What is ICD10 code for personal history of abscesses?
Z87.2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM Z87.2 became effective on October 1, 2020. This is the American ICD-10-CM version of Z87.2 - other international versions of ICD-10 Z87.2 may differ.
What is the diagnosis code for abscess?
Peritonsillar abscess
- Valid for Submission. J36 is a billable diagnosis code used to specify a medical diagnosis of peritonsillar abscess. ...
- Tabular List of Diseases and Injuries. ...
- Index to Diseases and Injuries. ...
- Approximate Synonyms
- Clinical Information. ...
- Convert J36 to ICD-9 Code
- Information for Patients. ...
What are the differential diagnoses for epidural abscess?
Work-up
- Strongly consider imaging the entire spine to assess for non-contiguous epidural abscess
- MRI with gadolinium is the diagnostic test of choice
- CT with IV contrast may provide usual information regarding bony integrity and fluid collections while awaiting MRI
How to code superficial incision and drainage of an abscess?
- CPT 10080 is for a “simple” incision and drainage of a pilonidal cyst.
- CPT 10081 is for a “complicated” incision and drainage.
- Our lay description of these procedures which can be found in resources such as Encoder Pro or the Coder’s Desk Reference tells us that simple incision and drainage procedure are ...
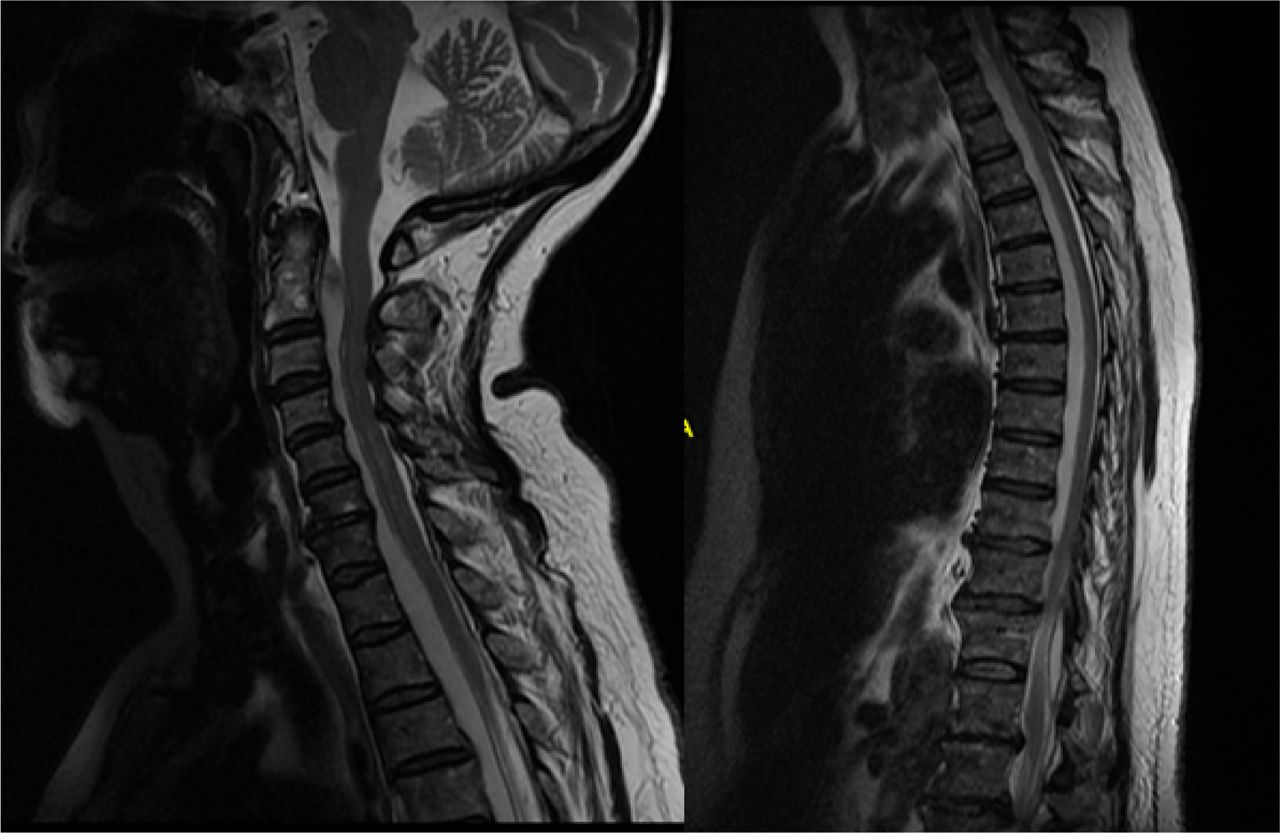
What is the ICD 10 code for epidural abscess?
Extradural and subdural abscess, unspecified G06. 2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM G06. 2 became effective on October 1, 2021.
What is epidural abscess?
An epidural abscess is an infection that forms in the space between your skull bones and your brain lining (intracranial epidural abscess). Quite often, it forms in the space between the bones of your spine and the lining membrane of your spinal cord (spinal epidural abscess).
What is the ICD 10 code for lumbar abscess?
ICD-10 code G06. 1 for Intraspinal abscess and granuloma is a medical classification as listed by WHO under the range - Diseases of the nervous system .
Is epidural abscess a CNS infection?
Epidural abscess is a rare but important suppurative infection of the central nervous system. Abscesses that are enclosed within the bony confines of the skull or spinal column can expand to compress the brain or spinal cord and cause severe symptoms, permanent complications, or even death.
How is a spinal epidural abscess diagnosed?
A spinal epidural abscess is an accumulation of pus in the epidural space that can mechanically compress the spinal cord. Diagnosis is by MRI or, if unavailable, myelography followed by CT. Treatment involves antibiotics and sometimes drainage of the abscess.
What are spinal abscesses?
Spinal cord abscess is the swelling and irritation (inflammation) and the collection of infected material (pus) and germs in or around the spinal cord.
What is the ICD 10 code for abscess?
L02. 91 - Cutaneous abscess, unspecified | ICD-10-CM.
What is an epidural mass?
Metastatic epidural spinal cord compression is defined as the presence of tumor in the spinal canal causing compression of the spinal cord.
What is the ICD 10 code for paraspinal abscess?
M60. 08 is the appropriate code for abscess muscle.
How common is spinal epidural abscess?
Spinal epidural abscess involving actinomycosis is rare. Spinal epidural abscess has an estimated incidence rate of 0.2 to 2.8 cases per 10,000 per year, with the peak incidence occurring in people who are in their 60s and 70s. The most common causative agent is Staphylococcus aureus.
Where is the epidural space?
vertebral columnThe epidural space is located within the vertebral column and extends from the foramen magnum to the sacral hiatus. Its main anatomic delineations are the tough dura mater, which is the outermost covering of the spinal cord, and the vertebral periosteum.
Is epidural abscess an emergency?
Spinal epidural abscess (SEA) is a rare, highly morbid, and often life-threatening, neurosurgical emergency characterized most often by a suppurative monomicrobial infection of the central nervous system, confined within the epidural space between the dura mater and the vertebral periosteum.
How is an epidural abscess treated?
The signs and symptoms of epidural abscess are nonspecific and can range from low back pain to sepsis. The treatment of choice in most patients is surgical decompression followed by four to six weeks of antibiotic therapy. Nonsurgical treatment may be appropriate in selected patients.
Is epidural abscess an emergency?
Spinal epidural abscess (SEA) is a rare, highly morbid, and often life-threatening, neurosurgical emergency characterized most often by a suppurative monomicrobial infection of the central nervous system, confined within the epidural space between the dura mater and the vertebral periosteum.
Can epidural abscess heal?
Treatments. Treatment of spinal epidural abscesses typically includes surgery and antibiotics or antifungals. In some cases, treatment may include only antibiotics. Antibiotics will be given typically for 4-6 weeks.
What causes abscess?
Most abscesses are caused by a bacterial infection. When bacteria enter your body, your immune system sends infection-fighting white blood cells to the affected area. As the white blood cells attack the bacteria, some nearby tissue dies, creating a hole which then fills with pus to form an abscess.
Popular Posts:
- 1. icd-10 code for death certificate
- 2. icd 10 code for history of carcinoma in situ breast
- 3. icd 10 code for systolic murmur
- 4. icd 10 code for venous thrombosis preven
- 5. icd 10 cm code for bydureon pen
- 6. icd-10 code for rotator cuff tendinitis unspecified
- 7. care for previous c section icd 10 code
- 8. icd 9 code for ventriculoperitoneal shunt
- 9. icd 10 code for dilation and curettage cpt code
- 10. icd 10 cm code for senile cataract of left eye