What is the diagnosis code for allergies?
What is the ICD 10 code for environmental allergies? T78. 40XA is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2020 edition of ICD-10-CM T78.
What is the ICD 10 code for allergies?
Allergy, unspecified, initial encounter T78. 40XA is a billable/specific ICD-10-CM code that ...
What is the diagnosis code for allergic reaction?
T78.40XA is a billable diagnosis code used to specify a medical diagnosis of allergy, unspecified, initial encounter. The code T78.40XA is valid during the fiscal year 2021 from October 01, 2020 through September 30, 2021 for the submission of HIPAA-covered transactions.
What is the ICD 10 code for latex allergy?
ICD-10-CM Code for Latex allergy status Z91.040 ICD-10 code Z91.040 for Latex allergy status is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .

What is ICD-10 code T78 40XA?
ICD-10 code T78. 40XA for Allergy, unspecified, initial encounter is a medical classification as listed by WHO under the range - Injury, poisoning and certain other consequences of external causes .
What is the ICD-10 code for unspecified allergies?
ICD-10 code: T78. 4 Allergy, unspecified | gesund.bund.de.
Can Z76 89 be used as a primary diagnosis?
The patient's primary diagnostic code is the most important. Assuming the patient's primary diagnostic code is Z76. 89, look in the list below to see which MDC's "Assignment of Diagnosis Codes" is first. That is the MDC that the patient will be grouped into.
What is the ICD-10 code for environmental allergies?
2.
What is the medical code for allergies?
T78. 40 - Allergy, unspecified. ICD-10-CM.
What are allergy codes?
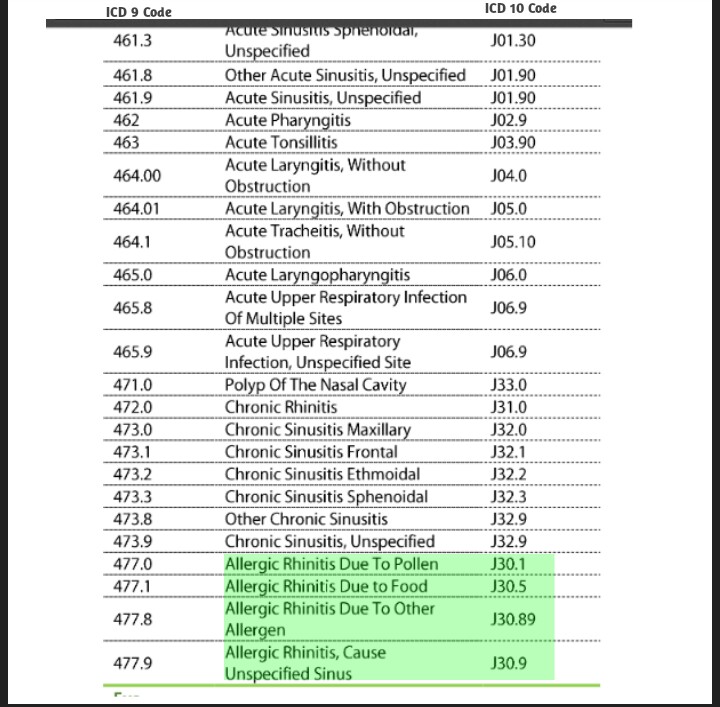
J30 – Vasomotor and allergic rhinitis.J30.0 – Vasomotor rhinitis.J30.1 – Allergic rhinitis due to pollen.J30.2 – Other seasonal allergic rhinitis.J30.5 – Allergic rhinitis due to food.J30.8 – Other allergic rhinitis. ... J30.9 – Allergic rhinitis, unspecified.
Is Z76 89 a billable code?
Z76. 89 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
Can Z15 01 be used as primary diagnosis code?
Codes from category Z15 should not be used as principal or first-listed codes.
Can you use Z codes as primary diagnosis?
Z codes may be used as either a first-listed (principal diagnosis code in the inpatient setting) or secondary code, depending on the circumstances of the encounter. Certain Z codes may only be used as first-listed or principal diagnosis.
What is an environmental allergy?
Environmental allergies involve an immune system overreaction to things that exist in our everyday surroundings, including home, work, and the great outdoors. You may also hear this immune system response referred to as hay fever or allergic rhinitis.
What is diagnosis code J30 89?
ICD-10-CM Code for Other allergic rhinitis J30. 89.
Are seasonal and environmental allergies the same?
Environmental Allergies Explained Environmental allergies are different from seasonal allergies in that they're found year-round versus different times of the year. Environmental allergies include exposure to dust mites, cockroaches and pet danger.
Can you bill for establishing care?
You can't code or bill a service that is performed solely for the purpose of meeting a patient and creating a medical record at a new practice.
What is the ICD-10 code for annual physical exam?
Z00.00ICD-10 Code for Encounter for general adult medical examination without abnormal findings- Z00. 00- Codify by AAPC.
What does obesity unspecified mean?
Having a high amount of body fat (body mass index [bmi] of 30 or more). Having a high amount of body fat. A person is considered obese if they have a body mass index (bmi) of 30 or more.
What is the ICD-10 code for referral to specialist?
Encounter for other administrative examinations The 2022 edition of ICD-10-CM Z02. 89 became effective on October 1, 2021. This is the American ICD-10-CM version of Z02.
What is an allergy?
An allergy is a reaction of your immune system to something that does not bother most other people. People who have allergies often are sensitive to more than one thing.
What is the term for an immunologic response to an initial exposure?
Hypersensitivity to an agent caused by an immunologic response to an initial exposure. Hypersensitivity; a local or general reaction of an organism following contact with a specific allergen to which it has been previously exposed and to which it has become sensitized.
What is an inflammatory response to an exogenous environmental antigen or an endogenous antigen initiated by the?
An inflammatory response to an exogenous environmental antigen or an endogenous antigen initiated by the adaptive immune system. [goc:jal, isbn:0781735149]
What is the secondary code for Chapter 20?
Use secondary code (s) from Chapter 20, External causes of morbidity, to indicate cause of injury. Codes within the T section that include the external cause do not require an additional external cause code. Type 1 Excludes.
When will the ICd 10 T78.40 be released?
The 2022 edition of ICD-10-CM T78.40 became effective on October 1, 2021.
What is dermatitis L23?
dermatitis ( L23 - L25, L27.-) A disorder characterized by an adverse local or general response from exposure to an allergen. A local or general reaction of an organism following contact with a specific allergen to which it has been previously exposed and to which it has become sensitized.
What is the ICD-10 code for allergies?
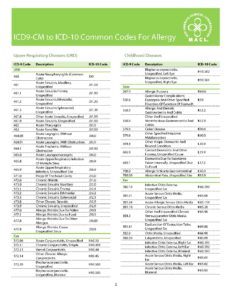
The ICD-10 Clinical Concept guide contains commonly used ICD-10 codes used in Allergy diagnosis. It is provided as a quick reference to help health care providers quickly find commonly used ICD-10 codes in the respective specialty. The complete list of ICD-10 diagnosis codes is also available in tabular format to find a specific code .
What is the meaning of J11.1?
J11.1 - Influenza due to unidentified influenza virus with other respiratory manifestations. J11.00 - Influenza due to unidentified influenza virus with unspecified type of pneumonia. J41.1 - Mucopurulent chronic bronchitis.
What is the ICd 10 code for Attention and Concentration Deficit?
R41.840 is a valid billable ICD-10 diagnosis code for Attention and concentration deficit . It is found in the 2021 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2020 - Sep 30, 2021 .
Do you include decimal points in ICD-10?
DO NOT include the decimal point when electronically filing claims as it may be rejected. Some clearinghouses may remove it for you but to avoid having a rejected claim due to an invalid ICD-10 code, do not include the decimal point when submitting claims electronically. See also: Deficit see also Deficiency.
What is delayed hypersensitivity skin testing?
Delayed Hypersensitivity Skin Testing has been commonly used in three ways: anergy testing, testing for infection with intracellular pathogens, and testing for sensitivity to contact allergens. Accurate testing for contact allergy requires careful attention to technique, and limitation of testing to the specific allergens known to be associated with a contact reaction.
What is allergy patch test?
Allergy patch testing is a covered procedure only when used to diagnose allergic contact dermatitis after the following exposures: dermatitis due to detergents, oils and greases, solvents, drugs and medicines in contact with skin, other chemical products, food in contact with skin, plants (except food), cosmetics, metals, rubber additives, other and unspecified. Patch tests may also be used and may be helpful when a distribution and persistence of dermatitis suggests a possible contact allergy, but the exact etiology of the dermatitis is unknown.
What is the purpose of the inhalation bronchial challenge test?
Inhalation Bronchial Challenge Testing involves the inhalation of agents that can trigger respiratory responses and are often used to evaluate new allergens and/or substantiate the role of allergens in patients with significant symptoms. Results of these tests are ordinarily evaluated by objective measures of pulmonary function and occasionally by characterization of bronchoalveolar lavage samples.
What is the treatment for a patient with an allergen?
Immunotherapy - this treatment involves injection of a patient with an allergen solution in an effort to develop an immune system tolerance. It treats the cause of the disease rather than managing the symptoms.
What is the medical record for allergy testing?
The medical record must document the elements of the medical and immunologic history including but not limited to correlation of symptoms; occurrence of symptoms; exposure profile; documentation of allergic sensitization by accepted means and where attempts at avoidance have proven unsuccessful (or the impracticality of avoidance exists); and a copy of the sensitivity results; along with the physical examination. Testing results and treatment need to justify the diagnosis and code on each claim form. The clinical condition that is claimed to justify this treatment must be clearly documented in the record. Note: A payable diagnosis alone does not support medical necessity of ANY service. The interpretation of the test results and how the results of the test was used in the patient’s plan of care for treatment and the management of the patient’s medical condition (s) must be documented. The treating physician must clearly document the medical necessity to initiate allergen immunotherapy and the continued need thereof. This plan of care needs to include the dosage regimen. Progress notes that document physician management during the course of the allergic disease, anticipated length of treatment, and explanation of any deviations from normal treatment frequency should be included. The record should be prepared so that the data regarding injection and responses can be appreciated in a logical and sequential sense. Documentation must support the use of the CPT code (e.g., number of venoms, number of vials) being billed.
What is documentation for allergy test?
There should be a permanent record of the allergy test and its interpretation including the test methodology and measurement (in mm) of reaction size of both wheal and erythema response in vivo testing. For the in vitro testing, the quantitative result (s) (in kIU/L) for specific IgE must be documented. If vitro testing is used, the medical necessity must be documented. All patient reaction (s) or complications should be recorded. The report should address or answer any specific clinical questions. If there are factors that prevent answering the clinical questions specific for this patient, this should be explained in the documentation. An official interpretation (final report) of the testing and plan for treatment, should be included in the patient’s medical record. Retention of the allergy test (s) and treatment plan should be consistent both with clinical need and with relevant legal and local health care facility requirements.
How many courses of allergy treatment are there?
There are three courses of treatments for allergy, which may be used individually, or in a combination with one another:
When an evaluation and management service is billed on the same day as allergen immunotherapy (by the same physician),?
When an evaluation and management service is billed on the same day as allergen immunotherapy (by the same physician), a separately identifiable service must be documented in the medical record.
How long is a reasonable supply of antigens?
A reasonable supply of antigens is considered to be not more than a 12-month supply of antigens that has been prepared for a particular patient at any one time. (CMS Pub 100-02 Medicare Benefit Policy Manual, Chapter 15- Covered Medical and Other Health Services, 50.4.4.1 – Antigens)
Is allergen immunotherapy effective?
1. Controlled studies have shown that allergen immunotherapy is effective for patients with:
Popular Posts:
- 1. icd-10 code for dialysis
- 2. icd 10 code for geographic atrophy
- 3. icd 10 code for fracture of right zygomatic bone
- 4. icd-10 code for delusions
- 5. icd 9 code for screening for hepatitis b immunity
- 6. what is icd-9 code for 786.09
- 7. icd 10 code for hyperkalemia due to missed dialysis
- 8. icd-10 code for surgical wound infection
- 9. icd 10 code for uncontrolled type 2 diabetes with complication
- 10. icd 10 code for 14. syncope resulting in fall