How do you fix vaginal prolapse?
What you can do
- List symptoms you've been having, and for how long
- List all medications, vitamins and supplements you take, including the doses
- List key personal and medical information, including other conditions, recent life changes and stressors
- Prepare questions to ask your doctor
Which vaginal procedure is best for uterine prolapse?
Your doctor will perform vaginal prolapse surgery using one of the following approaches:
- Minimally invasive surgery uses a laparoscope, which is a thin, lighted instrument with a small camera that transmits pictures of the inside of your body to a video screen. ...
- Open surgery allows your surgeon to directly view and access the inside of your body. ...
- Vaginal approach involves repairing your vaginal prolapse through the vagina. ...
How to reverse pelvic prolapse and avoid prolapse surgery?
- Leg press
- Squats
- Bicycle legs
- Leg raises How to exercise safely If you are ready to exercise, then your regular workout routine will have to be modified. ...
- Pelvic Organ Prolapse (POP) happens when pelvic floor muscles become loose or weaken
What are the surgical options for rectal prolapse?
What you can expect
- Before the procedure. Rectal prolapse surgery can be done through the abdomen (rectopexy) — either with a large incision (open surgery) or laparoscopic methods — or through the region around ...
- During the procedure. Rectal prolapse repair through the abdomen. ...
- After the procedure. ...
What is vault prolapse?
Vaginal prolapse, also known as vaginal vault prolapse, occurs when the top of the vagina weakens and collapses into the vaginal canal. In more serious cases of vaginal prolapse, the top of the vagina may bulge outside the vaginal opening.
What is vault prolapse repair?
What happens in this type of surgery? The aim is to restore the vagina to its natural position. This involves attaching the top of the vagina to a ligament in the pelvis using synthetic stitches (sutures). Surgeons may use stitches that eventually dissolve or stitches that remain in the body permanently.
How many degrees is a vault prolapse?
First-degree prolapse: The uterus droops into the lower portion of the vagina. Second-degree prolapse: The uterus falls to the level of the vaginal opening. Third-degree prolapse: The cervix, which is located at the bottom of the uterus, sags to the vaginal opening and protrudes outside the body.
What is prolapse of vaginal vault after hysterectomy?
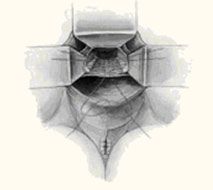
Vaginal Vault Prolapse (After Hysterectomy) The top of the vagina drops down, creating a bulge. In severe cases, the top of the vagina may protrude outside of the vagina. It also may occur with small intestine prolapse (shown here), anterior vaginal wall prolapse, or posterior vaginal vault prolapse.
How is vaginal vault prolapse diagnosed?
Symptoms of vaginal vault prolapse Weak urinary stream, straining to urinate and difficulty emptying the bladder. Increased urinary infections. Vaginal bleeding and discharge. A bulge of tissue that may protrude from the vagina, and the need to apply finger pressure to this bulge in order to urinate or empty the bowels.
What is the most common cause of vault prolapse following hysterectomy?
Vaginal vault prolapse commonly occurs following a hysterectomy (removal of the uterus (womb)). Because the uterus provides support for the top of the vagina, this condition occurs in up to 40% of women after a hysterectomy. In a vaginal vault prolapse, the top of the vagina gradually falls toward the vaginal opening.
What is vault in hysterectomy?
Abstract. Post-hysterectomy vaginal vault prolapse is a common disorder which generally manifests as a protrusion of the vagina through the genital hiatus, sometimes accompanied by urinary and gastrointestinal symptoms as well as sexual dysfunction.
What is vault eversion?
Vaginal vault prolapse refers to significant descent of the vaginal apex following a hysterectomy (see the image below), whereas uterovaginal prolapse denotes apical prolapse of the cervix, uterus, and proximal vagina. Enterocele and massive vaginal eversion.
What are the different types of prolapse?
Types of prolapse include:Vaginal vault prolapse. This is a condition where the upper walls of the vagina lose their normal shape, resulting in a collapse into the vaginal canal or lower. ... Uterine prolapse. ... Bladder prolapse. ... Rectocele prolapse. ... Enterocele prolapse. ... Preventing or treating a prolapse.
What is vault suspension surgery?
A Laparoscopic Vault Suspension is a minimally-invasive surgical procedure that is used to treat cases of vaginal vault prolapse. The aim of the surgery is to repair and support the vaginal vault in a way that does not interfere with vaginal capacity or sexual intercourse.
How can vaginal vault prolapse be prevented?
Suspension of the vaginal apex to the uterosacral ligaments (McCall culdoplasty) or to the sacrospinous ligaments at the time of vaginal hysterectomy is the mainstay for prevention of post hysterectomy vaginal vault prolapse.
How do you fix a prolapse without surgery?
The two non-surgical options for prolapse are pelvic floor muscle training (PFMT) and a vaginal pessary. PFMT can be effective for mild prolapse but is usually not successful for moderate and advanced prolapse. The main alternative to surgery for prolapse is a vaginal pessary.
How can I rebuild my vaginal walls?
Your surgeon will:Make a surgical cut through the front wall of your vagina.Move your bladder back to its normal location.May fold your vagina, or cut away part of it.Put sutures (stitches) in the tissue between your vagina and bladder. ... Place a patch between your bladder and vagina.More items...
MS-DRG Mapping
DRG Group #742-743 - Uterine and adnexa procedure for non-malignancy with CC or MCC.
ICD-10-CM Alphabetical Index References for 'N99.3 - Prolapse of vaginal vault after hysterectomy'
The ICD-10-CM Alphabetical Index links the below-listed medical terms to the ICD code N99.3. Click on any term below to browse the alphabetical index.
Equivalent ICD-9 Code GENERAL EQUIVALENCE MAPPINGS (GEM)
This is the official exact match mapping between ICD9 and ICD10, as provided by the General Equivalency mapping crosswalk. This means that in all cases where the ICD9 code 618.5 was previously used, N99.3 is the appropriate modern ICD10 code.
What is the ICd 10 code for a vaginal vault?
618.5 is a legacy non-billable code used to specify a medical diagnosis of prolapse of vaginal vault after hysterectomy. This code was replaced on September 30, 2015 by its ICD-10 equivalent.
What is the ICd-9 GEM?
The GEMs are the raw material from which providers, health information vendors and payers can derive specific applied mappings to meet their needs.

Popular Posts:
- 1. icd 10 code for hypogammaglobinemia
- 2. icd 10 code for intentional trazodone overdose
- 3. icd 9 code for grade 3 internal hemorrhage with ventriculoperitoneal shunt
- 4. icd 10 code for breast infection
- 5. icd 10 code for x rays both foot
- 6. icd 10 code for infected 2nd degree burn of scalp
- 7. icd 10 code for copd with asthma
- 8. icd 10 code for ibs diarrhea
- 9. icd-10 code for observation after fall
- 10. what icd-10-cm code is reported for a personal history of malignant neoplasm of the breast