What is the purpose of ICD 10?
Why ICD-10 codes are important
- The ICD-10 code system offers accurate and up-to-date procedure codes to improve health care cost and ensure fair reimbursement policies. ...
- ICD-10-CM has been adopted internationally to facilitate implementation of quality health care as well as its comparison on a global scale.
- Compared to the previous version (i.e. ...
What is ICD 10 code covers an ESR?
ICD Codes are listed on subsequent page(s) of this document. 85651, 85652 Sedimentation Rate, Erythrocyte Coverage Indications, Limitations, and/or Medical Necessity The erythrocyte sedimentation rate (ESR) is a sensitive but nonspecific test that is frequently the earliest indicator of disease when other chemical or physical signs are normal.
What is the ICD 10 diagnosis code for?
The ICD-10-CM is a catalog of diagnosis codes used by medical professionals for medical coding and reporting in health care settings. The Centers for Medicare and Medicaid Services (CMS) maintain the catalog in the U.S. releasing yearly updates.
What is the ICD 10 code for esophageal dysmotility?
What is the ICD 10 code for esophageal dysmotility? K22. 4 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2020 edition of ICD-10-CM K22.
How do you code esophageal dysphagia?
Dysphagia, pharyngoesophageal phase R13. 14 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM R13. 14 became effective on October 1, 2021.
What is esophageal dysphagia?
Esophageal dysphagia. Esophageal dysphagia refers to the sensation of food sticking or getting caught in the base of your throat or in your chest after you've started to swallow. Some of the causes of esophageal dysphagia include: Achalasia.
What is the ICD 10 code for oral dysphagia?
R13. 11, Dysphagia, oral phase.
What is R13 19 code?
Other dysphagiaR13. 19, Other dysphagia, which includes cervical dysphagia and neurogenic dysphagia.
Is GERD considered esophageal dysphagia?
While dysphagia can be attributed to a variety of causes, one of the most common is chronic acid reflux caused by gastroesophageal reflux disease (GERD). GERD is a common digestive disease characterized by chronic acid reflux, which occurs when stomach acid flows back into the esophagus.
What is the most common cause of esophageal dysphagia?
Mechanical or obstructive esophageal disorders are the most common causes of esophageal dysphagia, and patients generally present with dysphagia to solids alone with potential progression to include liquids. Mechanical obstruction can manifest with symptoms of intermittent dysphagia or progressive symptoms.
What is the ICD-10 code for esophagitis?
ICD-10 code K20. 9 for Esophagitis, unspecified is a medical classification as listed by WHO under the range - Diseases of the digestive system .
What is oral phase dysphagia?
Oral dysphagia refers to problems with using the mouth, lips and tongue to control food or liquid. Pharyngeal dysphagia refers to problems in the throat during swallowing. Dysphagia may lead to aspiration (where food or liquid gets into the lungs). Dysphagia can affect a person at any age, from infants to the elderly.
What is Oropharyngeal dysphagia?
Oropharyngeal or transfer dysphagia is characterized by difficulty initiating a swallow. Swallowing may be accompanied by nasopharyngeal regurgitation, aspiration, and a sensation of residual food remaining in the pharynx.
What does code Z12 11 mean?
Z12. 11: Encounter for screening for malignant neoplasm of the colon.
What is the ICD 10 code for GERD?
ICD-10-CM Code for Gastro-esophageal reflux disease without esophagitis K21. 9.
What is the ICD 10 code for choking on food?
Food in respiratory tract, part unspecified causing asphyxiation, initial encounter. T17. 920A is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM T17.
What are the two types of dysphagia?
Dysphagia is classified into two distinct types: oropharyngeal dysphagia due to malfunction of the pharynx and upper esophageal sphincter; and esophageal dysphagia due to malfunction of the esophagus. Difficulty in swallowing. Difficulty swallowing.
What is swallowing symptom?
A symptom referring to difficulty in swallowing. It may be observed in patients with stroke, motor neuron disorders, cancer of the throat or mouth, head and neck injuries, parkinson disease, and multiple sclerosis. Difficulty in swallowing which may result from neuromuscular disorder or mechanical obstruction.
What is esophageal motility?
Esophageal motility refers to contractions occurring in the esophagus, which propel the food bolus forward toward the stomach. When contractions in the esophagus become irregular, unsynchronized or absent, the patient is said to have esophageal dysmotility. Furthermore, what is Presbyesophagus?
What is the shape of the esophagus called?
Presbyesophagus is a term used to describe an abnormal shape of the swallowing tube (esophagus) that occurs in some individuals. In this situation, the esophagus appears wavier than a typically straight esophagus. This change may impact esophageal movement (motility).
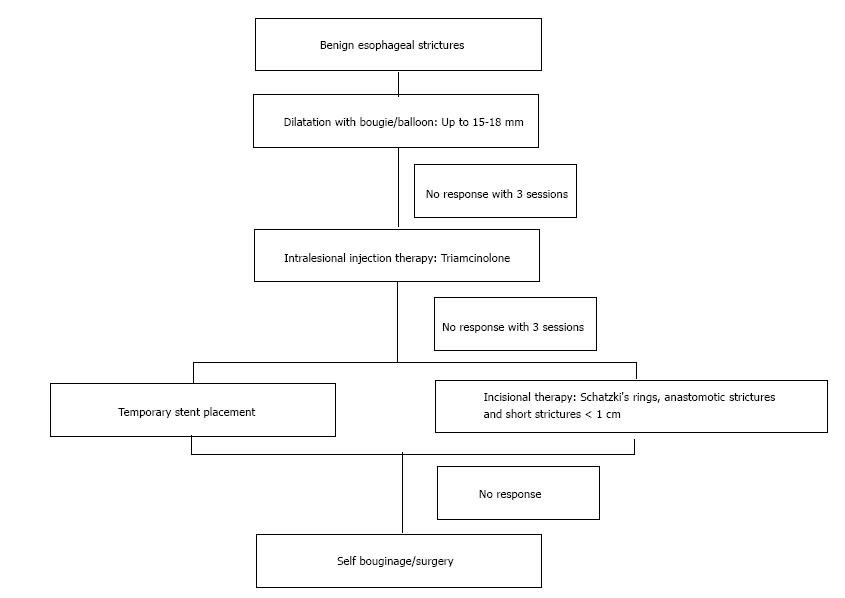
How to treat esophageal dysphagia?
Treatment for esophageal dysphagia may include esophageal dilation, surgery to remove esophageal tumor or diverticulum, or medication. Severe dysphagia may require the insertion of a feeding tube (96.6) or a percutaneous endoscopic gastrostomy tube (43.11).
What is the code for psychogenic dysphagia?
Psychogenic dysphagia is assigned to code 306.4, Gastrointestinal malfunction arising from mental factors. Since dysphagia is a symptom, it will not be sequenced as the principal diagnosis if the underlying cause has been documented by the physician. However, the appropriate code for dysphagia may be coded and sequenced as a secondary diagnosis ...
What are the complications of dysphagia?
Dysphagia can lead to the following complications: • malnutrition (categories 260 to 263) ; • dehydration (276.51); and. • aspiration pneumonia (507.0). Diagnosis. To diagnose the underlying cause of the dysphagia, a physician may perform any of the following tests: • barium swallow or modified barium swallow;
When should a symptom code not be sequenced as the principal diagnosis?
In other words, a symptom code should not be sequenced as the principal diagnosis when a related definitive diagnosis has been established. Since dysphagia is a symptom, it will not be sequenced as the principal diagnosis if the underlying cause has been documented by the physician. — Audrey Howard.
Is dysphagia a serious condition?
Dysphagia alone may not be of concern, but it may be indicative of a more serious condition requiring treatment if it persists or is severe. In addition, the condition may make it difficult for a patient to consume enough calories or fluids, which can lead to additional medical problems.
Can you swallow with dysphagia?
Dysphagia constitutes a difficulty in swallowing, which may also be associated with pain. Occasionally, a patient may not be able to swallow at all. Although dysphagia can occur at any age, it is more common in older adults. Dysphagia alone may not be of concern, but it may be indicative of a more serious condition requiring treatment ...
Can dysphagia be coded?
However, the appropriate code for dysphagia may be coded and sequenced as a secondary diagnosis if it is not inherent to the disease process. Symptoms. The following signs and symptoms are often associated with dysphagia: • pain while swallowing (odynophagia); • inability to swallow;
Popular Posts:
- 1. icd 10 code for septic left hip
- 2. icd 10 cm code for secondary lymph neoplasm
- 3. icd icd 10 code for family history of diabetes
- 4. icd 10 code for post right hip arthroplasty
- 5. icd 10 code for right proximal tibia fracture
- 6. what is the icd 10 code for pathologic fracture in neoplastice disease
- 7. icd 10 code for abdominal wall endometrioma
- 8. icd 10 code for preterm delivery third trimester
- 9. icd 10 code for retrolisthesis
- 10. icd 10 code for status post heart catheterization