What is the difference between initial fusion and Refusion in ICD 10?
In ICD-9, there were specific codes to show if the fusion was an initial fusion, or if it was a refusion. In ICD-10-PCS, initial fusions and refusion procedures are coded to the same root operation “fusion.” The definition in ICD-10-PCS for fusion is “joining together portions of an articular body part rendering the articular body part immobile.”
What is the ICD 10 version of fusion of spine?
Fusion of spine, cervical region. This is the American ICD-10-CM version of M43.22 - other international versions of ICD-10 M43.22 may differ.
What is the ICD 10 code for pseudarthrosis after fusion?
Pseudarthrosis after fusion or arthrodesis. 2016 2017 2018 2019 Billable/Specific Code. M96.0 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2018/2019 edition of ICD-10-CM M96.0 became effective on October 1, 2018.
What is the ICD-10 code for nonunion right first MTP fusion?
Anyone know the ICD-10 code for Nonunion right first MTP fusion? Thanks. This is in the Code Set M96: Intra-operative and Post-procedural complications and disorders of the musculoskeletal system, NEC.
What is the secondary code for Chapter 20?
When will the ICD-10-CM T84.098A be released?
About this website
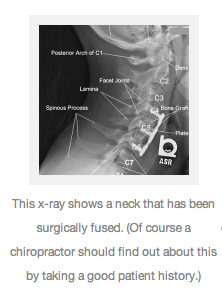
What is the ICD-10 DX code for fusion status?
Fusion of spine, site unspecified M43. 20 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM M43. 20 became effective on October 1, 2021.
What is pseudarthrosis after fusion?
Pseudarthrosis refers to a failure of fusion after an index procedure intended to obtain spinal arthrodesis [4,5,12]. The term suggests the presence of a false joint, although it is commonly used to describe a lack of fusion that occurs after an attempted arthrodesis.
What is the ICD-10 code for Status post cervical fusion?
ICD-10 code M43. 22 for Fusion of spine, cervical region is a medical classification as listed by WHO under the range - Dorsopathies .
What is the ICD-10 code for status post lumbar fusion?
Fusion of spine, lumbar region M43. 26 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM M43. 26 became effective on October 1, 2021.
What is a failed fusion?
The union of the fusion mass occurs over time. When the time for healing is extended or the fusion fails to unite, this is a called a "failed fusion" or pseudoarthrosis.
What is the meaning of pseudarthrosis?
Pseudarthrosis is defined as an absence of bridging bone between grafted bone and vertebral bodies and the presence of a radiolucent defect, a halo sign, or a loss of grafted bone.
How do you code a spinal fusion in ICD 10 PCS?
The code for the posterior lumbar fusion is 0SG107J, with the device value being 7 for autologous substitute. The code for the discectomy is 0SB20ZZ, with the root operation being Excision. If the operative report documents that a discectomy is performed, the correct root operation is Excision.
What does arthrodesis status mean?
Arthrodesis refers to the fusion of two or more bones in a joint. In this process, the diseased cartilage is removed, the bone ends are cut off, and the two bone ends are fused into one solid bone with metal internal fixation.
What is fusion of the spine?
Spinal fusion is surgery to permanently connect two or more vertebrae in your spine, eliminating motion between them. Spinal fusion involves techniques designed to mimic the normal healing process of broken bones.
Is a laminectomy the same as a spinal fusion?
Laminectomy (removal of lamina bone) and diskectomy (removing damaged disk tissue) are both types of spinal decompression surgery. Your provider may perform a diskectomy or other techniques (such as joining two vertebrae, called spinal fusion) during a laminectomy procedure.
What is the ICD-10 code for right ankle fusion?
0SGF05ZICD-10-PCS Code 0SGF05Z - Fusion of Right Ankle Joint with External Fixation Device, Open Approach - Codify by AAPC.
What are the symptoms of pseudarthrosis?
What are the symptoms of pseudarthrosis? The symptoms of pseudoarthrosis are similar to those of osteoarthritis and include; lack of mobility, persistent pain, joint clicking and in some cases, redness and even fever.
How do you fix pseudarthrosis?
Pseudarthrosis occurs when a spinal fusion surgery fails. Some people with this condition experience no symptoms; some people feel pain in their neck, back, arms or legs. Diagnosis of pseudarthrosis involves imaging tests of the spine. The treatment for pseudarthrosis is a second spinal fusion surgery.
What is the cause of pseudarthrosis?
Causes. Pseudarthrosis occurs when bones fail to fuse with one another after spinal fusion surgery. Factors that reduce the ability of bone-producing cells (called osteoblasts) to produce new bone for fusion increase the risk of Pseudarthrosis.
What does a failed spinal fusion feel like?
Symptoms may include chronic pain in the back, neck, or legs, which can be dull or sharp, aching, burning, or radiating. The pain may continue after surgery or reappear several days or weeks afterward. It can worsen as scar tissue builds in the spinal nerve roots, which extend from the spinal cord.
Removal of hardware | Medical Billing and Coding Forum - AAPC
If this is your first visit, be sure to check out the FAQ & read the forum rules.To view all forums, post or create a new thread, you must be an AAPC Member.If you are a member and have already registered for member area and forum access, you can log in by clicking here.If you've forgotten your username or password use our password reminder tool.
2022 ICD-10-CM Diagnosis Code T84.293A
Free, official coding info for 2022 ICD-10-CM T84.293A - includes detailed rules, notes, synonyms, ICD-9-CM conversion, index and annotation crosswalks, DRG grouping and more.
ICD10 EZ Sheet for Knee Arthroplasty ICD10 BITK S81.051 (R, +1 for L)*
ICD10 EZ‐Sheet for Knee Arthroplasty ICD10 BITK – S81.051 (R, +1 for L)* 1. OA of knee a. Bilateral primary – M17.0 b. Unilateral primary, R – M17.11
2022 ICD-10-CM Diagnosis Code T84.093A
ICD-10-CM Codes › S00-T88 Injury, poisoning and certain other consequences of external causes ; T80-T88 Complications of surgical and medical care, not elsewhere classified ; T84-Complications of internal orthopedic prosthetic devices, implants and grafts 2022 ICD-10-CM Diagnosis Code T84.093A
Revision of Failed Total Shoulder Arthroplasty - AHA Coding Clinic ...
AHA Coding Clinic ® for ICD-9 - 2004 Issue 1; Ask the Editor Revision of Failed Total Shoulder Arthroplasty. A 65-year old man with a history of total shoulder arthroplasty is being admitted for a revision of right total shoulder arthroplasty with glenoid component and cemented humeral components.
Failed Thumb Carpometacarpal Arthroplasty: Common Etiologies and ...
Carpometacarpal (CMC) arthroplasty surgery, although modifications have occurred over time, continues to be commonly performed and has provided patients with their desired pain relief and return of function. The complications of primary surgery, although relatively rare, can present in various clini …
What is the secondary code for Chapter 20?
Use secondary code (s) from Chapter 20, External causes of morbidity, to indicate cause of injury. Codes within the T section that include the external cause do not require an additional external cause code. Type 1 Excludes.
When will the ICD-10-CM T84.098A be released?
The 2022 edition of ICD-10-CM T84.098A became effective on October 1, 2021.
What is the ICd 10 code for internal fixation device?
Other mechanical complication of internal fixation device of vertebrae 1 T84.296 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail. 2 Short description: Mech compl of internal fixation device of vertebrae 3 The 2021 edition of ICD-10-CM T84.296 became effective on October 1, 2020. 4 This is the American ICD-10-CM version of T84.296 - other international versions of ICD-10 T84.296 may differ.
When will the ICd 10 T84.296 be released?
The 2022 edition of ICD-10-CM T84.296 became effective on October 1, 2021.
What is the secondary code for Chapter 20?
Use secondary code (s) from Chapter 20, External causes of morbidity, to indicate cause of injury. Codes within the T section that include the external cause do not require an additional external cause code. Type 1 Excludes.
Can you use T84.296 for reimbursement?
T84.296 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail.
Why do you need spinal fusion?
Here are the most common reason an initial spinal fusion may be needed: Degenerative disc disease/disc degeneration. Spinal stenosis/neurogenic claudication.
How long does it take for a spinal cord to fuse?
Oftentimes, it takes months for the spinal vertebrae to heal and fuse together. A successful fusion or refusion would be defined as; when the vertebrae that were fused together heal into a single solid bone. There is no time limit on when a fusion may be considered a failed fusion/non-union.
How long does it take for a spinal fusion to heal?
Oftentimes, it takes months for the spinal vertebrae to heal and fuse together. A successful fusion or refusion would be defined as; when the vertebrae that were fused together heal into a single solid bone. There is no time limit on when a fusion may be considered a failed fusion/non-union.
Why do we need a refusion of the spine?
Here are the most common reasons a refusion of the spine may be needed: Pseudoarthrosis/non-union/failed fusion. Injury resulting in damage to the initial fusion. Complications of the initial area fused. Spinal fusions are performed to permanently connect two or more vertebrae in the spine that eliminates motion between them.
Can a spinal fusion be performed on a specific vertebrae?
The patient could have had a past fusion at a different level, but it is determined based on the level that is being fused and not the past history. In the same operative note, there may be documentation of an initial level of fusion as well as another level that may have required a refusion. Here are the most common reason an initial spinal fusion may be needed:
Is there a time limit for fusion?
There is no time limit on when a fusion may be considered a failed fusion/non-union. Click here to read Part 1: Spinal Fusion Coding — Diagnoses Responsible. Be on the lookout for Part 3, that will discuss how to determine the level (s) of a fusion as well as number of vertebrae being fused together. References.
Is fusion and refusion the same operation?
Although, in ICD-10-PCS, the fusion and refusion are both coded to the same root operation of fusion, coders still need to know which the surgeon is performing. This will also alert the coder to look for additional procedures that may need to be captured in the operative note documentation (such as a removal of previous device).
What is the secondary code for Chapter 20?
Use secondary code (s) from Chapter 20, External causes of morbidity, to indicate cause of injury. Codes within the T section that include the external cause do not require an additional external cause code. Type 1 Excludes.
When will the ICD-10-CM T84.098A be released?
The 2022 edition of ICD-10-CM T84.098A became effective on October 1, 2021.
Popular Posts:
- 1. icd 10 code for dx code discuss colostomy reversal
- 2. icd 10 code for egg component panel
- 3. icd 10 pcs code for undifferentiated connective tissue disease
- 4. 2016 icd 10 code for fracture right wrist
- 5. icd 10 code for pes anserine bursitis of left knee
- 6. icd 10 code for rule out meniscal tear
- 7. icd 10 code for ulcer of right foot
- 8. icd 10 code for syringomyelia and syringobulbia
- 9. icd 10 code for left breast cancer upper outer quadrant
- 10. icd 10 code for lumbar spine mass