What ICD 10 cm code(s) are reported?
What is the correct ICD-10-CM code to report the External Cause? Your Answer: V80.010S The External cause code is used for each encounter for which the injury or condition is being treated.
What is the ICD 10 code for severe pain?
What is the ICD 10 code for severe pain? Pain, unspecified . R52 is a billable /specific ICD -10- CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is the diagnosis code for pain?
ICD-9 DIAGNOSIS ICD-10 DIAGNOSIS 724.1 Pain in thoracic spine M54.6 Pain in thoracic spine 724.2 Lumbago M54.5 Low back pain 725.4 Backache, unspecified M54.89 Other dorsalgia ...
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
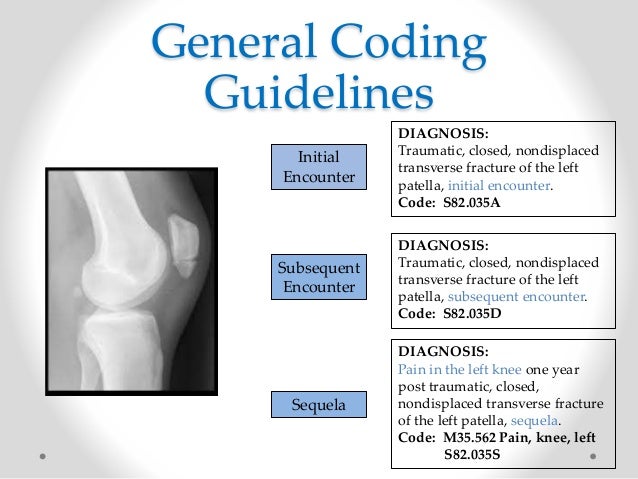
What is the icd10 code for pain?
ICD-10 code R52 for Pain, unspecified is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is the ICD-10-CM code for chronic pain?
NOTE: To utilize these chronic pain diagnosis codes, the exact nature of pain should be specifically documented in the patient medical records; such as “chronic” to utilize ICD-10 code G. 89.29 or the diagnosis term “chronic pain syndrome” to utilize ICD-10 code G89. 4.
What is the ICD-10-CM code for low back pain?
M54. 50 (Low back pain, unspecified) M54. 51 (Vertebrogenic low back pain)
How do you code Acute on chronic pain?
You may report the acute/chronic pain code (G89) as a secondary diagnosis if the diagnosis provides additional, relevant information not adequately explained by the primary diagnosis code.
What is the meaning of pain?
Pain is a feeling triggered in the nervous system. Pain may be sharp or dull.
How long does pain last?
Once you take care of the problem, pain usually goes away. However, sometimes pain goes on for weeks, months or even years.
When will the ICD-10-CM R52 be released?
The 2022 edition of ICD-10-CM R52 became effective on October 1, 2021.
What is the pain of the coccyx?
Pain of coccyx greater than 3 months, chronic. Clinical Information. A disorder characterized by the sensation of marked discomfort, distress or agony. An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons.
What is the ICd 10 code for pain?
The ICD-10-CM Index indicates that pain NOS is reported with code R52 (Pain, unspecified). However, reimbursement for this vague code is likely to be problematic, so try to obtain a more specific diagnosis whenever possible.
What is the code for abdominal pain?
In addition to the codes for pain in the various parts of the abdomen, there are codes for: Acute abdomen (R10.0): This is sudden, severe abdominal pain, often accompanied by rigidity of the abdomen.
What is the G89 code?
For example, you can assign a G89 code to indicate that the pain is acute or chronic. You should assign the site-specific pain code first unless the purpose of the encounter is pain management, in which case the G89 code is first. For example, a patient is referred for ankle x-rays for chronic right ankle pain.
What is a pain that does not point to a specific body system?
Pain that does not point to a specific body system is classified in the Symptoms and Signs chapter. For example, abdominal pain is classified to category R10. Certain specific types of pain are classified to category G89 (Pain, not elsewhere classified) in the Nervous System chapter.
Why do radiologists order pain studies?
Many imaging studies are ordered because the patient is experiencing pain. Once ICD-10 is implemented on October 1 of next year, radiology coders will need to be ready to assign the appropriate codes for these studies. In this article we’ll give you a run-down of how pain is classified in ICD-10, as well as the rules for sequencing the pain codes.
What is R10.81?
Abdominal tenderness (R10.81-): Tenderness is abnormal sensitivity to touch. While pain is a symptom that the patient reports, tenderness is a reaction that the physician observes while examining the patient’s abdomen.
What does R07.1 mean?
Chest pain on breathing (R07.1): This type of pain can be a sign of pulmonary embolism.
What is pain in the nervous system?
Intensely discomforting, distressful, or agonizing sensation associated with trauma or disease, with well-defined location, character, and timing. Pain is a feeling triggered in the nervous system. Pain may be sharp or dull. It may come and go, or it may be constant.
What does it mean to feel pain?
Sensation of unpleasant feeling indicating potential or actual damage to some body structure felt all over, or throughout the body. Severe pain of limited duration. The sensation of discomfort, distress, or agony, resulting from the stimulation of specialized nerve endings.
How long does pain last without pain?
Once you take care of the problem, pain usually goes away. However, sometimes pain goes on for weeks, months or even years. This is called chronic pain.
What is a disorder characterized by the sensation of marked discomfort, distress or agony?
An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons. Causing physical or psychological misery, pain or distress. Intensely discomforting, distressful, or agonizing sensation associated with trauma or disease, ...
How many codes are required to describe a condition?
A code also note instructs that 2 codes may be required to fully describe a condition but the sequencing of the two codes is discretionary, depending on the severity of the conditions and the reason for the encounter.
Is G89 a reimbursement code?
Pain, not elsewhere classified. G89 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. The 2021 edition of ICD-10-CM G89 became effective on October 1, 2020.

Popular Posts:
- 1. icd 10 code for other alcohol-induced disorder
- 2. icd 10 code for chronic cholithiasis
- 3. icd-10 code for stool burden
- 4. icd 10 code for postoperative wound
- 5. icd 10 code for focal hemorrhagic contusion of cerebrum
- 6. icd 10 code for r14.0
- 7. icd 10 code for capsule sprain
- 8. icd 10 code for facial basal cell carcinoma
- 9. icd 10 code for status post catheter
- 10. icd 9 code for high psa