What is the ICD 10 code for postural tachycardia syndrome (POTS)?
Postural tachycardia syndrome (preferred in Great Britain and abbreviated “PoTS.”) POTS has not been assigned a specific ICD-10 code; the following are commonly used: I49.8, Other specified cardiac dysrhythmia (POTS is listed as an example) I95.1, Orthostatic hypotension (sometimes occurs with POTS)
How is postural orthostatic tachycardia diagnosed?
The diagnosis of POTS is based on clinical history (>3 months of daily intolerance of upright position) coupled with postural tachycardia (>40 beats per minute increase). Acute and intermittent symptoms do not qualify for the diagnosis.
What are the genetic etiologies of postural orthostatic tachycardia (pots)?
The genetics of POTS are unknown. However, about 15% of patients with POTS have a first-degree relative with POTS, and POTS is much more common in whites than other races. [ Shaw: 2019] Presumably, there are some genetic origins of these variations.
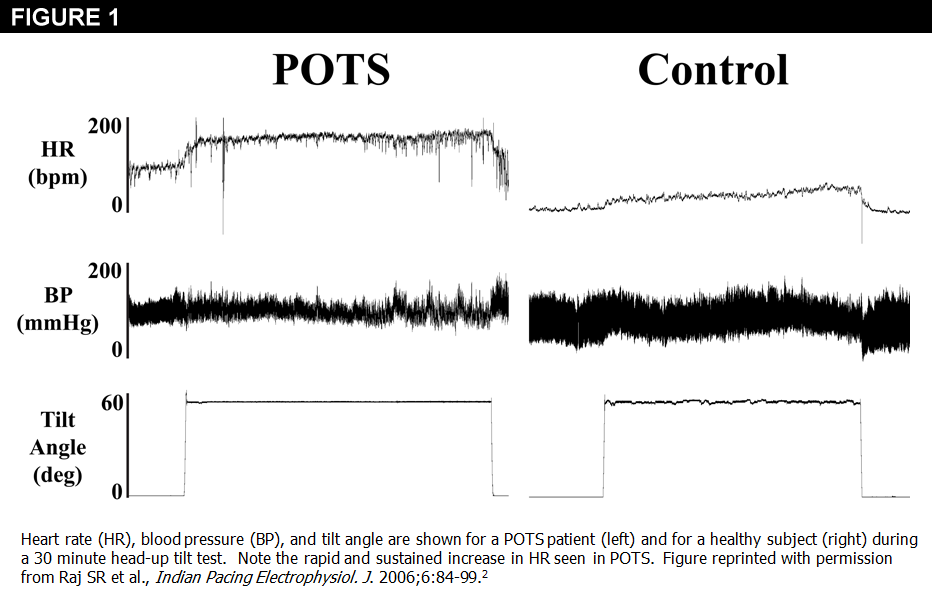
What is orthostatic tachycardia?
This is known as orthostatic (upright) tachycardia (fast heart rate). It occurs without any coinciding drop in blood pressure, as that would indicate orthostatic hypotension. Certain medications to treat POTS may cause orthostatic hypotension.
What is the ICD 10 code for postural orthostatic tachycardia syndrome?
As you may know, ICD-10 currently lists POTS under “I49. 8 – Other specified cardiac arrhythmias.” ICD-10 notes that this code also “applicable to” Brugada syndrome, coronary sinus rhythm disorder, ectopic rhythm disorder, and nodal rhythm disorder.
What does postural orthostatic tachycardia syndrome?
Postural orthostatic tachycardia syndrome (POTS) is a condition that affects blood flow. POTS causes the development of symptoms -- usually lightheadedness, fainting and an uncomfortable, rapid increase in heartbeat -- that come on when standing up from a reclining position and relieved by sitting or lying back down.
What is another name for postural orthostatic tachycardia syndrome?
However, POTS is not a new illness; it has been known by other names throughout history, such as DaCosta's Syndrome, Soldier's Heart, Mitral Valve Prolapse Syndrome, Neurocirculatory Asthenia, Chronic Orthostatic Intolerance, Orthostatic Tachycardia and Postural Tachycardia Syndrome.
What are the different types of postural orthostatic tachycardia syndrome?
There are two main forms of POTS:Partial dysautonomic - Patients appear to have mild damage to nerves that affect involuntary bodily function (peripheral autonomic neuropathy), such as the heartbeat. ... Hyperadrenergic - a less common type of POTS that appears more gradually and to have a genetic component.
How long does a POTS episode last?
In POTS, the heart rate stays elevated for more than a few seconds upon standing (often 10 minutes or more), symptoms occur frequently, and the condition lasts for more than a few days.
How long does it take for POTS to go away?
Some sources estimate that as many as 1 million people in the United States have POTS. Some people have symptoms that completely disappear within 2 to 5 years, and others have symptoms that come and go over their lifetime. People with POTS also experience different degrees of symptom severity.
When did POTS become a diagnosis?
POTS was first described 1940. Low et al from the Mayo clinic did the pioneering work on this condition. Robertson of the Vanderbilt autonomic laboratories stated it was one of the most common conditions in young females.
What is the difference between orthostatic hypotension and POTS?
POTs is defined by a fast pulse on standing, and is not the same as orthostatic hypotension (low blood pressure on standing), or syncope (passing out in any position).
Why is POTS called Grinch syndrome?
It seems reasonable to offer POTS a new name based on its underlying pathophysiology – “The Grinch Syndrome”, because in this famous children's book by Dr. Seuss, the main character had a heart that was “two sizes too small.”
What is the opposite of POTS syndrome?
Dysautonomia is the medical term for when the autonomic nervous system (ANS) does not work as it should. The symptoms vary widely, but they can include fainting, low blood pressure, and breathing problems.
What is the difference between POTS and dysautonomia?
Postural Orthostatic Tachycardia Syndrome (POTS) POTS is the most common dysautonomia and is characterized by symptoms in multiple organ systems and an abnormal increase in heart rate (30 bpm in adults, 40 bpm in teens) upon standing.
What can mimic POTS syndrome?
A pheochromocytoma can mimic POTS (or vice versa) because of the paroxysms of hyperadrenergic symptoms including palpitation, although pheochromocytoma patients are more likely to have these symptoms while supine than POTS patients. Plasma or urinary metanephrines22 can screen for pheochromocytoma.
What causes postural orthostatic tachycardia syndrome?
Causes of PoTS Sometimes it can develop suddenly after a viral illness or traumatic event, or during or after pregnancy. Some of the other known causes are: hypermobile Ehlers-Danlos syndrome. other underlying conditions – such as diabetes, amyloidosis, sarcoidosis, lupus, Sjögren's syndrome or cancer.
Can PoTS be life threatening?
POTS is not life-threatening. It's about dealing with the symptoms that you experience and trying to reduce the frequency of your palpitations, shortness of breath, and stop you from blacking out.
Does PoTS Increase Risk of Stroke?
These antibodies may be directed against clotting factors, platelets, and/or the cells that line blood vessel walls and they cause the blood to be too sticky. This results in an increased risk of blood clots in: 1) Arteries–causing most commonly stroke or heart attack.
Can you get disability for PoTS?
If your POTS symptoms are severe and you are unable to continue working or do not expect that you will be unable to work for at least the next 12 months, then you may be able to obtain a disability benefit from the SSA. The SSA uses a comprehensive guide called the Blue Book to classify disabilities.
What is postural orthostatic tachycardia syndrome?
Postural orthostatic tachycardia syndrome (POTS) is a form of autonomic dysfunction with orthostatic intolerance that affects up to 1% of adolescents with chronic fatigue, dizziness, and, often, gastrointestinal discomfort or other forms of chronic pain. With treatment, most patients can fully recover and return to normal life activities.
When is tachycardia testing needed?
Testing is useful only when needed to confirm postural tachycardia, narrow the differential diagnosis, or evaluate for comorbidities.
What is chronic orthostatic intolerance?
Chronic (>3 months) orthostatic intolerance with daily symptoms impairing normal function. Symptoms, such as dizziness, come on when upright and abate when recumbent.
How long to measure heart rate for postural dizziness?
With the patient resting calmly supine for at least a few minutes, measure the resting heart rate and blood pressure and measure them again after the patient stands and remains still for at least 3 minutes. An increase in heart rate of more than 40 beats per minute would be considered excessive. Formal tilt table testing could corroborate the finding.
Why are there no practice guidelines for POTS?
There are no official practice guidelines, mostly because of a lack of comparative studies of treatment options. However, these review articles focus on the management of POTS in adolescents:
Is there a classification of POTS?
There is no clinically useful classification of POTS – either the patient has it or not. A distinction is that similar symptoms without excessive postural tachycardia count as “orthostatic intolerance” instead of POTS. Orthostatic intolerance is treated similarly to POTS (increased fluid and salt intake, daily aerobic exercise, adequate sleep, cognitive behavioral therapy) but usually does not require medications.
What are the symptoms of a POTS?
Nausea and gastro-intestinal symptoms are common in POTS. Medication management of delayed gastric emptying and the dysmotility associated with irritable bowel syndrome (functional gastrointestinal disorder) are commonly experienced with POTS.
Is POTS a condition?
Surprisingly there is no ICD-10 code for POTS...... it is a well-documented condition after all.
Is POTS a diagnosis?
I have see that one used as well. POTS is a diagnosis that I see quite often and different physicians use different dx codes. Thanks for your input.
When was postural tachycardia syndrome first described?
Postural tachycardia syndrome was coined in 1982 in a description of a patient who had postural tachycardia, but not orthostatic hypotension. Ronald Schondorf and Phillip A. Low of the Mayo Clinic first used the name postural orthostatic tachycardia syndrome, POTS, in 1993.
What is the subtype of tachycardia?
The high norepinephrine levels contribute to symptoms of tachycardia. Another subtype, neuropathic POTS , is associated with denervation of sympathetic nerves in the lower limbs. In this subtype, it is thought that impaired constriction of the blood vessels causes blood to pool in the veins of the lower limbs.
What is the rate of heart rate when standing up?
In adults the primary manifestation is an increase in heart rate of more than 30 beats per minute within ten minutes of standing up. The resulting heart rate is typically more than 120 beats per minute. For people aged between 12 and 19, the minimum increase for diagnosis is 40 beats per minute. This is known as orthostatic (upright) tachycardia (fast heart rate). It occurs without any coinciding drop in blood pressure, as that would indicate orthostatic hypotension. Certain medications to treat POTS may cause orthostatic hypotension. It is accompanied by other features of orthostatic intolerance —symptoms that develop in an upright position and are relieved by reclining. These orthostatic symptoms include palpitations, light-headedness, chest discomfort, shortness of breath, nausea, weakness or "heaviness" in the lower legs, blurred vision, and cognitive difficulties. Symptoms may be exacerbated with prolonged sitting, prolonged standing, alcohol, heat, exercise, or eating a large meal.
What is POTS in medical terms?
Postural orthostatic tachycardia syndrome ( POTS) is a condition in which a change from lying to standing causes an abnormally large (or higher than normal) increase in heart beat rate. This occurs with symptoms that may include lightheadedness, trouble thinking, blurred vision, or weakness. Other commonly associated conditions include Ehlers–Danlos syndrome, mast cell activation syndrome, irritable bowel syndrome, insomnia, chronic headaches, chronic fatigue syndrome, and fibromyalgia. It can be treated with lifestyle changes such as increasing fluid and salt intake, compression stockings, rising slowly after lying down, avoiding prolonged bedrest, and medication.
Is POTS a chronic fatigue syndrome?
There are some overlaps between POTS and chronic fatigue syndrome, with evidence of POTS in 10–20% of CFS cases. Fatigue and reduced exercise tolerance are prominent symptoms of both conditions, and dysautonomia may underlie both conditions. POTS can sometimes be a paraneoplastic syndrome associated with cancer.
Is POTS a hereditary condition?
POTS can also co-occur in all types of Ehlers–Danlos syndrome (EDS), a hereditary connective tissue disorder marked by loose hypermobile joints prone to subluxations and dislocations, skin that exhibits moderate or greater laxity, easy bruising, and many other symptoms. A trifecta of POTS, EDS, and Mast Cell Activation Syndrome (MCAS) is becoming increasingly more common, with a genetic marker common among all three conditions. POTS is also often accompanied by vasovagal syncope, with a 25% overlap being reported. There are some overlaps between POTS and chronic fatigue syndrome, with evidence of POTS in 10–20% of CFS cases. Fatigue and reduced exercise tolerance are prominent symptoms of both conditions, and dysautonomia may underlie both conditions.
Can a person with POTS have a sinus tachycardia?
People with POTS can be misdiagnosed with inappropriate sinus tachycardia as they present similarly. One distinguishing feature is those with POTS rarely exhibit >100 bpm while in a supine position, while patients with IST often have a resting heart rate >100 bpm. Additionally patients with POTS display a more pronounced change in heart rate in response to postural change.
Popular Posts:
- 1. icd 10 code for lower extremity pain and swelling
- 2. icd 10 code for chf with preserved ejection fraction
- 3. icd-10 code for lipid panel screening
- 4. icd 10 code for abscess of right scrotum due to group b streptococcus
- 5. icd code for oral thrush
- 6. icd 10 code for dvt right basilic vein
- 7. icd 10 code for anhydramnios
- 8. icd 10 code for peripheral neuropathic pain
- 9. icd 10 code for epidural lipomatosis
- 10. what is the icd 10 code for fall