coders in the outpatient setting. Properly trained and certified medical coders and professional medical coders recogize the difference be…
Popular Posts:
- 1. icd 10 code for chronic leg edema
- 2. icd 10 cm code for pravastatin
- 3. icd 10 cm code for umbilical hernia
- 4. icd 9 cm code for carotid atherosclerosis
- 5. icd 10 diagnosis code for repeated falls
- 6. icd 10 code for lue edema
- 7. icd 10 code for thoracic spine fracture
- 8. icd-10 code for pulmonary edema with chf
- 9. icd 10 cm code for cellulitis on left lower extremity
- 10. icd 10 code for encounter for pain management