What is the prognosis of pericardial effusion?
The prognosis of pericardial effusion depends on the underlying etiology[10,11,15,16] being especially poor in patients with neoplastic pericardial effusion secondary to lung cancer and positive cytologic study (presence of malignant cells) in pericardial fluid. Prognosis is very good in idiopathic/viral pericarditis.
How is a pericardial effusion diagnosed?
The tests most commonly used to diagnose and evaluate pericardial effusion include:
- Chest x-ray.
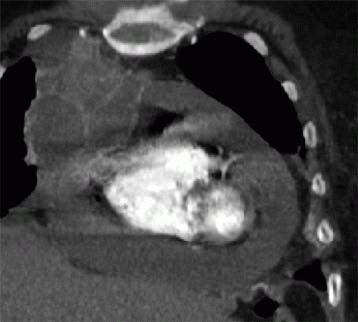
- Computed tomography (CT) scan of the chest.
- MRI of the heart.
- Echocardiogram.
- Pericardiocentesis: a procedure that uses a needle to remove fluid from the pericardium; the fluid is then examined to determine the cause of the effusion. ...
Does echocardiogram show pericardial effusion?
The main way to assess a pericardial effusion is an ultrasound scan of the heart known as an echocardiogram. The echo helps quantify the amount of fluid around the heart, tells us how the heart is handling the excess fluid, and determines what action must be taken.
What is normal pericardial fluid?
Normal pericardial fluid has small numbers of white blood cells (WBCs) but no red blood cells (RBCs) or microorganisms. Laboratories may examine drops of the pericardial fluid and/or use a special centrifuge (cytocentrifuge) to concentrate the fluid’s cells at the bottom of a test tube.
What is the CPT code for pericardial effusion?
3 - Pericardial effusion (noninflammatory)
What is acute pericardial effusion?
Overview. Pericardial effusion (per-e-KAHR-dee-ul uh-FU-zhun) is the buildup of too much fluid in the double-layered, saclike structure around the heart (pericardium). The space between these layers typically contains a thin layer of fluid.
Which is the correct code for unspecified acute pericarditis?
ICD-10 Code for Acute pericarditis, unspecified- I30. 9- Codify by AAPC.
What is the difference between acute pericarditis and pericardial effusion?
Acute pericarditis is the most common pericardial disease and in most instances is accompanied by pericardial effusion. On the other hand, pericardial effusion may appear as a separate clinical entity occasionally characterized by absence of inflammatory markers elevation.
What is the difference between pleural effusion and pericardial effusion?
pleural effusion - what is the difference? A: Pericardial effusion is the term for a buildup of fluid around the heart. Pleural effusion is the term for a buildup of fluid around the lungs, or, more accurately, in the space between the lungs and the chest cavity.
What is the difference between pericardial effusion and cardiac tamponade?
Pericardial effusion is the accumulation of fluid in the pericardial space. Cardiac tamponade. Pericarditis is the accumulation of pericardial fluid. Heart: Anatomy sufficient to impair cardiac filling and cause hemodynamic compromise.
What is acute pericarditis?
Acute pericarditis is a painful condition where the fluid-filled pouch around your heart is inflamed. This can happen because of infections, cancer or heart surgery. While it's usually not dangerous on its own, it shares symptoms with a heart attack.
What is the treatment for pericardial effusion?
Drainage procedures or surgery to treat pericardial effusion may include: Fluid drainage (pericardiocentesis). A health care provider uses a needle to enter the pericardial space and then inserts a small tube (catheter) to drain the fluid. Imaging techniques, typically echocardiography, are used to guide the work.
What is the ICD 10 code for pleural effusion?
ICD-10 Code for Pleural effusion in other conditions classified elsewhere- J91. 8- Codify by AAPC.
What is the most common cause of pericardial effusion?
Lung cancer is the most common cause of the malignant pericardial effusion. Trauma: Blunt, penetrating, and iatrogenic injury to the myocardium, aorta, or coronary vessels can lead to the accumulation of blood within the pericardial sac.
What medications cause pericardial effusion?
Causes of Pericardial Effusion Certain prescription drugs, such as hydralazine, a medication for high blood pressure; isoniazid, a tuberculosis drug; and phenytoin, a medication for epileptic seizures. Chemotherapy drugs, such as doxorubicin and cyclophosphamide. Blockage of the flow of pericardial fluids.
Does pericarditis always cause pericardial effusion?
Approximately 15 to 30 percent of people with sudden onset (acute) pericarditis have either recurrent or persistent disease, frequently with a pericardial effusion. This risk is reduced in people who initially take colchicine and in those without a known cause of pericarditis (idiopathic pericarditis).
What is the most common cause of a pericardial effusion?
Lung cancer is the most common cause of the malignant pericardial effusion. Trauma: Blunt, penetrating, and iatrogenic injury to the myocardium, aorta, or coronary vessels can lead to the accumulation of blood within the pericardial sac.
What is the treatment for pericardial effusion?
Drainage procedures or surgery to treat pericardial effusion may include: Fluid drainage (pericardiocentesis). A health care provider uses a needle to enter the pericardial space and then inserts a small tube (catheter) to drain the fluid. Imaging techniques, typically echocardiography, are used to guide the work.
How do you get pericardial effusion?
Pericardial effusion can happen after heart surgery, radiation therapy for cancer or as a side effect of some medications. Other. Pericardial effusion can also happen with heart failure, chronic kidney disease or kidney failure, liver cirrhosis or for unknown reasons.
Is pericardial effusion curable?
Depending on the severity of the buildup, pericardial effusion may be treatable with medicines. If the health care team determines that it's necessary to drain the excess fluid, they may recommend a procedure called pericardiocentesis, which uses a needle and small catheter to drain the fluid.
What is the ICD code for pericardial effusion?
I31.3 is a billable ICD code used to specify a diagnosis of pericardial effusion (noninflammatory). A 'billable code' is detailed enough to be used to specify a medical diagnosis.
What is the term for the accumulation of fluid in the pericardial cavity?
Pericardial effusion ("fluid around the heart") is an abnormal accumulation of fluid in the pericardial cavity. Because of the limited amount of space in the pericardial cavity, fluid accumulation leads to an increased intrapericardial pressure which can negatively affect heart function.
What is the ICD-10 code for pericardial effusion?
Look also at ICD-10-CM code I30.9 for acute neoplastic pericardial effusion present on admission (POA) plus the C code for secondary malignancy POA and finally, pericardial tamponade, not POA, suggests Robert S. Gold, MD, CEO of DCBA, Inc., in Atlanta.
What is the diagnosis code for malignant pleural effusion?
A: J91.0 (Malignant pleural effusion) is a manifestation code and cannot be sequenced as the principal diagnosis, says Sharon Salinas, CCS, Health Information Management, at Barlow Respiratory Hospital in Los Angeles.

Popular Posts:
- 1. icd 10 code for triamcinolone
- 2. icd 10 pcs code for total colectomy
- 3. 2017 icd 10 code for drug abuse
- 4. icd-10-cm code for obsessive-compulsive disorder
- 5. icd 10 code for bilateral upper extremity paresthesia
- 6. what is the icd 10 code for acute cervical trauma
- 7. icd 9 code for history of vitamin b12 deficiency
- 8. icd 10 code for family history of laryngeal cancer
- 9. icd-10 code for inury to nose right nare
- 10. icd 10 code for family history cad